| OCR Text |
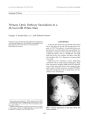
Show Journal of Ncuro- Ophtlialmology 16( 3): 208- 211, 1996. © 1996 Lippincott- Raven Publishers, Philadelphia Pseudotumor Associated With CNS Lymphoma Henry L. Hudson, M. D., David R. Hinton, M. D., Deborah I. Friedman, M. D., Michael Apuzzo, M. D., Para Chandrasoma, M. D., Mark Garbut, M. D., and Steven E. Feldon, M. D. A 42- year- old immune- competent woman with orbital pseudotumor and presumed intracranial extension into the temporal lobe responded well clinically and radio-logically to high- doses of corticosteroids. Five months later, she developed worsening headaches and recurrence of the temporal lobe lesion. Biopsy revealed a central nervous system ( CNS) lymphoma with severe reactive gliosis abutting an area of subarachnoid lymphocytic infiltrate. Key Words: Pseudotumor- Lymphoma. Common signs of orbital pseudotumor are pro-ptosis, soft tissue swelling, and impairment of muscle motility; less commonly, patients may also develop headache, orbital pain, ocular discomfort, loss of vision, or a palpable mass. Intracerebral extension of orbital pseudotumor has been described only rarely in the literature ( 1- 3). We report a patient who had an inflammatory orbital pseudotumor with i n t r a c e r e b r a l i n v o l v e m e nt that responded well to steroid therapy. During follow-up, the patient developed a recurrent temporal lobe lesion, biopsy of which showed " collision" between a ( CNS) lymphoma and the inflammatory pseudotumor. CASE REPORT Manuscript received June 6, 1995; accepted November 30, 1995. From the Departments of Ophthalmology ( H. L. H., D. I. F., S. E. F.), Pathology ( D. R. H., P. C.), and Neurological Surgery ( M. A., S. E. F.), University of Southern California, Los Angeles, California; Riverside, California ( M. G.); and at State University of New York, Health Science Center, Syracuse, New York ( D. I. F.). Address correspondence and reprint requests to Dr. Steven E. Feldon, Doheny Eye Institute, 1450 San Pablo Street, Los Angeles, CA 90033, U. S. A. This material was presented in part at the Walsh Society Meeting, February 22, 23, 1991, Salt Lake City, Utah. A 42- year- old obese woman presented with a 20- day history of increasing proptosis, blurred vision, and painful ophthalmoplegia in the right eye. Clinical details are summarized in Table 1. The computed tomography ( CT) scan showed enhancement of the anterior portion of the right temporal lobe, right superior and inferior orbital fissures, orbital apex, and cavernous sinus ( Fig. 1). Magnetic resonance imaging ( MRI) revealed an area of increased signal intensity in the right temporal tip extending to the surface of the brain ( Fig. 2A). Tissue from an orbital biopsy of t h e lesion was consistent with inflammatory pseudotumor. The patient was treated with corticosteroids for 3 weeks. Complete resolution of ocular complaints occurred within 7 days. Repeat MRI 2 months later showed marked improvement of the orbital process and complete resolution of the temporal lobe process ( Fig. 2B). At 5 months after initial presentation, the pa- 709, PSEUDOTUMOR ASSOCIATED WITH CNS LYMPHOMA 209 TABLE 1. Results of ophthalmologic examination at time of referral Hertel Eye VA° Motility" ( mm) Optic nerve head APD Tangent screen OD 20/ 25 + 2 4A x T 8A HT 19 Moderate edema None Enlarged blind spot OS 20/ 20 - 1 Normal 14 Normal None Normal APD, afferent pupillary defect. " Uncorrected. b Extracellular motility OD was limited in all directions. tient developed headaches. Follow- up MRI showed increased signal in the right temporal lobe ( Fig. 2C); there was no recurrence of the orbital lesion. The temporal lobe lesion continued to expand over the next 6 months and the patient underwent a transcranial biopsy of the lesion. PATHOLOGY OF THE INTRACRANIAL LESION Examination of tissue from biopsy of the temporal lobe lesion revealed two distinct components: ( a) intense chronic inflammatory infiltrate in the subaranchoid space with reactive gliosis and prominent perivascular parenchymal infiltration into neuropil in the adjacent cortex and ( b) tumor composed of a neoplastic proliferation of atypical lymphoid cells showing prominent perivascular ringing and numerous mitoses in the subcortical white matter ( Fig. 3). The tumor cells infiltrated widely into the adjacent white matter where they elicited a prominent atypical astrocytic response. Reactive lymphocytic response was also present, FIG. 1. Axial view of a CT scan of the brain shows enhancement of the anterior portion of the right temporal lobe ( white arrow). most intense in the intervening cortex. Immuno-peroxidase staining clearly showed the neoplastic cells to be B- cell in origin ( CLA + , L26 + ). Immu-nostaining for glial acidic fibrillary protein, a marker of glial cells, identified a prominent atypical glial response. CLINICAL COURSE The patient was evaluated for the presence of systemic lymphoma; no evidence of lymphoma was found. She was treated with 3,000 rads of cranial irradiation and, after 5 years follow- up, was free of symptoms or evidence of recurrence. DISCUSSION Extension of inflammatory orbital pseudotumor to the brain is rare. An association between inflammatory orbital pseudotumor