| OCR Text |
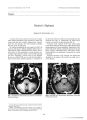
Show Journal of Neuro- Ophthalmology 17( 3): 156- 161, 1997. © 1997 Lippincott- Raven Publishers, Philadelphia Bilateral Anterior Ischemic Optic Neuropathy as a Presentation of Takayasu's Disease Matthias H. Schmidt, M. D.,* Allan J. Fox, M. D.,* and David A. Nicolle, M. B., ch. B., F. R. C. S. C, F. R. C. S. E., F. R. c. Ophth. f Takayasu's disease is an arteritis with a predilection for the proximal branches of the aortic arch. Chronic retinal hypoxic changes and ischemic ocular inflammation, resulting from cervical vascular occlusion, have been described extensively. Anterior ischemic optic neuropathy has rarely been reported in this condition, and only in conjunction with other ophthalmic findings. Here we present the case of a patient who developed bilateral anterior ischemic optic neuropathy in the absence of other eye findings, and was subsequently found to have an aortic arch syndrome compatible with Takayasu's disease. Key words: Anterior ischemic optic neuropathy- Takayasu's disease- Aortic arch syndrome- Pulseless disease. Takayasu's disease is an inflammatory condition that preferentially affects the aortic arch and its proximal branches. Involvement of the thoracic and abdominal aorta, however, also may occur. An initial inflammatory phase is characterized by fever, malaise, and elevation in erythrocyte sedimentation rate. This is followed by an obliterative phase in which involved vessels thrombose and cicatrize. Signs and symptoms of the obliterative phase are referable to end- organ ischemia. Ocular manifestations first were described by Takayasu ( 1). Classically, there is a progression of small vessel dilatation, microaneurysm formation, arteriovenous anastomosis, vitreous hemorrhage, and proliferative retinopathy ( 2). These changes are thought to be the result of chronic retinal ischemia secondary to aortic arch disease. Hypertensive retinopathy may supervene if the abdominal aorta is chiefly involved and there is renal artery stenosis ( 2- 4). There have been several recent reports of patients with Takayasu's disease exhibiting the classic ophthalmic findings ( 4- 9). Anterior ischemic optic neuropathy ( AION) has rarely been described in Takayasu's disease ( 8,9). Here, we present the case of a patient who devel- Manuscript received November 19, 1996; accepted January 13, 1997. From the * Department of Diagnostic Radiology and Nuclear Medicine, and IDepartments of Ophthalmology and Clinical Neurological Sciences, University of Western Ontario, London, Ontario, Canada. Address correspondence and reprint requests to Dr. David A. Nicolle, Department of Ophthalmology, University Hospital, 339 Windermere Road, London, Ontario, Canada, N6A 5A5. oped rapidly progressive, bilateral AION in the setting of an aortic arch syndrome most compatible with Takayasu's disease, but who did not exhibit the classic gradual funduscopic changes described earlier. CLINICAL PRESENTATION A 46- year- old white woman presented with a 3- week history of fatigue, fever, myalgia, and arthralgia. Five days before admission, she began to experience right temporal pain and jaw claudication. Over the next 4 days preceding her admission, she developed visual symptoms. Initially, she experienced blurring and gray- outin the left eye, progressing in a temporal- to- nasal direction until there was no vision in that eye. Then, overthe course of the day preceding admission, she lost vision in her right eye in a more uniform fashion. On arrivalat the hospital, she was completely blind. She had had several brief episodes of uniocular gray- out in the preceding year, and most of these had involved the left eye. Her past history was further significant for mild hypertension of 2 years' duration and right femoral angioplasty, carried out 2 years before her presentation, to relieve symptoms of claudication and night pain. She recalled that it had been difficult to measure her blood pressure in the right arm during the