| OCR Text |
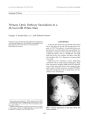
Show journal of Neuw- Ophthalmologij 16( 3): 188- 190, 1996. © 1996 Lippincott- Raven Publishers, Philadelphia Feature Photo Primary Optic Pathway Sarcoidosis in a 38- Year- Old White Man Gregory S. Kosmorsky, D. O., and Richard Pray son We report a case of primary optic pathway sarcoidosis in a 38- year- old white man. The disorder was limited to the optic nerves and was resistant to corticosteroids. Key Word: Sarcoidosis. Manuscript received March 21, 1995; accepted June 30, 1995. From the Division of Ophthalmology ( G. S. K.) and the Division of Pathology ( R. P.), Cleveland Clinic Foundation, Cleveland, Ohio, U. S. A. Address correspondence and reprint requests to Dr. Gregory S. Kosmorsky, Division of Ophthalmology, Cleveland Clinic Foundation, Cleveland, OH 44195- 5024, U. S. A. CASE REPORT A 38- year- old white man presented with visual loss in his right eye that he first recognized in August of 1993. The patient's visual loss slowly progressed over several months and was painless. Examination revealed a best- corrected visual acuity of 20/ 60 and 20/ 15, with 2+ RAPD OD. The right optic disc nerve was swollen, and there were retinal exudates ( Fig. 1); a diagnosis of neuroretinitis was made. Ultrasound was reported to show thickening consistent with an optic nerve meningioma. Magnetic resonance imaging ( MRI) showed enhancement of the right optic nerve that extended to the optic chiasm. Lumbar puncture revealed 15 WBCs. Alternative diagnoses such as lymphoma and sarcoidosis were entertained. FIG. 1. Swollen appearance of the optic nerve with retinal exudates. 188 PRIMARY OPTIC PATHWAY SARCOIDOSIS 189 Systemic workup failed to reveal any evidence of sarcoidosis; chest x- ray film, angidensin- con-verting enzymes, lysozymes, and anergy response were all normal. The patient was treated with high doses of oral prednisone yet continued to lose vision to " hand motions." A lateral orbitotomy was performed in January and the meninges were biopsied, revealing only normal tissue. Despite maintenance prednisone at 20 mg/ day, the patient began to experience transient episodes of visual blurring in the nasal field of the left eye. He described this blurring as a light-colored " mesh" that got progressively worse and that also seemed to be worse under darkened conditions. FIG. 2. A- D Coronal and axial contrast- enhanced MRI Repeat MRI revealed no change in the enhancement of the right optic nerve but the chiasm was felt to be thickened ( Fig. 2). Prednisone was increased to 20 mg b. i. d. In July the patient became aware of " zigzags" centrally and reported that he could see his pulse through his left eye. His vision also dimmed, and he had photopsias with postural change and extremes of gaze. The patient took 500 mg of Solu- Medrol q. i. d. for 3 days i. v. followed by 100 mg/ day of prednisone. Despite this therapy the vision in his left eye did not improve and his right eye was now NLP. Repeat MRI revealed intense enhancement of the right optic nerve and less enhancement of the left optic nerve in a perineural pattern. The scans demonstrate perineural enhancement ( arrows). / Neuro- Ophthalmot, Vol. 16, No. 3, ( 996 190 G. S. KOSMORSKY AND R. PRAYSON FIG. 3. Optic nerve shows two necrotizing granulomas and an associated chronic inflammatory infiltrate consisting primarily of lymphocytes ( hematoxylin- eosin, X400). 4V chiasm was thickened, with a perineural pattern of enhancement ( Fig. 2). It was decided to biopsy the optic nerve of the blind eye via a frontal craniotomy approach. The biopsy revealed noncaseating granulomas consistent with sarcoidosis ( Fig. 3). Pathologic analysis failed to reveal other causes for the granulomas ( e. g., tuberculosis or fungi). Subsequent treatment with Decadron, 1 mg q. i. d., caused a normalization of his visual fields, and acuity to return to the 20/ 15 level in the left eye; the disc edema was also resolved. ; Neum- Ophllhilmol, Vol. 16, No. 3, 1996 |