| OCR Text |
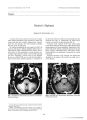
Show Journal of Neuw- Ophthulmolosy 17( 3): 183- 188, 1997. © 1997 Lippincoll- Ravcn Publishers, Philadelphia Neuro- Ophthalmologic Manifestations of Adenoid Cystic Carcinoma Andrew G. Lee, M. D., Paul H. Phillips, M. D., Nancy J. Newman, M. D., L. Anne Hayman, M. D., Jade S. Schiffman, M. D., Scott E. Segal, M. D., Hering J. Nauta, M. D., Mitchell J. Wolin, M. D., and Rosa A. Tang, M. D., M. P. H. Intracranial adenoid cystic carcinoma is uncommon. We report two unusual cases of intracranial adenoid cystic carcinoma. The first patient presented with a steroid- responsive optic neuropathy from an orbital mass that simulated orbital pseudotumor, and subsequently developed intracranial involvement, presumably by contiguous perineural spread. The second patient presented with proptosis of the left eye, right facial weakness and numbness, and an intracranial mass, presumably from hematogenous metastatic spread. Key Words: Adenoid cystic carcinoma- intracranial. Adenoid cystic carcinoma ( ACC) arises most frequently from the salivary, lacrimal, and other exocrine glands ( 1,2) and may be locally invasive. There are few reports, however, of intracranial ACC ( 3- 12). We report the clinical and neuroradiologic findings in two unusual cases and review the literature on intracranial ACC ( 3 - 12). CASE REPORTS Case 1 A 36- year- old pregnant white woman complained of a 2- month history of right facial pain, intermittent numbness of the right cheek, and diffuse, moderately severe headaches. Her symptoms began in March 1995, at the end of her first trimester of pregnancy. In April 1995, she Manuscript received December 19, 1996; accepted March 31, 1997. From the Departments of Ophthalmology, Neurology, and Neurosurgery ( A. G. L.) and the Department of Radiology, ( L. A. H.), Baylor College of Medicine, Houston, Texas; the Departments of Ophthalmology ( N. J. N., P. H. P.), Neurology ( N. J. N.), and Neurosurgery ( N. J. N.), Emory University School of Medicine, Atlanta, Georgia; University of Miami School of Medicine ( J. S. S.), Miami, Florida; the Anderson Eye and Ear Associates ( M. J. W.), Anderson, South Carolina; and the Departments of Ophthalmology and Neurosurgery ( R. A. T, H. J. N.), University of Texas Medical Branch at Galveston, Houston, Texas and the Division of Neurosurgery, University of Texas, M. D. Anderson Cancer Center, Houston, Texas, U. S. A. Address correspondence and reprint requests to Dr. A. G. Lee, Cullen Eye Institute, Baylor College of Medicine, 6501 Fannin, NC 200, Houston, TX 77030, U. S. A. Presented in part at the Frank B. Walsh Society Meeting, Salt Lake City, Utah, February 11, 1996. noted decreased vision in the inferior field of her right eye associated with a pressure sensation behind the right eye. Her past medical, surgical, and social history were noncontributory. A general medical, neurologic, and otolaryngologic evaluation were unremarkable. Results from a computed tomography ( CT) scan of the head, without contrast, on June 15, 1995, were normal. She then noted progressive loss of visual acuity, increasing proptosis, and retrobulbar pain of the right eye. She was seen by an ophthalmologist on July 7, 1995, and had a visual acuity of counting fingers in the right eye and 20/ 20 in the left eye. There was a relative afferent pupillary defect and 4 mm of proptosis in the right eye. Ophthalmoscopic study revealed mild disc edema in the right eye. A magnetic resonance ( MR) scan of the head and orbits without contrast showed a nonspecific soft tissue mass in the right orbital apex, extending posteriorly into the cavernous sinus with enlargement of the extraocular muscles in the right orbital apex ( Fig. I). The lacrimal glands were felt to be normal clinically, and appeared normal on the MR scan of the orbit. She was treated with an empiric trial of oral prednisone ( 60 mg per day) for the