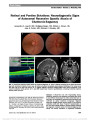
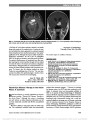
| OCR Text |
Show Literature Commentary Shahim P, Tegner Y, Wilson DH, Randall J, Skillbäck T, Pazooki D, Kallberg B, Blennow K, Zetterberg H. Blood biomarkers for brain injury in concussed professional ice hockey players. JAMA Neurol. 2014;71:684-692. Importance: Lack of objective biomarkers for brain damage hampers acute diagnosis and clinical decision-making about return to play after sports-related concussion. Objectives: To determine whether sports-related concus-sion is associated with elevated levels of blood biochemical markers of injury to the central nervous system and to assess whether plasma levels of these biomarkers predict return to play in professional ice hockey players with sports-related concussion. Design, Setting, and Participants: Multicenter prospective cohort study involving all 12 teams of the top professional ice hockey league in Sweden, the Swedish Hockey League. Two hundred eighty-eight professional ice hockey players from 12 teams contesting during the 2012-2013 season consented to participate. All players underwent clinical preseason baseline testing regarding concussion assess-ment measures. Forty-seven players from 2 of the 12 ice hockey teams underwent blood sampling before the start of the season. Thirty-five players had a concussion from September 13, 2012, to January 31, 2013; of these players, 28 underwent repeated blood sampling at 1, 12, 36, and 144 hours and when the players returned to play. Main Outcomes and Measures: Total tau, S-100 calcium-binding protein B, and neuron-specific enolase concen-trations in plasma and serum were measured. Results: Concussed players had increased levels of the axonal injury biomarker total tau (median, 10.0 pg/mL; range, 2.0-102 pg/mL) compared with preseason values (median, 4.5 pg/mL; range, 0.06-22.7 pg/mL) (P , 0.001). The levels of the astroglial injury biomarker S-100 calcium-binding protein B were also increased in players with sports-related concussion (median, 0.075 mg/L; range, 0.037-0.24 mg/L) compared with preseason values (median, 0.045 mg/L; range, 0.005-0.45 mg/L) (P , 0.001). The highest biomarker concentrations of total tau and S-100 calcium-binding protein B were measured imme-diately after a concussion, and they decreased during reha-bilitation. No significant changes were detected in the levels of neuron-specific enolase from preseason values (median, 6.5 mg/L; range, 3.45-18.0 mg/L) to postconcussion values (median, 6.1 mg/L; range, 3.6-12.8 mg/L) (P = 0.10). Conclusions and Relevance: Sports-related concussion in professional ice hockey players is associated with acute axonal and astroglial injury. This can be monitored using blood biomarkers, which may be developed into clinical tools to guide sport physicians in the medical counseling of athletes in return-to-play decisions. Athletes increasingly undergo preseason, baseline cognitive testing. In the event of a suspected concussion, comparing repeat performance to baseline helps in the evaluation process. I recently had an interesting conversation with a former professional hockey player. He and his teammates intentionally performed poorly on baseline testing to avoid receiving a concussion diagnosis during the season. Addi-tionally, neuro-ophthalmologists often see patients com-plaining of vague symptoms after a head injury from a car accident or work-related injury. In instances without objective signs, a perceived secondary gain could cloud the assessment. In both cases, an objective biomarker of concussion would help greatly. In this article, the authors found that plasma total tau levels were elevated in professional hockey players with concussion. This elevation persisted for several days and correlated well with the duration of postconcussion syn-drome symptoms. Plasma S-100B levels also were increased in players with concussion from baseline, but they were no different than S-100B levels after a game in which no concussions occurred. Although further study with larger samples is necessary, total tau may represent that elusive biomarker for concussion for which we have been searching. -Michael S. Lee, MD An objective sign of concussion, not relying on the athlete's subjective performance, is very important. The finding of elevated tau and the correlation of the level with time to recovery may improve the ability to appropriately counsel athletes with concussion. Objective biomarkers will also be helpful in caring for patients with concussions who may have nonphysiologic symptoms. -Mark L. Moster, MD Currò N, Covelli D, Vannucchi G, Campi I, Pirola G, Simonetta S, Dazzi D, Guastella C, Pignataro L, Beck-Peccoz P, Ratiglia R, Salvi M. Therapeutic outcomes of high-dose intravenous steroids in the treatment of dysthyroid optic neuropathy. Thyroid. 