| OCR Text |
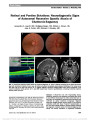
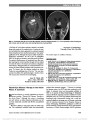
Show Diagnostic Features of Retinal Nerve Fiber Layer Rotation in Skew Deviation Using Optical Coherence Tomography John J. Chen, MD, PhD, Randy H. Kardon, MD, PhD, Reid A. Longmuir, MD Abstract: A 41-year-old woman with skew deviation had cyclotorsion of both eyes. This resulted in a falsely low probability plot of retinal nerve fiber layer thickness in adjacent clock hours on optical coherence tomography (OCT) due to displacement of the retinal nerve fiber layer peaks. Ocular cyclotorsion may cause misinterpretation of OCT probability plots. OCT retinal nerve fiber layer plots also may be used to objectively quantify the degree of ocular cyclotorsion. Journal of Neuro-Ophthalmology 2014;34:389-392 doi: 10.1097/WNO.0000000000000152 © 2014 by North American Neuro-Ophthalmology Society Optical coherence tomography (OCT) measurements of the retinal nerve fiber layer (RNFL) has become an essential tool in diagnosing and monitoring patients with glaucoma and other optic neuropathies. With the advent of spectral domain OCT, the resolution has mark-edly improved providing more accurate and faster measure-ments of the RNFL (1). Despite advances in OCT technology, a variety of factors can introduce variability in RNFL thickness, including age, poor signal strength, optic disc size, refractive error, and tilted optic disc syn-drome (2,3). We report a patient with skew deviation that led to a falsely low probability plot of the RNFL thickness in adjacent clock hours in both eyes. This can cause misdiagnosis of pathologic thinning of the RNFL. Our case also dem-onstrates that OCT may provide an objective measurement of ocular cyclotorsion in skew deviation and other disorders causing ocular cyclotorsion. CASE REPORT A 41-year-old woman with a history of multiple sclerosis complained of decreased vision and imbalance for 1 month. She had stopped interferon b-1a over the past 8 months in hopes of becoming pregnant. On examination, visual acuity was 20/25 in each eye. Although extraocular movements were full, she demonstrated impaired smooth pursuit, sac-cadic dysmetria, and subtle gaze-evoked jerk nystagmus. She had a 3-prism diopter left hyperdeviation that increased to 4-prism diopters on left gaze, but was otherwise comitant. Fundus examination was normal but revealed exclyclotor-sion of the right eye and incyclotorsion of the left (Fig. 1). Double Maddox rod testing revealed 5° of inclyclotorsion. Automated perimetry (Humphrey 24-2) showed normal thresholds bilaterally, but the physiological blind spot loca-tion was vertically displaced in opposite directions in each eye (Fig. 2). Magnetic resonance imaging demonstrated several enhancing white matter lesions in the cerebellum and cerebral cortex and one involving the right side of the pons (Fig. 3). Cirrus OCT (Carl Zeiss Meditec) showed a normal average RNFL thickness, but the spatial distribution of the arcuate bundles on the thickness plot seemed to be abnormal resulting in inferotemporal thinning, right eye and superotemporal thinning, left eye (Fig. 4). On careful examination of the RNFL profile, it became apparent that there was nasal displacement of the inferotemporal peak of RNFL thickness in the right eye and the superotemporal peak in the left eye. We determined that the ocular cyclo-torsion was responsible for the apparent focal thinning of the RNFL when compared with the normative database, and that the shift of the RNFL peaks compared with the normative database could be used to quantify the amount of cyclotorsion. Quantifying the shift of the peaks on the Department of Ophthalmology and Visual Sciences (JJC, RHK, RAL), University of Iowa, Iowa City, Iowa; and Department of Veterans Affairs (RHK), Veteran's Affairs Medical Center, Iowa City, Iowa. The authors report no conflicts of interest. Address correspondence to Reid A. Longmuir, MD, Department of Ophthalmology and Visual Sciences, University of Iowa Hospitals and Clinics, 200 Hawkins Drive PFP, Iowa