presumed diagnosis of pseudotumor of the orbit. One week after treatment with oral steroids, she experienced a dramatic improvement in visual acuity in the right eye to 20/ 40, the proptosis of the right eye had decreased by 1 mm, and the visual field defect had improved in the right eye. On July 20, 1995, the patient reported improvement in her headache and visual function, and the prednisone dosage subsequently was reduced to 40 mg per day. On August 16, 1995, the visual acuity measured 20/ 60 in the right eye, and the oral prednisone dosage was increased to 60 mg per day, alternating with 30 mg per day. Neuro- ophthalmologic examination on August 23, 1995, revealed a visual acuity of 20/ 60 in the right eye and 20/ 20 in the left eye. Hertel exophthalmometer measurements were 26 mm in the right eye and 22 mm in the left eye. The right pupil reacted sluggishly to light, and there was a right relative afferent pupillary defect. Gold-mann perimetry revealed a relative inferior nerve fiber bundle- related defect involving central fixation to the 183 184 A. G. LEEETAL. FIG. 1. Case 1. Axial T1 - weighted MR image without contrast of the orbit reveals an isointense mass in the right orbital apex ( arrow). I4e and III4e stimuli in the right eye and a normal visual field in the left eye. Results of slit lamp biomicroscopy, intraocular pressure measurements, and ocular motility examination were normal in each eye. Ophthalmoscopic study revealed mild right optic disc swelling. Findings on corneal reflex testing were normal in each eye. Sensation in the cutaneous distribution of the second division of the trigeminal nerve was decreased on the right. A second MR scan of the head and orbits, without contrast, on September 1, 1995, revealed an increase in the size of the soft tissue mass at the right orbital apex ( Fig. 2) and involvement of the pterygopalatine fissure and skull FIG. 2. Case 1. Axial T2- weighted MR image shows hyperin-tense signal intensity in the right orbital apex ( arrow) and along the right posterior optic nerve sheath. FIG. 3. Case 1. Histopathologic examination of the lesion reveals aggregates or islands of poorly differentiated, small, tightly packed epithelial cells that are outlined sharply against the surrounding hyaline- like stroma, consistent with adenoid cystic carcinoma. base. On September 6, 1995, the visual acuity was counting fingers in the right eye with worsening of the visual field defect in the right eye. A third MR scan, without contrast, revealed slight enlargement of the right orbital apex mass. At 37 weeks' gestation, she underwent an induced vaginal delivery without complication. The following day, she underwent a right frontal craniotomy. At the time of surgery, an irregular tan and pink soft tissue mass involving the meninges of the lesser wing of the sphenoid and the right optic canal was encountered. The margin of the lesion could not be grossly identified, and the mass seemed to infiltrate the meninges of the cavernous sinus and superior orbital fissure, as well as the greater wing of the sphenoid bone. The right optic nerve was decompressed by removing the roof of the optic canal, and the optic nerve appeared grossly normal. Histopathologic examination of the mass revealed ACC ( Fig. 3). No ectopic lacrimal gland tissue was seen. An extensive otolaryngologic and general medical examination failed to uncover a primary tumor site or other metastatic lesions. Results of a chest radiograph and bone scan were normal. A biopsy of the right lacrimal gland did not reveal any evidence of ACC. The patient underwent fractionated radiation therapy consisting of 6300 cGy over 5 weeks to the right sphenoid wing and posterior orbit. Examination on January 24, 1996, revealed a visual acuity of 20/ 30, a small paracentral scotoma to the I4e stimulus on Goldmann perimetry, and optic atrophy in the right eye. MR imaging revealed postoperative changes