| OCR Text |
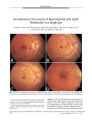
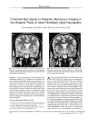
Show PHOTO ESSAY Simultaneous Occurrence of Neuroretinitis and Optic Perineuritis in a Single Eye Kenneth T. Wals, MD, Husam Ansari, MD, PhD, Szilard Kiss, MD, Kevin Langton, CRA, A. John Silver, MD, and Jeffrey G. Odel, MD FIG. 1. Fundus photographs of the OD at presentation ( A), and at 5 days ( B), 12 days ( C), and 33 days ( D) after presentation. Arrow indicates triangular patch of edema. These ophthalmoscopic findings are consistent with neuroretinitis. Edward S. Harkness Eye Institute, Department of Ophthalmology, ( KTW, HA, SK, KL, JGO), and the Department of Radiology ( AJS), Columbia University, New York, New York. Address correspondence to Jeffrey G. Odel, MD, Edward S. Harkness Eye Institute, 635 West 165th Street, New York, NY 10032, USA; E- mail: odell@ aol. com Abstract: A 52- year- old woman presented with pain, decreased visual acuity, decreased color vision, and visual field loss in the OD. Fundus examination revealed optic disc edema and later a macular star figure consistent with neuroretinitis. Magnetic resonance imaging showed enhancement of the orbital optic nerve sheath and perineural Copyright © Lippincott Williams & Wilkins. Unauthorized reproduction of this article is prohibited. 24 JNeuro- Ophthalmol, Vol. 23, No. 1, 2003 PHOTO ESSAY JNeuro- Ophthalmol, Vol. 23, No. 1, 2003 fat suggestive of optic perineuritis. The patient was not treated. At 11 months, visual function and fundus examination had returned to normal. This unusual simultaneous occurrence of neuroretinitis and optic perineuritis suggests that these two entities may have a similar pathogenesis. ( JNeuro- Ophthalmol 2003; 23: 24- 27) A 52- year- old woman with no significant medical or ocular history experienced pain and visual loss OD. Ten days earlier, she had awakened with pain on eye movement and tenderness OD. Four days later, she had noticed loss of vision OD. Best- corrected distance visual acuity was 20/ 140 OD and 20/ 20 OS. She could not identify any American Optical/ Hardy- Rand- Rittler color plates, including controls, with the OD; she identified three of six test plates with the OS. Humphrey 24- 2 perimetry revealed a central sco-oma with nasal visual field loss OD and a normal visual field OS. A 0.9 neutral density afferent pupillary defect was present OD. Moderate disc swelling and mild venous dilatation was present OD. A subretinal triangular yellow patch approximately 0.3 disc diameters in size was noted nasal to the fovea ( Fig. 1A). Fluorescein angiography showed disc leakage OD but did not reveal any abnormalities in the vicinity of the yellow patch. The left fundus and the remainder of her ophthalmologic and neurologic exams were normal. Syphilis serologies, cat- scratch titer, Lyme titer, anti- DNA antibody test, and chest radiograph were negative. A complete blood count, erythrocyte sedimentation rate, an-giotensin- converting enzyme level, thyroid stimulating hormone level, vitamin B12 level, and cerebrospinal fluid studies, including oligoclonal band testing, were normal. Anti- nuclear antibody titer was 1: 320 in a nucleolar pattern. Magnetic resonance imaging ( MRI) revealed postcontrast enhancement of the right optic nerve sheath and increased T2 signal in the intraconal fat of the right orbit ( Fig. 2). Five days later, visual acuity had improved slightly to 20/ 100 OD, the afferent pupillary defect had improved to 0.6 neutral density filter log units, color vision had not improved, and ophthalmoscopy revealed increased macular edema and a nerve fiber layer hemorrhage ( Fig. IB). Twelve days after presentation, the initial stages of macular star formation had appeared nasal to the fovea ( Fig. 1C). Thirty- three days after presentation, a fully formed macular star surrounded the fovea ( Fig. ID). Visual acuity had improved to 20/ 30, the afferent pupillary defect remained at 0.6,4.5 of 6 color plates were identified OD, and the patient's visual fields were normal. Eleven months after presentation, the patient's fundus and visual acuity had returned to normal. FIG. 2. Postcontrast T1 ( A) and fat-suppressed T2 ( B) coronal magnetic resonance imaging of the orbits. A: Enhancement and thickening of the right optic nerve sheath are evident ( arrow) with sparing of the optic nerve itself. B: Fat stranding within the orbital soft tissue is evident on the right side. These imaging findings are consistent with optic perineuritis. Copyright © Lippincott Williams & Wilkins. Unauthorized reproduction of this article is prohibited. 