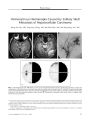
| Abstract |
Natural killer/T-cell lymphomas (NKTLs) are rare destructive lesions that usually involve the nasal cavity or paranasal sinuses. Orbital and intracranial involvement is rare. A 53-year-old man with systemic lupus erythematosus who was receiving chronic low-dose prednisone treatment developed proptosis of the right eye. Biopsy of a sino-orbital lesion suggested nonspecific inflammation. Clinical and imaging manifestations resolved with a higher dose of prednisone, but when the prednisone dose was tapered, the patient developed a complete right third cranial nerve palsy. Imaging showed return of the original lesion, now with intracranial extension and enhancement of the right third cranial nerve. Repeat biopsy showed features consistent with NKTL. Biopsy of this lesion in its early stage may misleadingly suggest a primary inflammatory disorder because of a paucity of neoplastic cells, a large number of inflammatory cells recruited by the innate natural killer (NK) cell immune response, and extensive necrosis caused by angiodestructive tumor cells. |
| Subject |
Antigens, Neoplasm, analysis; Antigens, Neoplasm, immunology; Antineoplastic Combined Chemotherapy Protocols, therapeutic use; Epstein-Barr Virus Infections, complications; Epstein-Barr Virus Infections, immunology; Fatal Outcome; Frontal Lobe, pathology; Humans; Immunosuppressive Agents, therapeutic use; Lung Neoplasms, diagnosis; Lung Neoplasms, secondary; Lupus Erythematosus, Systemic, complications; Lupus Erythematosus, Systemic, drug therapy; Lymphoma, Extranodal NK-T-Cell, complications; Lymphoma, Extranodal NK-T-Cell, diagnosis; Magnetic Resonance Imaging; Male; Middle Older people; Neoplasm Invasiveness, pathology; Oculomotor Nerve, pathology; Oculomotor Nerve, physiopathology; Oculomotor Nerve Diseases, etiology; Oculomotor Nerve Diseases, pathology; Oculomotor Nerve Diseases, physiopathology; Orbit, pathology; Orbit, radiography; Paranasal Sinuses, pathology; Paranasal Sinuses, radiography; Prednisone, therapeutic use; Radiotherapy; Tomography, X-Ray Computed; Treatment Failure; Tumor Markers, Biological, analysis; Tumor Markers, Biological, immunology |