| OCR Text |
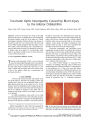
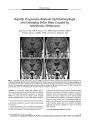
Show ORIGINAL CONTRIBUTION Ischemic Optic Neuropathy Following Spine Surgery in a 16- Year- Old Patient and a Ten- Year- Old Patient Jonathan W. Kim, MD, William L. Hills, MD, Joseph E Rizzo, MD, Robert A. Egan, MD, and Simmons Lessell, MD Abstract: Peri- operative ischemic optic neuropathy typically occurs in middle- aged or older patients. We report this condition in two patients aged 16 and 10 years. Only six other cases of peri- operative ischemic optic neuropathy have been reported in patients aged less than 30 years, all but one occurring after spinal surgery. Although the visual prognosis appears to be more favorable in younger patients, the pathogenesis of this rare complication of surgery is likely to be the same as that affecting older individuals. ( J Neuro- Ophthalmol 2006; 26: 30- 33) Peri- operative ischemic optic neuropathy is characterized by unilateral or bilateral visual loss following major surgical procedures such as spinal surgery, coronary artery bypass, radical neck dissection, and others ( 1- 8). While the pathogenesis has yet to be confidently explained, surgery- related anemia and hypotension have been postulated as possible mechanisms ( 1- 6). This potentially devastating complication typically occurs in middle- aged or older patients ( 2,3,9- 11). It is rare for patients under the age of 30 to develop it. We report two cases occurring in young patients undergoing spinal surgery. METHODS A literature search of the National Library of Medicine's PubMed database was performed with the following words and word combinations: ischemic optic Department of Neuro- Ophthalmology ( JWK, JFR, SL), Massachusetts Eye and Ear Infirmary and the Department of Ophthalmology, Harvard Medical School, Boston, Massachusetts; Department of Neuro- Ophthalmology ( WLH, RAE), Casey Eye Institute, Oregon Health & Science University, Portland, Oregon; Department of Ophthalmology ( JWK), University of California, Irvine, Irvine, California. Address correspondence to Simmons Lessell, MD, 243 Charles Street, Boston, MA, 02114; E- mail: simmons_ lessell@ meei. harvard. edu neuropathy, posterior ischemic optic neuropathy, postoperative visual loss, and postoperative blindness. CASE REPORTS Case 1 A 16- year- old girl with neuro- muscular scoliosis, dystonia, and athetosis underwent spinal fusion surgery. The patient's medical history was otherwise unremarkable and her past ocular history was notable only for moderate hyperopia. Arthrodesis from Tl to the sacrum was performed in the prone position with neck flexion. A molded face mask was used to avoid pressure on the globes. Her preoperative hemoglobin was 14.4 gm/ dl and hematocrit was 41.5%. Systolic blood pressure was 140/ 70 mm Hg immediately prior to the induction of anesthesia. There were no intra- operative or postoperative complications. The estimated blood loss was 4,000 mL and total duration of anesthesia was 13 hours. Intra- operative fluid replacement included 11 units of cell saver, three units of bank blood, six units of fresh frozen plasma, four units of platelets, 9 L of lactated Ringer's solution, and 2 L of normal saline. During surgery her systolic blood pressure ranged from 80- 100 mm Hg systolic. The diastolic blood pressure ranged from 40- 60 mm Hg except for brief periods when it was between 30- 40 mm Hg. The first day after surgery, she was transfused with two units of packed red cells to maintain her hematocrit, which was 17.5% ( hemoglobin 6.2 gm/ dl). On the third postoperative day, she complained of blurred vision in both eyes. She was alert and cooperative but had to be examined supine in her hospital bed. Visual acuity was hand movements OD and 20/ 200 OS. She could not identify any Ishihara color plates. On confrontation visual field testing, only the left superior visual field in the left eye appeared intact. There was a right relative afferent pupil defect. There were bilateral periocular edema and 30 J