| Title |
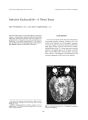
Painful Ophthalmoplegia Syndrome Secondary to Metastatic Renal Cell Carcinoma |
| Creator |
Mehelas, TJ; Kosmorsky, GS |
| Affiliation |
Cleveland Clinic, Ohio 44106, USA. |
| Subject |
Blepharoptosis/etiology; Brain/pathology; Brain Neoplasms/radiotherapy; Brain Neoplasms/secondary; Carcinoma, Renal Cell/radiotherapy; Carcinoma, Renal Cell/secondary; Cavernous Sinus/pathology; Humans; Kidney/pathology; Kidney Neoplasms/pathology; Kidney Neoplasms/radiotherapy; Magnetic Resonance Imaging; Male; Middle Older people; Ophthalmoplegia/etiology; Pain/etiology; Syndrome; Tomography, X-Ray Computed |
| Format |
application/pdf |
| Publication Type |
Journal Article |
| Collection |
Neuro-Ophthalmology Virtual Education Library: Journal of Neuro-Ophthalmology Archives: https://novel.utah.edu/jno/ |
| Publisher |
Lippincott, Williams & Wilkins |
| Holding Institution |
Spencer S. Eccles Health Sciences Library, University of Utah |
| Rights Management |
© North American Neuro-Ophthalmology Society |
| Setname |
ehsl_novel_jno |
| ID |
224780 |
| Reference URL |
https://collections.lib.utah.edu/ark:/87278/s6pc67fh/224780 |