| OCR Text |
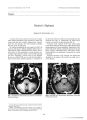
Show Journal of Neuro- Ophthalmology 17( 3): 189- 193, 1997. 1997 Lippincott- Raven Publishers, Philadelphia Acquired Supranuclear Ocular Motor Paresis Following Cardiovascular Surgery Todd R. Devere, M. D., Andrew G. Lee, M. D., M. Bowes Hamill, M. D., Dawn Bhasin, M. D., Silvia Orengo- Nania, M. D., and Joseph S. Coselli, M. D. Acquired supranuclear ocular motor paresis is a rare disorder characterized by impaired saccadic and smooth pursuit eye movements in one or more directions of gaze. Ves-tibularly induced eye movements, however, are preserved. Six adult patients developed an acquired supranuclear ocular motor paresis following cardiopulmonary bypass surgery. Neuroimaging studies were normal in two patients and were consistent with small vessel ischemia in four patients. The mean cardiopulmonary bypass time was 132.3 min, and mean circulatory arrest time was 38.7 min; these were not outside established norms for this type of surgery. Patients undergoing cardiopulmonary bypass pre-cedures with deep hypothermia are at risk for acquired supranuclear ocular motor paresis, but the development of this syndrome may not be predictable by duration of circulatory arrest or cardiopulmonary bypass times. Key Words: Ocular motor paresis- Ocular motor apraxia- Cardiopulmonary bypass. Manuscript received September 24, 1996; accepted October 9, 1996. From the Departments of Ophthalmology ( A. G. L., D. B., S. O. N., M. B. H.), Neurology ( A. G. L.), Neurosurgery ( A. G. L.), and Surgery ( J. S. C.), Baylor College of Medicine, Houston, Texas, U. S. A. Address correspondence and reprint requests to Dr. Andrew G. Lee, Department of Ophthalmology, Baylor College of Medicine, 6501 Fannin St., NC- 200, Houston, TX 77030, U. S. A. Acquired supranuclear ocular motor paresis ( ASOMP) is a rare disorder characterized by impaired volitional and reflexive saccades and often smooth pursuit in one or more directions of gaze. Patients with ASOMP have intact extraocular movements in response to vestibular stimulation ( doll's head maneuver). This differs from ocular motor apraxia, which is, strictly speaking, a disorder of initiation of voluntary saccades, with intact random and reflexive saccades ( 1,2). Although the terms are often used interchangeably, we prefer the term ASOMP when both random and voluntary saccades, as well as pursuit, are impaired. Ocular motor apraxia was originally described as a congenital form ( 3), and acquired forms of ocular motor apraxia and ASOMP have rarely been reported after lesions involving bilateral frontoparietal cortex ( 4), thalamus ( 5), or brain stem ( 6). The frontal eye fields are important in the generation of saccadic eye movements. Stimulation of the contralateral frontal eye field results in saccadic movement, and lesions involving the frontal eye fields may result in a deficiency of contralateral saccades ( 7,8). Lesions of the parietooccipital cortex and the projections to the frontal eye fields, thalamus, and superior colliculus may also affect saccadic generation ( 8,9). We describe the clinical and neuroimaging findings of six patients who developed ASOMP after cardiac surgery with deep hypothermia. CASE REPORTS Case 1 A 65- year- old black woman was admitted for shortness of breath. Pulmonary angiography confirmed a pulmonary embolism that did not resolve despite several months of anticoagulation. She underwent pulmonary thromboendarterectomy on March 29,1996. Operative findings included primary intimal sarcoma of the right pulmonary artery. The patient had no complications during surgery or hypotensive 189 190 T. R. DEVERE ET AL. episodes intraoperatively. Post- operatively, she was noted to have an " external ophthalmoplegia," and she developed a generalized seizure. Electroencephalography revealed an abnormality in the right temporal lobe. CT scan of the head on April 4,1996 revealed diffuse cerebral volume loss and moderate periventricular white matter changes consistent with small vessel ischemia. Ophthalmologic exam on April 8, 1996 revealed normal visual acuity, isocoric and reactive pupils, normal visual field testing, and mild bilateral ptosis. Slit- lamp examination, intraocular pressure measurements, and ophthalmoscopy were normal. A motility examination