| Title |
Ocular and Orbital Complications of Intraarterial Cisplatin |
| Creator |
Wu, HM; Lee, AG; Lehane, DE; Chi, TL; Lewis, RA |
| Affiliation |
Department of Ophthalmology, Baylor College of Medicine, Houston, Texas 77030, USA. |
| Abstract |
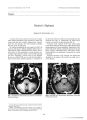
Despite advances in neurosurgery, radiation oncology, and chemotherapy, the prognosis for glioblastoma multiforme remains poor, with a median survival time of 11-12 months. Cisplatin (cis-diamminedichlorideplatinum II) is one treatment for glioblastoma multiforme. Higher response rates have been achieved by intraarterial (i.a.) infusion than by systemic infusion of this agent. Cisplatin therapy may cause neurologic complications, and i.a. delivery has been reported to cause ocular toxicity. We report a patient who experienced intraorbital and intraocular toxicity following supraophthalmic i.a. injection of cisplatin. |
| Subject |
Adult; Antineoplastic Agents/administration & dosage; Antineoplastic Agents/adverse effects; Brain Neoplasms/drug therapy; Cisplatin/administration & dosage; Cisplatin/adverse effects; Eye Diseases/chemically induced; Fatal Outcome; Female; Fluorescein Angiography; Fundus Oculi; Glioblastoma/drug therapy; Humans; Infusions, Intra-Arterial; Ophthalmoplegia/chemically induced; Optic Atrophy/chemically induced; Orbital Diseases/chemically induced; Pupil Disorders/chemically induced |
| Format |
application/pdf |
| Publication Type |
Journal Article |
| Collection |
Neuro-Ophthalmology Virtual Education Library: Journal of Neuro-Ophthalmology Archives: https://novel.utah.edu/jno/ |
| Publisher |
Lippincott, Williams & Wilkins |
| Holding Institution |
Spencer S. Eccles Health Sciences Library, University of Utah |
| Rights Management |
© North American Neuro-Ophthalmology Society |
| Setname |
ehsl_novel_jno |
| ID |
224833 |
| Reference URL |
https://collections.lib.utah.edu/ark:/87278/s6962pmg/224833 |