| OCR Text |
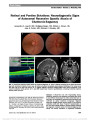
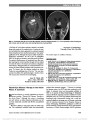
Show a "half bow-tie" with edema superiorly, inferiorly, and nasally along with atrophy of the temporal sector. A pattern of supe-rior and inferior disc edema separated by a nasal and temporal band of atrophy has been described previously as "twin peaks" papilledema (3-6). Although this was not readily visualized on funduscopic examination, the OCT plot of peripapillary RNFL in the right eye showed a twin peaks pattern of edema. Our patient's fundus pattern of hemiretinal nerve fiber atro-phy respecting the vertical meridian through the fovea helped to localize the lesion to the chiasm and constitutes a diagnostic retinal feature. Although Sanders (1) ends his historical com-mentary on Foster Kennedy syndrome with a humorous com-ment "In Gowers' day, the clinician localized the lesion. Today, the neuroradiologist does it for him." Our case dem-onstrates the ability of the ophthalmologist to localize a lesion with accuracy that rivals the best neuroimaging. Jesse M. Vislisel, MD John J. Chen, MD, PhD Randy H. Kardon, MD, PhD Department of Ophthalmology, University of Iowa, Iowa City, Iowa The authors report no conflicts of interest. REFERENCES 1. Lai AT, Chiu SL, Lin IC, Sanders M. Foster Kennedy syndrome: now and then. J Neuroophthalmol. 2014;34:92-94. 2. Hoyt WF, Kommerell G. Der fundus oculi bei homonymer hemianopsie (article in German). Klin Monbl Augenheilkd. 1973;162:456-464. 3. Czarnecki JS, Weingeist TA, Burton TC, Thompson HS. "Twin peaks" papilledema: the appearance of papilledema with optic tract atrophy. Can J Ophthalmol. 1976;11:279-281. 4. Paul TO, Hoyt WF. Funduscopic appearance of papilledema with optic tract atrophy. Arch Ophthalmol. 1976;94:467-468. 5. Ing EB, Leavitt EA, Younge BR. Papilledema following bowtie optic atrophy. Arch Ophthalmol. 1996;114:356-357. 6. Mehta JS, Plant GT, Acheson JF. Twin and triple peaks papilledema. Ophthalmology. 2005;112:1299-1301. Thyroid Eye Disease: Therapy in the Active Phase: A Comment Bhatti and Dutton (1) recently published an eloquent review entitled: "Thyroid Eye Disease: Therapy in the Active Phase." Although the review is interesting and well written, we believe important information was left out from randomized controlled trials (RCTs) and published guidelines. We wish to address 3 major topics. First, the authors state that "Few randomized controlled studies have systematically evaluated these treatment strategies. . .." However, in reviewing the literature, quite a few RCTs have been conducted on the subject. A systematic review and meta-analysis published in 2009 in the Journal of Clinical Endocrinology & Metabolism evaluated 33 RCTs comparing treatment modalities for Graves orbitopathy (GO) (2). This meta-analysis demonstrated that intravenous pulse corticosteroids therapy had a small but statistically significant advantage over oral therapy, correlating with the consensus statement by the European Group on Graves Orbitopathy (EUGOGO) published in 2008 (3) and the American Thyroid Association (ATA) and American Association of Clinical Endocrinologists (AACE) guidelines FIG. 5. Contrasted axial (A) and coronal (B) magnetic resonance imaging reveals a 3 · 5 cm suprasellar mass involving the optic chiasm and left optic nerve and causing obstructive hydrocephalus. Letters to the Editor: J Neuro-Ophthalmol 2014; 34: 422-428 425 Letters to the Editor Copyright © North American Neuro-Ophthalmology Society. Unauthorized reproduction of this article is prohibited. from 2011 (4). These guidelines are based on a strong body of evidence and should be cited as such. Second, in the flowchart included in the review, both oral and intravenous corticosteroids have been included as equal choices. As mentioned above, intravenous pulse methylprednisolone is more effective than oral predni-sone (success rate 74% vs 51%) and is better tolerated (adverse effects 56% vs 81%) (4). These treatment pro-tocols recommend a 12-week course of intravenous methylprednisolone (0.5 g as a single dose per week for 6 consecutive weeks followed by 0.25 g as single dose per week for 6 consecutive weeks, not to exceed a total of 8 g) for patients with moderate-to severe active GO. Finally, orbital radiotherapy without concomitant cortico-steroids is presented in the flowchart as an equally weighted arm for the management of active GO. This contrasts with the EUGOGO consensus