| Title |
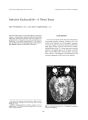
Neurosarcoidosis Presenting as an Intracranial Mass in Childhood |
| Creator |
Leiba, H; Siatkowski, RM; Culbertson, WW; Glaser, JS |
| Affiliation |
Bascom Palmer Eye Institute, Department of Ophthalmology, University of Miami School of Medicine, FL 33163, USA. |
| Abstract |
A 13-year-old boy presented with bilateral panuveitis and a superior oblique palsy. Exhaustive laboratory workup was unremarkable, but magnetic resonance imaging (MRI) revealed an enhancing pontine mass. The mass was resected, and histopathology revealed a necrotizing granuloma. Although rare, particularly in the pediatric population, the combination of panuveitis and an intracranial mass likely represents sarcoidosis. Necrosis, although also rare, may similarly be seen in neurosarcoidosis. |
| Subject |
Adolescent; Brain/pathology; Brain Diseases/diagnosis; Granuloma/diagnosis; Humans; Magnetic Resonance Imaging; Male; Necrosis; Oculomotor Nerve Diseases/diagnosis; Panuveitis/diagnosis; Sarcoidosis/diagnosis |
| Format |
application/pdf |
| Publication Type |
Journal Article |
| Collection |
Neuro-Ophthalmology Virtual Education Library: Journal of Neuro-Ophthalmology Archives: https://novel.utah.edu/jno/ |
| Publisher |
Lippincott, Williams & Wilkins |
| Holding Institution |
Spencer S. Eccles Health Sciences Library, University of Utah |
| Rights Management |
© North American Neuro-Ophthalmology Society |
| Setname |
ehsl_novel_jno |
| ID |
224775 |
| Reference URL |
https://collections.lib.utah.edu/ark:/87278/s6pc67fh/224775 |