work- up preceding her angioplasty. She had long- standing spondylopathy and bilateral knee arthropathy. Her medications consisted of hydrochlorothiazide/ triamterene, naproxen, and quinine sulfate. She had stopped smoking one to two packs of cigarettes per day 2 years before presentation and did not drink alcohol. Her family history was significant only for the death of her father of myocardial infarct at 53 years of age. On examination, her temperature was 36.2° C, andher blood pressure was 160/ 90. Her pupils were non- reactive bilaterally, with the right being 2.5 mm and the left being 4 mm in diameter. There was no light perception in either eye. Intraocular pressure was 18 mm Hgon the right and 20 mm Hg on the left side. Findingson biomicroscopy were unremarkable. Ophthalmoscopy revealed bilateral pale, swollen disks with hemorrhages. There was a patch of ischemic retina, on the left side, extending temporally from the disk. The retinal vessels appeared normal, and no microaneurysm was seen ( Fig. 1). Extraocular move- 156 BILATERAL A10N IN TAKAYASU'S DISEASE 157 FIG. 1. Funduscopic appearance. There is bilateral pallid swelling of the disks. A: Right fundus shows a prominent hemorrhage extending nasally from the disk margin ( arrow). B: Left fundus shows a patch of ischemic retina extending temporally from the disk margin ( arrow). ment was normal in range but painful. There was no arcus senilis or xanthelasma. Head and neck examination revealed mild bilateral parotid gland swelling, mild tenderness over the right temple, and slight neck stiffness. No temporal pulse could be palpated. Other pulse deficits included both carotid pulses; right radial and ulnar pulses; and left popliteal, posterior tibial, and dorsalis pedis pulses. Bruits were perceived bilaterally over the neck and over the femoral arteries. The remainder of the cardiovascular examination was unremarkable. Chest and abdominal examination revealed no abnormality. There was no active joint and no integumentary lesion. Neurologic examination was normal with the exception of hyperalgesia involving the entire right foot. This abnormality apparently was long- standing. INVESTIGATIONS Laboratory examination yielded the following abnormal values ( normal ranges in parentheses): erythrocyte sedimentation rate 32 mm/ hour ( 0- 15 mm/ hour); creatinine 136 mmol/ L ( 62- 112 mmol/ L); serum alpha- 1- globulin fraction 3.8% ( 1.7- 3.7%); and serum aIpha- 2- globulin fraction 16.1% ( 7.0- 13.4%). Serum lipid fractionation yielded a total triglyceride concentration of 3.0 mmol/ L (> 90th percentile for age older than 40 years). Total cholesterol and all other lipid fractions were normal. Other normal or negative determinations included the following: hemoglobin, leukocyte count, platelet count, International Normalized Ratio ( INR), partial thromboplastin time, electrolytes, urea, albumin, anticardiolipin antibody, antinuclear antibody, rheumatoid factor, Total Component ( CH50), C3, C4, C- reactive protein, and Ven-eral Disease Research Laboratory. The electrocardiogram, echocardiogram, and chest x- ray showed no significant abnormality. A segment of temporal artery, obtained shortly after admission, was devoid of giant cells, inflammatory cells, or atherosclerotic change. Color Doppler examination of the orbits demonstrated flow with low resistive indices, suggestive of significant hypoxia, in the central retinal arteries on both sides ( Table 1). No convincing Doppler signal could be elicited from the left common carotid artery. Magnetic resonance ( MR) imaging of the head corroborated occlusion or near occlusion of the carotid artery in its intracavern-ous portion ( Fig. 2). Also apparent on MR imagingwere TABLE 1. Peak systolic blood flow and resistive index of arteries assessed by color doppler" Central retinal artery Right Left Normal1' Ophthalmic artery Right Left Normal" Internal carotid artery Right Left Common carotid artery Right Left Flow ( cm/ s) 12.3 6.3 13.4 ± 6.3 11.3 10.1 30.1 ± 9.9 106 Occluded 66.7 Occluded Resistive index1' 0.39 0.34 0.80 + 0.08 0.48 0.35 0.72 ± 0.05 0.27 Occluded 0.35 Occluded " Quantum 2000 ( Quantum Medical Systems, Issaqua, WA), with a 5- MHz transducer. b Resistive index = ( peak systolic flow - peak diastolic flow) + peak systolic flow. c Mean ± standard deviation in 17 normal adults, using an Acuson 128 ( Mountain View, CA) with a 7.5- MHz transducer, reported by Bull et al ( 41). J Neuro- Ophthalmol, Vol. 17. No. 3. 