| Title |
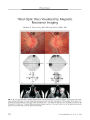
Leber Hereditary Optic Neuropathy Possibly Triggered by Exposure to Tire Fire |
| Creator |
Sanchez, RN; Smith, AJ; Carelli, V; Sadun, AA; Keltner, JL |
| Affiliation |
Department of Ophthalmology, Doheny Eye Institute, University of Southern California, Keck School of Medicine, Los Angeles, California, USA. |
| Abstract |
We report three members of one family, a mother and two daughters aged 4 and 7 years, who developed visual loss from Leber hereditary optic neuropathy within a 19-month period. All three had been exposed to smoke from two large rubber tire fires within the previous 24 months, suggesting the possibility of an epigenetic triggering factor. |
| Subject |
Adult; Air Pollutants, adverse effects; Carbon, adverse effects; Child; Child, Preschool; DNA Mutational Analysis; DNA, Mitochondrial, genetics; Female; Genetic Predisposition to Disease, genetics; Humans; Male; Mutation, genetics; Optic Atrophy, Hereditary, Leber, diagnosis; Optic Atrophy, Hereditary, Leber, etiology; Optic Atrophy, Hereditary, Leber, physiopathology; Optic Nerve, pathology; Optic Nerve, physiopathology; Pedigree; Petroleum, adverse effects; Rubber, adverse effects |
| Format |
application/pdf |
| Publication Type |
Journal Article |
| Collection |
Neuro-Ophthalmology Virtual Education Library: Journal of Neuro-Ophthalmology Archives: https://novel.utah.edu/jno/ |
| Publisher |
Lippincott, Williams & Wilkins |
| Holding Institution |
Spencer S. Eccles Health Sciences Library, University of Utah |
| Rights Management |
© North American Neuro-Ophthalmology Society |
| Setname |
ehsl_novel_jno |
| ID |
225508 |
| Reference URL |
https://collections.lib.utah.edu/ark:/87278/s6wt209n/225508 |