| OCR Text |
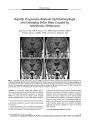
Show PHOTO ESSAY Rapidly Progressive Bilateral Ophthalmoplegia and Enlarging Sellar Mass Caused by Amelanotic Melanoma Saiju Jacob, MD, MRCP, Eleanor Pye, MRCP, Majed Hbahbih, MRCP, Nicholas Messios, DMRD, FRCR, and YusufA. Rajabally, MD FIG. 1. Serial MRI scans. A. Pre- contrast coronal T1 MRI at presentation shows a pituitary mass with minimal cavernous sinus extension bilaterally. B. Post- contrast scan at presentation shows an area of non- enhancement within the gland suggestive of a macroadenoma. C. Post- contrast coronal T1 MRI on day 14 after presentation shows further extension into the cavernous sinuses. Transsphenoidal hypophysectomy showed amelanotic melanoma. D. Post- contrast coronal T1 MRI on day 28 after presentation. There is continued growth of tumor in spite of radiation treatment. Abstract: A 63- year- old woman with diplopia and bilateral ptosis underwent brain MRI that showed a pituitary mass with signal characteristics suggestive of adenoma. Within one week she had developed nearly complete bilateral ophthalmoplegia. A repeat MRI showed extension Departments of Neurology ( SJ, EP, MH, YAR) and Neuroradiology ( NM), University Hospitals of Leicester, Leicester General Hospital, United Kingdom. Address correspondence to Dr. Y. A. Rajabally, MD, Department of Neurology, University Hospitals of Leicester, Leicester General Hospital, LE5 4PW, United Kingdom; E- mail: yusuf. rajabally@ uhl- tr. nhs. uk of the mass into both cavernous sinuses. Hypophysectomy disclosed an amelanotic melanoma. Extensive search for a primary source was unsuccessful. Despite local radiation treatment, the tumor continued to grow and the patient became blind and died within several months of diagnosis. There are seven reported cases of melanoma arising primarily in the sella turcica. Two cases of metastatic melanoma to the cavernous sinuses have been reported. Amelanotic melanoma has not been reported as a cause of cavernous sinus syndrome. ( J Neuro- Ophthalmol 2006; 26: 49- 50) J Neuro- Ophthalmol, Vol. 26, No. 1, 2006 49 Copyright © Lippincott Williams & Wilkins. Unauthorized reproduction of this article is prohibited. J Neuro- Ophthalmol, Vol. 26, No. 1, 2006 Jacob et al A 63- year- old woman had a four- week history of headache and a one- week history of diplopia and left upper lid ptosis. Her past medical history was unrevealing. Examination confirmed left upper lid ptosis with normal eye movements, alignment, pupillary size, and reactions. MRI scan showed enlargement of the pituitary gland to 11 mm with a non- enhancing area on its left side measuring 4X5 mm consistent with macroadenoma ( Fig. 1, A- B). No other intracranial abnormality was demonstrated. When examined two weeks later, she had no horizontal eye movements and markedly reduced vertical movements in the left eye. Repeat MRI ( Fig. IC) showed that the enhancing lesion arising from the pituitary gland had extended into the cavernous sinuses bilaterally. Investigations for infection, inflammation, autoantibodies, tumor markers, endocrine function, and cerebrospinal fluid abnormalities were unremarkable. Transsphenoidal hypophysectomy with debulking of the tumor revealed highly neoplastic cells in the adenohy-pophysis. Tumor markers for epithelial, germ cell, neuroendocrine, primitive neuroectodermal tumors, and lymphoma were negative. Immunoreactivity for SI00 Melan- A and HMB45 was later identified. No pigment was seen on staining with hematoxylin and eosin; Masson Fontana stain showed only very occasional focal pigmentation. The histologic diagnosis was amelanotic melanoma. Within six weeks of admission, she had lost all vision in the left eye, and later in the right eye. Repeat MRI scans during this period showed a rapidly enlarging tumor invading both cavernous sinuses ( Fig. 1, C- D). Detailed der-matological and ophthalmological examinations with CT scanning of the chest, abdomen, and pelvis failed to