1997 158 M. H. SCHMIDT ET Ah. FIG. 2. Coronal T^ weighted MR scan of the head with gadolinium enhancement. There is no flow void of the left intracavernous carotid artery, suggesting occlusion or near occlusion. Right cavernous carotid flow void is normal ( arrow). small areas of signal abnormality suggestive of infarction. These were present along the gyral surface of the left parietal lobe and in the subcortical white matter of the left hemisphere, in a posterior watershed distribution. There was no signal abnormality in the right hemisphere. Angiography of the aortic arch ( Figs. 3 and 4) revealed complete occlusion of the brachiocephalic trunk with a short, abrupt stump. The left common carotid artery was occluded at the level of the sixth cervical vertebra, whereas the left vertebral artery became occluded after ascending approximately one half of a segment. The right subclavian, vertebral, and common carotid arteries were reconstituted by extensive muscular collaterals from the left and, presumably, also by collaterals ascending ipsilaterally over the thoracic cage. The left vertebral artery also was reconstituted by muscular collaterals at mid- cervical level. The left internal carotid artery received supply only from a posterior communicating collateral, filling the left anterior and middle cerebral artery territories. The left ophthalmic artery, however, was not demonstrable. TREATMENT AND OUTCOME The diagnosis of Takayasu's disease was made, and the patient was treated with intravenous methylprednis-olone at a dose of 500 mg every 12 hours. On the sixth day of admission, methylprednisolone was changed to oral prednisone at a dose of 80 mg daily for a further 6 days and to 60 mg daily thereafter. After nearly 2 weeks, there was minimal light perception in the right eye, none in the left. The disks were no longer swollen and appeared pale bilaterally. Previously noted areas of hemorrhage had resolved. Otherwise, the ophthalmologic and neurologic examination remained unchanged, and the patient was discharged home on oral prednisone. Follow- up examinations at 1 and 2 months after discharge, including repeat ocular color Doppler examination, revealed no further improvement. Retinal fluorescein angiography, performed 2 months after discharge, still showed no microaneurysm or other chronic hypoxic change. Steroids were gradually tapered over this period and then discontinued. DISCUSSION In an analysis of over 100 cases, Ross and McKusick established a classic differential diagnosis of the aortic arch syndrome. In this differential diagnosis, they included extrinsic compression, thrombotic and embolic occlusion of the great vessels arising from the aortic arch, coarctation and congenital anomalies of the aortic branching pattern, as well as aortic trauma and dissection " FIG. 3. Cerebral arterial supply demonstrated by aortic arch injection. The right internal carotid artery ( large arrow) is patent. The left internal carotid artery ( small arrow) fills only from the posterior communicating artery, supplying left anterior and middle cerebral arteries. No left ophthalmic artery is seen. The vertebrobasilar circulation fills well. J Neuro- Ophllmlmol, Vol. 17. No. 3, 1997 BILATERAL AION IN TAKAYASU'S DISEASE 159 FIG. 4. Arch aortogram. A: Early phase: The brachiocephalic trunk ( large arrow) and left common carotid artery { small arrow) are occluded. B: Later phase: There is delayed filling of the right subclavian { large curved arrow), right vertebral ( small curved arrows), and