in the right orbital apex from the previous craniotomy. The lesion in the pterygopalatine fossa was better demonstrated after the administration of contrast material ( Fig. 4). Case 2 A 32- year- old Hispanic man presented with a 2- month history of increasing " fullness" of the left upper lid and ./ Neuro- Ophlhalmol. Vol. 17, No. 3, 1997 NEURO- OPHTHALMOLOGIC MANIFESTATIONS OF ACC 185 FIG. 4. Case 1. Axial T1 - weighted MR image demonstrates contrast enhancement of lesion on the right side ( arrow) in the area of the pterygopalatine fossa. proptosis of the left eye. He was treated by his local physician with topical antibiotic drops without relief of symptoms. One month before referral, he developed decreased vision in the left eye, binocular vertical diplopia in upgaze, mild weakness of the right face, and numbness in the left hand. His past medical history was unremarkable. Neuro- ophthalmologic examination revealed a visual acuity of 20/ 20 in the right eye and 20/ 30 in the left eye. There was a palpable fullness in the left upper eyelid, left infraplacement of the globe, 3 mm of left- sided proptosis, and decreased retropulsion in the left eye. The pupils were of equal size, and there was no relative afferent pupillary defect. Ocular motility examination revealed full movement of the right eye, but the left eye had limited elevation ( Fig. 5). Visual fields performed by Goldmann perimetry were normal in each eye. Ophthalmoscopic study revealed choroidal folds superiorly in the left eye. The remainder of the findings from retinal and optic nerve examination in each eye was normal. Neurologic examination revealed decreased sensation in the cutaneous distribution of the first and second divisions of the trigeminal nerve on the right side, a right peripheral seventh cranial nerve paresis, mild weakness and decreased sensation to light touch of the left upper and lower extremities, and agraphesthesia of the left hand. General physical examination revealed mild tenderness over the right mandibular angle and an enlarged, non-tender right cervical lymph node. MR scan of the brain and orbits revealed a left superior orbital mass with intracranial extension ( Fig. 6), and a 4- cm extraaxial mass in the right parietal region with surrounding meningeal enhancement. There was mini- < 5- FIG. 5. Case 2. Motility photographs demonstrate full movement of the right eye, but the left eye was limited in elevation. J Neum- Ophlhalmol, Vol. 17, No. 3, 1997 186 A. G. LEEETAL. FIG. 6. Case 2. Coronal T1- weighted MR image demonstrates slightly hypointense abnormal signal intensity in the left superior orbit with erosion of the orbital roof and intracranial extension. mal surrounding tissue edema, mass effect, or midline shift. A second mass was identified in the left superior orbital ridge compressing the superior portion of the left globe. CT of the brain and orbits revealed a lytic bone lesion in the right calvarium adjacent to the right parietal mass ( Fig. 7), a lytic bone lesion in the right mandibular angle, and a superior orbital mass with adjacent orbital bone destruction. CT of the chest, abdomen, and pelvis yielded normal results. A bone survey revealed the lytic bone lesions in the right calvarium and right mandibular angle, and a bone scan revealed increased uptake in the left orbit, right mandible, and midline of the skull. Biopsy of the right parietal mass revealed ACC. The patient was treated with palliative radiation and chemotherapy, but he developed metastatic lesions of the cervical and sacral vertebrae. DISCUSSION Adenoid cystic carcinoma most commonly arises from the major and minor salivary glands, and the mucous glands of the upper respiratory tract ( 1- 23). In the orbit, ACC usually arises from the lacrimal gland. Less commonly, ACC may develop from the cerumen glands of the external auditory canal, ectopic lacrimal gland tissue, and other organs such as