demonstrate a primary source or evidence of disease activity elsewhere. A six- week course of fractionated radiotherapy was administered to the sellar region. At that point, the patient was able to recognize shapes. Unfortunately, all vision was lost again within weeks. She died shortly thereafter. No autopsy was performed. Intracranial malignant melanomas have generally arisen as metastases from primary lesions outside the cranial cavity. Only 1% of all newly- diagnosed melanomas are primary to the intracranial space ( 1). Melanoma arising primarily from the sella turcica is exceedingly rare, only seven cases having been reported ( 2- 8). One case report of a cavernous sinus syndrome secondary to metastatic malignant melanoma has been published in the English literature ( 9). This patient presented with a cavernous sinus syndrome, the initial MRI being normal. Later he was found to have a metastatic malignant melanoma from a lymph node biopsy. Subsequent MRI showed an enhancing lesion in the region of the cavernous sinus presumably due to metastatic disease. There is a similar case report published in the Japanese literature ( 10). Sellar amelanotic melanoma has not been reported as a cause of cavernous sinus syndrome. Our case points out that MRI cannot differentiate initially between the more common pituitary adenoma and unusual tumors such as melanoma. Had there been more pigment in the tumor, areas of high Tl signal and low T2 signal corresponding to the pigment might have suggested the diagnosis ( 11). The rapidly progressive bilateral ophthalmoplegia and imaging evidence of tumor growth logically gave rise to the mistaken notion of a malignant pituitary adenoma. Pituitary abscess would have been a clinical consideration but imaging features were not consistent with this diagnosis. Given the rapid demise of our patient, we presume that she had occult metastatic disease undetected with CT surveillance. Positron emission tomography may have been more sensitive. Acknowledgments We are grateful for the assistance of Mr. T Hope, Consultant Neurosurgeon, J. Lowe, Professor of Pathology, Queens Medical Centre, Nottingham, United Kingdom, and Dr. R. R Symonds, Consultant Oncologist, Leicester Royal Infirmary, United Kingdom. REFERENCES 1. Greco Crasto S, Soffietti R, Bradac GB, et al. Primitive cerebral melanoma: case report and review of literature. Surg Neurol 2001 ; 5 5: 163- 8. 2. Rousseau A, Bernier M, Kujas M, et al. Primary intracranial melanocytic tumor simulating pituitary macroadenoma: case report and review of the literature. Neurosurgery 2005; 57: E369. 3. Tiittenberg J, Fink W, Back W, et al. A rare primary sellar melanoma. Case report. JNeurosurg 2004; 100: 931^ k 4. Aubin MJ, Hardy J, Comtois R. Primary sellar haemorrhagic melanoma: case report and review of literature. Br J Neurosurg 1997; 11: 80- 3. 5. Chappell PM, Kelly WM, Ercius M. Primary sellar melanoma simulating haemorrhagic pituitary adenoma: MR and pathologic findings. AMR Am J Neuroradiol 1990; 11: 1054- 6. 6. Copeland DD, Sink JD, Seigler HE Primary intracranial melanoma presenting as a suprasellar tumor. Neurosurgery 1980; 6: 542- 5. 7. Scholtz CL, Siu K. Melanoma of the pituitary. Case report. J Neurosurg 1976; 45: 101- 3. 8. Neilson JM, Moffat AD. Hypopituitarism caused by melanoma of the pituitary gland. J Clin Pathol 1963; 16: 144- 9. 9. Harkness KA, Manford MR. Metastatic malignant melanoma presenting as a cavernous sinus syndrome. J Neurol 2004; 251: 224- 5. 10. Nogami K, Nishijima M, Endoh S, et al. Malignant melanoma metastatic to the cavernous sinus and skull with an unknown primary origin: report of a case. No Shinkei Geka 1992; 20: 1017- 20. 11. Lynch SC, Lee AG, Graham SM, et al. Primary melanoma of the sphenoid sinus presenting with a third cranial nerve palsy. JNeuroophthalmol 2005; 25: 289- 92. 50 © 2006 Lippincott Williams & Wilkins Copyright © Lippincott Williams & Wilkins. Unauthorized reproduction of this article is prohibited. |