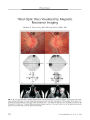
| Title |
The Ratio of Square Wave Jerk Rates to Blink Rates Distinguishes Progressive Supranuclear Palsy from Parkinson Disease |
| Creator |
Altiparmak, UE; Eggenberger, E; Coleman, A; Condon, K |
| Affiliation |
Department of Neurology, Michigan State University, East Lansing, Michigan 48824-1313, USA. |
| Abstract |
BACKGROUND: Distinguishing progressive supranuclear palsy (PSP) from Parkinson disease (PD) may be difficult, particularly in the early stages, because the characteristic vertical supranuclear eye movement abnormalities of PSP may be absent or delayed until late in the course of the disease. In this study we investigated the usefulness of comparing the square wave jerk rate (SWJR) and blink rate (BR) in the differentiation of these two disorders. METHODS: We studied 10 patients with PD (PD group) and 5 patients with PSP (PSP group) who met published diagnostic criteria. The SWJR and BR were measured from video recordings and were used to calculate a ratio (SWJR:BR). RESULTS: The PSP group exhibited a significantly higher SWJR, higher SWJR:BR, and lower BR than did the PD group. No patient with PSP exhibited a SWJR:BR of < 3; however, one patient with PD had a SWJR:BR of 5.3, creating overlap between the two groups. CONCLUSIONS: The SWJR:BR is a simple and reasonably useful clinical measure to distinguish established PSP from PD. Determining the value of this measure in differentiating early PSP from PD requires a prospective study. |
| Subject |
Older people; Blinking; Diagnosis, Differential; Electrodiagnosis, methods; Eye Movements; Female; Humans; Male; Muscle Contraction; Ocular Motility Disorders, diagnosis; Ocular Motility Disorders, physiopathology; Oculomotor Muscles, innervation; Oculomotor Muscles, physiopathology; Parkinson Disease, diagnosis; Parkinson Disease, physiopathology; Predictive Value of Tests; Supranuclear Palsy, Progressive, diagnosis; Supranuclear Palsy, Progressive, physiopathology |
| Format |
application/pdf |
| Publication Type |
Journal Article |
| Collection |
Neuro-Ophthalmology Virtual Education Library: Journal of Neuro-Ophthalmology Archives: https://novel.utah.edu/jno/ |
| Publisher |
Lippincott, Williams & Wilkins |
| Holding Institution |
Spencer S. Eccles Health Sciences Library, University of Utah |
| Rights Management |
© North American Neuro-Ophthalmology Society |
| Setname |
ehsl_novel_jno |
| ID |
225505 |
| Reference URL |
https://collections.lib.utah.edu/ark:/87278/s6wt209n/225505 |