breast, bronchus, intestine, pancreas, vulva, sweat glands, or genital organs ( 3,5,11,17). ACC usually grows slowly over many years, with progressive local extension and multiple local recurrences ( 17,21). Metastatic disease is a late finding and usually involves the lungs, but also may involve bone, liver, regional lymph nodes of the head and neck, and rarely, brain ( 5). Nevertheless, patients may continue to live for several years despite the development of metastases ( 7). The overall 5- year survival rate for all ACC is about 47%, and the 15- year survival rate is about 10% to 22% ( 7). The median age of patients with ACC is 38 years, with an equal incidence in male and female patients. ACC of the head and neck usually presents with a local mass or swelling with or without pain ( 2). Patients with orbital ACC may have proptosis, orbital pain, diplopia, or visual loss, depending on the location and infiltrating character of the tumor ( 2). Intracranial extension of ACC may occur in 4% to 22% of cases ( 3- 12,18,20). Most of these cases invade the skull base and are thought to extend directly or by perineural spread from lesions in adjacent structures, such as the lacrimal glands, salivary glands, paranasal sinuses, or from the nasopharynx ( 3- 12,18,20). Hematogenous metastasis to the brain are rare ( 4,5,24- 26). In Case 1, there was no clinical or radiologic evidence of a primary orbital or ectopic lacrimal gland origin of the ACC, and a lacrimal gland biopsy revealed no evidence of ACC. There was involvement of the pterygopalatine fissure on the initial imaging studies, suggesting that the tumor originated from minor salivary glands within the pterygopalatine fossa. An extensive general medical evaluation failed to disclose another primary tumor site or metastatic lesions. The intraorbital and intracranial tumor likely occurred through perineural or contiguous spread from the pterygopalatine fossa. The pterygopalatine fossa is located directly posterior to the maxillary sinus and is in communication with the orbit through the inferior and superior orbital fissures, as well as the cranium through the foramen rotundum. The maxillary division of the trigeminal nerve travels through the pterygopalatine fossa, and it is likely that involvement of this nerve in this location was the source of the intermittent numbness of the cheek experienced by this patient ( Fig. 8). Contiguous spread of tumor from the pterygopalatine fossa to the orbit has been reported ( 27- 29). FIG. 7. Case 2. Coronal CT scan of the head demonstrates a slightly hyperdense lesion in the right parietal region with erosion of the skull. J Neiiro- Oplilluilmol, Vol. 17, No. 3, 1997 NEURO- OPHTHALMOLOGIC MANIFESTATIONS OF ACC 187 I'll llAOROITAL FlSSUflf WAXILLAHT H. S. HFATER PETROSAL N inFTnenBirAi, u, S^ H¥ f. T\ KT\ C3 ' \ DLbP PETROSAL N PTFR^ COPMATlUti GANGLION in PTEHTOOP^ LATIrtE HOSSft SAGITTAL VIEW OF EEEUL. ORBIT^ L WALL FIG. 8. Schematic sagittal view of the infraorbital nerve and pterygopalatine fossa. ( Reproduced with permission from Wolin MJ. Neuro- ophthalmic manifestations of paranasal sinus disease. Ophthalmol Clin North Am 1991; 4: 585- 603.) Peipmeier and others reported on a patient with an intracranial ACC with involvement of the orbit, extraocular muscles, and optic nerve ( 10). These authors believed that the intracranial and intraorbital tumor was from perineural invasion of the trigeminal nerve ( 10). Our patient had symptoms of an ipsilateral trigeminal neuropathy and may have likewise experienced perineural trigeminal invasion. In Case 2, the left lacrimal gland is the most likely primary site. However, the right salivary glands may have been an alternative primary site, since this patient had a right CN VII palsy and a lytic lesion in the right mandibular angle. Although this patient had no discrete mass on neuroimaging of this region suggestive of a primary site, Cummings