City, IA 52242; E-mail: reid-longmuir@uiowa.edu Chen et al: J Neuro-Ophthalmol 2014; 34: 389-392 389 Clinical Observation Copyright © North American Neuro-Ophthalmology Society. Unauthorized reproduction of this article is prohibited. RNFL TSNIT (temporal-superior-nasal-inferior-temporal) plot demonstrated that the inferotemporal peak of the right eye was shifted 13° nasally, and the superotemporal peak of the left eye was shifted 20° nasally (Fig. 4). This was com-parable with the amount of cyclotorsion measured on fun-dus photography, which was 15° of excyclotorsion, right eye and 18.5° of incyclotorsion, left eye, relative to a normal inferior displaced fovea of 7.25° (Fig. 1). In addition, the larger degrees of incyclotorsion, right eye compared with the excyclotorsion, left eye, agreed with the clinically measured incyclotorsion of 5° between the eyes detected on double Maddox rod testing. DISCUSSION Our case demonstrates a rotational displacement of the RNFL profile due to skew deviation. The demyelinating lesion at the pontomedullary junction caused a right (ipsiversive) hypotropia with ocular torsion towards the lower eye (right exclyclotorsion and left incyclotorsion) (4). The inferotemporal RNFL bundle of the right eye and the superotemporal RNFL bundle of the left eye were both displaced nasally on the RNFL profile when compared with the normative database. This caused the analysis to display those areas within the ,1% level compared with the general population. There was no anatomic defect of the optic nerve or visual field defect corresponding to these areas of re-ported thinning, and the average RNFL thickness was normal. Our patient had potential reasons for a thin RNFL, including her history of multiple sclerosis and family history of glaucoma. Recognition of this artifact was important to avoid an incorrect diagnosis. Similar artifacts in RNFL analysis are seen in highly myopic and hyperopic eyes where the orientation of the superotemporal and inferotemporal RNFL bundles seem displaced in association with abnor-mally long or short axial lengths, resulting in an abnormal probability plot of the regional analysis of the RNFL when compared with the normative database (5-7). In our patient, it seems that the superior and inferior arcuate RNFL bundles of each eye have a more vertical angle of entrance about the optic nerve, without the torsion, typical FIG. 1. The fundi show 15° of excyclotorsion, right eye and 18.5° of incyclotorsion, left eye, relative to the normal inferiorly positioned fovea of 7.25° (blue triangle indicates the angle between the disc and fovea). FIG. 2. Automated visual fields are full but demonstrate inferior displacement of the right physiologic blind spot and superior displacement of the left blind spot. FIG. 3. Postcontrast T1 axial magnetic resonance imaging reveals an enhancing lesion (arrow) involving the right pons and middle cerebellar peduncle. 390 Chen et al: J Neuro-Ophthalmol 2014; 34: 389-392 Clinical Observation Copyright © North American Neuro-Ophthalmology Society. Unauthorized reproduction of this article is prohibited. of shorter, hyperopic eyes. Because of this, the superior arcuate bundle of the right eye was rotated into a more normal entrance angle, and the inferior arcuate bundle was shifted further away from the normal angle, causing the probability plot to be abnormal inferiorly but not supe-riorly. A similar effect was seen for the left eye, but in the opposite direction. Interestingly, the magnitude of the peak shifts from the normative data average peak locations on the RNFL TSNIT OCT profile from the skew-induced cyclotorsion provided very similar cyclotorsion measurements to those obtained from fundus photography. It is important to note that the artifact and rotational shift of RNFL peaks from cyclotorsion will not be seen on Spectralis OCT (Heidelberg, Germany) because of fovea-to-disc alignment software that uses foveal fixation and its intersection with the papillomacular bundle to correct for rotation of the eye. However, a recent