| OCR Text |
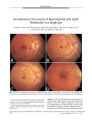
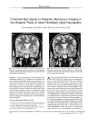
Show LETTERS TO THE EDITOR Editor's note: The Journal of Neuro- Ophthalrnology welcomes letters as written or e- mail correspondence. Send e- mail to jdtrobe@ umich. edu. Optic Nerve and Chiasmal Enhancement In Leber Hereditary Optic Neuropathy To the Editor: Optic nerve enhancement on magnetic resonance imaging ( MRI) has been used to help differentiate the acute phase of optic neuritis from Leber hereditary optic neuropathy ( LHON). However, retrobulbar optic nerve enhancement with gadolinium administration may occasionally occur in the acute phase of LHON ( 1). We describe three cases to emphasize that this MRI finding should not dissuade physicians from including LHON in the differential diagnosis of an acute optic neuropathy. Case 1 An 18- year- old man noted painless sequential visual loss in both eyes to count finger visual acuity OD and 20/ 80 OS. Goldmann perimetry showed large central scotomas OU. Pupils were 7 mm OU with normal reactivity and a 0.9 log unit right relative afferent pupillary defect. Ocular motility was normal. Ophthalmoscopy showed disc elevation with obscuration of the disc margins OU. A detailed neurologic examination was otherwise normal. MRI of the brain and orbits with and without orbital fat suppression and gadolinium showed enhancement of both optic nerves ( Fig. 1). Mitochondrial DNA testing revealed a mutation at nucleotide position 3460 compatible with LHON. Case 2 A 7- year- old boy noted bilateral painless visual loss to 20/ 100 OD and 20/ 400 OS. Goldmann perimetry showed large central scotomas OU. Pupils were 4 mm OU with normal reactivity and left relative afferent pupillary defect. Ocular motility was normal. Ophthalmoscopy showed disc pallor OU. A detailed neurologic examination was otherwise normal. MRI of the brain and orbits with and without orbital fat suppression and gadolinium showed enhancement of both optic nerves with enlargement of the optic chiasm ( Fig. 2). Mitochondrial DNA testing revealed a mutation at nucleotide position 11778 compatible with LHON. Case 3 A 24- year- old man noted bilateral painless sequential visual loss to 20/ 300 OU. Automated perimetry showed superior altitudinal and central defects OU. Pupils were 3 mm OU with normal reactivity without a relative afferent pupillary defect. Ocular motility was normal. Ophthalmoscopy showed disc elevation with obscuration of the disc margins with telangiectatic dilated vessels on both optic nerve heads. There was also a blot hemorrhage off the superi-otemporal arcade on the right ( Fig. 3D). A detailed neurologic examination was otherwise normal. MRI of the brain and orbits with and without orbital fat suppression and gadolinium showed enhancement of both optic nerves ( Fig. 3 A- C). Mitochondrial DNA testing revealed a mutation at nucleotide position 11778 compatible with LHON. Gadolinium, which does not normally cause optic nerve enhancement by crossing the blood- brain barrier, will do so in pathologic states, which disrupt the blood-brain barrier within the optic nerve ( 2). An affected optic nerve enhances because gadolinium induces a local magnetic field resulting in a bright signal on Tl- weighted fat suppressed images ( 2). Evidently, bridging of the blood-brain barrier occurs in LHON and in inflammatory optic neuropathies, as we demonstrate here. Our cases had other confounding diagnostic factors, namely enlargement of the optic nerves and chiasm on MRI ( Case 2) and retinal hemorrhage on funduscopy ( Case 3). Chiasmal enlargement in LHON was recently described in LHON ( 3); retinal hemorrhage has also been reported, but occurs rarely LHON ( 4). Acknowledgments This work was supported in part by an unrestricted grant from the Research to Prevent Blindness, Inc. New FIG. 1. Case 1. T- 1 axial ( A) and coronal ( B) fat- suppressed, enhanced magnetic resonance imaging scan of the orbits shows optic nerve enhancement bilaterally. Copyright © Lippincott Williams & Wilkins. Unauthorized reproduction of this article is prohibited. 