| OCR Text |
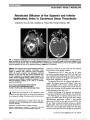
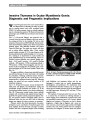
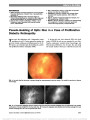
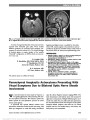
Show A variety of congenital disorders of the pons have been reported with horizontal gaze palsy. These include Moebius syndrome (2), associated with synergetic con-vergence (3) and with scoliosis (4,5). The clinical findings of scoliosis appear to require atrophy of the medulla ("butterfly" configuration on MRI), which was not pres-ent in our case. D. Vrushali, DNB R. Muralidhar, MD, DNB, MRCO, FRCS P. Vijayalakshmi, DO, MS Aravind Eye Hospital, Madurai, India K. G. Srinivasan, MD KGS Scans, Madurai, India The authors report no conflicts of interest. Supplemental digital content is available for this article. Direct URL citations appear in the printed text and are provided in the full text and PDF versions of this article on the journal's Web site (www.jneuro-ophthalmology.com). REFERENCES 1. Connors R, Ngan V, Howard J. A case of complete lateral gaze paralysis and facial diplegia: the 16 syndrome. J Neuroophthalmol. 2013;33:69-70. 2. Ouanounou S, Saigal G, Birchansky S. Möbius syndrome. AJNR Am J Neuroradiol. 2005;26:430-432. 3. dos Santos AV, Matias S, Saraiva P, Goulão A. MR imaging features of brain stem hypoplasia in familial horizontal gaze palsy and scoliosis. AJNR Am J Neuroradiol. 2006;27:1382-1383. 4. Rossi A, Catala M, Biancheri R, Di Comite R, Tortori-Donati P. MR imaging of brain-stem hypoplasia in horizontal gaze palsy with progressive scoliosis. AJNR Am J Neuroradiol. 2004;25:1046-1048. 5. Jain NR, Jethani J, Narendran K, Kanth L. Synergistic convergence and split pons in horizontal gaze palsy and progressive scoliosis in two sisters. Indian J Ophthalmol. 2011;59:162-165. Parenchymal Anaplastic Astrocytoma Presenting With Visual Symptoms Due to Bilateral Optic Nerve Sheath Involvement We read with interest the recent report by Traynis et al (1) regarding gliomatosis cerebri presenting with ante-rior visual pathway involvement. We evaluated a patient that further expands the neuro-ophthalmic spectrum of central nervous system gliomas. A 23-year-old man reported bilateral, transient visual obscurations. Examination revealed normal visual acuity, mild blind spot enlargement on visual field testing, and bilateral optic disc edema. Magnetic resonance imaging (MRI) of the brain demonstrated a left thalamic lesion with increased T2 signal and no enhancement. Multiple MRIs during the next 5 months were stable. Five and a half months after presentation, the visual obscurations became more frequent and the patient developed bilateral peripheral visual field loss. He denied headache and fever, and medical history, social history, and family history were unremarkable. FIG. 1. A. T2 axial magnetic resonance imaging (MRI) demonstrates a midsagittal cleft (arrow) producing "split pons sign." B. T1 sagittal MRI shows pontine hypoplasia with abnormal appearance of the floor of the fourth ventricle. Letters to the Editor: J Neuro-Ophthalmol 2013; 33: 307-318 313 Letters to the Editor Copyright © North American Neuro-Ophthalmology Society. Unauthorized reproduction of this article is prohibited. When we first examined the patient, visual acuity was 20/50, right eye, and 20/200, left eye. Visual fields were constricted bilaterally and there was marked optic disc edema with subretinal fluid extending into the macula in each eye. Ophthalmic and neurological examinations were normal otherwise. Two lumbar punctures had opening pressures of 23 and 22 cm of water. Cerebrospinal fluid (CSF) had 13 white blood cells/mL with monocytic predominance, 46 mg/dL protein, and normal or negative testing for glucose, bacterial culture, venereal disease research laboratory, oligoclonal bands, angiotensin-converting enzyme (ACE), and malig-nant cells. CSF cytology from a third lumbar puncture revealed rare spindle cells with mild atypia. Hematologic tests, including antinuclear antibody, aqua-porin 4 antibody, and ACE levels, were within normal limits as were studies for Lyme disease, coxsackie virus, varicella-zoster virus, arbovirus, West Nile virus, Bartonella henselae, syphilis, Cryptococcus neoformans, toxoplasmosis, Coccidioides, and HIV. Brain MRI demonstrated a stable, nonenhancing left thalamic mass (Fig. 1). Magnetic resonance (MR) spectros-copy showed decreased N-acetylaspartate resonance signal intensity and increased signal intensity, consistent with a low-grade neoplasm or inflammatory process. Orbital MRI showed increased fluid space and enlargement of the optic nerve sheaths (Fig. 2). Brain MR angiography and venography and spine MRI were within normal limits as were computed tomography of the chest, abdomen, and pelvis and a