| OCR Text |
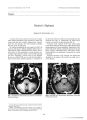
Show Journal of Nam- Ophthalmology 17( 3): 199- 201, 1997. © 1997 Lippincotl- Raven Publishers, Philadelphia Ocular Findings in Ramsay Hunt Syndrome Ahmad M. Mansour, M. D., and Byron J. Bailey, M. D. Ramsay Hunt syndrome is caused by varicella zoster virus ( VZV) infection of the geniculate ganglion of the seventh cranial nerve. Isolated case reports ( 2- 7) have mentioned neu-roophthalmic or ocular involvement in such a syndrome. Four consecutive cases with Ramsay Hunt syndrome examined by the authors and a literature review are presented to emphasize the polyneuropathic character of the syndrome. MATERIALS AND METHODS A computer- generated list of patients with Ramsay Hunt syndrome examined at the University of Texas Medical Branch was generated. Three patients had already had ophthalmic examination soon after diagnosis of the syndrome. These three patients were called for a follow- up examination, and an additional patient had an initial eye examination. CASE REPORTS Case 1 This 58- year- old black woman experienced right-sided otalgia and facial pain 10 days prior to admission. She experienced drooping of the right lips and visual loss in the right eye 1 day prior to admission. An audiogram revealed mild right sensorineural hearing loss and a decreased right acoustic reflex. The right facial compound active potential was 91% of that on the left side. Magnetic resonance imaging ( MRI) findings in the brain were unremarkable. She was started on intravenous acyclovir ( 650 mg three times daily) and oral prednisone. Best corrected visual acuities were hand motion in the right eye and 20/ 20 in the left eye. There was 5- mm exposure upon forced right eyelid closure. The right fundus had a pale disc, a cherry- red spot in the macula, and a pale retina in the posterior pole. There was poor filling and marked delay in both the choroidal and the retinal Manuscript received July 15, 1996. From the Departments of Ophthalmology ( A. M. M.) and Otolaryngology ( B. J. B.), University of Texas Medical Branch, Galveston, Texas, U. S. A. Address correspondence and reprint requests to Dr. A. Mansour, Department of Ophthalmology, American University of Beirut, Beirut, Lebanon. vascular filling by fluorescein angiography. Erythrocyte sedimentation rate and the results of rapid plasma reagent test, fluorescent treponemal antibody absorption test, carotid Doppler, and echocardiographic studies were within normal limits. Ophthalmic artery obstruction was diagnosed. Indirect fluorescent antibodies to VZV were 1: 2,048 on admission and 1: 1,024 four weeks later. There was optic disc pallor and attenuation of the retina and its vasculature in the right eye without visual improvement after 1 month of follow- up. Case 2 This 56- year- old black woman presented with right ear pain of 3 weeks' duration and a right facial droop with nausea and vertigo of few days' duration. Her medical history included positive antinuclear antibody titer, elevated sedimentation rate, and polyarthralgias. Examination revealed vesicular lesions in the right pinna and right facial palsy. She was placed on oral acyclovir ( 400 mg five times daily) and oral prednisone. Over the subsequent 2 weeks, she became increasingly tremulous and developed postural imbalance. She had an ataxic speech with broken sentences, mild rotary nystagmus, right hearing loss, and an unsteady wide- based gait, with falling to the right. Results of head computed tomography and MRI, cerebrospinal fluid chemistry and Venereal Disease Research Laboratory tests, as well as serum an-giotensin- converting enzyme, were within normal limits. Ophthalmologic consultation was then requested because she had been seeing rainbows in her right eye for 3 weeks. The patient had 3- mm exposure on eyelid closure on the right side. Intraocular tension was 40 mm Hg in the right eye ( cup- disc ratio, 0.8) and 16 mm Hg in the left eye ( cup- disc ratio, 0.6), with normal gonioscopic findings bilaterally and absence of anterior segment inflammation. The intraocular pressure was temporarily controlled by topical pilocarpine in the right eye. Her case had been followed thereafter for several years, with a normal range of intraocular pressure on no ocular medications. Case 3 This 29- year- old white woman with AIDS experienced severe left otalgia of 3 days' duration. Physical examination revealed a severely tender auricle without lesions. The admitting diagnosis was perichondritis, and she was started on intravenous ciprofloxacin and Cleocin. 