| Title |
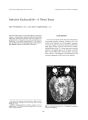
Normal Pressure Pseudotumor Cerebri |
| Creator |
Green, JP; Newman, NJ; Stowe, ZN; Nemeroff, CB |
| Affiliation |
Department of Ophthalmology, Emory University, Atlanta, Georgia, USA. |
| Abstract |
We present a case report of a patient with clinical features suggestive of pseudotumor cerebri (PTC), without a documented elevated measurement of intracranial pressure (ICP). Chart review was done of one patient's clinical course over a 28-month period. The patient was treated for PTC even though she never had a documented elevated ICP. Her signs and symptoms, including headache, disc edema, and visual field loss, all showed improvement with standard PTC therapy, which ultimately included optic nerve sheath fenestration (ONSF). Her presenting symptoms of clinical depression were also relieved with this treatment. PTC may present without an elevated ICP as defined by current standards. Some patients may be more susceptible to lower levels of ICP and develop this syndrome, and it may be responsive to standard PTC therapy. Further investigation may warrant that clinical depression be included as another minor symptom of PTC. |
| Subject |
Adolescent; Female; Fundus Oculi; Headache/pathology; Humans; Intracranial Pressure; Myelin Sheath; Optic Disk/pathology; Optic Nerve/surgery; Papilledema/pathology; Pseudotumor Cerebri/pathology; Pseudotumor Cerebri/surgery; Vision Disorders/pathology; Visual Fields |
| Format |
application/pdf |
| Publication Type |
Journal Article |
| Collection |
Neuro-Ophthalmology Virtual Education Library: Journal of Neuro-Ophthalmology Archives: https://novel.utah.edu/jno/ |
| Publisher |
Lippincott, Williams & Wilkins |
| Holding Institution |
Spencer S. Eccles Health Sciences Library, University of Utah |
| Rights Management |
© North American Neuro-Ophthalmology Society |
| Setname |
ehsl_novel_jno |
| ID |
224770 |
| Reference URL |
https://collections.lib.utah.edu/ark:/87278/s6pc67fh/224770 |