| OCR Text |
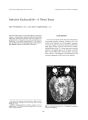
Show Journal of Neuw- Ophthalmologij 16( 4): 258- 263, 1996. 1996 Lippincott- Raven Publishers, Philadelphia Bilateral Ptosis due to Mesencephalic Lesions with Relative Preservation of Ocular Motility Timothy J. Martin, M. D., James J. Corbett, M. D., Paul V. Babikian, M. D., Stephen C. Crawford, M. D., and Robert D. Currier, M. D. Three cases of bilateral ptosis with relatively normal ocular motility are presented. In two of the patients, neu-roimaging demonstrated lesions in the region of the third cranial nerve subnuclei. These unusual clinical presentations are due to isolated involvement of the central caudal nucleus supplying the bilateral levator muscles, with, virtually complete sparing of other third cranial nerve structures. Key Words: Ptosis- Bilateral- Third cranial nerve- Central caudal nucleus. In 1953, Warwick demonstrated that the oculomotor nucleus in monkeys is arranged as discrete subnuclei, with the central caudal nucleus providing a common output to both levator palpebrae muscles ( 1). We present three cases of bilateral ptosis with relative preservation of other third cranial nerve functions. Magnetic resonance imaging ( MRI) demonstrated lesions in the area of the third- nerve nuclear complex in two patients. The third patient had definite multiple sclerosis and scattered white- matter lesions, although no lesion was visible in the third- nerve complex on neuroim-aging. We suggest that the bilateral ptosis in each of these cases is secondary to relatively isolated involvement of the central caudal nucleus, thus providing further clinical evidence that Warwick's scheme of oculomotor nuclear organization holds true for humans. CASE REPORTS Manuscript received September 27, 1995; accepted November 30, 1995. From the Department of Ophthalmology, Bowman Gray School of Medicine/ Wake Forest University ( T. J. M.), Department of Neurology, University of Mississippi ( J. J. C., S. C. C., R. D. C.), Department of Radiology, University of Mississippi ( S. C. C.), and private practice ( P. V. B.), Wichita, Kansas, U. S. A. T. J. M. and J. J. C. were with the Departments of Ophthalmology and Neurology, University of Iowa Hospitals and Clinics, during the inception of this paper. Case 1 A 67- year- old man was unable to open his eyes when he awoke in the morning. Eleven years earlier, he had had a posterior fossa arachnoid cyst with hydrocephalus that was treated with a cyst-peritoneal shunt, resulting in a gaze- directed nystagmus. He had a history of esotropia and amblyopia of the left eye. One year before his presentation with ptosis, he developed cervical and inguinal lymphadenopathy, and a cervical lymph node biopsy demonstrated non- Hodgkin large- cell lymphoma. Bone marrow biopsy and chest and abdominal computed tomography ( CT) were negative. He was treated with seven cycles of cyclophosphamide, doxorubicin, vincristine, and prednisone ( CHOP), and was judged to be in complete remission. 258 BILATERAL PTOSIS WITH NORMAL OCULAR MOTILITY 259 Examination of cranial nerves II- VII yielded otherwise normal findings. Extremity strength and sensation were normal. He had slight dysmetria bilaterally and a wide- based ataxic gait. Cranial CT demonstrated postoperative changes in the posterior fossa, where a large cyst communicated with the fourth ventricle. The shunt was functioning normally. MRI of the brain showed abnormal signal intensity in the periaqueductal area on T2- weighted imaging, which was enhanced by the administration of gadolinium ( Fig. 3), with additional enhancement in the left globus pallidus and the floor of the third ventricle. All blood studies, electrocardiography, and chest radiography were unremarkable. Cerebrospinal fluid had nine lymphocytes per mm3 with normal cytology. Cerebrospinal fluid protein, glucose, and cryptococcal antigen were all normal, and there was no growth on routine and fungal cultures. A repeat lumbar puncture 24 h later yielded normal