| OCR Text |
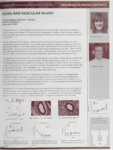
Show I THE UNIVERSITY OF UTAH HEALTH SCIENCES LEAP PROGRAM "CAN OPIOIDS INHIBIT THE SIGNALING OF PAIN AND FATIGUE BY MUSCLE AFFERENTS?" Rosa Belen Coronado, Kelsey Lila Knight (Alan R. Light, Ron Hughen) Department of Anesthesiology, School of Medicine University of Utah We are using calcium imaging to determine the effects of combinations of metabolites (the same metabolites that are produced by muscle contraction in both humans and mice) on dorsal root ganglion neurons (DRG) from mice. One of the questions is whether muscle dorsal root ganglia have functional opioid receptors expressed in sufficient quantities to decrease the metabolite signaling normally seen in muscle sensory DRG neurons that leads to muscle pain and fatigue. Methods: dorsal root ganglions (DRG) are harvested from the lumbar region of mice, previously sacrificed using isoflurane. The D R G neurons are mechanically dissociated, plated, and incubated overnight. Cells are loaded with Fura-2 acetoxymethyl ester, the dye that fluoresces when binding calcium, indicating calcium levels inside the cells. For controls, w e applied metabolites (lactate, ATP, and protons) that normally increase with muscle contractions that occur during normal exercise to each well while acquiring images. In experimental wells, w e added D A M G O , a very selective, m u opioid agonist prior to metabolites to determine its ability to block the activation of muscle sensory neurons. At the end of each metabolite series w e tested the cells with 200 nanoM capsaicin then 50 p M KCI. These applications should activate living neurons but not non-or dead neurons. (Capsaicin is a chemical that activates TRPV1 receptors that signal the burning sensation associated with hot peppers.) Conclusions: In our preliminary DAMGO experiments, the concentration of opioid agonist we used may be excessive and therefore, the results m a y not be physiologically relevant. W e observed more inhibition than expected. In addition, w e also observed greatly enhanced activation of DRG neurons by capsaicin following D A M G O administration. This increased activation cannot be explained by the known distribution of TRPV1 receptors and therefore, m a y be a nonspecific (non opioid receptor mediated) effect of D A M G O or it's vehicle. DAMGO reversibility on the responses of DRG neurons to tow pH •a-1 ?4tH '.r.pll 4 6uH.DA.MOI > -.4pH«hrr r>.vu<» 66pH*flrr (MMGO Rosa Belen Coronado Kelsey Lila Knight Ron Hughen Alan R. Light 165 |