study demonstrated that manually displacing the fovea location on Spectralis OCT, thereby mimicking inaccurate foveal fixation during image acquisition, can introduce torsional artifacts (8). In summary, the observation of a skew deviation causing a "skewed" artifact in the RNFL thickness is important when interpreting the RNFL of patients with clinically sig-nificant cyclotorsion. In addition, the amount of displace-ment in the superotemporal and inferotemporal RNFL bundles on OCT could theoretically be used to measure the degree of ocular cyclotorsion. FIG. 4. Optical coherence tomography of the retinal nerve fiber layer (RNFL). The average RNFL thickness is normal bilat-erally. There is an artifactual thinning of 2 adjacent clock hours inferotemporally in the right eye and superotemporally in the left eye compared with the normative database and corresponding thickening in the adjacent clock hour segment (white on the clock hour probability plot). On the RNFL profile, the inferotemporal RNFL peak in the right eye (orange arrow) and the superotemporal RNFL peak in the left eye (red arrow) are both displaced nasally compared with the normal inferotemporal RNFL peak (purple arrow) and superotemporal RNFL peak (blue arrow), respectively. Quantifying the shift of the peaks on the RNFL TSNIT (temporal-superior-nasal-inferior-temporal) plot demonstrates that the inferotemporal peak of the right eye was shifted 13° nasally and the superotemporal peak of the left eye was shifted 20° nasally. Chen et al: J Neuro-Ophthalmol 2014; 34: 389-392 391 Clinical Observation Copyright © North American Neuro-Ophthalmology Society. Unauthorized reproduction of this article is prohibited. ACKNOWLEDGMENTS The authors had full access to all the data in the study and take responsibility for the integrity of the data and the accuracy of the data analysis. REFERENCES 1. Leung CK, Cheung CY, Weinreb RN, Qiu Q, Liu S, Li H, Xu G, Fan N, Huang L, Pang CP, Lam DS. Retinal nerve fiber layer imaging with spectral-domain optical coherence tomography: a variability and diagnostic performance study. Ophthalmology. 2009;116:1257-1263. 2. Kim NR, Lim H, Kim JH, Rho SS, Seong GJ, Kim CY. Factors associated with false positives in retinal nerve fiber layer color codes from spectral-domain optical coherence tomography. Ophthalmology. 2011;118:1774-1781. 3. Ghadiali Q, Hood DC, Lee C, Manns J, Llinas A, Grover LK, Greenstein VC, Liebmann JM, Odel JG, Ritch R. An analysis of normal variations in retinal nerve fiber layer thickness profiles measured with optical coherence tomography. J Glaucoma. 2008;17:333-340. 4. Brandt T, Dieterich M. Skew deviation with ocular torsion: a vestibular brainstem sign of topographic diagnostic value. Ann Neurol. 1993;33:528-534. 5. Yamashita T, Asaoka R, Tanaka M, Kii Y, Yamashita T, Nakao K, Sakamoto T. Relationship between position of peak retinal nerve fiber layer thickness and retinal arteries on sectoral retinal nerve fiber layer thickness. Invest Ophthalmol Vis Sci. 2013;54:5481-5488. 6. Yoo YC, Lee CM, Park JH. Changes in peripapillary retinal nerve fiber layer distribution by axial length. Optom Vis Sci. 2012;89:4-11. 7. Hong SW, Ahn MD, Kang SH, Im SK. Analysis of peripapillary retinal nerve fiber distribution in normal young adults. Invest Ophthalmol Vis Sci. 2010;51:3515-3523. 8. Valverde-Megias A, Martinez-de-la-Casa JM, Serrador- Garcia M, Larrosa JM, Garcia-Feijoo J. Clinical relevance of foveal location on retinal nerve fiber layer thickness using the new FoDi software in spectralis optical coherence tomography. Invest Ophthalmol Vis Sci. 2013;54: 5771-5776. STATEMENT OF AUTHORSHIP All authors contributed for conception and design, acquisition of data, analysis and interpretation of data, drafting of the manuscript, revision of the manuscript for intellectual content, and final approval of the completed manuscript. 392 Chen et al: J Neuro-Ophthalmol 2014; 34: 389-392 Clinical Observation Copyright © North American Neuro-Ophthalmology Society. Unauthorized reproduction of this article is prohibited. |