findings. Edrophonium chloride ( 10 mg) was administered, but did not improve the ptosis. Although the ptosis improved considerably over the next several weeks, within a month, the patient had developed lower extremity weakness and ataxia. Subsequent MRI revealed additional en- FIG. 2. Case 1. Relatively normal ocular motility, except for a right abduction deficit ( longstanding), and a moderate upgaze deficiency. / Neuro- Ophthalmol, Vol. 16, No. 4, 1996 • A Case 1. Bilateral complete ptosis. At examination, he had complete bilateral ptosis ( Fig. 1). Motility was normal with the exception of a ( longstanding) mild right abduction deficit and moderately deficient upgaze ( Fig. 2). Downbeat nystagmus was present in the primary position. Visual acuity was 20/ 50 in the right eye and 20/ 300 in the amblyopic left eye; slit- lamp examination showed mild bilateral cataracts. Visual fields were full to confrontation. The ophthalmoscopic examination yielded normal findings. The pupils were 2 mm bilaterally and constricted to light and near, and there was no relative afferent pupillary defect. 260 T. /. MARTIN ET Ah. FIG. 3. Case 1. A: MRI demonstrates abnormal signal intensity in the periaqueductal grey matter on T2- weighted imaging, [ echo time ( TE) 100, resonance time ( TR) 2000]. The abnormality is not visible on T1 imaging ( TE 20, TR 535), but is evident with gadolinium enhancement ( B). hancing lesions in the brain, and a stereotactic biopsy confirmed the presence of lymphoma. Whole- brain irradiation was initiated, but progressive neurologic deterioration resulted in his death 8 months later. Case 2 A 70- year- old woman with known breast cancer metastatic to the brain presented with a 6- week history of increasing difficulty in opening her eyes. She had been admitted to the neurosurgery service 5 months earlier because of increasing headache, memory loss, and ataxia; at that time, MRI revealed a cystic mass in the region of the quad-rigeminal plate with compression of the Sylvian aqueduct and secondary hydrocephalus of the third and lateral ventricles. She had a vertical gaze disturbance, but no ptosis. Placement of a ventric-uloperitoneal shunt resolved her symptoms. Further workup revealed an infiltrating ductal carcinoma in the left breast that was treated with a modified radical mastectomy; none of nine biopsied lymph nodes was positive. The brainstem lesion, presumably metastatic, was treated with radiation therapy ( a total of 3,500 rads in 14 fractions to the whole brain). On presentation, the patient reported that she had not been able to see for the prior 6 weeks without manually holding her eyelids open, and that her vision was somewhat blurred; both the ptosis and the blurring were worse in the morning and improved somewhat as the day progressed. She had no complaints of headache, nausea, vomiting, diplopia, or systemic weakness. Dexameth-asone tablets, which she had begun taking 4 weeks before her visit, had helped the ptosis, which was always present to some degree. Current medications included prazosin hydrochloride for systemic hypertension, oxazepam, and dexamethasone. On examination, she had bilateral ptosis slightly greater on the right ( Fig. 4), with full ocular motility ( Fig. 5). Visual acuity was 20/ 20 in both eyes, FIG. 4. Case 2. Bilateral complete ptosis. / Neuro- Ophthalmol, Vol. 16, No. i, 1996 BILATERAL PTOSIS WITH NORMAL OCULAR MOTILITY 261 • -*^& tf2& ltLL • V **&> / '- v^ t- * FIG. 5. Case 2. Normal motility. The eyelids are held open with tape. with normal findings on pupillary examination, visual field, slit- lamp, and fundus examinations. MRI revealed a 1.5- cm cystic mass, associated with the quadrigeminal plate with a midbrain signal abnormality ( Fig. 6), but there was no obvious progression from her previous scans. Over the next 4 months, her ptosis became more profound and was accompanied by decreased hearing and speech difficulties. Neuroimaging then showed marked enlargement and progression of the midbrain mass, and the