| OCR Text |
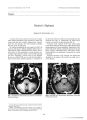
Show Journal of Neum- Oplulwlmohgy 17( 3): 207- 208, 1997. < Q 1997 Lippincoll- Ruvcn Publishers, Philadelphia Presumed Tuberculosis Presenting as a Cavernous Sinus Syndrome Shamik Bafna, M. D., and Andrew G. Lee, M. D. Cavernous sinus involvement by tuberculosis is rare. We present a 65- year- old woman with extrapulmonary tuberculosis who presented with a cavernous sinus syndrome clinically. A cervical lymph node biopsy revealed non- caseating granulomas but cultures were eventually positive for M. tuberculosis. Key Words: Tuberculosis- Cavernous sinus. CASE REPORT A 65- year- old woman presented with a 1- month history of mild pain in the right periorbital region and ptosis of the right eyelid. Past medical history was significant for noninsulin- dependent diabetes mellitus and hypertension. Results of the general physical examination were normal except for an enlarged left cervical lymph node. Ophthalmologic examination revealed a visual acuity of 20/ 400 right eye ( OD) and 20/ 30 left eye ( OS) and complete ptosis OD. The pupils measured 5 mm OD and 6.5 mm OS, with decreased light reaction OD and a brisk light reaction OS, and no afferent pupillary defect. Motility demonstrated an almost complete ophthalmoplegia ( partial adduction intact) OD and normal extraocular movement OS ( Fig. 1). Slit lamp biomicroscopic examination revealed an anterior stromal corneal scar, an old inferior posterior synechiae, and a moderate cataract OD believed to be consistent with her visual acuity. Visual fields, applanation tonometry, and fundus examination were normal both eyes ( OU). Findings on chest radiograph were normal. A serum angiotensin converting enzyme level was elevated at 88 IU ( normal, 18- 79 IU). Magnetic resonance scan of the head revealed a fullness in the right cavernous sinus in comparison with the left but no other intracranial abnormalities ( Fig. 2). A purified protein derivative test demonstrated 8 mm of induration consistent with prior tuberculosis exposure, and the patient was started on antituberculosis therapy consisting of isoniazid, rifampin, ethambutol, and pyrazinamide. The patient denied receiving the Bacillus Calmette- Guerin vaccine for tuberculosis. Manuscript received December 2, 1996; accepted March 27, 1997. From the Departments of Ophthalmology ( S. B., A. G. L.), Neurology ( A. G. L.), and Neurosurgery ( A. G. L.), Baylor College of Medicine, Houston, Texas, and the Division of Neurosurgery, University of Texas, M. D. Anderson Cancer Center, Houston, Texas ( A. G. L.) U. S. A. Address correspondence and reprint requests to Dr. A. G. Lee, Cullen Eye Institute, Baylor College of Medicine, 6501 Fannin, NC 200, Houston, TX 77030, U. S. A. Presented at the Walsh Society Meeting, Salt Lake City, Utah, February 10- 11, 1996. A left cervical lymph node biopsy was performed and revealed multiple noncaseating granulomas with epithelioid histiocytes and multinucleated giant cells ( Fig. 3). The pathologic findings were believed to be consistent with the diagnosis of sarcoidosis, and the patient was treated with 3 days of pulse dose intravenous methyl-prednisolone ( 1 g/ day) in conjunction with the antituberculosis medication. Four weeks later, tissue culture from the lymph node grew Mycobacterium tuberculosis. In addition, polymerase chain reaction detected DNA from Mycobacterium species. Approximately 6 weeks after initiating antituberculous therapy, the patient had partial resolution of her ptosis and motility deficits. A follow- up magnetic resonance scan of the head revealed resolution of the abnormal contrast enhancement within the right cavernous sinus. DISCUSSION Tuberculosis may present with extrapulmonary manifestations. In this patient, a right cavernous sinus syndrome led to the detection of a contrast- enhancing lesion within the right cavernous sinus. A cervical lymph node biopsy and