right common carotid ( large straight arrow) arteries from extensive collaterals. The left vertebral artery ( small straight arrows), occluded at its origin, is reconstituted in the mid- cervical region. ( 10). Clearly, none of these diagnoses applies to this patient. They further considered atherosclerosis and syphilitic and nonsyphilitic arteritis ( 10). Atherosclerosis is certainly a serious consideration in the aortic arch syndrome of this patient ( 11). Several risk factors were present: She had a family history of early myocardial infarction and a personal history of smoking. Her serum triglyceride level was somewhat high at presentation. However, other lipid fractions were normal, and she had no physical stigma of significant hyperlip-idemia. She was not diabetic. Her hypertension could be construed as a risk factor for atherosclerosis. On the other hand, hypertension may have been an effect, rather than a cause, of her vasculopathy. An elevated creatinine level at presentation suggests a renal etiology for the hypertension. Coincident development of hypertension and claudication 2 years before presentation implies significant involvement of renal and femoral arteries at that time. Anecdotal evidence of difficulty with blood pressure measurement during her admission for femoral angioplasty invites speculation that the process then involved upper extremity vessels as well. Such widespread large vessel involvement may certainly occur in atherosclerosis. However, occlusion of all proximal aortic branches and sparing of more distal vessels, as demonstrated by angiography, is not typical of atherosclerosis. Moreover, the laboratory findings of elevated erythrocyte sedimentation rate and alpha- 2- globulin, although not specific, point to an inflammatory process. Syphilitic aortitis, although it must certainly be considered in this context ( 12), is unlikely in view of the negative findings serologic study. Among the nonsyphilitic vasculitides, Ross and McKusick cited thromboangiitis obliterans, polyarteritis nodosa, temporal arteritis, and " young female arteritis" ( 10). Additional considerations include rheumatic and rheumatoid arteritis ( 13). Thromboangiitis obliterans and polyarteritis nodosa do not fit this patient's picture well. Thromboangiitis obliterans affects men almost exclusively. It has a distinct predilection for the lower extremities, although upper extremities may be involved. Medium and small caliber arteries are affected primarily, and venous disease in the form of thrombophlebitis is prominent ( 13- 15). Polyarteritis nodosa, similarly, is seen more frequently in men and is a disease of medium and small caliber arteries ( 13,15). Rheumatic arteritis, by definition, must be accompanied by endocarditis ( 13). Rheumatoid arteritis does affect the proximal aorta ( 13). Although spondylopathy and knee arthropathy in this patient might be consistent with rheumatoid arthritis, results of serologic study were negative. The diagnosis of temporal arteritis was entertained on the patient's admission. When temporal artery biopsy failed to confirm this diagnosis, more proximal vascular J Neuro- Ophiluilmol, Vol. 17, No. 3, 1997 160 M. H. SCHMIDT ET AL. compromise was suspected and soon was confirmed. The angiographic appearance strongly suggested the diagnosis of Takayasu's disease. Temporal arteritis is a disease of older men and women which affects primarily, but not exclusively, medium caliber cranial arteries ( 13,15), while Takayasu's disease, presumed to correspond to the " young female arteritis" of Ross and McKusick, is seen principally in younger women and affects large branches of the aorta, typically of the aortic arch ( 13,15, 16). Interestingly, temporal arteritis and Takayasu's disease, which are both characterized pathologically by arterial medial giant cell infiltration, may represent a spectrum of presentations of the same basic disease process, a more or less generalized " giant cell arteritis" ( 13,15- 17). The