2014;24:897-905. Background: Although pulsed intravenous methylpredniso-lone (iv-MP) has been shown to be effective and well tolerated in moderate-to-severe Graves orbitopathy (GO), Moster and Lee: J Neuro-Ophthalmol 2014; 34: 417-421 417 Literature Commentary Section Editors: Mark L. Moster, MD Michael S. Lee, MD Copyright © North American Neuro-Ophthalmology Society. Unauthorized reproduction of this article is prohibited. limited data are available on dysthyroid optic neuropathy (DON). The objective of this retrospective study was to investigate the efficacy of iv-MP in the treatment of DON and to seek parameters predictive of response. Methods: Twenty-four DON patients (40 eyes) treated with iv-MP from 2007 to 2012 were included in the study. Con-current neurological or ophthalmologic diseases or signs of corneal exposure were considered as exclusion criteria. Iv-MP was administered daily for 3 consecutive days and repeated the next week. At 6 months, eyes not requiring surgery to preserve visual function were considered as responsive to treatment. Visual acuity, color sensitivity, visual field, and optic discs were analyzed at 2 and 4 weeks, and at 3, 6, and 12 months after treatment. Activity of GO was graded using a clinical activity score (CAS). Visual and clinical characteristics of the eyes responsive to iv-MP were studied by comparison with those of nonresponsive eyes. Results: At 6 months, 17 of 40 (42.5%) eyes had complete visual recovery and were spared from surgical decompres-sion. At 2 weeks, visual acuity, color sensitivity, and visual field improved significantly in almost all eyes, but GO inactivated (CAS ,4) only in the eyes that permanently re-sponded to iv-MP (P , 0.01). The CAS at 2 weeks was a good predictor of response (cutoff $4; 66.7% sensitivity, and 76.9% specificity). Optic disc swelling at diagnosis was highly predictive for unresponsiveness to iv-MP (34% sensi-tivity, 100% specificity). At baseline, high CAS (cutoff .5; 40.2% sensitivity, and 94.1% specificity) and severely altered visual field mean defect (cutoff #6.31 dB; 73.9% sensitivity, and 58.8% specificity) were associated with unresponsive-ness to steroids. No major side effects were observed. Conclusions: High-dose iv-MP was effective in permanently restoring visual function in about 40% of the eyes treated. When successful, it generally induced inactivation of the orbital disease within 2 weeks and normalization of visual function within 1 month. The presence of optic disc swelling at diagnosis and persistent active disease at 2 weeks were good predictors of unresponsiveness to steroids. There is little written about the use of pulsed doses of methylprednisolone in dysthyroid optic neuropathy (DON) and although this is a retrospective, nonrandomized, and noncontrolled study, it adds some useful clinical informa-tion that is quite practical. Twenty-four patients with DON received IV steroids (either 500- or 1000-mg pulsed methylprednisolone) daily for 3 days and repeated 1 week later, followed by an oral or IV taper. The primary outcome was "not requiring decom-pressive surgery by 6 months later." Forty-two percent (17 of 40 eyes) were able to avoid surgery with complete recov-ery and no further relapse, but the time of final follow-up is not mentioned. Three patients had 1 eye responsive and the other requiring surgery (12.5%). Two features predicted a poor response to the pulsed steroid therapy. Those with optic disc edema at presentation failed and required surgery. Additionally, by using the clinical activity score (CAS), 70% of those with still active disease at 2 weeks required surgery, compared with only 