| Title |
The Heidenhain Variant of Creutzfeldt-Jakob Disease - A Case Series |
| Creator |
Parker, Sarah E; Gujrati, Meena; Pula, John H; Zallek, Sarah N; Kattah, Jorge C |
| Affiliation |
Departments of Neurology (SEP, JHP, SZ, JCK) and Neuropathology (MG), Illinois Neurologic Institute, University of Illinois, Peoria, Illinois |
| Abstract |
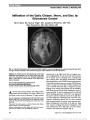
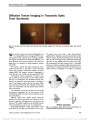
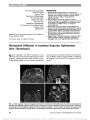
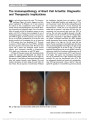
To study the neuro-ophthalmologic characteristics of patients with the visual variant of Creuztfeldt-Jakob disease (CJD) predominantly affecting the occipital and parietal lobes, known as the Heidenhain variant (HvCJD). The initial symptoms and findings may overlap with other posterior cerebral degenerative disorders. We reviewed our experience with HvCJD including clinical course and results of neuroimaging, electroencephalography (EEG), and cerebrospinal fluid (CSF) studies. Neuropathological postmortem findings were reviewed when available to confirm the clinical impression. Retrospective study of HvCJD patients examined in the past 15 years at a single tertiary referral university hospital. Rapid rate of visual and neurological deterioration and abnormal diffusion-weighted imaging (DWI) were characteristic for HvCJD. Three patients displayed abnormalities in DWI, EEG, and CSF and had rapid clinical progression, leading to a clinical diagnosis of HvCJD. None underwent diagnostic cerebral biopsy. In 2 patients, the diagnosis of sporadic CJD was confirmed by postmortem neuropathologic, immunohistochemical, and genetic studies. The gold standard for establishing the diagnosis of HvCJD is based on the characteristic histopathologic findings and molecular confirmation. Concern with potential iatrogenic CJD, related to surgical instrumentation or operating room prion contamination, has limited the availability of confirmatory brain biopsy. Our case series illustrates how the combination of clinical neuroimaging and EEG studies and 14:3:3 protein and other neuronal protein marker levels can lead to the diagnosis of HvCJD. Immunohistochemical analysis and genetic testing at a specialized prion research center will assist in identifying the sporadic variant and genetic forms of CJD. |
| Subject |
Older people; Brain; Creutzfeldt-Jakob Syndrome; Diagnosis, Differential; Electroencephalography; Fatal Outcome; Female; Follow-Up Studies; Humans; Magnetic Resonance Imaging; Male; Retrospective Studies |
| Format |
application/pdf |
| Publication Type |
Journal Article |
| Collection |
Neuro-Ophthalmology Virtual Education Library: Journal of Neuro-Ophthalmology Archives: https://novel.utah.edu/jno/ |
| Publisher |
Lippincott, Williams & Wilkins |
| Holding Institution |
Spencer S. Eccles Health Sciences Library, University of Utah |
| Rights Management |
© North American Neuro-Ophthalmology Society |
| Setname |
ehsl_novel_jno |
| ID |
227541 |
| Reference URL |
https://collections.lib.utah.edu/ark:/87278/s67979sg/227541 |