etiology of Takayasu's disease is still unknown. Streptococcal ( 18,19) and tuberculous ( 20) infection, as well as bacille Calmette- Guerin vaccination ( 21), have been proposed as triggers, although the association of these factors with Takayasu's disease is imperfect. Regardless of the trigger, an autoimmune etiology is favored. An association of Takayasu's disease with autoimmune disorders, such as systemic lupus erythematosus ( 22,23) and inflammatory bowel disease ( 24), has been noted. Certain human leukocyte antigens ( HLAs) are closely associated with Takayasu's disease in families with more than one affected member and are more prevalent in patients than in the general population ( 25). Indeed, the HLA haplotype Bw52- Dwl2 appears to be a predictor of active, severe disease in Japanese patients ( 26). These findings support a postulated autoimmune etiology with genetic predisposition. Anti- aorta antibodies have been identified in the serum of patients with the disease ( 27- 30), and some authors have demonstrated selective activity of these antibodies against the arterial media ( 29). It is not clear whether these antibodies are instrumental in the pathogenesis of the arteritis or are formed merely in response to vascular damage ( 30). Studies showing altered ratios of T- lymphocyte subsets and altered expression of interleukins occasionally have yielded conflicting results ( 31- 33). The most recent work suggests that infiltrating lymphocytes in patients' aortas target specific antigens ( 34) and damage vascular cells by releasing the pore- forming protein perforin ( 35). Recognition, adhesion, and cytotoxicity of these infiltrating lymphocytes may be aided, in turn, by the vascular cells themselves, which appear to express heat shock proteins, HLAs, and intercellular adhesion molecules ( 35). This patient's history clearly shows that her vasculop-athy developed over several years. The angiographic finding of multiple major vessel occlusions, which are likely to have occurred at different times over an extended period, also is in keeping with this conclusion. At the time of presentation, there was well- developed collateral circulation. Her deterioration may have resulted from a flare- up of inflammation related to Takayasu's disease, or to dehydration and prostration from an unrelated febrile illness superimposed on a chronically compromised circulation. The MR imaging finding of watershed cerebral infarction is consistent with an acute episode of hypoperfusion, but does not distinguish between the proposed etiologies. Certainly, retinal perfusion in Takayasu's disease has been shown to be exquisitely sensitive to postural changes during the inflammatory phase ( 2,9). History, physical examination, and laboratory findings again favor an active inflammatory process around the time of presentation. The rarity of AION as a presenting feature of Takayasu's disease in itself is noteworthy. Only two such cases have been described in the literature ( 8,9). More perplexing is the finding of AION in this patient without any of the classic findings attributed to chronic retinal hypoxia. Perhaps a retinal fluorescein angiogram at the time of presentation would have demonstrated microaneurysms that were not apparent by ophthalmoscopy. A later retinal angiogram showed no microaneurysm, but reversibility of this finding has been described by previous authors ( 2,7,9). Can there be long- standing, severe aortopathy, sufficient to cause extensive coUaterahzation in the head and neck region, without chronic hypoxic retinal changes? Some authors have cited a critical retinal artery systolic pressure of 30 mm Hg for the development of microaneurysms ( 2,5,7). In a study of 81 young Japanese patients with Takayasu's disease, Ish-ikawa and colleagues determined that microaneurysms or arteriovenous anastomoses were not seen until there was severe involvement of all four cervical arteries or until retinal artery systolic pressure was lower than 40 mm Hg ( 36). This