20% with CAS inactive disease. The CAS is the sum of 10 items: 2 symptoms (orbital pain at rest or with eye movement), 5 signs of orbital inflammation and/or conges-tion (soft tissue swelling, lid redness, conjunctival redness, chemosis, and swelling of the caruncle), and 3 signs of deterioration (worsening of proptosis, ductions, and visual acuity). Active disease was defined as $4/10. Despite its obvious limitations, this article has some practical information we can use in the office today. First, some patients with DON may have an excellent response to pulsed steroids. Second, if disc edema is present, response is likely to be poor. Finally if disease activity as measured by CAS is still present at 2-week posttreatment, long-term response is less likely. -Mark L. Moster, MD I find it interesting that smoking did not make a difference in who did or did not improve with pulsed steroids. Also, buried in the data is that those eyes that did not respond initially to steroids and went on to have an orbital decompression ended the study with worse visual acuity, mean deviation, and color vision than those who responded to steroids. At baseline, nonresponders had significantly worse mean deviation but similar visual acuity and color vision. This begs the question: would the nonresponding eyes have fared better if they had surgery right away? We do not have the answer based on this study, which is why a large prospective trial comparing the 2 modalities would be helpful. If one does not have easy access to a good orbital surgeon with a lot of experience decompressing the posterior orbit or if there are relative contraindications to surgery, then I think pulsed intravenous steroids could be a reasonable initial option for management of DON. -Michael S. Lee, MD Klink T, Geiger J, Both M, Ness T, Heinzelmann S, Reinhard M, Holl-Ulrich K, Duwendag D, Vaith P, Bley TA. Giant cell arteritis: diagnostic accuracy of MR imaging of superficial cranial arteries in initial diagnosis-results from a multicenter trial. Radiology. 2014. Epub ahead of print. Purpose: To assess the diagnostic accuracy of contrast material-enhanced magnetic resonance (MR) imaging of superficial cranial arteries in the initial diagnosis of giant cell arteritis (GCA). Materials and Methods: After institutional review board approval and informed consent, 185 patients suspected of having GCA were included in a prospective 3 university medical center trial. GCA was diagnosed or excluded clinically in all patients (reference standard [final clinical diagnosis]). In 53% of patients (98 of 185), temporal artery biopsy (TAB) was performed (diagnostic standard [TAB]). Two observers independently evaluated contrast-enhanced T1-weighted MR images of superficial cranial arteries by using a 4-point scale. Diagnostic accuracy, involvement pattern, and systemic corticosteroid (sCS) therapy effects were assessed in comparison with the reference standard 418 Moster and Lee: J Neuro-Ophthalmol 2014; 34: 417-421 Literature Commentary Copyright © North American Neuro-Ophthalmology Society. Unauthorized reproduction of this article is prohibited. (total study cohort) and separately in comparison with the diagnostic standard TAB (TAB subcohort). Statistical analy-sis included diagnostic accuracy parameters, interobserver agreement, and receiver operating characteristic analysis. Results: Sensitivity of MR imaging was 78.4% and speci-ficity was 90.4% for the total study cohort, and sensitivity was 88.7% and specificity was 75.0% for the TAB subcohort (first observer). Diagnostic accuracy was comparable for both observers, with good interobserver agreement (TAB subcohort, k = 0.718; total study cohort, k = 0.676). MR imaging scores were significantly higher in patients with GCA-positive results than in patients with GCA-negative re-sults (TAB subcohort and total study cohort, P , 0.001). Diagnostic accuracy of MR imaging was high in patients without and with sCS therapy for 5 days or fewer (area under the curve, $0.9) and was decreased in patients receiving sCS therapy for 6-14 days. In 56.5% of patients with TAB-positive results (35/62), MR imaging displayed symmetrical and simultaneous inflammation of arterial segments. Conclusions: MR imaging of superficial