| OCR Text |
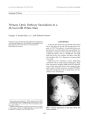
Show Journal of Neuro- Ophthalmology 16( 3): 191- 195, 1996. © 1996 Lippincott- Raven Publishers, Philadelphia Case Report Ocular Motor Consequences of Damage to the Abducens Nucleus Area in Humans Rene M. Miiri, M. D., Jean Francois Chermann, M. D., Laurent Cohen, M. D., Sophie Rivaud, Ph. D., and Charles Pierrot- Deseilligny, M. D. A patient with a complete unilateral conjugate gaze paralysis caused by a small lesion affecting the region of the right abducens nucleus, documented by magnetic resonance imaging, is reported. Eye movements were quantitatively evaluated using electro- oculography. A gaze- evoked nystagmus to the contralateral side and impairment of smooth pursuit and vestibular ocular reflex in the contralateral hemifield of movements were found. The differential diagnosis of conjugate gaze paralysis and the additional ocular motor abnormalities are interpreted in light of clinical and experimental findings. Key Words: Abducens nucleus- Humans- Eye movements- Gaze paralysis- Nystagmus. Manuscript received January 6, 1995; accepted June 30, 1995. From the Service de Neurologie ( J. F. C., L. C., C. P.- D.) and INSERM 289 ( R. M. M., S. R., C. P.- D.), Hopital de la Salpetriere, Paris, France. Address correspondence and reprint requests to Pr. Ch. Pierrot- Deseilligny, Clinique Paul Castaigne, Hopital de la Salpetriere, 47, Boulevard de l'Hopital, 75651 Paris, Cedex 13, France. The pontine tegmentum contains crucial structures for horizontal eye movements. The abducens nucleus forms the final common pathway for all horizontal conjugate eye movements. It receives multiple projections from the premotor structures involved in horizontal eye movement control, such as the paramedian pontine reticular formation ( PPRF), the cerebellum, the vestibular nuclei, and the nucleus prepositus hypoglossi ( for review, see 1). The abducens nucleus contains two populations of neurons: the motoneurons, which innervate the ipsilateral lateral rectus muscle, and the inter-nuclear neurons, which cross the midline and connect, via the medial longitudinal fasciculus ( MLF), with the contralateral subnucleus of the medial rectus muscle in the oculomotor nucleus. Acquired lesions limited to the abducens nucleus region in humans are uncommon ( 2- 6), and most of our knowledge about the role of the abducens nucleus in ocular motor control comes from primate electrophysiological and anatomical studies. The quantitative results presented in this report, which concerns a patient with a small lesion affecting the abducens nucleus region, enhance our knowledge of the clinical syndrome in humans corresponding to such damage. CASE REPORT A 49- year- old man with no previous notable medical history complained of intermittent horizontal diplopia. On clinical examination, 10 days after the onset of symptoms, the patient showed a right peripheral facial paresis and a slight right-ward gait deviation with eyes closed. A complete rightward gaze paralysis existed: The eyes could 191 192 R. M. MURI ET AL. not cross the midline with saccades, smooth pursuit, or vestibular- induced eye movements. On clinical examination, no exotropia or esotropia was found and a marked horizontal nystagmus was present when the patient looked leftward. Vertical eye movements and convergence were clinically normal. Magnetic resonance imaging ( MRI) showed, on T2- weighted images, a few small hyperintense signals in the periventricular areas and the corpus callosum. In the brainstem, there was only one hyperintense signal measuring about 10 mm and located in the right paramedian pontine tegmentum ( Fig. 1A). Intravenous Gadolinium administration effected an enhancement of this lesion. The cerebellum was normal. The white cell count of cerebrospinal fluid was 31/ mm3, with 94% lymphocytes. The protein level was slightly elevated ( 0.46 g/ L) with positive oligo-clonal bands. There was no risk factor for cerebrovascular disease, and extensive blood analysis to screen for systemic inflammatory or rheumatolog-ical diseases revealed normal values. Results of Doppler sonography of the cranial vessels were also normal. The presumed diagnosis was multiple sclerosis, and steroid therapy was administered. All clinical signs disappeared over the following 2 weeks. Control MRI 2 months after the episode showed unchanged hyperintense signals suprat-entorially, whereas the hyperintense signal was no longer detectable in the brainstem. Right Eye .. a^ wiwi*, h « Y^ mwYY" j ^/^.