tissue culture confirmed the diagnosis of extrapulmonary tuberculosis. Although a biopsy specimen was not taken from the cavernous sinus lesion, we presume that this lesion was also caused by extrapulmonary tuberculosis. The resolution of the patient's symptoms with antituberculosis therapy also supports this hypothesis, although other etiologies cannot be completely excluded. The anterior segment findings in the right eye consisting of an old anterior stromal scar, posterior synechiae, and cataract are nonspecific and may have been caused by prior trauma or inflammation. Tuberculosis is presumed to be the cause of this patient's cavernous sinus lesion. Although most pathologic studies in cases of tuberculosis reveal caseating rather than noncaseating granulomas, the demonstration of noncaseating granulomas in the cervical lymph node biopsy does not exclude the diagnosis of tuberculosis. The tuberculous granuloma may lack caseation and be indistinguishable from sarcoidosis in patients with good resistance against the tuberculous bacilli ( 1). Several reports document patients who initially were thought to have clinical sarcoidosis. Lymph node biopsies in these patients revealed noncaseating granulomas, but cultures eventually were positive for M tuberculosis ( 2,3). Therefore, the presence of noncaseating granulomas alone is 207 208 S. BAFNA AND A. G. LEE FIG. 2. Coronal MR imaging of the head demonstrating a fullness of the right cavernous sinus ( arrow). FIG. 3. Pathologic study ( x100) of cervical lymph node biopsy specimen displaying multiple noncaseating granulomas. total ophthalmoplegia of the right eye. not diagnostic for sarcoidosis. In addition, an elevated angiotensin converting enzyme level is not specific for sarcoidosis, and may be seen in tuberculosis as a measure of the total amount of granulomatous tissue in the body ( 4). In the setting of a positive finding on purified protein derivative, a tissue culture positive for M tuberculosis, and the fact that this bacteria was detected using polymerase chain reaction, tuberculosis appears to be the most likely diagnosis in this case. Ophthalmoplegia as a presenting sign of extrapulmonary tuberculosis is rare. Tuberculosis has presented as an abduction palsy secondary to a pontine tuberculoma ( 5). Mortada reported a case of tuberculosis presenting with total right ophthalmoplegia and ptosis caused by a tuberculoma of the orbital apex apex ( 6). Morris and Joyce reported a single case of tuberculosis presenting as a cavernous sinus mass ( 7). In summary, we report an unusual case of presumed extrapulmonary tuberculosis presenting as a cavernous sinus syndrome. In addition, we emphasize the importance of tissue culture for M tuberculosis, even in the presence of a noncaseating granuloma. Acknowledgment: This work was supported in part by the Baylor Neuro- ophthalmology Academic Fund. REFERENCES 1. Klech H. Sarcoidosis: differential diagnosis. Semin Resp Med 1986; 8: 72- 94. 2. Kent DC, Houk VN, Elliott RC, et al. The definitive evaluation of sarcoidosis. Am Rev Resp Dis 1970; 101: 721- 7. 3. Miyagawa Y, Mitsuyama T, Hayashi S, Nagata N, Yagawa K, Shigematsu N. A case of pulmonary tuberculosis with bilateral hilar lymphadenopathy diagnosed by sputum culture subsequent to open thoracic biopsy. Reap Med 1992; 59: 247- 249. 4. Studdy P, Bird H, James D, Sherlock S. Serum angiotensin-converting enzyme in sarcoidosis and other granulomatous disorders. Lancet 1978; 11: 1331- 4. 5. Monteiro ML, Coppeto JR. Cryptic disseminated tuberculosis presenting as a gaze palsy. J Clin Neuroophthalmol 1985; 5: 27- 9. 6. Mortada A. Orbital apex syndrome with contra- lateral hemiplegia due to tuberculoma of orbital apex. Mod Probl Ophthalmol 1975; 14: 657- 9. 7. Morris JT, Joyce MP. Central nervous system tuberculoma presenting as a cavernous sinus tumor. Clin Infect Dis 1992; 15: 181- 2. J Neum- Ophthalmol, Vol. 17, No. .?, 1997 |