cranial arteries is accurate in the initial diagnosis of GCA. Sensitivity probably decreases after more than 5 days of sCS therapy; thus, imaging should not be delayed.Clinical trial registration number: DRKS00000594. Patients suspected of having giant cell arteritis (GCA) underwent neuroimaging and masked reviewers evaluated the magnetic resonance imaging (MRI) for temporal and occipital artery mural thickening and enhancement. About half went on to have a temporal artery biopsy (TAB). Positive scans showed a sensitivity of approximately 80% and a specificity of approximately 87% for the entire cohort. The sensitivity and specificity were very different based on whether the diagnosis was made with or without a TAB. Looking at the group that underwent TAB, the sensitivity of MRI was about 90% and specificity was 75%. Among the subgroup that did not have a TAB, MRI sensitivity was about 64% and specificity was about 91%. I averaged the numbers for the 2 masked graders to calculate the values for sensitivity and specificity. Many older patients that present with visual loss or headache undergo a contrast-enhanced MRI of the head before they are referred to the neuro-ophthalmologist, and it seems worthwhile to look at the temporal and occipital arteries. Looking carefully at the MRI, one might choose to biopsy the artery that shows thickening and enhancement. A positive scan could also "tip the balance" for the clinician facing a biopsy-negative diagnosis of GCA. Certainly, MRI cannot replace TAB, but neuroimaging shows fair sensitivity and specificity and could represent another helpful adjunctive diagnostic test. -Michael S. Lee, MD MRI of the temporal and occipital arteries is a relatively noninvasive technique that makes sense for patients undergo-ing MRI anyway. I agree it will not replace TAB, and if an MRI is not planned, I would be reluctant to recommend it because MRI results should not deter the performance of a TAB. I think it will have a role as an ancillary test, such as intravenous fluorescein angiography or orbital color Doppler. It is interesting that the sensitivity of MRI was much lower in those diagnosed without a TAB in this study. Perhaps, these patients who have not been biopsied and were diagnosed by clinical criteria really do not have GCA. -Mark L. Moster, MD Lee J, Kim SW, Lee SC, Kwon OW, Kim YD, Byeon SH. Co-occurrence of acute retinal artery occlusion and acute ischemic stroke: diffusion-weighted magnetic resonance imaging study. Am J Ophthalmol. 2014;157:1231-1238. Purpose: To evaluate the co-occurrence of acute ischemic stroke and acute retinal artery occlusion (RAO). Design: Retrospective observational case series. Methods: We included 33 consecutive patients with acute RAO who underwent diffusion-weighted MRI within 7 days of the onset of visual symptoms. The causes of RAO were classified according to the Trial of Org 10172 in Acute Stroke Treatment (TOAST) criteria, which are based on clinical fea-tures and the results of etiological evaluations for athero-sclerosis, cardioembolism, and other prothrombotic conditions. We evaluated the prevalence of accompanying acute ischemic stroke in subjects with acute RAO and examined the relationships with etiological parameters. Results: Acute ischemic stroke was detected in 8 (24.2%) subjects with RAO. Among these subjects, 3 (37.5%) patients did not exhibit any neurologic symptoms or signs. Most of the infarction patterns were small, multiple, and scattered. All of the subjects with RAO who were positive for lesions on diffusion-weighted imaging (DWI) had identifiable causes, whereas only 36% of the subjects who were negative for le-sions had identifiable etiologies (P = 0.003). Carotid stenosis or cardioembolic sources were found more commonly in cases of central retinal artery occlusion (7/18, 38.9%) than in cases of branch retinal artery occlusion (1/15, 6.7%, P = 0.046). Conclusions: Acute cerebral infarctions frequently accom-pany RAO. We recommend DWI for patients with RAO, because the presence of lesions on DWI is accompanied by a significantly increased probability of identifying the cause. This study demonstrates that asymptomatic cerebral ische-mia seen on MRI with diffusion-weighted imaging (DWI) may accompany