104 JNeuro- Ophthalmol, Vol. 23, No. 1, 2003 LETTERS TO THE EDITOR JNeuro- Ophthalmol, Vol. 23, No. 1, 2003 FIG. 2. Case 2. T- 1 axial ( A) and coronal ( B, C) enhanced magnetic resonance imaging scan of the brain shows optic nerve enlargement and enhancement OU and chiasmal enlargement ( C). York, New York; the Fund for the New Jersey Blind, Newark, New Jersey; Lions Eye Research Foundation of New Jersey, Newark, New Jersey; and the Eye Institute of New Jersey, Newark, New Jersey. Roger E. Turbin, MD Department of Ophthalmology New Jersey Medical School Newark, New Jersey Michael S. Vaphiades, DO Departments of Ophthalmology, Neurology and Neurosurgery University of Alabama Birmingham, Alabama vaphiades@ eyes. uab. edu Paul H. Phillips, MD Department of Ophthalmology University of Arkansas for Medical Sciences Little Rock, Arkansas Phillip spaulh@ Uams. edu REFERENCES Vaphiades MS, Newman NJ. Optic nerve enhancement on orbital magnetic resonance imaging in Leber's hereditary optic neuropathy. J Neuro- ophthalmol 1999; 19: 238- 9. Guy J, Mancuso A, Quisling RG, et al. Gadolinium- DTPA-enhanced magnetic resonance imaging in optic neuropathies. Ophthalmology 1990; 97: 592- 600. Phillips PH. " I can't read." 33rd Annual Frank B. Walsh Meeting Platform Presentation, April 21- 22, 2001, Ann Arbor, Michigan. Newman NJ. Hereditary Optic Neuropathies. In: Miller NR, Newman NJ, eds. Walsh & Hoyt's Clinical Neuro- Ophthalmology. 5th ed. Baltimore: Williams & Wilkins. 1998: 741- 75. IP ^^ L^^ fc ^^ S^ JtM v _^ SB FIG. 3. Case 3. T- 1 weighted axial ( A, B) and coronal ( C) fat- suppressed, enhanced magnetic resonance imaging scan of the orbits shows optic nerve enhancement OU. Part D shows a blot hemorrhage near the superotemporal arcade in the right fundus. Copyright © Lippincott Williams & Wilkins. Unauthorized reproduction of this article is prohibited. 105 JNeuro- Ophthalmol, Vol. 23, No. 1, 2003 LETTERS TO THE EDITOR Photophobia in Anterior Visual Pathway Lesions To the Editor: Aki Kawasaki, MD, and Valerie Purvin, MD, reported five patients with photophobia associated with large compressive chiasmal lesions ( 1). They described some possible etiologies for this finding including chemical meningitis. In an accompanying editorial, Jonathan D. Trobe, MD, postulated " upregulated" or hypersensitive trigeminal endings as another possible mechanism ( 2). In reporting seeing several patients with pituitary adenomas and photophobia associated with progressive loss of vision, we postulated that one potential mechanism for photophobia was damage to the thalamus and secondary " central dazzle" ( 3, 4,5). We wonder if the authors could comment on the presence or absence of compression of the hypothalamic axes in their patients and the possibility of dazzle as a mechanism for photophobia. Andrew G. Lee, MD The University of Iowa Hospitals and Clinics Iowa City, Iowa andrew- lee@ uiowa. edu Neil R. Miller, MD The Johns Hopkins Hospital Baltimore, Maryland nrmiller@ jhmi. edu REFERENCES 1. Kawasaki A, Purvin VA. Photophobia as the presenting visual symptom of chiasmal compression. J Neuro- ophthalmol 2002; 22: 3- 8. 2. Trobe JD. Photophobia in anterior visual pathway disease. J Neuro-ophthalmol 2002; 22: 1- 2. 3. Lee AG, Miller NR. Neuro- ophthalmological findings in pituitary adenomas. In Landolt AM, Vance ML, Reilly PL, eds. New York: Churchill Livingstone, 1996: 170. 4. Gutrecht JA, Lessell IM, Zamani AA. Central dazzle in trigeminal sensory neuropathy. Neurology 1990; 40: 722- 3. 5. Cummings JL, Gittinger JW Jr. Central dazzle. A thalamic syndrome? Arch Neurol 1981; 38: 372- 4. Reply: The authors thank Andrew G. Lee, MD, and Neil R. Miller, MD for their interest in our paper and their comment on their own experience with pituitary adenomas and photophobia ( 1). The radiographs of two of our five patients ( Cases 1 and 3) showed involvement of the infundibulum and/ or hypothalamic region by the suprasellar mass ( 2). The origin of central dazzle is not exactly known, but it is postulated to be related to an alteration of the " optic- trigeminal summation system," an interaction that presumably occurs at the upper midbrain- thalamic