| Title |
Vasospastic Transient Monocular Visual Loss: Effect of Treatment With Different Doses of Nifedipine |
| Creator |
Hanna Pitkänen, MD, Ville Saarela, MD, PhD |
| Affiliation |
Department of Ophthalmology, Oulu University Hospital, Oulu, Finland |
| Abstract |
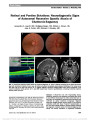
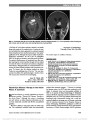
Transient monocular visual loss (TMVL) usually is due to hypoperfusion of the optic nerve or retinal circulation. After the exclusion of thromboembolic and carotid artery diseases, retinal vasospasm should be considered as an underlying cause of TMVL. We report a patient with an increasing number of transient attacks of unilateral blindness. Vasospasm was confirmed as the etiology by fundus photography during an attack. Nifedipine 10 mg/d decreased the severity of the visual loss and the number of attacks. The patient was relieved of symptoms entirely with a nifedipinedose of 20 mg/d. |
| Subject |
Adult; Calcium Channel Blockers; Female; Functional Laterality; Humans; Magnetic Resonance Imaging; Neurologic Examination; Nifedipine; Vasospasm, Intracranial; Vision Disorders; Visual Fields |
| Format |
application/pdf |
| Publication Type |
Journal Article |
| Collection |
Neuro-Ophthalmology Virtual Education Library: Journal of Neuro-Ophthalmology Archives: https://novel.utah.edu/jno/ |
| Publisher |
Lippincott, Williams & Wilkins |
| Holding Institution |
Spencer S. Eccles Health Sciences Library, University of Utah |
| Rights Management |
© North American Neuro-Ophthalmology Society |
| Setname |
ehsl_novel_jno |
| ID |
227650 |
| Reference URL |
https://collections.lib.utah.edu/ark:/87278/s6fv1s4v/227650 |