^ v^^^'^^ yY'^ jy^^ Y^^'^ ( TV'^^ irf 35 ( leg 400 dcg/ s Left Eye M L . Position M^ wr*. iWwvw^ fyY'Wf * ^ Velocity FIG. 1. Patient's lesion and recordings. A: T2- weighted cranial magnetic resonance imaging scan showing an isolated hyperintense signal in the right dorsal pontine tegmentum ( arrow). B: Recordings of both eyes showing the gaze- evoked nystagmus on the left side while the eye attempted to hold a 35- degree eccentricity, with an exponentially declining slow- velocity component. Note also the existence of some rightward saccades ( arrows). M, midline; L, left. Stimulus / Neuw- Ophtlmlmol, Vol. 16, No. 3, 1996 OCULAR CONSEQUENCES OF ABDUCENS NUCLEUS LESION 193 Eye- movement Recordings Horizontal eye movements were recorded 12 days after the onset of symptoms, separately for each eye, using direct current electro- oculography. Electrodes ( Ag- AgCl) were placed at the outer and inner canthi. The system had a bandwidth of 0 to 100 Hz. The patient was seated in a darkened room; his head was restrained. Stimulation was induced using a ramp of horizontal red- light-emitting diodes. Amplitude and peak velocity of saccades ( with target eccentricity of 13 degrees), the gain of sinusoidal smooth pursuit ( frequency = 0.125 Hz, peak velocity = 15 degrees), the gain of optokinetic nystagmus ( OKN) ( stimulation of 60 degrees of the visual field, using black and white stripes, with a 20 degrees/ s constant velocity), and the gain of the vestibulo- ocular reflex ( VOR) ( stimulated sinusoidally in the dark, with a frequency of 0.31 Hz, and a peak velocity of 58 degrees/ s) were quantitatively analyzed. Results of 10 consecutive eye movements were averaged and compared with those of 13 normal control subjects ( mean age, 49 years; SD = 13), using the normal range ( mean ± 2 SD). Symmetry between the eyes was studied using Student's t test. No conjugate lateral eye movements across the midline toward the right side were observed. Convergence, however, was preserved. A gaze- evoked nystagmus was found on the left side, including an exponentially declining slow- velocity component ( Fig. IB). Its amplitude increased with eccentricity. This nystagmus was clearly visible from an eccentricity of 10 degrees to the left. Table 1 shows the quantitative analysis of eye movements in the left hemifield. Visually guided saccades in the centrifugal direction ( i. e., from the midline to the left side) showed normal velocity in both eyes, although with significant asymmetry ( p < 0.001) of amplitude, with hypometria in the right eye. Velocity of the right eye was normal compared with the velocity of 11- degree saccades of normals ( mean, 165 ± 36 degrees/ s). Centripetal saccades, from the left back to the midline, were slowed ( normal mean velocity for 7- degree saccades: 142 ± 21 degrees/ s) and hypometric. The smooth- pursuit gain ( peak eye velocity over peak target velocity) was reduced for both eyes in the centrifugal direction ( left eye, 0.66 ± 0.20; right eye, 0.82 ± 0.20), whereas the gain in the centripetal direction was normal ( left eye, 0.99 ± 0.15; right eye, 0.98 ± 0.16). The OKN gain was reduced in the centrifugal direction ( left eye, 0.44 ± 0.10; right eye, 0.38 ± 0.06) but slightly increased in the centripetal direction ( left eye, 09 ± 0.28; right eye, 0.9 ± 0.29). The VOR gain was reduced in both directions and for both eyes ( for centrifugal direction: left eye, 0.46 ± 0.08; right eye, 0.41 ± 0.07; for centripetal direction: left eye, 0.33 ± 0.11; right eye, 0.23 ± 0.11) furthermore, with