| OCR Text |
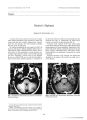
Show Journal of Neuro- Ophlhalmology 17( 3): 166- 169, 1997. © 1997 Lippincott- Raven Publishers, Philadelphia Bilateral Diffuse Uveal Melanocytic Proliferation Simulating an Arteriovenous Fistula Marjorie A. Murphy, M. D., William M. Hart Jr., M. D., Ph. D., and R. Joseph Oik, M. D. Bilateral diffuse uveal melanocytic proliferation is a rare paraneoplastic syndrome that causes visual loss in patients with systemic carcinoma. We report the case of a patient with this syndrome whose initial presentation and striking anterior segment findings mimicked that of an arteriovenous fistula. Key Words: Bilateral diffuse uveal melanocytic proliferation- Paraneoplastic syndrome- Arteriovenous fistual. Bilateral diffuse uveal melanocytic proliferation ( BDUMP) is a rare paraneoplastic syndrome that causes visual loss in patients with systemic carcinoma ( 1- 16). It is characterized by bilateral proliferation throughout the uveal tract of benign melanocytes. Clinically, the typical ocular features ( 10,13,16) include ( a) multiple round red or yellow- orange patches at the level of the retinal pigment epithelium that angiographically show a distinctive pattern of early hyperflourescence, ( b) proliferation of choroidal nevus- like lesions as well as diffuse thickening of the uveal tract, ( c) exudative retinal detachment, and ( d) rapidly developing cataracts. Additional signs that may be present include iridocyclitis ( 3- 5,13), glaucoma ( 3,5,8,12,13), dilated episceral vessels ( 3,4,12,13,16), shallow anterior chambers ( 5,8), iris and ciliary body cysts ( 4,5,8,12), and iridodonesis ( 6). Previous reports have primarily emphasized the fundus findings, both clinical and histopathologic. We report the case of a patient with BDUMP whose initial presentation and striking anterior segment findings mimicked that of an arteriovenous fistula. Manuscript received July 16,1996; accepted November 8,1996. From the Department of Ophthalmology and Visual Sciences, Washington University School of Medicine, St. Louis, Missouri, U. S. A. Address correspondence and reprint requests to Dr. William M. Hart, Jr., Department of Ophthalmology and Visual Sciences, Washington University School of Medicine, Box 8096, 660 S. Euclid Ave., St. Louis, MO, 63110- 1093, U. S. A. CASE REPORT On May 4, 1995, a 77- year- old Caucasian woman was referred to the Neuro- Ophthalmology Service at Washington University with bilateral visual loss felt to be out of proportion to her cataracts. Her past medical history was remarkable for stage 1 anaplastic uterine carcinoma diagnosed in May 1994. Her treatment had included a hysterectomy and 6 weeks of local irradiation. She also had a history of hypertension adequately controlled with medical therapy. She complained of a progressive decrease in acuity starting in February 1995. Her eyes had also been noted by her family to have become increasingly red over the previous several months. She first saw her ophthalmologist on April 5, 1995 and was found to have vision of counting fingers OU, posterior subcapsular cataracts, intra- ocular pressures of 26 OD and 14 OS, and cupping of the left greater than right optic disc. Threshold static perimetry showed marked general- 166 UVEAL MELANOCYTIC PROLIFERATION 167 ized depression in both eyes, and a head CT on April 21,1995 at an outside hospital was reportedly normal. A later review by us revealed the presence of bilateral retinal detachments. On initial examination in our office on May 4,1995, visual acuity was counting fingers in both eyes. Pupils were 4 mm and reactive to light, with a trace afferent pupillary defect in the right eye; 13/ 16 Ishihara color plates were correctly identified with the right eye and 15/ 16 with the left eye. Extraocular motility was full, and Goldmann visual fields revealed marked generalized depression with small central islands. Slit- lamp examination ( Fig. 1) showed vascular injection bilaterally with markedly dilated conjunctival and episcleral vessels, and dense posterior subcapsular as well as nuclear sclerotic cataracts. Intraocular pressures were 26 mm Hg OD and 18 mm Hg OS on Ocupress OU bid. Dilated fundus exam revealed normal- appearing optic discs with a cup- to- disc ratio of 0.4 in the right eye and 0.5 in the left eye. Bilateral inferior retinal detachments with shifting subretinal fluid were present, with no evidence of choroidal detachment or mass on B- scan. Patchy nummular reddish- orange and yellow RPE changes were also noted superiorly in areas where the retina remained attached ( Fig. 2). A bruit could neither be auscultated nor subjectively appreciated by the patient. Due to the presence of markedly dilated conjunctival and episcleral vessels with elevated intraocular pressure and exudative retinal detachments, the differential diagnosis was initially felt to include an arteriovenous fistula with secondary uveal effusion. The patient subsequently underwent a cerebral arteriogram, which