| Title |
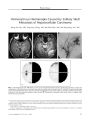
Histopathologic Features of Multiple Myeloma Involving the Optic Nerves |
| Creator |
Yeung, SN; Paton, KE; Dorovini-Zis, K; Chew, JB; White, VA |
| Affiliation |
Department of Ophthalmology and Visual Sciences, Eye Care Centre, Vancouver, British Columbia, Canada. sonia.y@gmail.com |
| Abstract |
We report a case of optic nerve involvement by multiple myeloma in which progressive visual loss heralded leukemic transformation and intracranial involvement. Imaging showed enhancing nodules in the intracranial segments of both optic nerves posterior to the optic canals and in the anterior optic tract, optic chiasm, and basal leptomeninges. Postmortem histopathologic examination disclosed malignant plasma cells in the subarachnoid spaces around the optic nerves and in the optic nerves. Infarctions were present in both optic nerves near their junction with the globes. Microscopic examination also showed malignant plasma cell infiltration of the leptomeninges of the cerebrum, brain stem, optic chiasm, pituitary gland, cranial bone marrow, and subarachnoid blood vessels. This is the first reported histopathologic examination in conjunction with MRI of multiple myeloma involving the anterior visual pathway. The mechanism of optic neuropathy in this case is probably related to infiltration of the optic nerve meninges by malignant plasma cells and impaired vascular supply caused by aggregated intraluminal plasma cells and monoclonal hypergammaglobulinemia. |
| Subject |
Older people; Brain, pathology; Disease Progression; Fatal Outcome; Humans; Hypergammaglobulinemia, etiology; Hypergammaglobulinemia, pathology; Hypergammaglobulinemia, physiopathology; Leukemic Infiltration, pathology; Magnetic Resonance Imaging; Male; Meninges, pathology; Multiple Myeloma, pathology; Optic Nerve, pathology; Optic Nerve, physiopathology; Optic Nerve Neoplasms, pathology; Plasma Cells, pathology; Retinal Artery, pathology; Skull, pathology; Vision, Low, etiology; Vision, Low, pathology; Vision, Low, physiopathology; Visual Pathways, pathology |
| Format |
application/pdf |
| Publication Type |
Journal Article |
| Collection |
Neuro-Ophthalmology Virtual Education Library: Journal of Neuro-Ophthalmology Archives: https://novel.utah.edu/jno/ |
| Publisher |
Lippincott, Williams & Wilkins |
| Holding Institution |
Spencer S. Eccles Health Sciences Library, University of Utah |
| Rights Management |
© North American Neuro-Ophthalmology Society |
| Setname |
ehsl_novel_jno |
| ID |
225663 |
| Reference URL |
https://collections.lib.utah.edu/ark:/87278/s6vt4z6b/225663 |