| OCR Text |
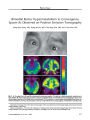
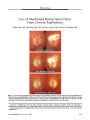
Show ORIGINAL CONTRIBUTION Spontaneous Resolution of a Meckel's Cave Arachnoid Cyst Causing Sixth Cranial Nerve Palsy Maud Jacob, MD, Sachin Gujar, MD, Jonathan Trobe, MD, and Dheeraj Gandhi, MD Abstract: A 32-year-old pregnant woman devel-oped a progressive right sixth cranial nerve palsy as an isolated finding. Brain MRI disclosed a discrete lobulated lesion centered in the right Meckel's cave with intermediate signal on T1, high signal on T2, and diffusion characteristics similar to those of cerebro-spinal fluid on apparent diffusion coefficient mapping. The initial radiologic diagnosis was schwannoma or meningioma. No intervention occurred. Shortly after cesarean delivery, the abduction deficit began to lessen spontaneously. One month later, the abduction deficit had further improved; 7 months later it had completely resolved. Repeat MRI after delivery failed to disclose the lesion, which was now interpreted as consistent with an arachnoid cyst arising within Meckel's cave. Twenty-one similar cases of Meckel's cave arachnoid cyst or meningocele have been reported, 7 found incidentally and 14 causing symptoms, 2 of which produced ipsilateral sixth cranial nerve palsies. All previously reported symptomatic patients were treated surgically. This is the first report of an arachnoid cyst arising from Meckel's cave in pregnancy and having spontaneous resolution. (J Neuro-Ophthalmol 2008;28:186-191) Evagination of arachnoid or arachnoid plus dura from Meckel's cave into the petrous apex is rare. Twenty-one cases have been well documented (1-10). The signature MRI findings are a discrete cystic mass that has low signal on T1 and high signal on T2 and cerebrospinal fluid (CSF)- like signal on apparent diffusion coefficient (ADC) map-ping. Although some cysts have been found incidentally, others have caused either diplopia or trigeminal dysfunc-tion by compression of adjacent structures or a CSF leak. We report a patient who developed a sixth cranial nerve palsy as the result of an ipsilateral Meckel's cave arachnoid cyst. After delivery, the sixth cranial nerve palsy improved. A follow-up MRI 1 month later showed complete dis-appearance of the lesion. We believe this to be the first case of a Meckel's cave arachnoid cyst reported in pregnancy and having spontaneous resolution afterwards. CASE REPORT A 32-year-old woman in the 28th week of a normal pregnancy complained of binocular horizontal diplopia of 2 weeks' duration. On her initial examination, abduction of the right eye was reduced to 60%. Measurements of alignment showed a 10 prism-diopter esotropia in primary gaze, worsening to 20 on right gaze and improving to 4 on left gaze. Results for the rest of the neuro-ophthalmologic examination were normal. Examination 1 month later disclosed a complete lack of abduction in the right eye. At that time, she reported having experienced a 3-week episode of intense right periocular pain that resolved spontaneously. Otherwise, there were no neurologic manifestations. Brain MRI performed without contrast injection because of her pregnancy showed a well-defined, lobulated, extra-axial lesion with its epicenter in the right Meckel's cave. The lesion measured 11 mm anteroposteriorly and 6 mm transversely. It demonstrated intermediate signal intensity on T1 and high (fluid-like) signal on T2. On the ADC map, the lesion showed diffusion coefficient values similar to those of CSF (Fig. 1). The initial radiologic diagnosis was nerve sheath tumor (schwannoma) or, less likely, meningioma. Ten weeks after the onset of diplopia, she underwent cesarean section delivery for fetal distress. The birth was otherwise normal. On the day after delivery, she noticed slight improvement in her diplopia. By 1 month after delivery, abduction of the right eye had improved to 70%, and there were no other