retinal artery ischemia, both central retinal artery occlusion (CRAO) and branch retinal artery occlusion (BRAO). The presence of cerebral ischemia was more often associated with a definitive etiology being found for the ischemia, such as embolic cardiac disease. This and previous findings in other studies showing that asymptomatic brain infarcts are associated with an increased risk of subsequent clinical infarct prompt the authors to recommend MRI with DWI on all patients with retinal artery occlusion (RAO). This concurs with the American Heart Association/American Stroke Association guidelines, which do not distinguish retinal artery ischemia from hemispheric ischemia. The recommendations that patients with RAO be evaluated at an emergency room or outpatient stroke unit Moster and Lee: J Neuro-Ophthalmol 2014; 34: 417-421 419 Literature Commentary Copyright © North American Neuro-Ophthalmology Society. Unauthorized reproduction of this article is prohibited. rather than a nonemergent elective outpatient workup make sense and are appropriately amplified in the accompanying editorial by Biousse (1). However if one does not read the article carefully, one can be misled into thinking that 24.2% of patients with isolated BRAO or CRAO have acute ischemic stroke. Indeed, 5 of the 8 patients in this study with DWI changes had hemispheric brain symptoms as well, most often unilateral weakness. Despite this possible overestimation of asymptomatic cerebral ischemia, it is important for the oph-thalmologic and neurologic communities to take transient or permanent monocular visual loss more seriously and treat it as an emergency, similar to cerebral transient ischemic attack or infarct. -Mark L. Moster, MD A patient of mine lost visual field in 1 eye and received a diagnosis of branch RAO from a retina specialist. The ophthalmologist asked the patient to see his primary care doctor for an embolic workup. Two days later, he suffered an occipital lobe stroke and now cannot legally drive. Needless to say, he is devastated. He might have experienced the second stroke even if the RAO were investigated and managed urgently, but the risk could have been reduced. It is extremely common for ophthalmologists to regard RAO as nonurgent. We surveyed neurologists about acute RAO ,48 hours old, and less than half would pursue an urgent evaluation for stroke (2). Therefore, even if an oph-thalmologist sent the patient for an urgent evaluation, the consulting neurologist may not deem it so. The North American Symptomatic Carotid Endarterectomy Trial (NASCET) emphasized that amaurosis fugax shows lower risk of subsequent stroke. This may contribute to the feeling that retinal ischemia is less concerning. Whatever the rea-son, I think it suggests a need for better education for both specialties, and neuro-ophthalmologists are in a unique position to help with both. -Michael S. Lee, MD REFERENCES 1. Biousse V. Acute retinal arterial ischemia: an emergency often ignored. Am J Ophthalmol. 2014;157:1119-1121. 2. Abel AS, Carpenter SR, Hussein HM, Lee MS. Practice patterns following retinal artery occlusion. Poster presented at: Annual meeting of the North American Neuro-ophthalmology Society; March, 2014; San Juan, PR. Wang X, Jia Y, Spain R, Potsaid B, Liu JJ, Baumann B, Hornegger J, Fujimoto JG, Wu Q, Huang D. Optical coherence tomography angiography of optic nerve head and parafovea in multiple sclerosis. Br J Ophthalmol. 2014;98:1368-1373. Aims: To investigate swept-source optical coherence tomography (OCT) angiography in the optic nerve head (ONH) and parafoveal regions in patients with multiple sclerosis (MS). Methods: Fifty-two MS eyes and 21 healthy control (HC) eyes were included. There were 2 MS subgroups: 38 MS eyes without an optic neuritis (ON) history (MS-ON) and 14 MS eyes with an ON history (MS + ON). The OCT images were captured by high-speed 1050-nm swept-source OCT. The ONH flow index (FI) and parafoveal FI were quantified from OCT angiograms. Results: The mean ONH FI was 0.160 ± 0.010 for the HC group, 0.156 ± 0.017 for the MS-ON group, and 0.140 ± 0.020 for the MS + ON group. The ONH FI of the MS + ON group was reduced by 12.5% compared with HC eyes (P = 0.004). A higher percentage of MS + ON eyes