| Title |
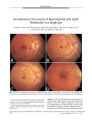
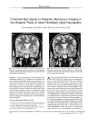
Chiasmal High Signal on Magnetic Resonance Imaging in the Atrophic Phase of Leber Hereditary Optic Neuropathy |
| Creator |
Batio?lu, F; Atilla, H; Eryilmaz, T |
| Affiliation |
Ankara University, School of Medicine, Department of Ophthalmology, Ankara, Turkey. batioglu@hotmail.com |
| Abstract |
A 30-year-old man with Leber hereditary optic neuropathy mutation 11778 displayed no magnetic resonance imaging abnormalities during the acute phase of visual loss in the right eye. Three months later, during the acute phase of visual loss in the left eye, magnetic resonance imaging showed T2 hyperintense signal changes on the right half of the optic chiasm. Six months later, magnetic resonance imaging revealed T2 hyperintense signal changes on both sides of the optic chiasm. This is the first reported case of optic chiasmal involvement on magnetic resonance imaging in the atrophic phase of Leber hereditary optic neuropathy. |
| Subject |
Adult; Fluorescein Angiography; Humans; Magnetic Resonance Imaging/methods; Male; Optic Atrophy, Hereditary, Leber/diagnosis; Optic Atrophy, Hereditary, Leber/pathology; Optic Atrophy, Hereditary, Leber/physiopathology; Optic Chiasm/pathology; Optic Chiasm/physiopathology; Visual Fields/physiology |
| Format |
application/pdf |
| Publication Type |
Journal Article |
| Collection |
Neuro-Ophthalmology Virtual Education Library: Journal of Neuro-Ophthalmology Archives: https://novel.utah.edu/jno/ |
| Publisher |
Lippincott, Williams & Wilkins |
| Holding Institution |
Spencer S. Eccles Health Sciences Library, University of Utah |
| Rights Management |
© North American Neuro-Ophthalmology Society |
| Setname |
ehsl_novel_jno |
| ID |
225255 |
| Reference URL |
https://collections.lib.utah.edu/ark:/87278/s6fr32qh/225255 |