findings. Seven months after delivery, she had had completely recovered normal ocular motility. A second MRI, performed with contrast medium at 1 month after delivery and 3 months after the beginning of her symptoms, failed to disclose the lesion (Fig. 2). Departments of Ophthalmology (MJ, JT), Neurology (JT), and Radiology (Neuroradiology) (SG, DG),University of Michigan, Ann Arbor, Michigan. Address correspondence to Jonathan Trobe, MD, Kellogg Eye Center, 1000 Wall Street, Ann Arbor, MI 48105; E-mail: jdtrobe@umich.edu 186 J Neuro-Ophthalmol, Vol. 28, No. 3, 2008 Head CT performed 3 months after delivery disclosed no erosion of the petrous apex. Based on the typical location of the lesion and its imaging characteristics, a diagnosis of an arachnoid cyst arising from Meckel's cave was made in retrospect. DISCUSSION Our patient developed a right sixth cranial palsy during pregnancy that was associated with a cystic lesion in the right Meckel's cave. After delivery, the sixth nerve palsy regressed, and at 1 month after delivery the lesion had vanished on MRI. Cystic lesions in that region have been given various names: Meckel's cave arachnoid cyst (1,2), petrous apex cephaloceles (3-5), petrous apex arachnoid cyst (6-9), and arachnoid cyst involving the Gasserian ganglion (10). They are all cystic lesions centered in the posterior portion of Meckel's cave that may expand into the petrous apex when they grow and erode the bone in this case. If the surgeon discovers a herniation of dura and arachnoid, the term ‘‘meningocele'' is applied; if the cyst lining consists only of arachnoid, the term ‘‘arachnoid cyst'' is applied (9). The arachnoid cyst may have herniated through a hole in the adjacent dura (10). Eighteen cases of petrous apex arachnoid cysts have been studied previously by MRI (1-10,13). In two cases, imaging descriptions included only T2 imaging character-istics (2,5). Low T1 and high T2 signals have been found in all but one reported case (3,4,6-9), in which intermediate to high T2 signal was reported (7) (Fig. 3). Mild rim enhancement on postcontrast scans has been noted in FIG. 1. MRI performed during pregnancy. A. Precontrast T1 axial MRI shows a lesion in the right Meckel's cave with intermediate signal intensity. B-C. T2 axial MRI shows a fluid-like high signal on T2. Note the prominent septations within the lesion (black arrows). D. Apparent diffusion coefficient map shows cerebrospinal fluid-like diffusion characteristics (arrow). FIG. 2. MRI performed 1 month after delivery. Precontrast T1 axial MRI (A), postcontrast T1 axial MRI (B), and T2 axial MRI (C) show that the Meckel's cave lesion has vanished and that the cave now appears normal on both sides. 187 Meckel's Cave Arachnoid Cyst J Neuro-Ophthalmol, Vol. 28, No. 3, 2008 two cases (3,6) and no enhancement in five cases (3,4,7-9). Lobulation was described once (9). Similar to previous descriptions, the presumed Meckel's cave arachnoid cyst in our patient had high T2 signal paralleling that of CSF. The only atypical feature in our patient was intermediate (rather than low) T1 signal. In all likelihood, the high T1 signal intensity in our patient derived from averaging of the septae within the lesion with the low T1 signal from CSF (Fig. 1C). The diffusion characteristics of Meckel's cave arach-noid cysts have not been reported previously, although they may be expected to be helpful. Arachnoid cysts, like the lesion shown in our patient, demonstrate a CSF-like signal, a clear distinction from epidermoid cysts, which also arise in this region and which demonstrate a diffusion signal of brain parenchymal intensity (11,12). In our patient, the initial imaging diagnosis was schwannoma or meningioma, although such a high T2 signal would not be consistent with either diagnosis. Lack of familiarity with this lesion, which has been infrequently reported, probably led to the error. Larger lesions