| OCR Text |
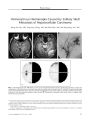
Show ORIGINAL CONTRIBUTION Multiple Intracranial Meningiomas Causing Papilledema and Visual Loss in a Patient With Nevoid Basal Cell Carcinoma Syndrome Jonathan T. Pribila, MD, PhD, Shawn M. Ronan, MD, and Jonathan D. Trobe, MD Abstract: A 27- year- old man with nevoid basal cell carcinoma syndrome ( NBCCS, Gorlin syndrome) who had undergone craniospinal irradiation for a childhood brain stem medulloblastoma complained of progressive binocular visual loss. Ophthalmologic examination disclosed subnormal visual acuity and visual fields in both eyes attributed to chronic papilledema. Brain MRI demonstrated mass effect from multiple large meningiomas. After embolization and surgical resection of the largest meningioma, papilledema disappeared and visual dysfunction resolved partially. This is the sixth reported patient with NBCCS, medulloblastoma, and craniospinal radiation who has developed intracranial meningioma, further documenting the fact that such patients have a relatively high likelihood of developing meningiomas, especially multiple meningiomas. Because patients with NBCCS are often mentally impaired and because papilledema can progress silently before causing irreversible visual loss, periodic ophthalmologic examination is advisable after craniospinal radiation. { J Neuro- Ophthalmol 2008; 28: 41- 46) Nevoid basal cell carcinoma syndrome ( NBCCS), also called basal cell nevus syndrome, Gorlin syndrome, and Gorlin- Goltz syndrome, is a rare autosomal dominant disorder with a prevalence of 1 in 57,000- 164,000 ( 1- 3). It is characterized by early basal cell carcinomas, craniofacial abnormalities ( odontogenic keratocysts, macrocephaly Departments of Ophthalmology and Visual Science ( JTP, SMR, JDT), Kellogg Eye Center, and Department of Neurology ( JDT), University of Michigan, Ann Arbor, Michigan. Address correspondence to Jonathan D. Trobe, MD, Kellogg Eye Center, 100 Wall St., Ann Arbor, MI 48109; E- mail: jdtrobe@ umich. edu frontal bossing, cleft lip or palate, hypertelorism, and calcification of the falx cerebri) and skeletal anomalies ( bifid, fused, or splayed ribs, pectus deformity, and syndactyly of digits) ( 4,5). Medulloblastoma occurs in approximately 3%- 5% of patients with NBCCS with a 3: 1 male gender predilection ( 6). In the general population, medulloblastoma presents at age 7- 8 years, whereas in NBCCS it presents at age 1- 2 years ( 1,4). Surgical resection and craniospinal radiation are standards in the postoperative care of patients with medulloblastoma. There have been several reports of meningiomas in patients with NBCCS after craniospinal radiation ( 4,7- 10), but the relationship between the development of these tumors and previous exposure to craniospinal radiation has not been reviewed in detail. We report a patient with NBCCS who developed multiple intracranial meningiomas decades after having had resection of a medulloblastoma and postoperative craniospinal radiation. The meningiomas produced increased intracranial pressure that went unrecognized until he complained of worsening vision caused by chronic papilledema. CASE REPORT A 27- year- old man with known NBCCS presented to an optometrist with the gradual development of blurred vision in both eyes over several months. The patient was found to have bilateral optic nerve edema and was referred to an emergency room. He also described worsening headaches accompanied occasionally by nausea and vomiting over the previous month. The patient's family reported a slow mental decline over the previous several years marked by difficulty in word finding and following simple instructions. An avid reader of Shakespeare, he had stopped this 2 months earlier. He denied neck pain, difficulty with coordination, and focal numbness and weakness. A brain stem medulloblastoma had been resected at age 17 months and treated with craniospinal radiation. J Neuro- Ophthalmol, Vol. 28, No. 1, 2008 41 J Neuro- Ophthalmol, Vol. 28, No. 1, 2008 Pribila et al [ I] FIG. 