demonstrated global inability to generate horizontal or vertical eye movements voluntarily. No voluntary or reflex saccade could be generated in any direction. Smooth pursuit was severely impaired and markedly slow in all directions. Oculocephalic ( doll's head) movements, however, were completely intact bilaterally in horizontal and vertical planes. Bell's phenomenon ( upward deviation with forced eyelid closure) was also present bilaterally. Case 2 A 48- year- old white woman with a history of Mar-fan's Syndrome underwent surgical repair of an ascending aortic aneurysm on July 28,1994. Postoperative complications included adult respiratory distress syndrome, left arm weakness, and " ophthalmoplegia." CT scan of the head on August 4 and 11,1994 were unremarkable, and electroencephalography on August 14,1994 revealed only diffuse slowing without focal discharge. Postoperative examination notes described the patient's " inability to track with cither eye or voluntarily move her eyes." On September 9, 1994 her visual acuity was 20/ 25 bilaterally, the pupils were isocoric and normally reactive, and mild ptosis was present bilaterally. Slit- lamp examination, intraocular pressure measurements, and ophthalmoscopy were normal. A motility examination demonstrated a complete inability to generate either random or voluntary saccades or pursuit in horizontal or vertical planes. Oculocephalic movements were intact bilaterally in horizontal and vertical planes, and she demonstrated intact Bell's phenomenon bilaterally. Case 3 A 74- year- old white woman underwent a coronary artery bypass operation November 1,1995. Postoperatively, she developed an aortic arch dissecting aneurysm and underwent surgical repair on November 8, 1995. Postoperatively, the patient complained of an inability to " focus on things as well." MR scan of the head on November 27,1995 ( Fig. 1) revealed several areas of bilateral subcortical white matter abnormalities and two small areas of abnormal enhancement of the left cerebellum consistent with ischemia. Ophthalmologic exam on November 28, 1995 revealed normal visual acuity, isocoric and reactive pupils, and full visual fields. Slit- lamp examination, intraocular pressure measurements, and ophthalmoscopy were normal. A motility examination demonstrated a complete inability to generate random or voluntary sac-cades or pursuit in upgaze or horizontal gaze. Voluntary saccades and smooth pursuit were slow and hypometric, but present in down gaze. Oculocephalic movements were intact bilaterally in horizontal and vertical planes, and Bell's phenomenon was intact in both eyes. Case 4 A 59- year- old white man was found to have a large chronic dissecting ascending aortic aneurysm. He underwent right carotid endarterectomy on March 18, 1996 followed by aneurysm repair and aortic valve replacement on March 25,1996. Postoperatively, the patient noted difficulty " focusing on objects." MR scan of the head on April 10, 1996 demonstrated several punctate subcortical white matter high- signal areas in frontal, frontoparietal, and paraventricular regions, in addition to the right pons consistent with small vessel ischemia. An ophthalmologic examination on April 8, 1996 revealed normal visual acuity, isocoric and reactive pupils, and full visual fields. Slit-lamp examination, intra- ocular pressure, and ophthalmoscopy were normal. Motility testing showed extremely slow and markedly hypometric horizontal and vertical voluntary reflexive saccades. Smooth pursuit was markedly slowed, with markedly reduced gain. Oculocephalic movements were intact bilaterally in horizontal and vertical planes, and demonstrated full range of extraocular motility. FIG. 1 MR scan of the head of case 3. Note several areas of sbucortical white matter abnormalities consistent with ischemia. J Neuro- Ophthalmol, Vol. 17, No. 3, 1997 ACQUIRED SUPRANUCLEAR OCULAR MOTOR PARESIS 191 Case 5 A 56- year- old white woman with a history of ascending aortic dissecting aneurysm repair in 1985 developed aortic valve insufficiency and an ascending aortic aneurysm at the graft site, requiring surgery on March 18, 1996. Postoperatively, she developed difficulty " following objects" with her eyes. MR scan of the head on April 16, 1996 revealed nonspecific abnormalities in the subcortical