Neuro- Ophthalmol, Vol. 26, No. 1, 2006 Copyright © Lippincott Williams & Wilkins. Unauthorized reproduction of this article is prohibited. Postoperative AION in Young Patients J Neuro- Ophthalmol, Vol. 26, No. 1, 2006 small ecchymoses in her right upper eyelid. Ocular motility examination revealed normal versions and alignment and no nystagmus. Dilated fundus examination showed pallid edema of both optic discs. Apart from visual loss, there were no other neurologic deficits. Blood pressure was 95/ 50 mm Hg, hematocrit 24.4%, and hemoglobin 8.7 g/ dl. She was transfused for the second time with two units of packed red cells and hematocrit increased to 34% the following day. A brain CT scan showed no abnormalities. Over the ensuing weeks, she noted gradual visual improvement. Two weeks after surgery, visual acuities were finger counting OD and 20/ 30 OS. The right relative afferent pupillary defect was still evident. Both optic discs were pale but less edematous. Nine months after surgery, visual acuities were 5/ 200 OD and 20/ 25 OS. She could not be positioned for perimetry, but confrontation visual field testing showed extensive central and nasal depression in the right eye and depression of the lower field in the left eye. Ophthalmoscopic examination showed bilaterally pale optic discs without edema ( Fig. 1). Case 2 A ten- year- old boy with a low thoracic meningomyelocele and severe lumbosacral kyphosis underwent a posterior release and instrumentation. His medical history was otherwise unremarkable and his past ocular history was significant for alternating esotropia and moderate hyperopia. Kyphectomy was performed in the prone position with the face resting in a doughnut. Preoperative hemoglobin was 13.9 g/ dL and hematocrit was 40.5%. Preoperative blood pressure immediately prior to induction of anesthesia was 130/ 80 mm Hg. Estimated blood loss was 3600 cc during a total of 11.5 hours of anesthesia. Infra- operative fluid replacement included 920 mL via the cell saver, four units of packed red blood cells, two units of fresh frozen plasma, 4 L lactated Ringer's solution, 5 L normal saline, and five units of cryoprecipitate. Five units of platelets were given postoperatively in the pediatric intensive care unit. During surgery the lowest blood pressure was 70/ 35, which persisted for one hour. Lowest infra- operative hemoglobin was 7.5 g/ dL and lowest hematocrit was 21.8%. Postoperatively, he received one unit of packed red cells, raising his hemoglobin to 9.6 g/ dL and hematocrit to 27.4%. However, the following morning his hemoglobin fell to 7.3 g/ dL and hematocrit to 21.1%. On the second postoperative day, his face was markedly swollen and his parents noted that he did not see normally. He confabulated during visual acuity testing and did not appear to perceive light. His pupils were non- reactive. Dilated fundus examination demonstrated normal- appearing optic discs. Ten months later, visual acuity had improved to 20/ 200 in the left eye, but still no light perception ( NLP) in the right eye. He demonstrated a right relative afferent pupillary defect. Both optic discs were pale. DISCUSSION Our two cases are presented because peri- operative ischemic optic neuropathy is so unusual in young patients. We identified only six other cases in patients aged 30 years or younger ( Table 1) ( 2,5,11- 14). Although the sample size is small, we recognize similarities between younger and older patient groups with this condition. Spinal surgery appears to be the most common setting for patients of all ages ( 2,9,10,14). Including our cases, seven of the eight reported cases in patients under age 30 occurred after spinal surgery. The only exception was a 16- year- old girl with chronic renal failure and anemia FIG. 1. Case 1. Fundus photographs taken with a hand- held camera nine months after spine surgery in a 16- year- old patient. They show bilateral optic disc pallor, left greater than right. Visual acuities were 5/ 200 OD and 20/ 25 OS. 31 Copyright © Lippincott Williams & Wilkins. Unauthorized