significant asymmetry of the gain in the centripetal direction, which was more decreased in the right eye ( p < 0.02). DISCUSSION A complete unilateral conjugate gaze paralysis associated with a peripheral facial paresis, as in our patient, suggests a lesion affecting the ipsilat-eral abducens nucleus and the immediately adjacent facial nerve fibers ( 5,6). This localization was confirmed by MRI. Relatively small lesions affecting this area are rare, and reported causes have included infarction, tumor, histiocytosis X, inflammation, Wernicke- Korsakoff syndrome, and trauma ( 2- 4, 7- 10). In our patient, the presumed cause was multiple sclerosis. The absence of all horizontal eye movements ( including smooth pursuit and VOR) from the midline to the right side implies that the abducens nucleus was damaged, as this nucleus is the final common pathway for such movements. A lesion TABLE 1. Eye movements in the left hemifield Saccades Amplitude ( deg) Peak velocity ( deg/ s) Smooth pursuit ( Gain) OKN ( Gain) VOR ( Gain) Left eye 14 284 0.66b 0.44" 0.46b Cen1 : rifugal movements3 Right eye 11b 192 0.84b 0.38b 0.41b Controls ( Mean ± SD) 13 ± 0.5 202 ± 46 1.02 ± 0.06 0.67 ± 0.09 0.81 ± 0.12 Left eye 7b 86" 0.99 0.9" 0.33" Cer itripetal movements" Right eye 7b 86b 0.98 0.9 0.23" Controls ( Mean ± SD) 13 ± 0.5 171 ± 40 1.04 ± 0.07 0.74 ± 0.10 0.85 ± 0.12 OKN, optokinetic nystagmus; VOR, vestibulo- ocular reflex. a Centrifugal means movements from the midline to the left side, whereas centripetal means eye movements from the left to the midline. b Outside the normal limits ( mean of controls ± 2 SD). / Neum- OphtlMlmol, Vol. 36, No. 3, 1996 194 R. M. MURIET AL. affecting the caudal PPRF, which is the immediate premotor structure for horizontal saccades, would have preserved ipsilateral smooth pursuit and VOR. Furthermore, such a lesion would have resulted in an absence of all ipsilateral saccades, including those in the contralateral hemifield. In our patient, centripetal rightward saccades in the left hemifield still existed. Such saccades are explained by the excitatory activity of the right PPRF on the right inhibitory burst neurons, which inhibit the left abducens nucleus ( 11- 14). Velocity and amplitude of these centripetal saccades were symmetrically decreased, probably because only such phasic inhibition of the antagonist muscle motoneurons ( without any activity of the agonist muscles) persisted for these movements. Therefore, the ocular motor syndrome of our patient resulted from an abducens nucleus lesion and was not due to combined PPRF damage. In lesions affecting the abducens nucleus or the PPRF, the adjacent MLF is also frequently damaged, resulting in a " one- and- a- half" syndrome ( 15,16), i. e., a combination of gaze paralysis and internuclear ophthalmoplegia on the same side. Although there was a discrete hypometria of adduction saccades in the right eye, saccade velocity was normal, which is a strong argument against an additional internuclear ophthalmoplegia due to a damage of the right MLF. Furthermore, such damage should also have an asymmetrical influence on the gain of smooth pursuit, which was not the case in our patient. Another marked eye movement abnormality was the nystagmus observed in leftward gaze, with an approximately exponential declining slow phase ( Fig. IB). Such a nystagmus induced by an eccentric eye position, known as gaze- evoked nystagmus, suggests the existence of a gaze- holding deficit ( 5). Gaze- evoked nystagmus can be caused by sedatives, antiepileptic drugs, or alcohol ( 6). Lesions affecting the flocculonodular lobe also result in gaze- evoked nystagmus ( 17). Neither condition was present in our patient. Three other causes, either singly isolated or in association, could explain the gaze- holding deficit in this patient. The nucleus prepositus hypoglossi ( NPH), which is located close to the abducens nucleus, or the fibers reciprocally connecting these two nuclei, could have been damaged by the lesion. The NPH is thought to be an