| Title |
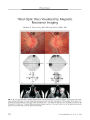
Pontine Tuberculoma Presenting With Horizontal Gaze Palsy |
| Creator |
Saxena, R; Menon, V; Sinha, A; Sharma, P; Kumar, DA; Sethi, H |
| Affiliation |
Dr. Rajendra Prasad Centre for Ophthalmic Sciences, All India Institute of Medical Sciences, New Delhi, India. rohitsaxena80@yahoo.com |
| Abstract |
A 38-year-old immunocompetent man presented with a horizontal supranuclear gaze palsy as the only neurologic manifestation of a pontine tuberculoma. Although a biopsy of the brain lesion was not performed, it was attributed to tuberculosis because of chest x-ray evidence. The patient was given empirical anti-tuberculous therapy. After one month, the gaze palsy had fully recovered and repeat MRI showed a decrease in the size of the lesion. This is the first reported case of supranuclear gaze palsy without diplopia as a manifestation of a tuberculous brain stem lesion. |
| Subject |
Abducens Nerve, pathology; Abducens Nerve, physiopathology; Abducens Nerve Diseases, microbiology; Abducens Nerve Diseases, pathology; Abducens Nerve Diseases, physiopathology; Adult; Humans; Magnetic Resonance Imaging; Male; Neural Pathways, pathology; Neural Pathways, physiopathology; Ocular Motility Disorders, microbiology; Ocular Motility Disorders, pathology; Ocular Motility Disorders, physiopathology; Oculomotor Muscles, innervation; Oculomotor Muscles, physiopathology; Pons, microbiology; Pons, pathology; Pons, physiopathology; Reticular Formation, pathology; Reticular Formation, physiopathology; Tuberculoma, Intracranial, diagnosis; Tuberculoma, Intracranial, pathology; Tuberculoma, Intracranial, physiopathology; Tuberculosis, complications |
| Format |
application/pdf |
| Publication Type |
Journal Article |
| Collection |
Neuro-Ophthalmology Virtual Education Library: Journal of Neuro-Ophthalmology Archives: https://novel.utah.edu/jno/ |
| Publisher |
Lippincott, Williams & Wilkins |
| Holding Institution |
Spencer S. Eccles Health Sciences Library, University of Utah |
| Rights Management |
© North American Neuro-Ophthalmology Society |
| Setname |
ehsl_novel_jno |
| ID |
225510 |
| Reference URL |
https://collections.lib.utah.edu/ark:/87278/s6wt209n/225510 |