patient underwent a left occipital craniotomy via a transtentorial approach to the pineal region for debulking of the tumor, followed by additional radiation to the brain, chemotherapy, and hormone therapy. Her profound bilateral ptosis was present until her death, which occurred 7 months after her initial presentation. Case 3 A 41- year- old woman with a 9- year history of relapsing/ remitting multiple sclerosis presented with increasing bilateral ptosis for 2 days. She had no diplopia, and neurological review of systems showed no abnormal findings other than chronic intermittent paresthesias of the face and limbs. She had episodic urinary incontinence, as well as an optic neuritis in the right eye that had developed 2 years earlier. She had taken cyclophosphamide and methotrexate in the past; at presentation, she was taking 20 mg/ day of prednisone. Neuro- ophthalmic and neurologic examinations showed no abnormalities other than bilateral flaccid ptosis ( Figs. 7 and 8). Administration of edrophonium chloride did not alter her ptosis. MRI of the brain showed abnormal signal within the periventricular white matter, superior to the frontal horns, adjacent to the left occipital horn, and within the left substantia nigra and parietooccipital area. No periaqueductal mesencephalic lesion could be identified. Lumbar puncture showed no abnormalities. The patient's ptosis was believed to be secondary to an exacerbation of her multiple sclerosis, and she was admitted to the hospital for a course of parenteral adrenocorticotrophic hormone ( 80 U/ day). Within 2 days, improvement in lid function was noted, and within a week, her ptosis had / Neuro- Ophthalmol, Vol 16, No. 4, 1996 262 T. ]. MARTIN ET AL. FIG. 6. Case 2. A: MRI at presentation demonstrates a cystic mass in intimate association with the quad-rigeminal plate on sagittal T1 image ( TE 25, TR 535). B: Axial T2 image ( TE 100, TR 2000) shows the periaqueductal midbrain signal abnormality produced by the mass and surrounding edema, and hydrocephalus with presumed transependymal flow of cerebrospinal fluid ( CSF). disappeared. Although she has had additional exacerbations of multiple sclerosis during the 4 years since her initial presentation, she has had no recurrence of her ptosis. DISCUSSION Warwick's studies using retrograde chromatoly-sis of the cells of the oculomotor complex of monkeys demonstrated discrete subnuclei, arranged in a rostro- caudal fashion ( 1). A central caudal nucleus provided bilateral innervation to the levator palpebrae muscles. Other subnuclei, serving the parasympathetic innervation to the pupillary sphincter, the inferior oblique, as well as to the medial, inferior, and superior recti, were paired, innervating ipsilateral third cranial nerve components. Paired superior rectus subnuclei had decussating efferent outflow, innervating the superior rectus contralaterally. There is ample clinical evidence to suggest a similar arrangement in humans, with reports of discrete periaqueductal midbrain lesions affecting certain third- nerve functions while entirely sparing others ( 2- 8). In addition to our three cases, we have discovered additional reports of relatively isolated midbrain ptosis, beginning with Stevenson and Hoyt's description of bilateral ptosis associated with minimal adduction weakness in the left eye of a patient with breast cancer metastatic to the midbrain ( 9). Conway et al. ( 6) described a 45- year- old man with isolated bilateral ptosis, who had discrete inflammatory lesions in the brain and brainstem and a lesion in the dorsal, midline aspect of the oculomotor complex. Meienberg et al. ( 10) reported the case of a 65- year- old man with apparent brainstem ischemia who eventually developed a " locked- in syndrome," but, at one point, exhibited bilateral ptosis with normal eye movements. Beck and Smith ( 11) described a 24- year- old man with bilateral ptosis and 4 diopters of left hypertropia on right gaze. MRI showed a mass in the region of the third nerve