25 JNeuro- Ophthalmol, Vol. 23, No. 1, 2003 PHOTO ESSAY Neuroretinitis is an inflammatory optic neuropathy characterized by disc swelling followed 1 to 3 weeks later by the precipitation of hard exudates in the macula in a star or wing shape ( 1). There is ipsilateral visual acuity and field loss, dyschromatopsia, and a relative afferent pupillary defect. Prior to macular star development, neuroretinitis is virtually indistinguishable from papillitis but may be suspected if intraretinal or subretinal fluid is seen. Optic perineuritis, another inflammatory optic neuropathy, is defined by involvement of one or more of the following: the optic nerve periphery, the optic nerve sheath, and the perineural orbital fat ( 2). This peripheral involvement can be seen on MRI or can be inferred clinically by the relative absence of signs or symptoms other than disc swelling and peripheral visual field loss. It is very important to distinguish optic perineuritis and neuroretinitis from papillitis as the latter is associated with an increased risk of developing multiple sclerosis whereas the other conditions are not ( 3- 5). Our patient had neuroretinitis and optic perineuritis simultaneously in the same eye. She experienced the acute onset of pain on eye movement and ocular tenderness followed by ipsilateral visual loss 4 days later. Examination revealed a visual field defect, a relative afferent pupillary defect, and a swollen optic disc. Although this combination of signs and symptoms is highly suggestive of optic neuritis, the patient's age and the presence of a triangular yellow patch in the macula are atypical. The average age at the time of the initial attack of optic neuritis is 33 years, with 85% of cases occurring between the ages of 20 and 50 ( 6). Because of her atypical presentation, the patient underwent a full neurologic work- up, which included cerebrospinal fluid analysis that was normal and MRI studies that showed perineural sheath and intraconal fat enhancement. Thirty percent of patients with optic neuritis develop clinically definite multiple sclerosis within 5 years of the onset of symptoms ( 3). In contrast, patients with neuroretinitis do not have an increased risk of developing multiple sclerosis ( 5). Neuroretinitis is an acute inflammatory disorder in which the specific etiology is rarely found. When an etiology is found, it is most often due to cat scratch disease, syphilis, Lyme disease, toxoplasmosis, or leptospirosis ( 7). While neuroretinitis may be difficult to distinguish from optic neuritis on initial presentation, the subsequent appearance of the macular star confirms the diagnosis of neuroretinitis. In our patient, the triangular yellow patch seen on presentation was most likely a lipid- rich deposition that eventually formed the macular star. There was no leakage of macular vessels on fluorescein angiography, so the macular star must have originated from disc leakage. When evaluating for neuroretinitis, it is common clinical practice to examine the patient 2 weeks after the onset of symptoms for the presence of macular star. In our patient, the macular star was not evident until approximately 3 weeks after the onset of symptoms, suggesting that 2- week follow- up may not be sufficient to rule out neuroretinitis. Optic perineuritis can also have a presentation that mimics optic neuritis. MRI with fat suppression and Gd- DTPA contrast enhancement is the diagnostic tool of choice in differentiating between these two disease processes. In optic neuritis, MRI may reveal enhancement of both the optic nerve and its sheath, and in 62% of patients, shows multiple demyelinating lesions in the central nervous system ( 8). In optic perineuritis, enhancement of the optic nerve sheath and orbital fat is more prominent than enhancement of the nerve itself ( 4). This was true in our patient who had no evidence of demyelinating lesions on MRI. It is important to distinguish optic neuritis from optic perineuritis because their treatment protocols and prognoses differ. Optic perineuritis generally responds rapidly to high dose oral corticosteroids