had abnormal ONH FI compared with HC (43% vs 5%, P = 0.01). Mean parafoveal FIs were 0.126 ± 0.007, 0.127 ± 0.010, and 0.129 ± 0.005 for the HC, MS-ON, and MS + ON groups, respectively, and did not differ significantly among them. The coefficient of variation (CV) of intravisit repeatability and intervisit reproducibility were 1.03% and 4.53% for ONH FI, and 1.65% and 3.55% for parafoveal FI. Conclusions: Based on OCT angiography, the FI measure-ment is feasible and highly repeatable and reproducible, and it is suitable for clinical measurement of ONH and parafoveal perfusion. The ONH FI may be useful in detecting damage from ON and quantifying its severity. Optical coherence tomography (OCT) in patients with a history of MS and optic neuritis (ON) can show retinal nerve fiber layer or inner plexiform/ganglion cell layer thinning. In addition to these structural deficiencies, it has also been proposed that ON and multiple sclerosis (MS) may affect ocular perfusion. Existing techniques including fluorescein angiography, laser Doppler flowmetry, and color Doppler imaging tend to be qualitative or lack precision and repeatability. Wang et al describe a prototypical custom OCT imaging algorithm of the intraocular vasculature called OCT angiog-raphy. This noninvasive imaging technique acquires approx-imately 1600 B-scans in ,3.5 seconds. OCT angiography differentiates between moving and static tissue with the mov-ing tissue presumed to be flowing blood. The area of the large and capillary vessels can be averaged into a dimensionless number between 0 and 1 called flow index (FI). In this study, the authors measure the FI from the optic nerves and the parafoveal region in eyes of healthy controls (HCs) and patients with MS. The MS eyes were divided into those with and without a history of ON. There was no difference in the FI among the 3 groups in the parafoveal retina. The MS eyes without ON and HCs showed no difference in the flow indices of the optic disc. The MS eyes with ON showed a statistically significant reduction in FI of the optic disc compared with the other 2 groups. I think this could suggest that MS alone does not cause substantial ocular vascular injury but ON may affect the capillary flow to the optic disc. OCT angiography provides high-resolution images of the large and capillary vessels of the optic disc and retina. Although it is not yet clear of its ongoing utility in MS, I am excited about its potential application in other optic nerve 420 Moster and Lee: J Neuro-Ophthalmol 2014; 34: 417-421 Literature Commentary Copyright © North American Neuro-Ophthalmology Society. Unauthorized reproduction of this article is prohibited. and retinovascular disorders. The level of quantitation, repeatability, and image registration holds great promise for monitoring change over time. Unfortunately, it is not yet widely available. -Michael S. Lee, MD Noninvasive angiography of optic nerve and retina will be a welcome addition for clinical and research purposes in a whole host of ocular and neurologic disorders. Not surprisingly, blood flow in the optic nerve is decreased after ON. However, in this study, even with highly skilled technical personnel who developed this OCT technique, many eyes had to be excluded for technical reasons. As the resolution of commercially available OCTs continue to improve, these techniques should become more reliable and clinically valuable. -Mark L. Moster, MD Siddiqui AH, Zivadinov R, Benedict RH, Karmon Y, Yu J, Hartney ML, Marr KL, Valnarov V, Kennedy CL, Ramanathan M, Ramasamy DP, Dolic K, Hojnacki DW, Carl E, Levy EI, Hopkins LN, Weinstock-Guttman B. Prospective randomized trial of venous angioplasty in MS (PREMiSe). Neurology. 