199 200 A. M. MANSOUR AND B. J. BAILEY The T- helper cell count was markedly low ( 2 T- helper cells/ mm3). There was minimal improvement in symptomatology and, 1 week later, tender erythematous ve-siculopustular lesions appeared throughout the left auricle, extending down into the conchal bowl. She was placed on intravenous acyclovir ( 800 mg five times daily). Audiogram revealed no hearing loss bilaterally. Urine culture was positive for cytomegalovirus. Ophthalmologic examination revealed peripheral retinitis with active whitish granular borders temporally in the left eye consistent with cytomegalovirus retinitis. The patient was stated on intravenous ganciclovir. One month later, the auricular lesions were still present but the ear pain had subsided. The retinal lesions healed after 3 months of ganciclovir therapy. Case 4 This 32- year- old white man seropositive for HIV presented with nausea, dizziness, and a nonpainful skin eruption behind the right ear accompanied by tingling. Physical examination revealed crusted vesicles behind the right auricle, in the auricle, and bordering on the canal. Neurologic examination revealed a rotary nystagmus increasing on left gaze, a right- sided facial palsy, and a moderate mixed hearing loss on the right side. Tzanck preparation of the crust base showed inflammatory cells and necrotic debris, but no multinucleated cells. There was mild depression of the T- helper cell count ( T- helper cell count, 323/ mm3). Head computed tomography and MRI were nonrevealing. The patient was placed on acyclovir ( 800 mg five times daily), with subsequent resolution of the auricular lesions. Ophthalmologic examination 1 year after admission revealed 1 mm of right lagophthalmos with resolved facial palsy, and normal fundi. DISCUSSION Since the first description of the syndrome in 1906 ( 1), many cases ( 2- 7) and clinical series have been reported in the otolaryngologic and neurologic literature. Patients with Ramsay Hunt syndrome accounted for 1/ 1,000 of new patients attending an otolaryngology clinic ( 8) and between 0.3% and 18% of facial palsy series ( 9). Ramsay Hunt syndrome results from infection of the gasserian ganglion by VZV as demonstrated by a typical skin rash, a change in acute and convalescent serum titers for VZV, and immunofluorescent techniques ( 10). VZV remains latent in ganglia after primary exposure in childhood, and reactivation occurs in elderly or immunosuppressed subjects and uncommonly in young healthy subjects. Two cases seropositive for HIV have been reported with Ramsay Hunt syndrome ( 6,11). Two patients in the present series were younger than age 40, and both were seropositive for HIV. Young patients with zoster reactivation need to be worked up for a defect in cellular immunity ( 12). James Ramsay Hunt divided the syndrome into four categories: ( a) isolated zoster oticus ( as in case 3) ( Fig. 1); ( b) zoster oticus and facial palsy; ( c) zoster oticus, ^ ^ ^ 1 2 ' \ \ 1. HELIX \ ^) 2. ANTIHELIX %^ J ^ 3 3. LOBULE 4. EXTERNAL AUDITORY MEATUS 5. " ZOSTER ZONE" FIG. 1. Schematic distribution of auricular zoster lesions. facial palsy, and hearing loss; and ( d) zoster oticus, facial palsy, hearing loss, and disturbance of labyrinthine function ( as in cases 1, 2, and 4). After the facial nerve, the cranial nerves involved in the syndrome are in decreasing order: the eighth, the ninth, the fifth, the tenth, the ocular motor nerves, and the optic nerve ( 2). Cranial nerve palsies in Ramsay Hunt syndrome carry a generally favorable prognosis ( 3), though the facial palsy in Ramsay Hunt syndrome is more severe than in Bell ( herpes simplex) palsy ( 13). While two- thirds of patients with VZV ophthalmicus have