guidelines, which do not include orbital radiotherapy as a treatment option for active GO (3) and with the findings of the meta-analysis (2), which found that the efficacy of orbital radiotherapy as single therapy remains un-clear, whereas the combination of radiotherapy with cortico-steroids has better efficacy than either radiotherapy or oral corticosteroids alone. The review by Bhatti and Dutton is a commendable effort, since suboptimal management of patients with GO is widespread (5). Familiarity with the current lit-erature is extremely important, as both oral and intra-venous corticosteroids are associated with severe adverse effects, including fatal cases (6). Hadas Stiebel-Kalish, MD Neuroophthalmology Unit, Department of Ophthalmology, Rabin Medical Center, Sackler School of Medicine, Tel-Aviv University, Tel-Aviv, Israel Eyal Robenshtok, MD Institute of Endocrinology and Metabolism, Rabin Medical Center, Beilinson Hospital and Sackler School of Medicine, Tel-Aviv University, Tel-Aviv, Israel The authors report no conflicts of interest. REFERENCES 1. Bhatti TM, Dutton JJ. Thyroid eye disease: therapy in the active phase. J Neuroophthalmol. 2014;34:186-197. 2. Stiebel-Kalish H, Robenshtok E, Hasanreisogly M, Ezrachi D, Shimon I, Liebovici L. Treatment modalities for Graves' ophthalmopathy: systematic review and meta-analysis. J Clin Endocrinol Metab. 2009;94:2708-2716. 3. Bartalena L, Baldeschi L, Dickinson AJ, Eckstein A, Kendall- Taylor P, Marcocci C, Mouritis MP, Perros P, Boboridis K, Bosch A, Currö N, Daumerie C, Kahaly GJ, Krassas G, Lane CM, Lazarus JH, Marinö M, Nardi M, Neoh C, Orgiazzi J, Pearce S, Pinchera A, Pitz S, Salvi M, Sivelli P, Stahl M, von Arx G, Wiersinga WM. Consensus statement of the European group on Graves' orbitopathy (EUGOGO) on management of Graves' orbitopathy. Thyroid. 2008;18:333-346. 4. Bahn-Chair RS, Burch HB, Cooper DS, Garber JR, Greenlee MC, Klein I, Laurberg P, McDougall IR, Montori VM, Rivkees SA, Ross DS, Sosa JA, Stan MN. Hyperthyroidism and other causes of thyrotoxicosis: management guidelines of the American Thyroid Association and American Association of Clinical Endocrinologists. Thyroid. 2011;21:593-646. Erratum in: Thyroid. 2011;21:1169. Thyroid. 2012;22:1195. 5. Perros P, Baldeschi L, Boboridis K, Dickinson AJ, Hullo A, Kahaly GJ, Kendell-Taylor P, Krassas GE, Lane CM, Lazarus JH, Marcocci C, Marino M, Mouritis MP, Nardi M, Orgiazzi J, Pinchera A, Pitz S, Prummel MF, Wiersinga WM. A questionnaire survey on the management of Graves' orbitopathy in Europe. The European Group of Graves' Orbitopathy. Eur J Endocrinol. 2006;155:207-211. 6. Marcocci C, Watt T, Altea MA, Rasmussen AK, Feldt- Rasmussen U, Orgiazzi J, Bartalena L. Fatal and non-fatal adverse events of glucocorticoid therapy for Graves' orbitopathy: a questionnaire survey among members of the European Thyroid Association. Eur J Endocrinol. 2012;166:247-253. Thyroid Eye Disease: Therapy in the Active Phase: A Comment: Reply We thank Drs Stiebel-Kalish and Robenshtok for their interest in our State-of-the-Art review on the treat-ment of active thyroid eye disease (TED) (1). Here are our responses to their 3 major critiques. First, Drs Stiebel-Kalish and Robenshtok take issue with our statement: "Few randomized controlled studies have systematically evaluated these treatment strat-egies. . .." Based on their very impressive review and meta-analysis on the treatment modalities of TED pub-lished in 2009, there were 33 randomized controlled trials (RCTs) conducted on TED (2). In fairness, our complete sentence should have been included in their letter: "Few randomized controlled studies have systematically evalu-ated these treatment strategies, and of those trials that have been executed, they are difficult to compare and contrast because of inconsistencies in study design and outcome meas-ures." We did not intend to suggest that in total, there have not been a number of RCTs performed in TED but rather that for each treatment modality (corticosteroids, orbital ra-diotherapy [ORT], and orbital decompression), the number of RCTs has not been very robust and variable in terms of study design and outcome measures. That point was empha-sized in the 3 tables included as electronic digital supplement 426 Letters to the Editor: J Neuro-Ophthalmol 2014; 34: 422-428 Letters to the Editor Copyright © North American Neuro-Ophthalmology Society. Unauthorized reproduction of this article is prohibited. |