described two cases of ACC in which local signs occurred 4 to 6 years before the development of a clinically detectable parotid mass ( 24). Our patient in Case 2 likely had intracranial involvement from hematogenous metastatic spread, since the intracranial mass was anatomically isolated and on the opposite side of the orbital mass. Hematogenous metastases to the brain are rare ( 4,5,24- 26). Gelber and coworkers ( 25) described a patient with ACC of the right parotid gland with a histologically confirmed metastatic lesion to the inner table of the left frontal calvaria, epidural compartment, and brain parenchyma. Variakojis and associates ( 26) described a patient with ACC arising in the right submaxillary salivary gland with a metastatic lesion to the left frontoparietal region of the skull, which invaded the underlying dura and brain. Hara and colleagues ( 4) reported on a patient with an isolated ACC of the frontal lobe from an unknown primary site. These metastatic CNS lesions occurred in anatomic positions inconsistent with direct or retrograde perineural spread from the primary site. Intracranial ACC usually appears on CT as a well-demarcated, hyperdense, extraaxial mass that shows homogeneous enhancement after contrast administration ( 4, 6,9,11). The features of intracranial ACC seen on MR imaging include isointense signal intensity on Tl-weighted images, hyperintense signal intensity on T2- weighted images, and homogeneous enhancement after the administration of gadolinium- DTPA. Morioka and others reported linear meningeal thickening and enhancement adjacent to an intracranial ACC similar to the " dural tail" seen more commonly in meningiomas ( 9). The natural history of ACC seems to be a prolonged course with local recurrences and variable metastatic disease. Treatment regimens include chemotherapy, radiation therapy, and surgical excision. Radical complete surgical excision, when possible at the time of initial diagnosis, seems to be the best treatment option, but often is not feasible because of infiltrative involvement of contiguous vital structures ( 1,2,12,17,20). ACC is radiosensitive but not radiocurable ( 7,9,11,12,15,18,20). Chemotherapy has been tried for ACC, but with limited success, presumably secondary to the slow growth rate of these tumors ( 2,11,19,20). Gormley and colleagues ( 12) presented 16 cases of ACC with cranial base and intracranial extension. These authors focused on neurosurgical treatment and recommended the following: ( 1) preliminary cerebral revascularization with cervical carotid to middle cerebral artery bypass in cases with carotid artery involvement; ( 2) as complete as possible removal of tumor from the cavernous sinus with attempts to preserve the ocular motor cranial nerves; ( 3) orbital exenteration in cases with intraconal involvement; and ( 4) consideration for palliative surgery even in cases where local disease precludes surgical cure. The dramatic response to steroid therapy in Case 1 suggested the erroneous diagnosis of orbital pseudotumor, but the transient numbness of the cheek and intracranial extension of the tumor were atypical features that prompted biopsy. ACC should be considered in the differential diagnoses of painful, steroid- responsive optic neuropathies and of intraorbital as well as intracranial masses. Acknowledgment: This work was supported in part by an unrestricted grant from Research to Prevent Blindness. REFERENCES 1. Conley J, Dingman DL. Adenoid cystic carcinoma in the head and neck ( cylindroma). Arch Otolaryngol 1974; 100: 81- 90. 2. Eby LS, Johnson DS, Baker HW. Adenoid cystic carcinoma of the head and neck. Cancer I972; 29: l 160- 8. 3. Fortuna A, Gambacorta D. Cylindroma in the region of the Gas-serian ganglion: case report. J Neurosurg 1971; 34: 427- 31. 4. Hara H, Tanaka Y, Tsuji T, Momose G, Kobayashi S. Intracranial adenoid cystic carcinoma: a case report. Ada Ncitrochlr ( Wieti) 1983; 69: 291- 5. 