important part of the neural integrator for lateral eye movements ( 18,19). Because a unilateral lesion affecting the NPH is known to cause a bilateral gaze- holding deficit in animals ( 18,20), such a lesion could have contributed here to the leftward gaze- holding deficit. Another explanation could be that the connections with the medial vestibular nucleus ( MVN), which also forms a part of the neural integrator ( 18), were damaged in our patient. These connections with the abducens nuclei are ipsilateral for the inhibitory fibers and contralateral for the excitatory fibers ( 21), the latter passing close to and through the ipsilateral abducens nucleus before crossing the midline ( 22). In our patient, the decrease in the gain of the leftward VOR supports the hypothesis of damage to the excitatory vestibular fibers and, therefore, a possible contribution of this mechanism to the leftward gaze- holding deficit. Furthermore, the cell groups of the MLF and paramedian tracts, receiving an afferent tract from the abducens nucleus and projecting bilaterally to the flocculus and mid-vermis, could also play a role in gaze- holding ( 23,24). Because these cells are located partly in the rostral part of the abducens nucleus, they were probably damaged in our patient, and this could also have contributed to the gaze- holding deficit. It should be noted that these different disturbances could result from damage either to the abducens nucleus itself or to immediately adjacent structures and that a similar gaze- evoked nystagmus has been reported in a patient with a single small lesion, affecting the region of this nucleus ( 4). Therefore, such a gaze- evoked nystagmus might be considered to belong to the clinical abducens nucleus syndrome. The decreased gain of contralateral ( leftward) smooth pursuit and OKN could also be explained by damage to the structures involved in gaze- holding control ( for review, see 5). This finding confirms and amplifies the results of the previously reported patient with a similar lesion of the abducens nucleus area, in whom analogous contralateral smooth pursuit abnormalities were observed using qualitative analysis of eye movements ( 4). It should be noted that, for centripetal ( right-ward) movements, the VOR was impaired, but smooth pursuit and OKN were preserved. This seems contradictory, as smooth pursuit, OKN, and the VOR are supposed to be mediated by the same pathways between the vestibular and the abducens nuclei. In fact, such a dissociation could be explained by a difference in stimulation velocities used here for pursuit movements and the VOR. For relatively low velocities, as those used for pursuit movements, a simple disfacilitation of the antagonist muscles could be sufficient to result in a normal gain of centripetal eye movements. For much higher velocities, such as those used for the VOR, an excitation of the agonist muscles ( lacking | Naim- Ophtlmlmol, Vol. 16, No. 3, 1996 OCULAR CONSEQUENCES OF ABDUCENS NUCLEUS LESION 195 here because of the abducens nucleus damage) would be required, besides the decrease in activity in the antagonist muscles, to ensure a normal gain of centripetal movements. Therefore, the absence of activity in the agonist muscle would result in a decrease in the gain of centripetal slow eye movements for high- stimulation velocities ( i. e., for the VOR), without significant effect for low- stimulation velocities ( i. e., for pursuit movements). Thus, it may be concluded that the clinical abducens nucleus syndrome consists of ( a) paralysis of all ipsilateral eye movements and peripheral facial paresis; ( b) a gaze- evoked nystagmus associated with smooth- pursuit and VOR disorders in the contralateral hemifield, as these abnormalities may be explained by damage either to the nucleus itself or to immediately adjacent tracts. Acknowledgment: R. M. Miiri received financial support from the Swiss National Research Foundation. REFERENCES 1. Evinger C. Extraocular motor nuclei: location, morphology and afferents. In: Biittner- Ennevcr JA, ed. Neuroanatomy of the oculomotor system. Reviews of oculomotor research, vol 2. Amsterdam: Elsevier, 1988: 81- 118. 