gallium scan. Despite empiric treatment with systemic corticosteroids, visual function worsened. Stereotactic biopsy of the thalamic lesion and left frontal meninges revealed parenchymal ana-plastic astrocytoma, World Health Organization (WHO) grade III, in thalamic tissue samples and findings suggestive of leptomeningeal spread of glioma (Fig. 3). Immunohisto-chemistry studies showed that tumor cells were positive for glial fibrillary acidic protein (GFAP) and negative for leukocyte common antigen, CD68, CD3, and CD20. Many cells stained with p53, consistent with the presence of p53 muta-tion in tumor cells. The Ki-67 proliferation marker stained more than 5% of tumor cells, and the leptomeningeal sample demonstrated focal staining of a low number of cells with GFAP, p53, and Ki-67. Optic nerve sheath biopsy (Fig. 3C) was not diagnostic of tumor spread or another process. The patient was treated for 6 weeks with concurrent temozolomide (75 mg/m2 daily) and whole brain radiation of 45 Gy in 1.8 Gy fractions and then placed on FIG. 1. Axial fluid attenuated inversion recovery image of thalamic mass (arrows) 5 months after the symptom onset. The lesion was isointense on T1 and did not demonstrate contrast enhancement. FIG. 2. Postcontrast, fat-saturated T1 magnetic resonance imaging of optic nerves 5 months after the symptom onset demonstrates variable thickening and enhancement of both optic nerve sheaths. 314 Letters to the Editor: J Neuro-Ophthalmol 2013; 33: 307-318 Letters to the Editor Copyright © North American Neuro-Ophthalmology Society. Unauthorized reproduction of this article is prohibited. maintenance chemotherapy with temozolomide (200 mg/m2 daily for 5 days every 28 days for a planned total of 6 cycles). Visual acuity stabilized at hand motion in the right eye and light perception in the left eye with some expansion of the right eye visual field. Ophthalmoscopic examination showed bilateral optic disc pallor. MRI of the brain and orbits revealed slight interval decrease in size of the thalamic tumor, reduction in mass effect on the third ventricle, and enhancement of both optic nerves. The patient developed left buttock pain, and MRI showed new leptomeningeal enhancement within the thoracic spine suggestive of further tumor spread. Our patient had a parenchymal anaplastic astrocytoma and presented with transient visual obscurations due to presumed neoplastic spread to the optic nerve sheaths. Although we do not have pathological confirmation of leptomeningeal spread, the findings of the optic nerve sheath biopsy, CSF analysis, and clinical course provide supportive evidence. Leptomeningeal spread of malignant astrocytomas is well described. In a study of patients with high-grade gliomas (33 anaplastic astrocytoma and 35 glioblastoma multiforme) reported by Saito et al (2), 25% had intracranial dissemination and 6 (9%) had spinal dissemination. All those with spinal dissemination had primary thalamic or temporal lobe tumors and the authors proposed proximity to CSF circulation as a risk factor for dissemination. In a case series of postmortem con-firmed cases of leptomeningeal infiltration, Boyle et al (3) found that 18 of 63 cases were associated with an intracranial mass lesion and 7 of these were astrocytomas. Of the 18 cases associated with an intracranial mass lesion, CSF contained ma-lignant cells in only 21%, and presenting signs included optic disc edema in 45%. The authors proposed that papilledema may have represented either elevated intracranial pressure or neoplastic optic nerve infiltration but did not have sufficient clinical data to make this distinction. In our patient, elevated intracranial pressure was excluded by serial lumbar punctures. In our patient, the nonenhancing appearance of the thalamic mass on MRI and its stability on serial scans led to the initial diagnostic consideration of a low-grade neoplasm unrelated to his neuro-ophthalmic symptoms and signs. Several case series reinforce that neuroimaging characteristics do not reliably predict histological grade. In both retrospective and prospective studies of parenchymal brain lesions without enhancement, between 35% and 45% are WHO grade III on histological examination (4,5). One study estimated that 9% of malignant supra-tentorial gliomas lack contrast enhancement (6). It has been suggested that advanced imaging modalities, such as perfusion-weighted imaging and MR spectroscopy, may provide additional insight into the malignant poten-tial of intracranial lesions (7-9). Yet as our case illustrates, false-negative results limit the utility of these techniques. One possible reason for imaging and histological discrep-ancy might be heterogeneity within the tumor with focal high-grade transformation (10). Kelly M. Bui, MD