ocular findings, the ocular findings in Ramsay Hunt syndrome have been scarce. Abducens nerve ( three cases) ( 3,5), trochlear nerve ( two cases) ( 4,5), and oculomotor nerve ( one case) ( 4) palsies have been reported. One case of oculosympathetic paralysis in Ramsay Hunt syndrome was thought to result from inflammatory involvement of the caroticotympanic fibers as they course through the middle ear toward the orbit ( 7). Acute retinal necrosis ( 6), uveitis ( 2), and retrobulbar optic neuropathy ( 4) were reported in one case each. Acute retinal necrosis has been attributed to direct infection of the retina by VZV, while the retrobulbar optic neuropathy to a demy-elinative process view its transient course. Case 1 had ophthalmic artery obstruction without signs of carotid disease, heart disease, or temporal arteritis. The temporal sequence and ipsilaterality to the side of zoster oticus also favor a zoster- induced arteritis in case 1. Segmental arteritis has been demonstrated histo-pathologically in the central nervous system and in the eye ( 14- 16). Acute ipsilateral glaucoma, as in case 2, J Neitro- Ophthalnwl, Vol. 17, No. 3, 1997 OCULAR FINDINGS IN RAMSAY HUNT SYNDROME 201 may complicate herpes zoster ophthalmicus ( 17,18) and is though to be a sequela of anterior segment inflammation probably of a vasooclusive character. Ramsay Hunt syndrome appears to be a cranial polyneuropathy presenting as zoster oticus, facial palsy, and auditory and labyrinthine symptoms, in addition to ocular involvement. The optic nerve and the ocular motor nerves are often involved because of their proximity to the facial nerve. Young patients with Ramsay Hunt syndrome need to be worked up for a defect in cellular immunity. REFERENCES 1. Hunt JR. On herpetic inflammation of the geniculate ganglion: a new syndrome and its complications. J Nerv Merit Dis 1907; 34: 73- 96. 2. Aviel A, Marshak G. Ramsay Hunt syndrome: a cranial polyneuropathy. Am J Otolaryngol 1982; 3: 61- 6. 3. Heathfiekl KWG, Mee AS. Prognosis of the Ramsay Hunt syndrome. BMJ 1978; 1: 343- 4. 4. Carroll WM, Mastaglia FL. Optic neuropathy and ophthalmoplegia in herpes zoster oticus. Neurology 1979; 29: 726- 9. 5. Keane JR. Delayed trochlear nerve palsy in a case of zoster oticus. Arch Ophthalmol 1975; 93: 382- 3. 6. Yeo JH, Pepose JS, Stewart JA, Sternberg P Jr, Liss RA. Acute retinal necrosis syndrome following herpes zoster dermatitis. Ophthalmology 1986; 93: 1418- 22. 7. Jarrett WH. Horner's syndrome with geniculate zoster occurring in association with trigeminal herpes in which the ophthalmic division was spared. Am J Ophthalmol 1967; 63: 326- 30. 8. Devriese PP. Facial paralysis in cephalic herpes zoster. Ann Otol Rhinol Laryngol 1968; 77: 1101- 19. 9. Mair IWS, Birkland Flugsrud L. Peripheral facial palsy and herpes zoster infection. J Laryngol Otol 1976; 90: 373- 9. 10. Fujiwara Y, Yanagihara N, Kurata T. Middle ear mucosa in Ramsay Hunt syndrome. Ann Otol Rhinol Laryngol 1990; 99: 359- 62. 11. Mishell JH, Applebaum EL. Ramsay- Hunt syndrome in a patient with HIV infection. Otolaryngol Head Neck Surg 1990; 102: 177- 9. 12. Cole EL, Meisler DM, Calabrese LH, Holland GN, Mondino BJ, Conant MA. Herpes zoster ophthalmicus and acquired immune deficiency syndrome. Arch Ophthalmol 1984; 102: 1027- 9. 13. Robillard RB, Hilsinger RL, Adour KK. Ramsay Hunt facial paralysis: clinical analyses of 185 patients. Otolaryngol Head Neck Surg 1986; 95: 292- 7. 14. Linnemann CC Jr, Alvira MM. Pathogenesis of varicella- zoster angiitis in the CNS. Arch Neurol 1980; 37: 239- 40. 15. Naumann G, Gass JDM, Font RL. Histopathology of herpes zoster ophthalmicus. Am J Ophthalmol 1968; 65: 533- 41. 16. Culbertson WW, Blumenkranz MS, Pepose JS, Stewart J A, Curtin VT. Varicella zoster virus is a cause of the acute retinal necrosis syndrome. Ophthalmology 1986; 93: 559- 69. 17. Edgerton AE. Herpes zoster ophthalmicus: report of cases and review of the literature. Arch Ophthalmol 1945; 34: 40- 62, 114- 53. 18. Womack LW, Liesegang TJ. Complications of herpes zoster ophthalmicus. Arch Ophthalmol 1983; 101: 42- 5. J Neuro- Ophthalmol, Vol. 17, No. 3, 1997 |