white matter of the right frontal region, bilateral cerebellar hemispheres, and pons consistent with small vessel ischemia. An ophthalmologic examination on April 15, 1996 revealed normal visual acuity, pupil examination, slit-lamp examination, intraocular pressure measurements, and ophthalmoscopy. A motility examination revealed a complete inability to perform random or voluntary saccades or smooth pursuit in horizontal or vertical planes. Oculocephalic movements were intact bilaterally horizontally and vertically. Case 6 A 58- year- old white man with a history of Marfan's syndrome underwent surgical repair of a recurrent ascending aortic aneurysm, an aortic arch aneurysm, and an aortic valve replacement on May 15, 1996. His ocular history included cataract extraction, with lens implant in both eyes, and repair of a left retinal detachment and scleral buckle. He also had a stable inferiorly dislocated intraocular lens in his left eye. Upon awakening from the bypass surgery, the patient noted that he could not look right, left, up, or down. MR scan of the head on May 23, 1996 was normal. An ophthalmologic exam on May 22, 1996 revealed a visual acuity of 20/ 100 in the right eye and 20/ 200 in the left eye, which was felt to be due to intraocular lens dislocation. The left iris was irregular due to postsurgical changes, but both pupils were normally reactive. Visual field testing was normal. Slit- lamp examination revealed intraocular lens implantation in the right eye and an inferiorly dislocated intraocular lens in the left eye. Intraocular pressure and ophthalmoscopy were normal. A motility examination demonstrated an inability to voluntarily elevate, depress, or horizontally move his eyes. Voluntary and reflex saccades were unable to be performed. Oculocephalic movements were intact bilaterally in vertical and horizontal planes. This patient had mild bilateral lid retraction, but no evidence of proptosis, lid lag, or thyroid disease. DISCUSSION ASOMP has been reported after cardiac arrest ( 10), after cardiac surgery ( 11,12), in association with a cortical angioma with bifrontal and parietal lobe atrophy ( 13), and with other bilateral cerebral lesions ( 4). Robinson et al. ( 11) reported five cases of choreo-athetosis and supranuclear ophthalmoplegia in children who underwent cardiopulmonary bypass operations with deep hypothermia. All of these cases experienced at least partial resolution of symptoms over a period of weeks to months. Zackon and Noel ( 12) described two children who developed ASOMP after cardiac surgery for congenital heart anomalies. Both patients had poor saccades and diminished pursuit gain both horizontally and vertically, and neither patient had any abnormalities on CT or MR scans. Dehaene and Lammens ( 10) reported a 73- year- old woman who suffered a cardiac arrest and developed an inability to generate voluntary saccades or pursuit with impaired optokinetic nystagmus. At autopsy, the brain stem was normal, but there were bilateral lesions in the posterior part of the middle frontal gyrus and posterior parietal lobe. We report ASOMP as a complication of cardiac surgery utilizing total circulatory arrest and deep hypothermia. Cases 2- 6 underwent surgery involving the thoracic aorta, and case 1 had a pulmonary throm-boendarterectomy. Surgery in all six cases included cardiopulmonary bypass with deep hypothermia. Five patients demonstrated an inability to generate either random or voluntary saccades or pursuit in horizontal or vertical planes, and one patient ( case 3) retained some voluntary saccade and pursuit function in downgaze only. Oculocephalic movements were intact in all six patients. No other focal neurologic findings were present in four patients ( cases 3- 6). Case 1 had a seizure, and case 2 had mild left arm weakness. CT or MR scans were performed on all six patients. The imaging studies demonstrated findings consistent with small vessel ischemia in cases 1, 3, 4, and 5, but is is unknown if these abnormalities were present preoperatively. Cases 2 and 6 had normal imaging studies. None of the patients had radiographic evidence of focal cerebral infarction. Follow- up examination was performed in four of our six cases. One year follow- up on case 1 showed persistence of slow horizontal pursuit and