have disclosed bone erosion (Fig. 4A), which was found on high-resolution temporal bone CT in all of the 10 patients in whom such a study was performed (3-10). Our patient lacked these findings, perhaps because the lesion was short-lived and relatively small (Fig. 4B). The clinical features of similar cystic lesions arising from Meckel's cave have been adequately documented in 21 cases (Table 1), including 15 women and 6 men with a mean age of 46 years (range 1.5-82 years). Seven of these 21 patients were asymptomatic (3,4,7-9), with brain imaging having been performed for symptoms unrelated to the lesion. Among the 14 symptomatic patients, 10 had manifestations related to cyst mass effect on adjacent structures (1-3,6-10) and 4 had manifestations related to a CSF fistula (3,5,7,13). Cyst mass effect was responsible for binocular diplopia in four patients [1 with third cranial nerve palsy (3), 2 with sixth cranial nerve palsy (1,3), and 1 FIG. 3. Typical MRI characteristics of previously reported bilateral Meck-el's cave arachnoid cysts, called ‘‘petrous apex cephalocoeles'' in this article (4). Precontrast T1 axial (A) and T2 (B) images show cystic lesions arising from Meckel's cave and extending along the petrous apex with low signal on T1 and high signal on T2. FIG. 4. A. Typical CT characteristics of a previously reported Meckel's cave arachnoid cyst (3). The cyst has caused bone erosion (asterisk). B. Our patient's CT performed 3 months after delivery shows normal bone configuration on the side where a Meckel's cave arachnoid cyst had previously been identified (asterisk). 188 q 2008 Lippincott Williams & Wilkins J Neuro-Ophthalmol, Vol. 28, No. 3, 2008 Jacob et al TABLE 1. Clinical features of previously reported Meckel's cave arachnoid cysts Reference and case no. Age (years) Sex Ocular motor manifestation Fifth cranial nerve involvement Effects of CSF fistula Other manifestations Postoperative outcome Moore et al (3) (Case 1) 25 F Sixth cranial nerve palsy Numbness Diplopia improved, but not trigeminal numbness Beck et al (1) (Case 12) 1.5 M Sixth cranial nerve palsy Ipsilateral exophthalmos Normal examination 6 years later Moore et al (3) (Case 3) 48 F Third cranial nerve palsy Present Wo¨rner et al (2) 44 M Transient diplopia Dysesthesia Transient vertigo Lesion recurred 3 months after surgery; asymptomatic 15 months after second surgery. Achilli et al (6) 40 F Pain, dysesthesia, and numbness (V1, V2) Dizziness without vestibular dysfunction Trigeminal pain disappeared almost immediately; total right conductive hearing loss developed; headache and facial paresthesias improved but persisted; no lesion present on MRI 1 year after surgery Moore et al (3) (Case 4) 59 F Pain Jelsma et al (10) 58 F Pain (V1), dysesthesia, and numbness (V1,V3) Trigeminal anesthesia (V3) persisted, but dysesthesia subsided Cheung et al (7) (Case 1) 46 F Pain (V1, V2) Carbamazepine eventually failed to control facial pain preoperatively; postoperatively, pain controlled with low-dose carbamazepine during 6-month follow-up Chang et al (8) (Case 12) 9 M Numbness (V1, V2, V3) Headache Batra et al (9) 55 F Pain (V3), dysesthesia (V3), and numbness Trigeminal dysesthesia resolved after 6 weeks Moore et al (3) (Case 2) 5 M Otorrhea into the middle ear CSF otorrhea resolved Motojima et al (5) 6 F Rhinorrhea and recurrent meningitis Headache, vomiting, and rhinorrhea resolved Hall et al (13) 33 M Otorrhea CSF otorrhea resolved Chang et al (8) (Case 13) 70 F Chronic suppurative otitis media Moore et al (3) (Case 5) 45 F Moore et al (3) (Case 6) 82 F Moore et al (3) (Case 7) 46 F Moore et al (3) (Case 8) 72 F Moore et al (3) (Case 9) 66 F Moore et al (3) (Case 10) 36 M Srinivasan et al (4) 65 F CSF, cerebrospinal fluid; M, male, F, female. 