| Title |
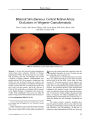
Bilateral Optic Neuritis in Wegener Granulomatosis |
| Creator |
Monteiro, MLR; Borges, WIS; do Val Ferreira Ramos, C; Lucato, LT; Leite, CC |
| Affiliation |
Department of Ophthalmology, Hospital das Clínicas of the University of São Paulo Medical School, São Paulo, Brazil. mlrmonteiro@terra.com.br |
| Abstract |
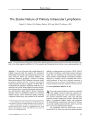
A 32-year-old patient with recurrent sinusitis had severe visual loss from optic neuropathy. Imaging revealed severe bone destruction and soft tissue densities of the paranasal sinuses and enhancement of the dura of the frontal sinuses, optic canals, and superior orbital fissures bilaterally. Endoscopic sinusectomy with biopsy showed granulomatous vasculitis compatible with Wegener granulomatosis (WG). The patient was treated with intravenous and oral corticosteroids and oral cyclophosphamide that led to rapid and dramatic visual recovery. This case draws attention to the fact that optic neuritis may be an early inflammatory manifestation of WG and that rapid diagnosis and aggressive anti-inflammatory treatment is critical before inflammation of arteries leads to infarction and irreversible visual loss. |
| Subject |
Adult; Cyclophosphamide, therapeutic use; Drug Therapy, Combination; Glucocorticoids, therapeutic use; Humans; Magnetic Resonance Imaging; Male; Optic Neuritis, complications; Optic Neuritis, etiology; Prednisone, therapeutic use; Recurrence; Sinusitis, diagnosis; Sinusitis, etiology; Treatment Outcome; Vision Disorders, etiology; Vision Disorders, physiopathology; Visual Acuity; Visual Fields; Wegener Granulomatosis, complications |
| Format |
application/pdf |
| Publication Type |
Journal Article |
| Collection |
Neuro-Ophthalmology Virtual Education Library: Journal of Neuro-Ophthalmology Archives: https://novel.utah.edu/jno/ |
| Publisher |
Lippincott, Williams & Wilkins |
| Holding Institution |
Spencer S. Eccles Health Sciences Library, University of Utah |
| Rights Management |
© North American Neuro-Ophthalmology Society |
| Setname |
ehsl_novel_jno |
| ID |
225415 |
| Reference URL |
https://collections.lib.utah.edu/ark:/87278/s6dr61jp/225415 |