was normal. The technique involved selective catheterization of the right internal and external carotid arteries, the left internal and external carotid arteries, and the vertebral artery. Biplane cervical angiography as well as intracranial angiography of all catheterized vessels were performed and revealed no evidence of a carotid cavernous fistula or dural arteriovenous malformation. The patient was seen in follow- up 10 days later ( May 15, 1995), at which time visual acuity had m . ' - Nl ''^ 9 H • jflfiH FIG. 1. External photos of the right and left eyes ( top right and top left, respectively) showing vascular injection and posterior subcapsular cataracts on retroillumination bilaterally. Marked dilation of conjunctival and episcleral vessels in both eyes is evident on higher magnification ( bottom left and bottom right). J Neuro- Ophthalmol, Vol. 17, No. 3, 1997 168 M. A. MURPHY ET AL. FIG. 2. Patchy, nummular RPE changes superiorly in an area of attached retina of the right eye. dropped to hand motions in the right eye and remained counting fingers in the left eye. Fundus exam now revealed a 1 to 2- disc- diameter, dark brown nevus- like choroidal lesion in the temporal periphery in both eyes, with no significant change in the inferior retinal detachments or RPE changes. At this point, a diagnosis of BDUMP was entertained. A fluorescein angiogram ( Fig. 3) showed a characteristic pattern of hyperfluorescent patches of choroid separated by a reticular, honeycombed network of nonfluorescence that was strikingly similar in appearance to the cases of BDUMP reported by numerous other investigators ( 4,6,8,10,11,15,16), further supporting the diagnosis. On exam 1 week later ( May 26, 1995), there were pigment cells in the anterior chamber with 1+ corneal endothelial pigment in both eyes. An extensive oncologic work- up, including MRI of the head and orbits and CT of the chest, abdomen, and pelvis, failed to reveal evidence of recurrent or new malignancy. A trial course of prednisone 80 mg qd ( or per day) was then started, with no clinical improvement after 1 month, and it was therefore tapered and discontinued. By July 24, 1995, visual acuity had dropped to light perception in both eyes, with total retinal detachments and intraocular pressures of 24 mm Hg OU. In addition, B-scan showed an enlarged superior ophthalmic vein in the right orbit, again suggestive of an arteriovenous fistula. A repeat MRI of the head and orbits was normal. The patient was NLP OU by September 18, 1995 and living at home with assistance. DISCUSSION BDUMP is a rare paraneoplastic syndrome that causes visual loss in patients with an underlying systemic carcinoma. It frequently causes visual symptoms prior to the presentation of the primary tumor, though in our patient the onset of symptoms was 9 months following the diagnosis and treatment of a stage 1 uterine carcinoma. To date, her repeat oncologic work- up has been negative. Of the 21 previously reported cases, the primary tumor, when identified, was found in lung, ovary, uterus, cervix, colon, pancreas, gallbladder, breast, and esophagus ( 1- 16). The clinical features of BDUMP are summarized in Table 1. The presence of dilated episcleral vessels and/ or conjunctival hyperemia has been noted by a number of investigators ( 3,4,12,13,16) and can be attributed to infiltration and enlargement of the ciliary body. It presents a striking anterior segment finding that may mimic an arteriovenous fistula, especially in the presence of increased intraocular pressure or a shallow anterior chamber. FIG. 3. Mid- phase frames of the fluorescein angiogram of the right eye, showing hyperfluorescent patches of choroid separated by a reticular, honey- combed network of nonfluorescence in the mid- periphery ( left) and temporal to the macula ( right). J Neuro- Ophthalmol, Vol. 17, No. 3, 1997 UVEAL MELANOCYTIC PROLIFERATION 169 TABLE 1. Ocular signs of BDUMP Anterior segment Dilated episcleral vessels Iridocyclitis Iris cysts Shallow anterior chamber Rapidly developing cataracts Glaucoma Posterior segment Multiple, round or oval, yellow- orange to red patches at level of the RPE scattered throughout posterior pole Hyperfluorescence corresponding with these patches as well as in relatively normal- appearing retina Multiple, slightly elevated choroidal nevus- like lesions Exudative retinal detachment Increased intraocular pressure has been noted in many patients with BDUMP ( 3,5,8,12,13). Possible mechanisms include outflow obstruction secondary to thickening of the ciliary body, angle closure due to swelling and forward rotation of the ciliary body, obstruction of the trabecular meshwork by melano-phages similar to melanomalytic glaucoma, goniosy-nechiae, and chronic retinal detachment. The histopathologic features of BDUMP have been well documented ( 3,5,7,9- 13,16). Macroscopi-cally, the entire uveal tract is diffusely thickened. Microscopically, the infitrate is composed of benign-appearing melanocytes