region ( 3). Because none of our patients demonstrated lesions in this area, we did not believe that central dazzle was a component of the light-induced discomfort experienced by our patients. However, as we mentioned in our paper, the mechanism for the photophobia in our series of patients with chiasmal compression remains speculative, and as Drs. Lee and Miller implied, may be multifactorial. Aki Kawasaki, MD Hopital Ophtalmique Jules Gonin Lausanne, Switzerland Fborruat@ hola. hospvd. ch Valerie Purvin, MD Midwest Eye Institute Indianapolis, Indiana Vpurvin@ iupui. edu REFERENCES 1. Lee AG, Miller NR. In: Landolt AM, Vance ML, Reilly PL, eds. Neuro- ophthalmological findings in pituitary adenomas. New York: Churchill Livingstone, 1996: 170. 2. Kawasaki A, Purvin VA. Photophobia as the presenting visual symptom of chiasmal compression. J Neuro- ophthalmol 2002 ; 22: 3- 8. 3. Eckardt LB, McLean JM, Goodell H. Experimental studies on headache: the genesis of pain from the eye. In: Wolff HG, Gasser HS, Hinsey JC, eds. Proceedings of the Association for Research in Nervous and Mental Disease Baltimore: Williams and Wilkins. 1943: 209- 27. Micropsia and Dissociative Disorders To the Editor: The vast majority of micropsia cases in PubMed literature are attributed to organic pathology. In clinical practice, there are many cases without any relevant organic findings. In dissociative disorders, there are distortions of perceptions as well as self experience and memory, while reality testing remains adequate. The Dissociative Experiences Scale ( DES) is a patient- administered self- rating scale that can be easily used without special education ( 1). In psychiatric practice, we have come across three patients with micropsia as a prominent symptom. A 40- year- old woman reported seeing things, especially cars, smaller than they were, and was afraid that she would be run over by one; a 22- year- old woman suffering from micropsia felt that the walls around her were tumbling down; and a 51- year- old railroad worker occasionally saw trains as small as toy trains. Their DES scores ( 31.4, 30.4, and 51.0) were far above normal range ( 0- 20/ 100), and each of them received the diagnosis of a dissociative disorder in a structured Copyright © Lippincott Williams & Wilkins. Unauthorized reproduction of this article is prohibited. 106 © 2003 Lippincott Williams & Wilkins LETTERS TO THE EDITOR JNeuro- Ophthalmol, Vol. 23, No. 1, 2003 psychiatric examination. A strong correlation between micropsia and DES score was also found in a nonclinical sample of 297 subjects ( 2). We suggest that neuro- ophthalmologists consider that micropsia may be a manifestation of a dissociative disorder. The DES can be used to screen for dissociative disorders in psychiatric examinations. Tapio Lipsanen, MD Jyrki Korkeila, MD, PhD Simo Saarijarvi, MD, PhD Hannu Lauerma, MD, PhD Psychiatric Clinic University of Turku Turku, Finland hannu. lauerma@ om. fi REFERENCES 1. Steinberg M, Rounsaville B, Cicchetti D. Detection of dissociative disorders in psychiatric patients by a screening instrument and a structured diagnostic interview. Am J Psychiatry 1991; 148: 1050- 4. 2. Lipsanen T, Lauerma H, Peltola P, Kaet al. Visual distortions and dissociation. JNerv Merit Dis 1999; 187: 109- 12. Guillain- Barre Syndrome To the Editor: I was surprised to read the claim by Delaney and El-ston ( 1) that they " describe the first reported case of crocodile tears in Guillain- Barre syndrome," especially since it was indeed reported before in the Journal of Clinical Neuro- Ophthalmology ( 2) 14 years ago! Authors, reviewers, and editors should remain aware that an apparently new clinical observation has probably been made before. Thomas Hedges, III, MD Boston, Massachusetts REFERENCES 1. Delaney YM, Elston JS. Bilateral crocodile tears in a patient with Guillain- Barre syndrome. J Neuro- Ophthalmol 2002; 22: 113- 5. 2. Bloom SM, Hedges TR. Crocodile tears following the Guillain- Barre syndrome. J Clin Neuro- Ophthalmol 1988: 8: 113- 4. Copyright © Lippincott Williams & Wilkins. Unauthorized reproduction of this article is prohibited. 107 |