| Title |
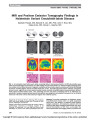
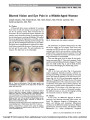
Reversal of Ischemic Retinopathy Following Balloon Angioplasty of a Stenotic Ophthalmic Artery |
| Creator |
Hwang, Gyo Jun; Woo, Se Joon; Hwang, Jeong-Min; Jung, Cheolkyu; Park, Kyu Hyung; Kwon, O-Ki |
| Affiliation |
Department of Neurosurgery, Seoul National University College of Medicine, Seoul National University Bundang Hospital |
| Abstract |
A 65-year-old woman who had undergone internal carotid artery stenting and was being maintained on antiplatelet therapy developed features suggesting ipsilateral reduced retinal artery perfusion. Injection of urokinase into the ophthalmic artery provided temporary improvement. When manifestations of retinal arterial ischemia recurred, angiography revealed worsening stenosis at the origin of the ophthalmic artery. Balloon angioplasty at that site successfully restored visual acuity and reversed the ischemic fundus abnormalities. This is the first report of ophthalmic artery balloon angioplasty in this setting. |
| Subject |
Older people; Angioplasty, Balloon; Constriction, Pathologic; Coronary Angiography; Female; Fluorescein Angiography; Humans; Ophthalmic Artery |
| Format |
application/pdf |
| Publication Type |
Journal Article |
| Collection |
Neuro-Ophthalmology Virtual Education Library: Journal of Neuro-Ophthalmology Archives: https://novel.utah.edu/jno/ |
| Publisher |
Lippincott, Williams & Wilkins |
| Holding Institution |
Spencer S. Eccles Health Sciences Library, University of Utah |
| Rights Management |
© North American Neuro-Ophthalmology Society |
| Setname |
ehsl_novel_jno |
| ID |
227084 |
| Reference URL |
https://collections.lib.utah.edu/ark:/87278/s6f79jm2/227084 |