with rare mitoses, though a wide spectrum of melanocytic atypia may be found. The RPE and photoreceptor layers usually show atrophy and degeneration, whereas the choriocapillaris is generally spared. The pathogenesis of BDUMP is unknown. Several investigators ( 2,13,16) have speculated that patients with BDUMP might have bilateral diffuse congenital uveal melanocytosis because only such nevus cells, unlike normal uveal melanocytes, have the ability to proliferate. They theorize that these hypopigmented melanocytic nevi are clinically silent until the systemic cancer develops and causes proliferation and melanin production through a cellular growth factor or hormone. Such a mechanism, however, does not account for the full spectrum of changes observed in BDUMP, such as cataract formation, retinal detachment, necrosis, and photoreceptor degeneration. These extramelanocytic manifestations might be caused by local toxic or immune- mediated reactions ( 13). The prerequisite for the presence of congenital diffuse uveal melanocytosis might account for the rarity of the syndrome ( 16). Although several patients with BDUMP have shown a transient improvement in the amount of retinal detachment in response to systemic corticosteroid and radiation treatment ( 9), no therapy has so far been successful in halting the progressive course of visual loss. Aggressive treatment of the systemic carcinoma offers the best hope for the patient's survival. In patients with a previous diagnosis of carcinoma who develop BDUMP, an intensive work- up should be undertaken to search for tumor recurrence or metastasis. Though our patient has shown no recurrence of cancer to date, she continues to be closely monitored. We report a patient with BDUMP and emphasize that the dilated episcleral vessels and increased intraocular pressure most often seen with arteriovenous fistulas may also be presenting signs of BDUMP, especially if associated with exudative retinal detachments, choroidal nevus- like lesions, and cataracts. In cases where the anterior segment findings are more striking and well developed than the fundus findings, imaging procedures, including cerebral arteriography, may still be necessary to exclude the diagnosis of an AV fistula, which, unlike BDUMP, has a potential for curative therapy. REFERENCES 1. Machemer R. Zur Palhogenese des flachcnhaften malignen Melanoms. Klin Monatsbl Augenheilkd 1966; 148: 641- 52. 2. Ryll DL, Campbell ARJ, Robertson DM, Brubaker SJ. Pseu-dometastatic lesions of the choroid. Ophthalmology 1980; 87: 1181- 6. 3. Barr CC, Zimmerman LE, Curtin VT, Font RL. Bilateral diffuse uveal melanocytic tumors associated with systemic malignant neoplasms. A recently recognized syndrome. Arch Ophthalmol 1982; 100: 249- 55. 4. Prusiner PE, Butler A, Yavitz EQ, Stern WH. Metastatic adenocarcinoma presenting as bilateral blindness. Ann Ophthalmol 1983; 15: 653- 6. 5. Prause JU, Jensen OA, Eisgart F, Hansen U, Kieffer M, Bilateral diffuse malignant melanoma of the uvea associated with large cell carcinoma, giant cell type, of the lung. Case report of a newly described syndrome. Ophthalmologica 1984; 189: 221- 8. 6. Mullaney J, Mooncy D, O'Connor M, McDonald GSA. Bilateral ovarian carcinoma with bilateral uveal melanoma. Br J Ophthalmol 1984; 68: 261- 7. 7. de Wolff- Rouendaal D. Bilateral diffuse benign melanocytic tumors of the uveal tract. Int Ophthalmol 1985; 7: 149- 60. 8. Tsukahara S, Wakui K, Ohzeki S. Simultaneous bilateral diffuse malignant uveal melanoma: case report with pathologic examination. Br J Ophthalmol 1986; 70: 33- 8. 9. Filipic M, Ambler JS. Bilateral diffuse melanocytic uveal tumors associated with systemic malignant neoplasm. Aust N ZJ Ophthalmol 1986; 14: 293- 9. 10. Gass JDM. Bilateral diffuse melanocytic proliferation associated with systemic carcinoma. In: Stereoscopic Atlas of Macular Disease. Vol. 1. 3rd ed. St. Louis: Mosby, 1987: 188- 9. 11. Margo CE, Pavin PR, Gendelman D, Gragoudas E. Bilateral melanocytic uveal tumors associated with non- ocular malignancy. Malignant melanomas or benign paraneoplastic syndrome? Retina 1987; 7: 137- 41. 12. Rohrbach JM. Roggendorf W, Thanos S, Steuhl KP, Thicl HJ. Simultaneous bilateral diffuse melanocytic hyperplasia. Am J Ophthalmol 1990; 110: 49- 56. 13. Gass JDM, Gieser RG, Wilkinson CP, Bcahm DE, Pautler SE. Bilateral diffuse uveal melanocytic proliferation in patients with occult carcinoma. Arch Ophthalmol 1990; 108: 527- 33. 14. Gass JDM, Glatzer RJ. Acquired pigmentation simulating Peutz- Jeghers syndrome: initial manifestation of diffuse uveal melanocytic proliferation. Br J Ophthalmol 1991; 75: 693- 5. 15. Leys AM, Dierick HG, Sciot RM. Early lesions of bilateral diffuse melanocytic proliferation. Arch Ophthalmol 1991; 109: 1590- 4. 16. Borruat FX, Othenin- Girard P, Uffer S, Othenin- Girard B, Regli F, Hurlimann J. Natural history of diffuse uveal melanocytic proliferation. Case report. Ophthalmology 1992; 99: 1698- 704. J Neuro- Ophthalmol, Vol. 17, No. 3, 1997 |