1. Fundus photographs obtained at presentation demonstrate optic disc edema ( papilledema) in both eyes. He had not had regular medical care since age 5. His mother reported that she also had NBCCS. At the time of presentation, the patient had become unemployed and was living with his parents. Multiple basal cell nevi were present on the head and trunk. He was alert, fully oriented, and able to perform simple calculations. Repetition and naming were intact, but he had difficulty with word finding and following complex commands. The rest of the neurologic examination was normal except for visual function. Best- corrected visual acuity was 20/ 60 in both eyes. An afferent pupillary defect was present in the right eye. Results of slit lamp examination were unremarkable. Fundus examination revealed bilateral optic disc edema ( Fig. 1). Visual fields, performed on the Humphrey perimeter, showed mean deviations of 10.21 dB in the right eye and 6.11 dB in the left eye with nerve fiber bundle loss in both eyes ( Fig. 2). Brain MRI demonstrated ventriculomegaly and six intracranial but extra- axial enhancing masses ( Fig. 3). The largest mass was in the left temporoparietal region. It measured 7.2 by 5.7 cm and compressed the lateral ventricle and brain stem. There were also two masses in the right frontal lobe, two in the left frontal lobe, and one in the right temporal lobe. Calcification was seen throughout the tentorium and falx cerebri. The patient underwent embolization and surgical resection of the left temporoparietal meningioma. Histologic analysis revealed a grade 1 transitional, microcystic, and fibrous meningioma with a proliferation index range from 0% to 5%- 10% in MIB- 1 stained sections. Three months after resection of the meningioma, the patient's best- corrected visual acuity was 20/ 30 in the right eye and 20/ 20 in the left eye. The optic disc edema had disappeared ( Fig. 4), but the afferent pupillary defect in the right eye persisted. Repeat Humphrey visual field perimetry demonstrated an improvement in visual fields with mean deviations of 6.9 dB in the right eye and 4.4 dB in the left eye ( Fig. 5). MRI demonstrated that the tumor mass effect had disappeared ( Fig. 6). The patient has since undergone excision of the remaining tumors and had no neurologic setbacks. Histopathologic examination showed all tumors to be meningiomas. DISCUSSION We have described a patient with NBCCS who, after having received craniospinal radiation for a medulloblas-toma as a child, developed multiple large meningiomas causing an intracranial mass effect that led to the m 2* 38 tj T0TflL DEYIRTION s • • s>. •••• B • & x m • • B B • • • • • B • • • ' • • • • • • • • • • • • • • • • • • • • s » • » • B B S FIG. 2. Humphrey perimetry performed at presentation shows mean deviations of - 10.21 dB in the right eye and - 6.11 dB in the left eye with nerve fiber bundle loss in both eyes. 42 © 2008 Lippincott Williams & Wilkins Meningiomas in Nevoid Basal Cell Carcinoma Syndrome J Neuro- Ophthalmol, Vol. 28, No. 1, 2008 FIG. 3. Postcontrast T1 axial brain MRI performed at presentation. The left temporoparietal meningioma ( A- C) exerts mass effect on the lateral ventricle and brain stem. There are also masses in the right temporal lobe ( B-C), right frontal lobe ( C), and left frontal lobe ( D). development of chronic papilledema and consequent visual acuity and visual field loss. The patient's complaint of blurred vision brought the meningiomas to medical attention. Twelve other patients with NBCCS who developed meningiomas have been reported ( Table 1). Six patients, including ours, had undergone craniospinal radiation for medulloblastoma between age 15 and 34 years before FIG. 4. Fundus photographs obtained 3 months after resection of the temporoparietal meningioma demonstrate resolution of papilledema. 