and brain lymphoma has not, to our knowledge, been reported. Possibly, the two lesions coexisted, with " collision" of pathology, or, perhaps, brain lymphoma induced an adjacent chronic inflammatory response. Alternatively, the initially reactive lesions may have evolved over time into a neoplastic lymphoid tumor ( 4). Differentiating between inflammatory pseudotumor and an orbital lymphoid neoplasm can be difficult, but the pain and decreased extraocular motility in this patient suggested pseudotumor ( 5). Pathology revealed only reactive fibrosis and minimal inflammatory cell infiltration ( 6). It is also possible that the brain lymphoma was the primary lesion and that the orbital inflammatory process represents an extension of, or reaction to, the CNS process. Extension of CNS lymphoma into the orbit is most unlikely, although intraocular involvement by such lymphomas is seen ( 7). However, monoclonal lymphomas of the CNS are often associated with a polyclonal infiltrate of reactive lymphocytes in the adjacent brain tissue and lep-tomeninges, and this process could induce reactive lymphocytic infiltration into the orbit. The patient's rapid response to steroids supports the possibility that the initial brain lesion rep- / Neiiw- Oyliilmlmol Vol. 16, No. 3, / 5) 5) 6 210 H. L, HUDSON ET AL. FIG. 2. A: MRI coronal view of the brain performed at the time of presentation shows an area of diffusely increased signal intensity in the light temporal tip that extends to the surface of the brain ( black arrow). B: Repeat MRI done 2 months later shows no evidence of the prior process. C: MRI performed 11 months after presentation shows a distinct area of increased signal intensity, which spares the cortical surface, in the right temporal lobe. All MRIs shown here are T- 2- weighted and gadolinium- enhanced. FIG. 3. Lymphoma cells are identified infiltrating through the brain tissue. Note the atypical reactive astrocytes ( A with arrow) with abundant cytoplasm, and the mitotic figure ( arrow). Hematoxylin and eosin x450). <£.&> I Neitm- Oplilhiilniol, Vol. 16, No. 3, 1996 PSEUDOTUMOR ASSOCIATED WITH CNS LYMPHOMA 211 resented intracerebral extension of the inflammatory pseudotumor. Although CNS lymphoma may regress ( 8,9) and, on occasion, even resolve ( 10) on corticosteroid therapy, recurrence of lymphoma in the brain would most likely have been accompanied by a similar recurrence in the orbit. In the present case, the extent of inflammatory infiltrate in the brain was excessive and was away from the tumor. It was adjacent to the orbital roof, thus suggesting the likely possibility that both orbital pseudotumor with intracranial extension and brain lymphoma coexisted and, in fact, collided pathologically. The incidence of primary CNS lymphoma is rising dramatically in both immunocompromised and immunocompetent individuals ( 11). The patient described in this report had no known immunode-pression and was human immunodeficiency virus ( HlV)- antibody negative. The coexistence of two rare lesions ( pseudotumor with CNS extension and brain lymphoma in an immunocompetent individual) in the context of an increasing incidence of CNS lymphoma suggests the possibility of a common etiology, such as an undetected infection by a lymphotropic virus with transforming ability. Acknowledgment: This work was supported in part by an award from Research to Prevent Blindness, Inc., New York, New York. REFERENCES 1. Kaye AH, Hahn JF, Cracium A, et al. Intracranial extension of inflammatory pseudotumor of the orbit: case report. / Neurosurg 1984; 60: 625- 9. 2. Noble SC, Chandler WF, Lloyd RV. Intracranial extension of orbital pseudotumor: a case report. Neurosurgery 1986; 18: 798- 801. 3. Frohman LP, Kupersmith MJ, Lang J, et al. Intracranial extension and bone destruction in orbital pseudotumor. Arch Ophthalmol 1986; 104: 380- 4. 4. Jakobicc FA, Neri A, Knowles DM II. Genotypic monoclon-ality in immunophenotypically polyclonal orbital lymphoid tumors: a model of tumor progression in the lymphoid system. The 1986 Wendell Hughes Lecture. Ophthalmology 1987; 97: 980- 94. 5. Mauriello JA, Jr, Flanagan JC. Pseudotumor and lymphoid tumor: distinct clinicopathologic entities. Surv Ophthalmol 989; 34: 142- 8. 6. Jakobiec FA. Orbital inflammations and lymphoid tumors. In: Symposium on diseases and surgery of the lids, lacrimal apparatus, and orbit. Transactions of the New Orleans Academy of Ophthalmology. St. Louis: CV Mosby, 1982: 52- 85. 7. Rockwood E), Zakov ZN, Bay JW. Combined malignant lymphoma of the eye and CNS ( reticulum- cell sarcoma): report of three cases. / Neurosurg 1984; 61: 369- 74. 8. Singh A, Strobos RJ, Singh I3M, et al. Steroid- induced remissions in CNS lymphoma. Neurology 1982; 32: 1267- 71. 9. Todd FD, Miller CA, Yates AJ, Mervis LJ. Steroid- induced remission in primary malignant lymphoma of the central nervous system. Surg Neurol 1986; 26: 79- 84. 10. Pohl P, Oberhuber G, Dietze O, et al. Steroid- induced complete remission in a case of primary cerebral non- Hodgkin's lymphoma. Clin Neurol Neurosurg 1989; 91: 247- 50. 11. Eby NL, Grufferman S, Flannelly CM, et al. Increasing incidence of primary brain lymphoma in the US. Cancer 1988; 62: 2461- 5. / Neiiro- Ophtlmlmol, Vol. 16, No. 3, 1996 |