Asim V. Farooq, MD Heather E. Moss, MD, PhD Department of Ophthalmology and Visual Sciences, University of Illinois at Chicago, Chicago, Illinois, hemoss@uic.edu Amy Y. Lin, MD Department of Pathology, University of Illinois at Chicago, Chicago, Illinois Department of Ophthalmology and Visual Sciences, University of Illinois at Chicago, Chicago, Illinois Tibor Valyi-Nagy, MD, PhD Department of Pathology, University of Illinois at Chicago, Chicago, Illinois FIG. 3. Biopsy specimens of thalamus (A), leptomeninges (B), and optic nerve sheath (C). There is pleomorphism and glial nuclear atypia with increased cellularity and scattered mitotic figures in the thalamic specimen (A), small focal collections of atypical cells in the leptomeninges (B), but none in the optic nerve sheath (C) (hematoxylin and eosin, ·200). Insets of p53 immunohistochemistry show staining of many thalamic tumor cells (A), atypical leptomeningeal cells (B), and rare optic nerve sheath cells (C). Letters to the Editor: J Neuro-Ophthalmol 2013; 33: 307-318 315 Letters to the Editor Copyright © North American Neuro-Ophthalmology Society. Unauthorized reproduction of this article is prohibited. J. Lee Villano, MD, PhD Department of Oncology, University of Illinois at Chicago, Chicago, Illinois Dr. Moss receives support from the National Institutes of Health (Grant number K12EY021475). The authors report no conflict of interest. REFERENCES 1. Traynis I, Singer S, Winterkorn K, Rosenblum M, Dinkin M. Infiltration of the optic chiasm, nerve and disc by gliomatosis cerebri. J Neuroophthalmol. 2013 Jan 2(epub ahead of print). 2. Saito R, Kumabe T, Jokura H, Shirane R, Yoshimoto T. Symptomatic spinal dissemination of malignant astrocytoma. J Neurooncol. 2003;61:227-235. 3. Boyle R, Thomas M, Adams JH. Diffuse involvement of the leptomeninges by tumour-a clinical and pathological study of 63 cases. Postgrad Med J. 1980;56:149-158. 4. Kondziolka D, Lunsford DL, Martinez AJ. Unreliability of contemporary neurodiagnostic imaging in evaluating suspected adult supratentorial (low-grade) astrocytoma. J Neurosurg. 1993;79:533-536. 5. Barker FG II, Chang SM, Huhn SL, Davis RL, Gutin PH, McDermott MW, Wilson CB, Prados MD. Age and the risk of anaplasia in magnetic resonance-nonenhancing supratentorial cerebral tumors. Cancer. 1997;80:936-941. 6. Scott JN, Brasher PMA, Sevick RJ, Rewcastle NB, Forsyth PA. How often are nonenhancing supratentorial gliomas malignant? A population study. Neurology. 2002;59:947-949. 7. Zonari P, Baraldi P, Crisi G. Multimodal MRI in the characterization of glial neoplasms: the combined role of single-voxel MR spectroscopy, diffusion imaging and echo-planar perfusion imaging. Neuroradiology. 2007;49:795-803. 8. Batra A, Tripathi RP, Singh AK. Perfusion magnetic resonance imaging and magnetic resonance spectroscopy of cerebral gliomas showing imperceptible contrast enhancement on conventional magnetic resonance imaging. Australas Radiol. 2004;48:324-332. 9. Chaskis C, Stadnik C, Michotte A, Van Rompaey K, D'Haens J. Prognostic value of perfusion-weighted imaging in brain glioma: a prospective study. Acta Neurochir (Wien). 2006;148:277-285. 10. Frazier JL, Johnson MW, Burger PC, Weingart JD, Quinones- Hinojosa A. Rapid malignant transformation of low-grade astrocytomas: report of 2 cases and review of the literature. World Neurosurg. 2010;73:53-62. Linezolid-Associated Optic Neuropathy in a Patient With Drug-Resistant Tuberculosis We enjoyed reading the review article by Wang and Sadun (1) dealing with drug-induced mitochon-drial optic neuropathies. Recently, we evaluated a patient taking linezolid, a synthetic antimicrobial agent effective against gram-positive bacteria, including vancomycin-resistant enterococci and methicillin-resistant staphylo-cocci as well as drug-resistant strains of Mycobacterium tuberculosis (2,3). This antibiotic has been linked to optic neuropathy (4-11). Our patient's presentation appears unusual in that it was not associated with prominent optic disc swelling. A 41-year-old woman was referred for evaluation of visual function. She had a history of pulmonary tuberculosis and had been treated with linezolid for 17 months. Initial visual acuity was 20/20, right eye and 20/20, left eye. No abnormalities were detected in the examination of the FIG. 1. (A) Twenty months after beginning linezolid, automated visual fields demonstrate subtle field loss in the right eye and reduced sensitivity in the left eye. (B) Two months after linezolid was discontinued, visual fields show improvement bilaterally. 316 Letters to the Editor: J Neuro-Ophthalmol 2013; 33: 307-318 Letters to the Editor Copyright © North American Neuro-Ophthalmology Society. Unauthorized reproduction of this article is prohibited. |