markedly hypometric horizontal saccades, but vertical movements were normal. Case 2 presented 1 year after developing ASOMP with mild vertical diplopia, and examination revealed persistence of ocular motor paresis in vertical more than horizontal saccades, not significantly improved from her initial presentation. Case 4 was examined 2 weeks after his initial examination and was improving slightly in horizontal movements, although vertical movements remained markedly impaired. Case 6 was examined 1- 2 weeks after her initial examination and continued to demonstrate prominent gaze palsy in essentially all positions. Cases 3 and 5 had not returned for follow- up examinations at the time this case report was published. Svensson et al. ( 14) reported on 656 cases of aortic surgery using deep hypothermia with circulatory arrest. The median circulatory arrest time in these patients was 31 min, the median total cardiopulmonary bypass pump time was 126 min, and the median quantity of transfused packed red blood cells was 6 U. / Neuro- Ophthalmot, Vol. 17, No. 3, 1997 192 T. R. DEVERE ET AL. Transient or permanent stroke, defined as clinical evidence of neurologic injury, either global or hemi-paretic, occurred in 7% of patients. Predictors of stroke included circulatory arrest time of > 40 min and extended total cardiopulmonary bypass pump time. Davis et al. ( 15) reported on 60 adults who underwent surgical procedures requiring hypothermic circulatory arrest. Mean circulatory arrest time was 28.5 min, and the incidence of perioperative neurologic injury was 15%. Only intraoperative hypotension was found to be a risk factor for neurologic injury. Treasure et al. ( 16) performed an experimental study in gerbils and found neurologic dysfunction to occur after 45 min of hypothermic circulatory arrest. Possible mechanisms for neurological complications after cardiac surgery that have been proposed include embolism, hypothermia, hypotension, hypoxia, metabolic changes, and hyperglycemia ( 12). As shown in Table 1, the mean circulatory arrest time among our six patients was 38.7 min and the mean total cardiopulmonary bypass time was 132.3 min. These values are consistent with the average normal times reported in previous studies of hypothermic cardiac surgery ( 14,15). Cases 2, 5, and 6 had circulatory arrest times of > 40 min, but cases 1, 3, and 4 had times of 27, 31, and 20 min, respectively. The development of ASOMP following deep hypothermic bypass procedures may not be predictable based upon the duration of cardiopulmonary bypass pump time or circulatory arrest, and the etiology may be multifactorial. Deep hypothermia is used with cardiopulmonary bypass because it allows for longer periods of circulatory arrest by providing some protection from neurologic injury. Tabaddor et al. ( 17) reported significant declines in cerebral oxygen consumption and blood flow, with relatively stable cortical partial pressure of oxygen, in dogs with profound hypothermia. However, the utilization of deep hypothermia requires longer total bypass times because of additional minutes needed to cool and warm the patient ( 14). This may allow other complications such as microembol-ism and platelet abnormalities to occur as a consequence of longer cardiopulmonary bypass times ( 14). Hypothermia may cause hemoconcentration, increased blood viscosity, and sequestration of platelets during cooling causing necrosis throughout the brain ( 18). Coselli et al. ( 19) reported that the temperature required to achieve electrocerebral silence and a safe level of hypothermia varied from 12.8° C to 28.6° C by rectal temperature. The mean temperature during circulatory arrest in our six patients was 15.8° C, with a range of 10.9- 29° C. The role of hypothermia in ASOMP is unknown. The pathogenesis of ASOMP after cardiac surgery with deep hypothermia is not known. Each of these patients had undergone surgery that included a period of deep hypothermia. No obvious complications such as unexpected hypotension or metabolic abnormalities occurred in these six cases. Circulatory arrest and total cardiopulmonary bypass times were variable, and only three of our six patients had circulatory arrest times of > 40 min. The preservation of oculo-cephalic movements in the presence of globally impaired