2014;83:441-449. Objective: We report the results of the investigation of safety and efficacy of venous angioplasty in patients with multiple sclerosis (MS) with findings of extracranial venous anomalies, considered hallmarks of chronic cerebrospinal venous insufficiency (CCSVI), in a 2-phase study (ClinicalTrials.gov: NCT01450072). Methods: Phase 1 was an open-label safety study (10 pa-tients); phase 2 was sham-controlled, randomized, and double-blind (10 sham procedure, 9 treated) study. All study patients fulfilled venous hemodynamic screening criteria indicative of CCSVI. Assessment was at 1-, 3-, and 6-month postprocedure with MRI, clinical, and hemodynamic out-comes. Primary end points were safety at 24 hours and 1 month, venous outflow restoration .75% at 1 month, and effect of angioplasty on new lesion activity and relapse rate over 6 months. Secondary end points included changes in disability, brain volume, cognitive tests, and quality of life. Results: No perioperative complications were noted; how-ever, 1 patient with history of syncope was diagnosed with episodic bradycardia requiring placement of a pacemaker before discharge. Doppler evidence-based venous hemody-namic insufficiency severity score (VHISS) was reduced .75% compared with baseline in phase 1 (at 1 month) but not phase 2. In phase 2, higher MRI activity (cumulative number of new contrast-enhancing lesions [19 vs 3, P = 0.062] and new T2 lesions [17 vs 3, P = 0.066]) and relapse activity (4 vs 1, P = 0.389) were identified as non-significant trends in the treated versus sham arm over 6 months. Using analysis of covariance, significant cumu-lative new T2 lesions were related to larger VHISS decrease (P = 0.028) and angioplasty (P = 0.01) over the follow-up. No differences in other end points were detected. Conclusions: Venous angioplasty is not an effective treat-ment for MS over the short term and may exacerbate underlying disease activity. Classification of Evidence: This is a Class I study demon-strating that clinical and imaging outcomes are no better or worse in patients with MS identified with venous outflow restriction who receive venous angioplasty compared with sham controls who do not receive angioplasty. This study also includes a Class IV phase 1 study of safety in 10 patients receiving the angioplasty procedure. In 2009, Zamboni et al (1) published an unmasked study showing that 90% of patients with MS have venous outflow abnormalities in the internal jugular and/or azygos vein and that angioplasty improved clinical and MRI outcomes. The condition is known as chronic cerebrospinal venous insuffi-ciency (CCSVI). Since then, many other articles have come out, mostly not supportive of the original study. In 2012, the FDA issued a warning about the lack of proof of benefit and the dangers of the procedure, including stroke and death. Interventional radiologists and others have performed venous angioplasty on thousands of patients worldwide. The Prospective Randomized Trial of Venous Angioplasty in MS (PREMiSe) trial is the first randomized double-blind trial to compare venous angioplasty with a sham angioplasty for patients with findings of CCSVI. The findings showed no clinical benefit at 6 months for the treatment. In fact, there was a trend towards increased MRI disease activity in those receiving the treatment. Additionally, self-reported im-provements were seen in the sham group and the treated group, suggesting a placebo effect of treatment. Although a small study of only 19 patients, it is the first to provide Class I evidence against venous angioplasty for MS and unless proven beneficial in future Class I studies, the procedure is likely should be abandoned. -Mark L. Moster, MD I am thrilled to see the results of this rigorous study. In the September 2010 "Literature Commentary," we expressed our doubt that CCSVI truly causes MS and that treating it would benefit patients. I would hope that the issue has been laid to rest based on the outcome of this study and for other reasons including: 1) lack of consistent benefit from retrospective stud-ies, 2) lack of a strong pathoetiologic argument, and 3) signif-icant potential risk of angioplasty. Although the numbers were small in this study, it would seem unlikely to me that others would attempt another clinical trial of this sort. -Michael S. Lee, MD REFERENCE 1. Zamboni P, Galeotti R, Menegatti E, Malagoni AM, Gianesini S, Bartolomei I, Mascoli F, Salvi F. A prospective open-label study of endovascular treatment of chronic cerebrospinal venous insufficiency. J Vasc Surg. 2009;50:1348-1358.e1-e3. Moster and Lee: J Neuro-Ophthalmol 2014; 34: 417-421 421 Literature Commentary Copyright © North American Neuro-Ophthalmology Society. Unauthorized reproduction of this article is prohibited. |