43 J Neuro- Ophthalmol, Vol. 28, No. 1, 2008 Pribila et al FIG. 5. Humphrey perimetry performed 3 months after surgical resection of the temporoparietal meningioma shows improvement relative to the preoperative visual fields with mean deviations of - 6.9 dB in the right eye and - 4.4 dB in the left eye. the diagnosis of meningioma ( 4,7- 10). Six patients had received no radiation, and one patient had received low-dose external radiation for basal cell carcinoma ( 11). The six patients who had received craniospinal radiation had a higher incidence of development of multiple meningiomas than the seven patients who had not received such radiation. Five ( 83%) of the six patients who received radiation developed multiple meningiomas. In comparison, of the seven patients who had not received craniospinal irradiation, only one ( 8.3%) developed multiple meningiomas. One of these patients also developed a left temporal fossa schwannoma and a lip-osarcoma of the scalp. The development of meningiomas after craniospinal radiation in patients without NBCCS appears to be less common than in those with NBCCS ( 17,18). In a review of 77 reports of patients who developed meningiomas after high- dose craniospinal radiation, Musa et al ( 17) estimated the overall frequency of meningioma to be 3.5%. In that review, 6 patients ( 7.9%) had multiple meningiomas ( 17). The biochemical basis for NBCCS provides some insight into a potential molecular mechanism for the proclivity to develop second tumors. The NBCCS gene PTCH has been mapped to chromosome 9q22.3 and encodes Patched, a transmembrane receptor critical to sonic hedgehog- mediated cell cycle control through its inhibition of downstream modulators such as Smoothened ( 3,19- 21). In patients with NBCCS, one allele produces a nonfunctional protein, leaving the cell sensitive to a " second mm ' r \ \ • kAv k '^ mm FIG. 6. Postcontrast T1 axial brain MRI performed 3 months after surgical resection of the temporoparietal meningioma shows resolution of the mass effect. A- D are comparable in level to those of Fig. 3. hit" that would disrupt the other allele and render the cell resistant to sonic hedgehog- mediated regulation of the cell cycle. Craniospinal radiation would probably provide the mutagenic force necessary to cause this second hit and allow for unregulated cell growth and tumor formation. Although craniospinal irradiation is a mainstay of treatment for medulloblastomas, it should be acknowledged that patients with NBCCS develop multiple meningiomas at a much higher frequency than the general population after craniospinal irradiation. These tumors may cause increased intracranial pressure by mass effect or blockage of cerebrospinal fluid egress. When intracranial pressure increases slowly, an important adverse consequence is chronic papilledema and optic nerve damage. Periodic ophthalmologic examination, especially of the optic fundus, is recommended in these patients for two reasons: 1) they may be mentally impaired and unaware or unable to articulate visual problems; and 2) papilledema may progress for a long time before causing visual loss, at which time the visual loss may be irreversible. 44 © 2008 Lippincott Williams & Wilkins Meningiomas in Nevoid Basal Cell Carcinoma Syndrome J Neuro- Ophthalmol, Vol. 28, No. 1, 2008 TABLE 1. Reported cases Patient 1( 12) 2( 13) 3( 14) 4( 11) 5( 15) 6( 16) 7( 11) 8( 4) 9( 7) 10 ( 10) 11( 9) 12( 8) ( Ref.) 13 ( present case) Age ( years) 64 60 18 47 60 24 44 26 19 28 35 19 27 of meningiomas in patients with nevoid basal cell carcinoma syndrome Gender M M F F M F M M F M M F M NA, not applicable. * Received external radiation to the Number and location of tumor( s) 1 meningioma 1 craniopharyngioma ( location not described) 1 olfactory meningioma Multiple meningiomas ( location not described) 1 right frontoparietal meningioma 1 left temporal fossa meningioma 1 left temporoparietal meningioma 1 left parietal lobe meningioma Multiple meningiomas with brain stem compression 1 frontal lobe meningioma with extracranial extension 1 right temporal fossa meningiomal right temporal fossa meningiomal left temporal fossa schwannomal liposarcoma of the scalp 1 tuberculum sellae meningioma3 parasellar