| Title |
Traumatic Optic Neuropathy Caused by Blunt Injury to the Inferior Orbital Rim |
| Creator |
Nishi, T; Ueda, T; Yukawa, E; Ohta, T; Hara, Y |
| Affiliation |
Department of Ophthalmology, Nara Medical University, Nara, Japan. ntomo24@r7.dion.ne.jp |
| Abstract |
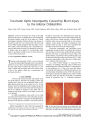
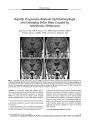
A 48-year-old woman was struck on the right inferior orbital rim by a gardening device and immediately developed complete visual loss in the right eye. Clinical and imaging evaluations failed to disclose any damage to the globe or optic nerve or to their nearby soft tissues and bones. Within months, ipsilateral optic disc pallor, a nerve fiber bundle visual field defect, and a persistently subnormal visual acuity developed. We attribute the visual loss to indirect optic nerve injury. To our knowledge, blunt injury to the inferior orbital rim has not been reported as a cause of this phenomenon. |
| Subject |
Eye Injuries, complications; Eye Injuries, diagnosis; Female; Humans; Middle Older people; Optic Nerve Diseases, diagnosis; Optic Nerve Diseases, etiology; Orbit, injuries; Orbit, radiography; Perimetry; Tomography, X-Ray Computed; Trauma Severity Indices; Visual Acuity; Visual Fields; Wounds, Nonpenetrating, complications; Wounds, Nonpenetrating, diagnosis |
| Format |
application/pdf |
| Publication Type |
Journal Article |
| Collection |
Neuro-Ophthalmology Virtual Education Library: Journal of Neuro-Ophthalmology Archives: https://novel.utah.edu/jno/ |
| Publisher |
Lippincott, Williams & Wilkins |
| Holding Institution |
Spencer S. Eccles Health Sciences Library, University of Utah |
| Rights Management |
© North American Neuro-Ophthalmology Society |
| Setname |
ehsl_novel_jno |
| ID |
225548 |
| Reference URL |
https://collections.lib.utah.edu/ark:/87278/s6n90gwz/225548 |