2. Bennett AH, Savill T. A case of permanent conjugate deviation of the eyes and head, the result of a lesion limited to the sixth nucleus; with remarks on associated lateral movements of the eyeballs, and rotation of the head and neck. Brain 1889; 12: 102- 16. 3. Meienberg O, Biittner- Ennever JA, Kraus- Ruppert R. Unilateral paralysis of conjugate gaze due to lesion of the abducens nucleus. Clinico- pathological case report. Neuro-ophthalmology 1981; 2: 47- 52. 4. Pierrot- Deseilligny C, Goasguen J. Isolated abducens nucleus damage due to histiocytosis X. Electro- oculographic analysis and physiological deductions. Brain 1984; 107: 1019- 32. 5. Leigh RJ, Zee DS. The neurology of eye movements, 2nd ed. Philadelphia: FA Davis, 1991.'' 6. Miller NR. Walsh and Hoyt's clinical neuro- ophthalmology, 4th ed. vol. 2, Baltimore: Williams and Wilkins, 1985. 7. Minor RH, Kearns TP, Millikan CH, Siekert RG, Sayre GP. Ocular manifestation of occlusive disease of the vertebral-basilar arterial system. Arch Ophthalmol 1959; 62: 112- 24. 8. Derby BM, Guiang RL. Spectrum of symptomatic brainstem metastasis. / Neurol Neurosurg Psychiatr 1975; 38: 888- 95. 9. Abad VC, Wolintz A. Bilateral horizontal gaze palsy. Ann Ophthalmol 1982; 14: 1046- 8. 10. Cogan DG, Victor M. Ocular signs of Wenicke's disease. Arch Ophthalmol 1963; 70: 757- 71. 11. Biittner- Ennever JA, Henn V. An autoradiographic study of the pathways from the pontine reticular formation involved in horizontal eye movements. Brain Res 1976; 108: 155- 64. 12. Kaneko CRS, Fuchs AF. Inhibitory burst neurons in alert trained cats: comparison with excitatory burst neurons and functional implication. In: Fuchs AF, Becker W, eds. Progress in oculomotor research. New York: Elsevier, 1981; 63- 70. 13. Strassman A, Highstein SM, McCrea RA. Anatomy and physiology of saccadic burst neurons in the alert squirrel monkey. 1. Excitatory burst neurons. / Comp Neurol 1986; 249: 337- 57. 14. Strassman A, Highstein SM, McCrea RA. Anatomy and physiology of saccadic burst neurons in the alert squirrel monkey. II. Inhibitory burst neurons. / Comp Neurol 1986; 249: 358- 80. 15. Wall M, Wray SH. The one- and- a- half syndrome. A unilateral disorder of the pontine tegmentum: a study of 20 cases and review of the literature. Neurology 1983; 33: 971- 80. 16. Sharpe JA, Rosenberg MA, Hoyt WF, Daroff RB. Paralytic pontine exotropia: a sign of acute unilateral pontine gaze palsy and internuclear ophthalmoplegia. Neurology 1974; 24: 1076- 81. 17. Zee DS, Yamazaki A, Butler PH, Gucer G. Effects of ablation of flocculus and paraflocculus on eye movements in primate. / Neurophysiol 1981; 46: 878- 99. 18. Cannon SC, Robinson DA. Loss of neural integrator of the oculomotor system from brainstem lesions in monkey. / Neurophysiol 1987; 57: 1383^ 109. 19. Lopez- Barneo J, Darlot C, Berthoz A, Baker R. Neuronal activity in prepositus nucleus correlated with eye movement in the alert cat. / Neurophysiol 1982; 47: 329- 52. 20. Cheron G, Mettens P, Godaux E. Gaze holding defect induced by injections of ketamine in the cat brainstem. Neu-roreport 1992; 3: 97- 100. 21. Belknap DB, McCrea RA. Anatomical connections of the prepositus and abducens nuclei in the squirrel monkey. / Comp Neurol 1988; 268: 13- 28. 22. McCrea RA, Yoshida K, Evinger C, Berthoz A. The location, axonal arborization, and termination sites of eye-movement- related secondary vestibular neurons demonstrated by intra- axonal HRP injection in the alert cat. In: Fuchs AF, Becker W, eds. Progress in oculomotor research. New York: Elsevier, 1981; 379- 86. 23. Biittner- Ennever JA, Horn AKE, Schmidtke K. Cell groups of the medial longitudinal fasciculus and paramedian tracts. Rev Neurol 1989; 145: 533- 9. 24. Langer T, Kaneko CRS, Scudder CA, Fuchs AF. Afferents to the abducens nucleus in the monkey and cat. / Comp Neurol 1986; 245: 379^ 100. | Nctiw- Ophtlmlmol, Vol. 16, No. 3, 1996 |