| Title |
A Case of Isolated Susac Occlusive Retinal Vasculitis |
| Creator |
Seamone, Mark E; Fielden, Michael |
| Affiliation |
Faculty of Medicine (MES, MF), University of Calgary, Calgary, Alberta, Canada Calgary Retina Consultants (MF), Calgary, Alberta, Canada |
| Abstract |
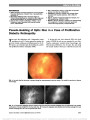
Susac syndrome is characterized by encephalopathy, sensorineural hearing loss, and branch retinal artery occlusion. Additional ocular findings include arteriolar wall hyperfluorescence and Gass plaques. We present a 51-year-old Caucasian woman with ophthalmologic findings indicative of Susac syndrome in the setting of tinnitus and migraine with aura. |
| Subject |
Female; Fluorescein Angiography; Humans; Middle Older people; Migraine with Aura; Susac Syndrome; Tinnitus |
| Format |
application/pdf |
| Publication Type |
Journal Article |
| Collection |
Neuro-Ophthalmology Virtual Education Library: Journal of Neuro-Ophthalmology Archives: https://novel.utah.edu/jno/ |
| Publisher |
Lippincott, Williams & Wilkins |
| Holding Institution |
Spencer S. Eccles Health Sciences Library, University of Utah |
| Rights Management |
© North American Neuro-Ophthalmology Society |
| Setname |
ehsl_novel_jno |
| ID |
227482 |
| Reference URL |
https://collections.lib.utah.edu/ark:/87278/s6gr03wb/227482 |