patient may have fulfilled these criteria for retinal sparing until acute worsening of her ar-teriopathy led to critical ischemia. A specific mechanism for such retinal sparing is suggested by several clinical and pathologic studies that emphasize that retinal perfusion pressure depends on a balance between central retinal artery pressure and intraocular pressure ( 37- 40). Cervical artery occlusion affects anterior segment, retinal, and choroidal circulations. Compromise of the choroidal circulation, in turn, results in decreased flow to the ciliary body, decreased aqueous humor production, and lowered intraocular pressure. Despite decreased central retinal artery pressure, retinal perfusion thus may be preserved if choroidal blood supply is concomitantly diminished ( 2,7). Systemic hypertension in this patient may have augmented ocular perfusion for some time as well. In summary, Takayasu's disease is an important consideration in the differential diagnosis of an aortic arch syndrome, although it is a rare entity in the North American population, in which AION, cerebral vascular disease, and peripheral vascular disease are more commonly attributed to atherosclerosis. The classic features of this patient's history and the physical, laboratory, and imaging findings support a diagnosis of Takayasu's disease. AION is a rare presenting feature of this rare disease. This is the first report of bilateral AION as an isolated funduscopic finding in this setting. The balance among anterior segment, retinal, and choroidal circulations in J Neiiro- Ophthalmol, Vol. 17. No. 3, 1997 BILATERAL AION IN TAKAYASU'S DISEASE 161 the course of an aortic arch syndrome such as Takayasu's disease may determine the pattern of funduscopic changes that are observed. Acknowledgments: We thank Drs. Donal Downey and Donald Lee who conducted the orbital color Doppler and MR imaging examinations, respectively, and Dr. Ian Mackenzie who examined the temporal artery biopsy specimen. We also thank Mrs. Rosemary Hominick for secretarial assistance. REFERENCES 1. Takayasu M. A case with peculiar changes of the central retinal vessels. Acta Soc Ophthalmol Jpn 1908; 12: 554- 55. English translation in: Judge RD, Currier RD, Grade WA, Figley MM. Takayasu's arteritis and the aortic arch syndrome. Am J Med I962; 32: 379- 92. 2. Uyama M, Asayama K. Retinal vascular changes in Takayasu's disease ( pulseless disease): occurrence and evolution of the lesion. Doc Ophthalmol Proc Ser 1976; 9: 549- 54. 3. Nasu T. Takayasu's truncoarteritis: pulseless disease or aortitis syndrome. Acta Pathol Jpn 1982;( suppl 1) 32: 117- 31. 4. Bodker FS, Tessler HH, Shapiro MJ. Ocular complications of Takayasu's disease in a hispanic woman. Am J Ophthalmol 1993; 115: 676- 77. 5. Offret H, Foels A, Renard G. Manifestations oculaires severes au coins d'un cas de maladie de Takayashu. Bull Soc Ophthalmol Fr 1981; 81: 1171- 2. 6. Edwards KK, Lindsley HB, Lai C- W, Van Veldhuizen PJ. Takayasu arteritis presenting as retinal and vertebrobasilar ischemia. J Rheumatol 1989; 16: 1000- 2. 7. Didier T, Brasseur G, Charlin J- F, Hufault D, Langlois J. Arterite de Takayasu: evolution des signes ophtalmologiques apres greffe vasculaire. A propos d'une observation. Bull Soc Ophthalmol Fr 1986; 86: 909- 11. 8. Leonard TJK, Sanders MD. Ischaemic optic neuropathy in pulseless disease. Br J Ophthalmol 1983; 67: 389- 92. 9. Lewis JR, Glaser JS, Schatz NJ, Hutson DG. Pulseless ( Takayasu) disease with ophthalmic manifestations. J Clin Neuroophthalmol 1993; 13: 242- 9. 10. Ross RS, McKusick VA. Aortic arch syndromes: diminished or absent pulses in arteries arising from arch of aorta. Arch Intern Med 1953; 92: 701^ tO. 11. Jorens PG, Williame LM, Tombeur JP, Kockx MM, Parizel GA, Zeyen TG. Takayasu's disease and atherosclerosis. J Cardiovasc Suit- 1991; 32: 373- 5. 12. Valentin A, Karnik R, Anzbock W, Slany J. Multiple zere-brovaskulare Lasionen als letale luetische Spatfolgen. Deutsch Med Wochenschr 1991; 116: 1553- 6. 