volitional ocular movements may result from bilateral lesions in the subcortical white matter, but this was not demonstrated in our patients by neuro-imaging studies. No other comment can be made regarding localization of the presumed lesion based upon our results. Neuroimaging studies were normal or showed small vessel ischemic changes without focal cerebral infarction. Because preoperative imaging studies were not available, it is unknown if these presumed ischemic changes were present before surgery. Although some of our patients experienced gradual and slow, but limited, improvement in their extraocular movements, others remained essentially the same. We do not have long- term follow- up of complete resolution of ASOMP in any of these patients. Ophthalmologists and cardiac surgeons should be aware of the risk of ASOMP following cardiac surgery with deep hypothermia. Further prospective study is needed to better define the etiologic risk factors and underlying pathophysiology of this disorder. Acknowledgment: This work was supported in part by a grant from Research to Prevent Blindness, Inc. TABLE 1. Cardiopulmonary bypass data Case 1 2 3 4 5 6 Average Procedure Pulmonary thromboendarterectomy AAorta repair AArch repair AAorta repair AAorta and AV repair AAorta, AArch, and AV repair Total bypass time ( min) 80 103 110 124 225 152 132.3 Circulatory arrest time ( min) 27 55 31 20 50 49 38.7 Aortic clamp time ( min) 74 N/ A 78 75 138 no 95 Transfused PRBCs ( U) 3 8 6 9 8 17 8.5 Minimum core temperature (° C) 17.0 17.5 19.8 10.9 13.9 N/ A 15.82 PRBCs, packed red blood cells; AAorta, ascending aorta; AArch, aortic arch; AV, aortic valve; N/ A, not available. J Nettro- Ophthalmol, Vol. 17, No. 3, 1997 ACQUIRED SUPRANUCLEAR OCULAR MOTOR PARESIS 193 REFERENCES 1. Cogan DG, Adams RD. A type of paralysis of conjugate gaze ( ocular motor apraxia). AMA Arch Ophthalmol 1953; 50: 434- 42. 2. Sharpe JA, Johnston JL. Ocular motor paresis versus apraxia. Ann Neurol 1989; 25: 209. 3. Cogan DG. A type of congenital motor apraxia presenting jerky head movements. Trans Am Acad Ophthalmol Otolaryngol 1952; 56: 853- 62. 4. Cogan DG. Ophthalmic manifestations of bilateral non-occipital cerebral lesions. Br J Ophthalmol 1965; 49: 281- 97. 5. Mills RP, Swanson PD. Vertical oculomotor apraxia and memory loss. Ann Neurol 1978; 4: 149- 53. 6. Zackon DH, Sharpe JA, Midbrain paresis of horizontal gaze. Ann Neurol 1984; 16: 495- 504. 7. Godoy J, Luders H, Dinner DS, et al. Versive eye movements elicited by cortical stimulation of the human brain. Neurology 1990; 40: 296- 9. 8. Schiller PH, True SD, Conway LJ. Deficits in eye movements following frontal eye- field and superior colliculus ablations. J Neurophysiol 1980; 44: 1175- 89. 9. Schlag RM, Schlag J. Eye movement- related neuronal activity in the central thalamus of the monkey. Prog Ocular Motor Res 1981: 169- 76. 10. Dehaene I, Lammens M. Acquired ocular motor apraxia. Neu-roophthalmology 1991 ; 40: 262- 9. 11. Robinson RO, Samuels M, Pohl KR. Choreic syndrome after cardiac surgery. Arch Dis Child 1988; 63: 1466- 9. 12. Zackon DH, Noel L- P. Ocular motor apraxia following cardiac surgery. Can J Ophthalmol 1991; 26: 316- 9. 13. Monaco F, Pirishi A, Sechi GP, et al. Acquired ocular motor apraxia and right- sided cortical angioma. Cortex 1980; 16: 159- 67. 14. Svensson LG, Crawford ES, Hess KR, el al. Deep hypothermia with circulatory arrest. J Thorac Cardiovasc Surg 1993; 106: 19- 28. 15. Davis EA, Gillinov AM, Cameron DE, et al. Hypothermic circulatory arrest as a surgical adjunct: a five- year experience with 60 adult patients. Ann Thorac Surg 1992; 53: 402- 7. 16. Treasure T, Naftel DC, Conger KA, et al. The effect of hypothermic circulatory arrest time on cerebral function, morphology, and biochemistry. J Thorac Cardiovasc Surg 1983; 86: 761- 70. 17. Tabaddor K, Gardner TJ, Walker AE. Cerebral circulation and metabolism at deep hypothermia. Neurology 1972; 22: 1065- 70 18. Bjork VO, Hultquist G. Contraindications to profound hypothermia in open- heart surgery. J Thorac Cardiovasc Surg 1962; 44: 1- 13. 19. Coselli JS, Crawford ES, Beall AC, et al. Determination of brain temperature for safe circulatory arrest during cardiovascular operation. Ann Thorac Surg 1988; 45: 638- 42. / Neuro- Ophthalmol, Vol. 17, No. 3, 1997 |