| OCR Text |
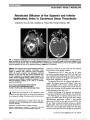
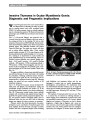
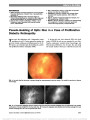
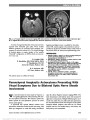
Show Invasive Thymoma in Ocular Myasthenia Gravis: Diagnostic and Prognostic Implications We read with great interest the recent article by Bruce and Kupersmith (1) discussing the safety of predni-sone in treating patients with ocular myasthenia gravis (OMG). Yet before treatment, there are critically important steps in evaluating these patients. We illustrate this point by presenting 2 cases of OMG that were found to have invasive thymoma. Case 1: A 50-year-old Hispanic man presented with a 4-month history of ptosis and diplopia, which was worse in the evening and better in the morning. He had no other symptoms. Visual acuity was 20/20 bilaterally. External exami-nation showed bilateral variable ptosis, which increased with sustained upgaze, mild orbicularis weakness, and positive Cogan lid twitch sign. The pupils were isocoric, and there was no relative afferent pupillary defect. Ocular motility revealed variable exotropia of 12-16 prism diopters and bi-lateral pseudointernuclear ophthalmoplegia. Ice test was pos-itive, resulting in an improvement in ocular motility and ptosis. Ophthalmoscopy was normal bilaterally. Serum ace-tylcholine receptor antibodies were elevated: binding anti-body = 33.0 nmol/L (positive, .0.5 nmol/L); blocking antibody = 48% (positive, .25%); modulating antibody = 44% (positive, .26%). Electromyographic and nerve con-duction studies were diagnostic of myasthenia gravis. Com-puted tomography (CT) of the chest revealed a thymic mass (Fig. 1A). At surgery, in addition to thymectomy, pericardial resection was performed because the tumor was found to be invading the pericardium. Pathology confirmed invasive thymoma, with mixed pattern grade B1, B2, and focal B3, and no lymphovascular or perineural invasion (stage III). Following surgery, the patient had near complete resolution of his myasthenic symptoms. Case 2: A 67-year-old Caucasian woman developed left-sided ptosis and diplopia, and edrophonium testing and acetylcholine receptor antibodies were positive. CT of the chest disclosed nodular densities in the anterior mediastinum (Fig. 1B). Thymectomy revealed invasive thymic epithelial neoplasm with conventional and atypical features (stage II, grade B3). The patient received postoperative radiation ther-apy, and positron emission tomography (PET) and CT performed within the first year and a half the following surgery were negative for tumor recurrence or metastases. Nineteen months after initial presentation, the patient developed an acute exacerbation of myasthenia gravis with ptosis, diplopia, shortness of breath, and upper extremity weakness. She had a complicated hospital course including atrial fibrillation and respiratory failure, and she was discharged 4 months later on weekly plasmapheresis, pyridostigmine, and prednisone. On examination, there was mild bilateral orbicularis weakness, but no Cogan lid twitch sign and variable exotropia of 20-50 prism-diopters and right hypertropia. Follow-up PET and chest CT have remained stable. We emphasize 3 important points from our cases. First, it is essential that we remind our referring clinicians to obtain imaging of the mediastinum in patients with ocular and generalized myasthenia gravis (2,3). Second, delayed diagnosis and treatment of thymoma can lead to disease progression, a higher stage at diagnosis, and a worse sys-temic outcome as more invasive stages correlate with higher mortality rates (4,5). Third, patients who have undergone thymectomy for malignant or invasive disease and present FIG. 1. A. Case 1. Thymic mass measures 20 · 20 · 23 mm. B. Case 2. Thymoma appears as multiple nodular densities measuring 14 · 10 mm. Circle denotes thymoma. Letters to the Editor: J Neuro-Ophthalmol 2013; 33: 307-318 307 Letters to the Editor Copyright © North American Neuro-Ophthalmology Society. Unauthorized reproduction of this