13. Oslberg G. Morphological changes in the larger arteries in polymyalgia arteritica. Acta Med Scand Suppl 1972; 533: 133- 59. 14. Emmrich R. Zur Differenlialdiagnose Arteriosclerosis obliterans Thromboangiitis obliterans. Zeitsch Gesamt Inn Med Grenzgeb 1973; 28: 389- 94. 15. Emmrich R. Zur Differenlialdiagnose der Arteriitis. Zeitsch Gesamt Inn Med Grenzgeb 1974; 29: 265- 72. 16. Hamrin B. Aortic arch syndrome. Acta Med Scand Suppl 1972; 533: 86- 99. 17. Baumann JM. Klinische Diagnose der generalisierten Riesenzell- Arteriitis. Zeitsch Klin Med 1964; 158: 22- 53. 18. Ask- Upmark E. On the " pulseless disease" outside of Japan. Acta Med Scand 1954; 149: 173- 8. 19. Maekawa M, Ishikawa K. Occlusive thromboaortopathy..//;/; Circ J 1966; 30: 79- 85. 20. Kinare SG. Aortitis in early life in India and its association with tuberculosis. J Pathol 1970; 100: 69- 76. 21. Kothari SS. Aetiopathogenesis of Takayasu's arteritis and BCG vaccination: the missing link? Med Hypotheses 1995; 45: 227- 30. 22. Igarashi T, Nagaoka S, Matsunaga K, et al. Aortitis syndrome ( Takayasu's arteritis) associated with systemic lupus erythematosus. J Rheumatol 1989; 16: 1579- 83. 23. Saxe PA, Altman RD. Aortitis syndrome ( Takayasu's arteritis) associated with SLE. J Rheumatol 1990; 17: 1251- 2. 24. Ikenaga H, Ogihara T, Iyori S, Kou S, Yoshikawa H, Okura MM. Does a common pathophysiological basis exist in the association of ulcerative colitis and Takayasu's aortitis? Report of a case. Postgrad Med J 1989; 65: 761- 4. 25. Numano F, Isohisa I, Maezawa H, Juji T. HL- A antigens in Takayasu's disease. Am Heart J 1979; 98: 153- 9. 26. Numano F, Ohta N, Sasazuki T. HLA and clinical manifestations in Takayasu disease. Jpn Circ J 1982; 46: 184- 9. 27. Ikeda M. Immunologic sludies on Takayasu's arteritis. Jpn Circ J 1966; 30: 87- 9. 28. Ito I. Aortitis syndrome with reference to detection of anti- aorta antibody from patients' sera. Jpn Circ J 1966; 30: 75- 8. 29. Ito I, Saito Y, Nonaka Y. Immunological aspects of aortitis syndrome. Jpn Circ J 1975; 39: 459- 62. 30. Nakao K, Ikeda M, Kimata S- I, et al. Takayasu's arteritis: clinical report of eighty- four cases and immunological studies of seven cases. Circulation 1967; 35: 1141- 55. 31. Alcocer- Varela J, Reyes- Lopez PA, Sanchez- Torres G, Alarcon- Segovia D. Immunologic studies in patients with Takayasu's arteritis. III. Immunoregulatory changes. Clin Exp Rheumatol 1989; 7: 345- 50. 32. Sagar S, Ganguly NK, Koicha M, Sharma BK. Immunopalhogen-esis of Takayasu arteritis. Heart Vessels Suppl 1992; 7: 85- 90. 33. Hosotani A, Uchida H, Teramoto S. Cellular immunocompetence in aortitis syndrome. Acta Med Okayama 1993; 47: 273- 80. 34. Seko Y, Sato O, Takagi A, et al. Restricted usage ol'T- cell receptor Va - Vp genes in infiltrating cells in aortic tissue of patients with Takayasu's arteritis. Circulation 1996; 93: 1788- 90. 35. Seko Y, Minota S, Kawasaki A, et al. Perforin- secreting killer cell infiltration and expression of a 65- kD heat- shock protein in aortic tissue of patients with Takayasu's arteritis. ./ Clin Invest I994; 93: 750- 8. 36. Ishikawa K, Uyama M, Asayama K. Occlusive thromboaortopathy ( Takayasu's disease): cervical arterial stenoses, retinal arterial pressure, retinal microaneurysms and prognosis. Stroke 1983; 14: 730- 5. 37. Kahn M, Knox DL, Green WR. Clinicopathologic studies of a case of aortic arch syndrome. Retina 1986; 6: 228- 33. 38. Sturrock GD, Mueller HR. Chronic ocular ischaemia. Br J Ophthalmol 1984; 68: 716- 23. 39. Hayreh SS, Podhajsky P. Ocular neovascularization with retinal vascular occlusion. II. Occurrence in central and branch retinal artery occlusion. Arch Ophthalmol 1982; 100: 1585- 96. 40. Font RL, Naumann G. Ocular hislopalhology in pulseless disease. Arch Ophthalmol 1969; 82: 784- 8. 41. Butt Z, McKilliop G, O'Brien C, Allan P, Aspinall P. Measurement of ocular blood flow velocity using colour doppler imaging in low tension glaucoma. Eye 1995; 9: 29- 33, J Neuro- Ophlhalmol, Vol. 17, No. J, 1997 |