189 Meckel's Cave Arachnoid Cyst J Neuro-Ophthalmol, Vol. 28, No. 3, 2008 with transient diplopia without any further details (2)], fifth cranial nerve dysfunction in 9 patients (2,3,6-10), exophthalmos in 1 patient (1), and vertigo in 2 patients (2,6)). The lesion triggered a CSF fistula in four patients (3,5,7,13) when a tear occurred in the cyst wall, allowing CSF to leak into the petrous apex. Because the aerated petrous bone communicates with the middle ear, CSF otorrhea (2 patients) (3,13) or rhinorrhea (1 patient) (5) resulted. CSF fistula was also responsible for recurrent meningitis (1 patient) (5) and chronic otitis media (1 patient) (8). Five patients had headache (3,8), but whether it was caused by that particular lesion is uncertain. Surgery was performed on all symptomatic patients (except 2, for whom treatment was not described (3,8) and on none of the asymptomatic patients. The surgical procedure was designed to collapse the cyst or to cure the CSF fistula or both. Diplopia improved after surgery in 1 patient (3) (Table 1) and had disappeared in 2 patients after 15 months (2) and after 6 years in another patient (1). For the remaining patient with diplopia, the outcome was not given (3). When the fifth cranial nerve was involved, the pain seemed to resolve postoperatively more often than the numbness (3,6,7,9,10). When described, the pain disappeared shortly after surgery. CSF fistulas finally resolved in all patients for whom an outcome was reported (3,5,13). In none of the seven asymptomatic patients was a follow-up examination reported, so the natural course of the lesion remains unknown. To our knowledge, ours is the first reported instance of the spontaneous resolution of a symptomatic Meckel's cave arachnoid cyst. Frequently found on imaging as an incidental finding, arachnoid cysts at any intracranial location may require surgical treatment when they enlarge and become symp-tomatic. On the basis of endoscopic observation of a supra-sellar prepontine arachnoid cyst (14,15), a ball-valve mechanism is suspected to be the basis of enlargement. An alternative hypothesis is that cells lining the cyst wall continuously secrete fluid, which is then trapped (16). Spontaneous disappearance of arachnoid cysts, as occurred in our patient, is rare in adults, with only one reported case in a 21-year-old patient (17). There are 13 reported cases in patients aged 16 years or younger (18-30). A provocative factor such as head trauma (20,29), meningitis (28), the Valsalva maneuver (31), coughing, sneezing, crying, or sporting activities (24,26,27,32) has sometimes been identified. Arachnoid cysts may pro-gressively shrink without provocation or symptoms, a phenomenon observed in 9 patients (17-25) in whom the putative explanation is formation of a communication between the cyst and the subarachnoid space, allowing the cyst to drain through the normal CSF pathways. Whether there is direct transport through the cyst wall or whether CSF is released through a ball-valve mechanism is uncertain (24). An alternative explanation for cyst disappearance, described in 5 patients (26-30), is sudden rupture into the subdural space, allowing fluid to spread and subsequently be reabsorbed. A subdural hematoma may sometimes initially accompany the subdural hygroma. In such cases, a tear in the cyst outer wall establishes a communication between the cyst and the subdural space (24,26,29). Supporting this hypothesis is the observation during craniotomy that a Valsalva maneuver caused a tear in the outer cyst wall (31). In our patient, the spontaneous resolution of the lesion occurred without any visible subdural effusion, even though the small size of the initial arachnoid cyst would have made it difficult to observe. The clinical improvement was concomitant with both the delivery and the lesion disappearance on MRI, suggest-ing the possibility that increased intra-abdominal or thoracic pressure during delivery may have been a triggering factor. The discovery of a Meckel's cave arachnoid cyst during pregnancy based on