article is prohibited. with worsening myasthenic symptoms, including ocular complaints, might benefit from repeat mediastinal imaging to rule out recurrent or residual thymoma (6). Cynthia Ishin Tung, MD Department of Ophthalmology The University of Texas Medical Branch, Galveston, TX Department of Ophthalmology The Methodist Hospital, Houston, TX Diana Chao, MD Department of Ophthalmology The University of Texas Medical Branch, Galveston, TX Department of Ophthalmology The Methodist Hospital, Houston, TX Nagham Al-zubidi, MD Department of Ophthalmology The Methodist Hospital, Houston, TX Monica Yalamanchili Saint Bonaventure University Saint Bonaventure, NY Andrew Go Lee, MD Department of Ophthalmology The University of Texas Medical Branch, Galveston, TX Department of Ophthalmology The Methodist Hospital, Houston, TX Baylor College of Medicine, Houston, TX Departments of Ophthalmology Neurology, and Neurosurgery Weill Cornell Medical College, New York, NY Department of Ophthalmology The University of Iowa Hospitals and Clinics Iowa City, IA aglee@tmhs.org Supported in part by an unrestricted grant from the Research to Prevent Blindness to the University of Texas Medical Branch, Galveston, TX. The authors report no conflicts of interest. REFERENCES 1. Bruce BB, Kupersmith MJ. Safety of prednisone for ocular myasthenia gravis. J Neuroophthalmol. 2012;32:212-215. 2. Masaoka A, Yamakawa Y, Niwa H, Fukai I, Kondo S, Kobayashi M, Fujii Y, Monden Y. Extended thymectomy for myasthenia gravis patients: a 20-year review. Ann Thorac Surg. 1996;62:853-859. 3. Roberts PF, Venuta F, Rendina E, De Giacomo T, Coloni GF, Follette DM, Richman DP, Benfield JR. Thymectomy in the treatment of ocular myasthenia gravis. J Thor Cardiovasc Surg. 2001;122:562-568. 4. Masaoka A, Yamakawa Y, Niwa H, Fukai I, Saito Y, Tokudome S, Nakahara K, Fujii Y. Thymectomy and malignancy. Eur J Cardiothorac Surg. 1994;8:251-253. 5. Liu W, Tong T, Ji Z, Zhang Z. Long-term prognostic analysis of thymectomized patients with myasthenia gravis. Chinese Med J. 2002;11:235-237. 6. Ito M, Fujimura S, Monden Y, Watanabe Y, Shimizu N, Hirono T, Iuchi K, Tsubota N, Masaoka A. A retrospective group study on post-thymectomy myasthenia gravis. Nippon Kyobu Geka Gakkai Zasshi. 1992;40:189-193. Idiopathic Sclerosing Orbital Inflammation: Presentation of an Unusual Case With Isolated Bilateral Optic Nerve Involvement We read with great interest the report by Levin et al (1) regarding the role of the optic nerve biopsy in the management of progressive optic neurop-athy. We had the opportunity to evaluate a 50-year-old man with progressive deterioration of vision in his left eye for 2 months with minimal periocular pain. Visual acuity was 20/20, right eye, and no light perception, left eye. The right fundus was normal but there was marked optic disc edema in the left eye (Fig. 1). Magnetic reso-nance imaging (MRI) of the brain and orbits demon-strated enhancement and thickening of the left optic nerve (Fig. 2). An extensive work-up including hemato-logic tests, lumbar puncture, and computed tomography of chest, abdomen, and pelvis was unremarkable. The patient was given 1 g of methylprednisolone intra-venously for 3 days followed by a tapering dose of oral steroids over several months. Although there was im-provement in the left optic disc edema, vision remained unchanged. Four months after onset of symptoms, the patient reported vision loss in the right eye. Acuity was 20/40, right eye, and no light perception, left eye. Funduscopy revealed right optic disc edema and left optic atrophy. MRI demonstrated thickening of the right optic with marked enhancement following intravenous contrast. Prednisone was restarted at a dose of 1 mg/kg/d, and there was rapid improvement in the vision in the right eye with resolution of right optic disc edema. 308 Letters to the Editor: J Neuro-Ophthalmol 2013; 33: 307-318 Letters to the Editor Copyright © North American Neuro-Ophthalmology Society. Unauthorized reproduction of this article is prohibited. |