| OCR Text |
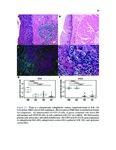
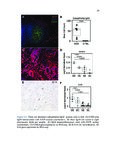
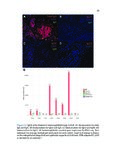
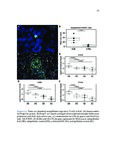
Show 52 predicting EoE food triggers identified by diet elimination trials is shown in Table 5.2. Of the nineteen patients with known food triggers, eleven opted for therapeutic diet elimination. These patients eliminated foods that demonstrated FSA reactivity. All 11 patients who eliminated FSA-reactive foods achieved clinical resolution of their disease, as defined by eosinophil count on biopsy (Figure 5.1A). These patients all showed decrease in their edema, rings, exudates, furrows, and strictures (EREFS) score after elimination of FSA-reactive foods (Figure 5.1B). Of the eighteen resolved patients with previous diagnoses of EoE who were enrolled, one was only on proton pump inhibitor therapy (PPI), five patients on topical corticosteroids (TCS), eleven patients were on diet elimination trials, and one was taking topical steroids while eliminating dairy. Mean FSA concentration was calculated and compared for active EoE patients and patients resolved upon PPI, TCS, or dietary adjustment. Treatment resolved patients had a mean eosinophil count of 1.6 (SD=2.5). Food-specific IgA was undetectable in all treatment-resolved patients (Figure 5.2A). Food-specific IgG4 was detectable in two treatment-resolved patients (Figure 5.2B). For one patient treated successfully with topical steroids, FSAs were undetectable (Figure 5.2A,B). Four patients in the resolved EoE group had undergone IgA and IgG4 testing prior to food elimination and then after dietary guided resolution of disease. One of these underwent repeated testing with only IgG4 studies to foods. After diet elimination and resolution of esophageal eosinophilia, three patients no longer demonstrated food specific antibodies in their esophageal secretions. In the third patient (for whom only IgG4 testing was performed), gluten-specific IgG4 was detectable in their esophageal secretions. Of interest, this patient admitted to consuming crackers for a several days prior to the follow-up endoscopy. In order to determine whether total immunoglobulin concentration in esophageal secretions was associated with EoE status, we performed quantitative immunoassays for IgG, IgA, IgM, and IgE. Total concentration of these immunoglobulin isotypes were not significantly associated with active EoE, treatment-resolved EoE, or control (Figure 5.3). In order to determine whether FSAs in serum or saliva could also be used to predict trigger foods for EoE, we performed IgG4 profiling for a single patient known to have EoE triggered by wheat. In esophageal secretions, only anti-wheat IgG4 was detectable (Figure |