new symptoms raises the question of growth induced by the pregnancy itself (33-36). Three cases of intracranial arachnoid cyst have reportedly been diagnosed during pregnancy or the peri-partum period because they had become symptomatic during those periods (33,34,36). The 2 patients who had become symptomatic during pregnancy (right hand tremor associated with headache in one and seizure in the other) underwent cesarean sections under general anesthesia to prevent the pushing efforts in delivery and to avoid increases in intracranial pressure by injection of anesthetic drugs into the epidural spaces (33,34). In the third case (36), the mother had a seizure 9 hours after delivering twins, and brain CT revealed a large medial fossa arachnoid cyst without any sign of rupture or hemorrhage into the subdural space. A fourth patient (35), known before pregnancy to have a posterior fossa arachnoid cyst, underwent cesarean section under epidural anesthesia and showed no change in cyst appear-ance in the peripartum period. An immunocytochemical study has shown progesterone receptors in the nuclei of cells lining the arachnoid cyst, suggesting an inhibitory influence of progestins on CSF absorption and evoking a similarity with hormone-dependent growth of meningiomas (37). We found no reported cases of Meckel's cave arachnoid cysts discovered during pregnancy. This case report describes a Meckel's cave arachnoid cyst responsible for a sixth cranial nerve palsy during pregnancy and which spontaneously resolved after delivery. Because all of the previously described symptomatic patients had been treated surgically, this is the first reported instance of spontaneous resolution of both clinical and imaging findings. The imaging characteristics may vary 190 q 2008 Lippincott Williams & Wilkins J Neuro-Ophthalmol, Vol. 28, No. 3, 2008 Jacob et al more than previously thought, including an intermediate signal on T1 and the absence of bone erosion in the petrous apex on CT. Pregnancy may have had a role in increasing the cyst size, and the pushing effort during labor may have triggered cyst rupture. Given the experience with this patient, arachnoid cysts should not be surgically treated during pregnancy unless they produce life-threatening manifestations. REFERENCES 1. Beck DW, Menezes AH. Lesions in Meckel's cave: variable presentation and pathology. J Neurosurg 1987;67:684-9. 2. Wo¨ rner BA, Noll M, Rahim T, et al. Recurrent arachnoid cyst of Meckel's cave mimicking a brain stem ischaemia. Report of a rare case. Zentralbl Neurochir 2003;64:76-9. 3. Moore KR, Fischbein NJ, Harnsberger HR, et al. Petrous apex cephaloceles. AJNR Am J Neuroradiol 2001;22:1867-71. 4. Srinivasan A, Ibrahim M, Mukherji SK. Radiology quiz case 2: bilateral petrous apex cephaloceles (PACs). Arch Otolaryngol Head Neck Surg 2006;132:1265-7. 5. Motojima T, Fujii K, Ishiwada N, et al. Recurrent meningitis associ-ated with a petrous apex cephalocele. J Child Neurol 2005;20:168-70. 6. Achilli V, Danesi G, Caverni L, et al. Petrous apex arachnoid cyst: a case report and review of the literature. Acta Otorhinolaryngol Ital 2005;25:296-300. 7. Cheung SW, Broberg TG, Jackler RK. Petrous apex arachnoid cyst: radiographic confusion with primary cholesteatoma. Am J Otol 1995; 16:690-4. 8. Chang P, Fagan PA, Atlas MD, et al. Imaging destructive lesions of the petrous apex. Laryngoscope 1998;108:599-604. 9. Batra A, Tripathi RP, Singh AK, et al. Petrous apex arachnoid cyst extending into Meckel's cave. Australas Radiol 2002;46:295-8. 10. Jelsma F, Ross PJ. Traumatic intracranial arachnoid cyst involving the Gasserian ganglion: case report. J Neurosurg 1967;26:439-41. 11. Tsuruda JS, Chew WM, Moseley ME, et al. Diffusion-weighted MR imaging of the brain: value of differentiating between extraaxial cysts and epidermoid tumors. AJNR Am J Neuroradiol 1990;11:925-34. 