meningiomas 1 left parietal lobe meningiomal right parietal lobe meningioma 1 left temporoparietal lobe meningiomal right temporal lobe meningioma2 right frontal lobe meningiomas2 left frontal lobe meningiomas scalp. Initial symptom N/ A N/ A N/ A Hemiparesis and seizures Sixth cranial nerve palsy and decreased vision Ventricular fibrillation Aphasia and dysarthria; weakness and numbness of the right hand Neurologic symptoms ( not described) Forehead mass Depression Visual field defects and visual loss Change in affect Blurred vision Craniospinal radiation ( years to presentation) No No No No No No No* Yes ( 22) Yes ( 15) Yes ( 26) Yes ( 34) Yes ( 17) Yes ( 25) REFERENCES Evans DG, Ladusans EJ, Rimmer S, et al. Complications of the naevoid basal cell carcinoma syndrome: results of a population based study. J Med Genet 1993; 30: 460^ k Pratt MD, Jackson R. Nevoid basal cell carcinoma syndrome: a 15- year follow- up of cases in Ottawa and the Ottawa Valley. J Am Acad Dermatol 1987; 16: 964- 70. Chenevix- Trench G, Wicking C, Berkman J, et al. Further localization of the gene for nevoid basal cell carcinoma syndrome ( NBCCS) in 15 Australasian families: linkage and loss of heterozygosity. Am J Hum Genet 1993; 53: 760- 7. Kimonis VE, Goldstein AM, Pastakia B, et al. Clinical manifestations in 105 persons with nevoid basal cell carcinoma syndrome. Am J Med Genet 1997; 69: 299- 308. Gorlin RJ. Nevoid basal cell carcinoma ( Gorlin) syndrome. Genet Med 2004; 6: 530- 9. 6. Lacombe D, Chateil JF, Fontan D, et al. Medulloblastoma in the nevoid basal- cell carcinoma syndrome: case reports and review of the literature. Genet Counsel 1990; 1: 273- 7. 7. Albrecht S, Goodman JC, Rajagopolan S, et al. Malignant meningioma in Gorlin's syndrome: cytogenetic and p53 gene analysis: case report. J Neurosurg 1994; 81: 466- 71. 8. Campbell RM, Mader RD, Dufresne JRG. Meningiomas after medulloblastoma irradiation treatment in a patient with basal cell nevus syndrome. J Am Acad Dermatol 2005; 53: S256- 9. 9. Fukushima Y, Oka H, Utsuki S, et al. Nevoid basal cell carcinoma syndrome with medulloblastoma and meningioma- case report. Neurol Med- Chir 2004; 44: 665- 8. 10. O'Malley S, Weitman D, Olding M, et al. Multiple neoplasms following craniospinal irradiation for medulloblastoma in a patient with nevoid basal cell carcinoma syndrome: case report. J Neurosurg 1997; 86: 286- 8. 45 J Neuro- Ophthalmol, Vol. 28, No. 1, 2008 Pribila et al 11. Mortimer PS, Geaney DP, Liddell K. Basal cell naevus syndrome and intracranial meningioma. J Neurol Neurosurg Psychiatry 1984; 47: 210- 2. 12. TamoneyHJJr. Basal cell nevoid syndrome. Am Surg 1969; 35: 279- 83. 13. Stoelinga PJ, Peters JH, van de Staak WJ, et al. Some new findings in the basal- cell nevus syndrome. Oral Surg Oral Med Oral Pathol 1973; 36: 686- 92. 14. Southwick GJ, Schwartz RA. The basal cell nevus syndrome: disasters occurring among a series of 36 patients. Cancer 1979; 44: 2294- 305. 15. Aumaitre O, Sampoux P, Georget AM, et al. Neurologic manifestations of basal cell nevomatosis: a case ( in French). Presse Med 1986; 15: 2105- 7. 16. Jones KL, Wolf PL, Jensen P, et al. The Gorlin syndrome: a genetically determined disorder associated with cardiac tumor. Am Heart J 1986; 111: 1013- 5. 17. Musa BS, Pople IK, Cummins BH. Intracranial meningiomas following irradiation- a growing problem? Br J Neurosurg 1995; 9: 629- 37. 18. Mack EE, Wilson CB. Meningiomas induced by high-dose cranial irradiation [ see comment]. J Neurosurg 1993; 79: 28- 31. 19. Compton JG, Goldstein AM, Turner M, et al. Fine mapping of the locus for nevoid basal cell carcinoma syndrome on chromosome 9q. J Invest Dermatol 1994; 103: 178- 81. 20. Johnson RL, Rothman AL, Xie J, et al. Human homolog of patched, a candidate gene for the basal cell nevus syndrome. Science 1996; 272: 1668- 71. 21. Villavicencio EH, Walterhouse DO, larmaccone PM. The sonic hedgehog- patched- glia pathway in human development and disease. Am J Hum Genet 2000; 67: 1047- 54. 46 © 2008 Lippincott Williams & Wilkins |