| Title |
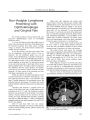
Successful Treatment of Invasive Cavernous Sinus Aspergillosis with Oral Intraconazole Monotherapy |
| Creator |
Browning, AC; Sim, KT; Timms, JM; Vernon, SA; McConachie, NS; Allibone, R; Jones, NS |
| Affiliation |
Department of Ophthalmology, University Hospital, Queen's Medical Centre, Nottingham, United Kingdom. |
| Abstract |
An 83-year-old woman receiving long-term prednisolone treatment presented with a right optic neuropathy and right third, fourth, fifth, and sixth cranial nerve palsies secondary to sino-orbital aspergillosis with cavernous sinus involvement. Because the patient refused conventional treatment, she was given a two-year course of oral itraconazole 200 mg/day, leading to a complete imaging resolution of the lesion. Three years after completing treatment, there is no clinical or imaging evidence of disease recurrence. Visual and ocular motor function did not recover, but ptosis and proptosis improved. We believe this to be the first documented case of successful treatment of such a lesion with oral itraconazole monotherapy. |
| Subject |
Administration, Oral; Older people, 80 and over; Antifungal Agents, administration & dosage; Aspergillosis, diagnosis; Aspergillosis, drug therapy; Aspergillosis, microbiology; Aspergillus, genetics; Aspergillus, isolation & purification; Biopsy; Cavernous Sinus, microbiology; DNA, Fungal, analysis; Diagnosis, Differential; Female; Follow-Up Studies; Humans; Itraconazole, administration & dosage; Magnetic Resonance Imaging |
| Format |
application/pdf |
| Publication Type |
Journal Article |
| Collection |
Neuro-Ophthalmology Virtual Education Library: Journal of Neuro-Ophthalmology Archives: https://novel.utah.edu/jno/ |
| Publisher |
Lippincott, Williams & Wilkins |
| Holding Institution |
Spencer S. Eccles Health Sciences Library, University of Utah |
| Rights Management |
© North American Neuro-Ophthalmology Society |
| Setname |
ehsl_novel_jno |
| ID |
225565 |
| Reference URL |
https://collections.lib.utah.edu/ark:/87278/s6hh9r4n/225565 |