12. Hakyemez B, Aksoy U, Yildiz H, et al. Intracranial epidermoid cysts: diffusion-weighted, FLAIR and conventional MR findings. Eur J Radiol 2005;54:214-20. 13. Hall GM, Hallberg OE. Persistent cerebrospinal fluid otorrhea. Arch Otolaryngol 1967;86:377-81. 14. Schroeder HW, Gaab MR. Endoscopic observation of a slit-valve mechanism in a suprasellar prepontine arachnoid cyst: case report. Neurosurgery 1997;40:198-200. 15. Santamarta D, Aguas J, Ferrer E. The natural history of arachnoid cysts: endoscopic and cine-mode MRI evidence of a slit-valve mechanism. Minim Invasive Neurosurg 1995;38:133-7. 16. Krawchenko J, Collins GH. Pathology of an arachnoid cyst: case report. J Neurosurg 1979;50:224-8. 17. Wester K, Gilhus NE, Hugdahl K, et al. Spontaneous disappearance of an arachnoid cyst in the middle intracranial fossa. Neurology 1991; 41:1524-6. 18. Przybylo HJ, Radkowski MA, Przybylo J, et al. Spontaneous resolution of an asymptomatic arachnoid cyst. Pediatr Neurosurg 1997;26:312-4. 19. Takagi K, Sasaki T, Basugi N. Spontaneous disappearance of cerebellopontine angle arachnoid cyst: report of a case (in Japanese). No Shinkei Geka 1987;15:295-9. 20. Takizawa H, Sugiura K, Kudo C, et al. Spontaneous disappearance of a middle fossa arachnoid cyst-a case report (in Japanese). No To Shinkei 1991;43:987-9. 21. McDonald PJ, Rutka JT. Middle cranial fossa arachnoid cysts that come and go: report of two cases and review of the literature. Pediatr Neurosurg 1997;26:48-52. 22. Beltramello A, Mazza C. Spontaneous disappearance of a large middle fossa arachnoid cyst. Surg Neurol 1985;24:181-3. 23. Pandey P, Tripathi M, Chandra PS, et al. Spontaneous decompression of a posterior fossa arachnoid cyst: a case report. Pediatr Neurosurg 2001;35:162-3. 24. Moon KS, Lee JK, Kim JH, et al. Spontaneous disappearance of a suprasellar arachnoid cyst: case report and review of the literature. Childs Nerv Syst 2007;23:99-104. 25. Yamauchi T, Saeki N, Yamaura A. Spontaneous disappearance of temporo-frontal arachnoid cyst in a child. Acta Neurochir (Wien) 1999;141:537-40. 26. Mori T, Fujimoto M, Sakae K, et al. Disappearance of arachnoid cysts after head injury. Neurosurgery 1995;36:938-42. 27. Inoue T, Matsushima T, Tashima S, et al. Spontaneous disappearance of a middle fossa arachnoid cyst associated with subdural hematoma. Surg Neurol 1987;28:447-50. 28. Yoshioka H, Kurisu K, Arita K, et al. Spontaneous disappearance of a middle cranial fossa arachnoid cyst after suppurative meningitis. Surg Neurol 1998;50:487-91. 29. Yamanouchi Y, Someda K, Oka N. Spontaneous disappearance of middle fossa arachnoid cyst after head injury. Childs Nerv Syst 1986; 2:40-3. 30. Rakier A, Feinsod M. Gradual resolution of an arachnoid cyst after spontaneous rupture into the subdural space: case report. J Neurosurg 1995;83:1085-6. 31. Cullis PA, Gilroy J. Arachnoid cyst with rupture into the subdural space. J Neurol Neurosurg Psychiatry 1983;46:454-6. 32. Cokluk C, Senel A, Celik F, et al. Spontaneous disappearance of two asymptomatic arachnoid cysts in two different locations. Minim Invasive Neurosurg 2003;46:110-2. 33. Buitron Garcia R, Juarez Azpilcueta A, Bravo Gutierrez R, et al. Arachnoid cyst and pregnancy: report of a case (in Spanish). Ginecol Obstet Mex 2003;71:476-9. 34. Ruprai CK, Pring DW, Vipond A, et al. Pregnancy complicated by a large intracranial arachnoid cyst: multidisciplinary approach to safe delivery. J Obstet Gynaecol 2007;27:83-5. 35. Rupasinghe MM, McLoughlin L, Singaraju V. Intracranial arachnoid cyst: anaesthetic management in pregnancy. Int J Obstet Anesth 2007;16:265-8. 36. McCormick RN, Stutley JE, Green RJ. An unusual cause of postpartum collapse or a red herring? Anaesthesia 2003;58: 398-9. 37. Go KG, Blankenstein MA, Vroom TM, et al. Progesterone receptors in arachnoid cysts: an immunocytochemical study in 2 cases. Acta Neurochir (Wien) 1997;139:349-54. 191 Meckel's Cave Arachnoid Cyst J Neuro-Ophthalmol, Vol. 28, No. 3, 2008 |