| Title |
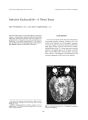
Dorsal Midbrain Syndrome due to Mesencephalic Hemorrhage |
| Creator |
Lee, AG; Brown, DG; Diaz, PJ |
| Affiliation |
Department of Ophthalmology, Baylor College of Medicine, Houston, TX 77030, USA. |
| Abstract |
Spontaneous, nontraumatic, nonhypertensive, midbrain hemorrhage is an uncommon cause of the dorsal midbrain syndrome. We describe a patient with this syndrome in whom the initial neuroimaging studies failed to clearly identify the lesion. Subsequent magnetic resonance imaging studies disclosed a dorsal midbrain hemorrhage. The patient experienced gradual spontaneous resolution of her dorsal midbrain signs and symptoms over several months. The evolution on serial neuroimaging studies of the dorsal midbrain hemorrhage in this patient is described. |
| Subject |
Older people; Brain Diseases/diagnosis; Brain Diseases/etiology; Cerebral Hemorrhage/complications; Cerebral Hemorrhage/diagnosis; Female; Humans; Magnetic Resonance Imaging; Mesencephalon/pathology; Ocular Motility Disorders/etiology; Syndrome |
| Format |
application/pdf |
| Publication Type |
Journal Article |
| Collection |
Neuro-Ophthalmology Virtual Education Library: Journal of Neuro-Ophthalmology Archives: https://novel.utah.edu/jno/ |
| Publisher |
Lippincott, Williams & Wilkins |
| Holding Institution |
Spencer S. Eccles Health Sciences Library, University of Utah |
| Rights Management |
© North American Neuro-Ophthalmology Society |
| Setname |
ehsl_novel_jno |
| ID |
224778 |
| Reference URL |
https://collections.lib.utah.edu/ark:/87278/s6pc67fh/224778 |