nucleus, presumed to be a brainstem glioma. Barton et al. ( 12) discusses a patient with acquired immune deficiency syndrome ( AIDS) who presented with the acute onset of a bilateral complete ptosis and minimal vertical gaze disturbance. Neuroimaging revealed a periaqueductal FIG. 7. Case 3. Bilateral ptosis. / Neuro- Ophthatmol, Vol. 16, No. 4, 1996 BILATERAL PTOSIS WITH NORMAL OCULAR MOTILITY 263 FIG. 8. Case 3. midbrain lesion ( thought to be impinging on the central caudal subnucleus) and bilateral masses in the caudate nuclei. Neuropathology revealed that the midbrain lesion was most consistent with AIDS encephalopathy, although the caudate lesions showed lymphoma of B- cell origin. We propose that the bilateral ptoses in our three patients were caused by lesions involving the median group of nerve cells supplying both levator muscles, i. e., the central caudal nucleus, with relative sparing of the remainder of the oculomotor subnuclei. In the first patient, recurrence of central nervous system ( CNS) lymphoma was demonstrated, with a lesion in the periaqueductal gray matter. In the second patient, a metastatic breast lesion to the midbrain tectum was identified, with compression of the dorsal aspect of the oculomotor nuclear complex. In the third patient, who had definite multiple sclerosis, many white matter plaques were demonstrated on MRI, although a discrete plaque in the region of the central caudal nucleus/ fascicles could not be seen with neuroim-aging. The existence of such a lesion seems reasonable, however, as small active plaques frequently are not shown on MRI, and no other lesion or process can adequately explain the patient's symptoms. Furthermore, the remitting nature of the ptosis is consistent with multiple sclerosis. Generally, lesions of the oculomotor complex affect multiple functions. The discreteness of the effect of a lesion on a single midline nucleus might suggest a vascular mechanism. However, as in our three cases, nonvascular causes represent the ma- Normal motility. jority of reported cases of isolated midbrain ptosis, suggesting that there may be some structural predisposition of this nucleus to the effects of intrinsic lesions at this location. REFERENCES 1. Warwick R. Representation of the extraocular muscles in the oculomotor nuclei of the monkey. ] Comp Neurol 1953; 98: 449- 95. 2. Biller ], Shapiro R, Evans LS, et al. Oculomotor nuclear complex infarction. Clinical and radiologic correlation. Arch Neurol 1984; 41: 985- 7. 3. Growdon JH, Winkler GF, Wray SH. Midbrain ptosis. A case with clinicopathologic correlation. Arch Neurol 1974; 30: 179- 81. 4. Keane JR, Zaias B, Itabashi HH. Levator- sparing oculomotor nerve palsy caused by a solitary midbrain metastasis. Arch Neurol 1984; 41: 210- 2. 5. Pusateri TJ, Sedwick LA, Margo CE. Isolated inferior rectus muscle palsy from a solitary metastasis to the oculomotor nucleus. Arch Ophthalmol 1987; 105: 675- 7. 6. Conway VH, Rozdilsky B, Scheider RJ, Sundaram M. Iso lated bilateral complete ptosis. Can / Ophthalmol 1983; 18: 37- 40. 7. Caplan LR, Zervas NT. Survival with permanent midbrain dysfunction after surgical treatment of traumatic subdural hematoma: The clinical picture of a duret hemorrhage? Ann Neurol 1977; 1: 587- 9. 8. Liu GT, Carrazana EJ, Charness ME. Unilateral oculomotor palsy and bilateral ptosis from paramedian midbrain infarction. Arch Neurol 1991; 48: 983- 6. 9. Stevenson GC, Hoyt WF. Metastasis to midbrain from mammary carcinoma. JAMA 1963; 186: 514- 6. 10. Meienberg O, Mumenthaler M, Karbowski I. Quadriparesis and nuclear oculomotor palsy with total bilateral ptosis mimicking coma. A mesencephalic Tocked- in syndrome'? Arch Neurol 1979; 36: 708- 10. 11. Beck RW, Smith CH. Neuro- ophthalmology: a problem-oriented approach. Boston: Little, Brown, and Company, 1988: 229. 12. Barton JJS, Kardon RH, Slagel D, Thompson HS. Bilateral central ptosis in acquired immunodeficiency syndrome. Can ] Neurol Sci 1995; 22: 52- 5. / Neuro- Ophtlmlmol, Vol. 16, No. 4, 1996 |