| Title |
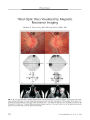
Papilledema in the Assessment of Ventriculomegaly |
| Creator |
Mizrachi, IB; Trobe, JD; Gebarski, SS; Garton, HJ |
| Affiliation |
Goldschleger Eye Institute, Chaim Sheba Medical Center, Tel Hashomer, Israel. irismizrachi@yahoo.com |
| Abstract |
To determine whether ventriculomegaly is associated with ongoing increased intracranial pressure (ICP), physicians often rely on corroborative imaging features such as altered periependymal signal, distortion of ventricular shape, subarachnoid space flattening, and an increase in ventricular size over time. In 2 patients with new headache and altered mental status, symptoms and ventriculomegaly were dismissed as long-standing and not reflective of current ICP elevation. In the first patient, ICP was considered normal because there were no corroborative imaging features of elevated ICP. In the second patient, ICP was considered normal because ventricular size was stable over a 1-year period. The diagnosis of ICP elevation was finally made by ICP monitoring after papilledema was recognized. Ventriculoperitoneal shunting rapidly resolved the papilledema and markedly improved mentation. Brain imaging may often be an unreliable guide to the presence of elevated ICP. In such patients, the finding of papilledema is a critical determinant of management. |
| Subject |
Adult; Cognition Disorders, diagnosis; Cognition Disorders, etiology; Cognition Disorders, physiopathology; Diagnosis, Differential; Diagnostic Errors, prevention & control; Female; Humans; Hydrocephalus, diagnosis; Hydrocephalus, physiopathology; Intracranial Hypertension, diagnosis; Intracranial Hypertension, physiopathology; Lateral Ventricles, pathology; Lateral Ventricles, physiopathology; Lateral Ventricles, radiography; Middle Older people; Papilledema, diagnosis; Papilledema, etiology; Papilledema, physiopathology; Predictive Value of Tests; Tomography, X-Ray Computed; Treatment Outcome; Ventriculoperitoneal Shunt, methods; Ventriculostomy, methods; Vision Disorders, diagnosis; Vision Disorders, etiology; Vision Disorders, physiopathology |
| Format |
application/pdf |
| Publication Type |
Journal Article |
| Collection |
Neuro-Ophthalmology Virtual Education Library: Journal of Neuro-Ophthalmology Archives: https://novel.utah.edu/jno/ |
| Publisher |
Lippincott, Williams & Wilkins |
| Holding Institution |
Spencer S. Eccles Health Sciences Library, University of Utah |
| Rights Management |
© North American Neuro-Ophthalmology Society |
| Setname |
ehsl_novel_jno |
| ID |
225506 |
| Reference URL |
https://collections.lib.utah.edu/ark:/87278/s6wt209n/225506 |