and is not associated with the development of multiple sclerosis ( 9). Initial treatment with oral corticosteroids, however, is contraindicated in patients with demyelinating optic neuritis ( 10). Whereas visual symptoms resolve without treatment in patients with neuroretinitis ( 11), failure to treat patients with optic perineuritis usually results in further deterioration of vision ( 9). The resolution of visual symptoms in our patient suggests that this case behaved more like neuroretinitis than optic perineuritis. Zhang et al ( 12) previously reported a case of a macular star with optic perineuritis. In this case, the diagnosis of optic perineuritis was made histopathologically because a postcontrast computed tomography ( CT) scan, which does not usually provide enough resolution to distinguish perineural from neural enhancement ( 9), demonstrated diffuse thickening of both the optic nerve and sheath. Our case is unique because we were able to diagnose optic perineuritis by using MRI. Nevertheless, taken together, our case and that of Zhang et al ( 12) suggest a link between the pathogenesis of optic perineuritis and that of neuroretinitis. The only reported etiology common to both neuroretinitis and optic perineuritis is syphilis ( 7,13), a condition that was ruled out in our patient. There is evidence that macular star formation is associated with leakiness of optic disc vessels, implying a vasculopathic or vasculitic process ( 11). Similarly, vascu-litides have been shown to occur in cases of optic perineuritis ( 9,12,14,15). Furthermore, our case demonstrates that a macular star does not exclude retrobulbar pathology. Although no obvious etiologic factors were identified in this patient, she had a positive antinuclear antibody titer with a nucleolar pattern. This can be found in patients with either scleroderma or polymyositis. However, this patient had no signs or symptoms of either of these diseases. Copyright © Lippincott Williams & Wilkins. Unauthorized reproduction of this article is prohibited. 26 © 2003 Lippincott Williams & Wilkins PHOTO ESSAY JNeuro- Ophthalmol, Vol. 23, No. 1, 2003 REFERENCES 1. Gass JD. Diseases of the optic nerve that may simulate macular disease. Tr Am Acad Ophth Otol 1977; 83: 763- 70. 2. Albert DM, Jakobiec FA. Principles and Practice of Ophthalmology: Clinical Practice. Philadelphia: WB Saunders; 1994: 1923- 32. 3. Optic Neuritis Study Group. The 5 - year risk of MS after optic neuritis. Experience of the optic neuritis treatment trial. Neurology 1997; 49: 1404- 13. 4. Fay AM, Kane SA, Kazim M, et al. Magnetic resonance imaging of optic perineuritis. J Neuro- Ophthalmol 1997; 17: 247- 9. 5. Parmley VC, Schiffman JS, Maitland CG, et al. Does neuroretinitis rule out multiple sclerosis? Arch Neurol 1987; 44: 1045- 8. 6. Rizzo JF, Lessel S. Risk of developing multiple sclerosis after uncomplicated optic neuritis: a long- term prospective study. Neurol-ogy 1988; 38: 185- 90. 7. Ghauri RR, Lee AG. Optic disk edema with a macular star. Surv Ophthalmol 1998; 43: 270- 4. 8. Frederiksen JL, Larsson HB, Henriksen O, et al. Magnetic resonance imaging of the brain in patients with acute monosymptomatic optic neuritis. Acta Neurol Scand 1989; 80: 512- 7. 9. Purvin V, Kawasaki A, Jacobson DM. Optic perineuritis: clinical and radiographic features. Arch Ophthalmol 2001; 119: 1299- 1306. 10. Beck RW, Cleary PA. Optic neuritis treatment trial. One- year follow- up results. Arch Ophthalmol 1993; 111: 773- 5. 11. Casson RJ, O'day J, Crompton JL. Leber's idiopathic stellate neuroretinitis: differential diagnosis and approach to management. ANZ J Ophthalmol 1999; 27: 65- 9. 12. Zhang TL, Shao SF, Zhang T, et al. Idiopathic inflammation of optic nerve simulating optic nerve sheath meningioma: CT demonstration. JComput Assist Tomogr 1987; 11: 360- 1. 13. Frohman L, Wolansky L. Magnetic resonance imaging of syphilitic optic neuritis/ perineuritis. J Neuro- Ophthalmol 1997; 17: 57- 9. 14. Margo CE, Levy MH, Beck RW. Bilateral idiopathic inflammation of the optic nerve sheaths. Light and electron microscopic findings. Ophthalmol 1989; 96: 200- 6. 15. Rush JA, Kennerdell JS, Martinez AJ. Primary idiopathic inflammation of the optic nerve. Am J Ophthalmol 1982; 93: 312- 6. Copyright © Lippincott Williams & Wilkins. Unauthorized reproduction of this article is prohibited. 27 |