5. Roller M, Ram Z, Findler G, Lipshitz M. Brain metastasis: a rare manifestation of adenoid cystic carcinoma of the breast. Surg Neurol 1986; 26: 470- 2. 6. Lee YY, Castillo M, Nauert C. Intracranial perineural metastasis of adenoid cystic carcinoma of head and neck. ./ Compul Assist To-mogr 1985; 9: 219- 23. 7. Marsh JL, Wise DM, Smith M, Schwartz H. Lacrimal gland adenoid cystic carcinoma: intracranial and extracranial en bloc resection. Plast Reconstr Surg 1981; 68: 577- 85. 8. Massey EW, Brannon WL, Friedman A. 1, Pleet AB. Cylindroma ( adenoid cystic carcinoma) causing unilateral cranial neuropathy. South Med J 1979; 72: 1003- 5. J Ncuro- Opluhalmol, Vol. 17, No. 3, 1997 188 A. G. LEEETAL. 9. Morioka T, Matsushima T, Ikezaki K, et al. Intracranial adenoid cystic carcinoma mimicking meningioma: report of two cases. Neuroradiology 1993; 35: 462- 5. 10. Piepmeier JM, Virapongse C, Kier EL, Kim J, Greenberg A. Intracranial adenoid cystic carcinoma presenting as a primary brain tumor. Neurosurgery 1983; 12: 348- 52. 11. Wakisaka S, Nonaka A, Morita Y, Fukui M, Kinoshita K. Adenoid cystic carcinoma with intracranial extension: report of three cases. Neurosurgery 1990; 26: 1060- 5. 12. Gormley WB, Sekhar LN, Wright DC, et al. Management and long- term outcome of adenoid cystic carcinoma with intracranial extension: a neurosurgical perspective. Neurosurgery I996; 38: 1105- 13. 13. Levartovsky S, Milstein A, Nissim F, Loven D, Shani A. An unusual presentation of adenoid cystic carcinoma of the lacrimal gland. Ophthal Plast Reconstr Surg 1993; 9: 47- 50. 14. Martin DS, Awwad EE, Maves MD. Imaging facial pain of trigeminal origin. Am J Otolaryngol 1995; 16: 132- 7. 15. Rounthwaite FJ, Frei JV, Wallace AC, Watson TA. The effect of radiotherapy in the treatment of adenoid cystic carcinoma of the head and neck arising in minor salivary glands. J Otolaryngol 1977; 6: 297- 308. 16. Singh J, Boparai MS, Ahmed KA. Unusual presentation of lacrimal gland tumours. Indian J Ophthalmol 1992; 40: 118- 21. 17. Smith LC, Lane N, Rankow RM. Cylindroma ( adenoid cystic carcinoma): a report of fifty- eight cases. Am J Surg 1965; 110: 519- 26. 18. Swash M. Invasion of cranial nerves by salivary cylindroma: four cases treated by radiotherapy. J Neurol Neurosurg Psychiatry 1971; 34: 475- 80. 19. Tannock IF, Sutherland DJ. Chemotherapy for adenocystic carcinoma. Chemotherapy for adenocystic carcinoma. Cancer 1980; 46: 452- 4. 20. Vincentelli F, Grisoli F, Leclercq TA, Ardaud B, Diaz- Vasquez P, Hassoun J. Cylindromas of the base of the skull: report of four cases. J Neurosurg 1986; 65: 856- 9. 21. Spiro RH, Huvos AG, Strong EW. Adenoid cystic carcinoma: factors influencing survival. Am J Surg 1979; 138: 579- 83. 22. Wright JE, Rose GE, Garner A. Primary malignant neoplasm of the lacrimal gland. Br J Ophthalmol 1992; 76: 386 23. Yoshimura Y, Hasegawa K, Wada T, Fujita K, Kawakatsu K. Metastasis of adenoid cystic carcinoma of the mandible to the Gasserian ganglion. J Am Dental Assoc 1978; 96: 469- 73. 24. Cummings CW. Adenoid cystic carcinoma ( cylindroma) of the parotid gland. Ann Otol Rhinol Laryngol 1977; 86: 280- 92. 25. Gelber ND, Ragland RL, Knorr JR, Smioth TW, Stone BB. Intracranial metastatic adenoid cystic carcinoma: presumed hematogenous spread from a primary tumor in the parotid gland. Am J Radiol 1992; 158: 1163- 4. 26. Variakojis D, Archer FL, Feldman SA, Moody RA. Rapidly progressing adenoid cystic carcinoma. Arch Otolaryngol Head Neck Surg 1970; 92: 90- 3. 27. Osborn AG. Radiology of the pterygoid plates and pterygopalatine fossa. Am. J Radiol 1979; 132: 389- 94. 28. Slavin ML, Abramson AL. Squamous cell carcinoma of the pterygopalatine fossa ( retroantral space). J Clin Neuroophthalmol 1986; 6: 254- 7. 29. Wolin MJ. Neuro- ophthalmic manifestations of paranasal sinus disease. Ophthalmol Clin North Am 1991; 4: 585- 603. J Neiiro- Ophthalnwl, Vol. 17, No. 3, 1997 |