reproduction of this article is prohibited. J Neuro- Ophthalmol, Vol. 26, No. 1, 2006 Kim et al TABLE 1. Reported cases of peri- operative ischemic optic neuropathy in patients aged thirty years or less Case no. ( ref. no) Age ( years) Sex ( M/ F) Surgery type Surgery duration ( hours) Blood loss ( liters) Lowest operative blood pressure Lowest hematocrit % or hemoglobin g/ dL ( hours after surgery) 1( 13) 2( 2) 3( 11) 4( 12) 5( 5) 6( 14) 7 ( our 8 ( our Case Case 1) 2) 24 27 12 13 16 19 16 10 M F M M F M F M Spinal Spinal Spinal Spinal Parathyroid Spinal Spinal Spinal > 5 9 6 7 7 7 13 11.5 7 5.0 2.5 8.0 7 2.7 4.0 3.6 80/ 55 7 80/ 50 52 ( mean) 100/ 45 7 80/ 30 70/ 35 24% ( intra- operative) 36% (?) 26% ( intra- operative) 7.1 g/ dL ( intra- operative) 7- 8.0 g/ dL ( intra- operative) 29.9% (?) 18%, 8.7 g/ dL ( 24) 21.1%, 7.3 g/ dL ( 24) Continued who was noted to have optic disc pallor following total parathyroidectomy ( 5). As in the older patients, most of the younger patients had normal optic discs in the immediate postoperative period with disc pallor developing during the first year of follow- up. Younger patients appear to have a better visual prognosis than do older patients. In the series of Sadda et al ( 9) of 28 adult patients, 44% of eyes had a final visual acuity of hand motions or worse. The recent review of Buono and Foroozan ( 15) of all 83 peri- operative ischemic optic neuropathy cases reported before 2004 showed that 55% of eyes had a final visual acuity of hand motions or worse. In our study of young patients, only two ( 17%) out of 12 eyes had hand movement perception or worse visual acuity ( when measured); five ( 42%) out of 12 eyes had a final visual acuity of 20/ 30 or better. None of the young patients were identified to have vasculopathic risk factors such as hypertension, diabetes, hypercholesteremia, obesity, or a history of smoking. Why should peri- operative ischemic optic neuropathy be less apt to afflict younger patients? Part of the explanation could be that the procedures frequently implicated in peri- operative optic neuropathies are not performed as frequently in younger groups. In the review of Shapira et al ( 3), of 602 patients who underwent open heart operations at the Lahey Clinic, the youngest patient to develop peri- operative ischemic optic neuropathy was 54 years old. However, complex spinal surgeries, the procedure most often associated with this complication, are commonly performed in young people ( 16,17). Therefore, a more satisfactory explanation is that the optic nerve in young individuals is better able to withstand the ischemic insult that results from intra- operative hypotension and blood loss. Some authors have found an association between peri- operative ischemic optic neuropathy and vasculopathic and arteriosclerotic risk factors ( 1,4). Because the commonly identified risk factors ( chronic hypertension, smoking, diabetes mellitus, and systemic atherosclerosis) are much less prevalent in the young, this disparity may be a contributing factor. For all demographic groups, spinal surgery is the most common setting. In the series of Sadda et al ( 6), 50% of patients had undergone spinal surgery. The incidence of peri- operative ischemic optic neuropathy following spinal surgery has been estimated to be as high as 0.2% ( 2,10,13). By comparison, the largest series of cardiac bypass patients with peri- operative ischemic optic neuropathy identified by a retrospective study showed an incidence of 0.06% during an 18- year period ( 3). The risk of peri- operative ischemic optic neuropathy is reported at 1: 61,000 in a general surgery population ( 18). There are special features of spine surgery that may predispose to this complication, including long operative times, substantial intra- operative blood loss, and deliberate hypotensive anesthesia. Prone patient positioning has also been implicated as a causative factor. Direct pressure on the globe from a badly- positioned headrest has also been cited as a factor contributing to visual loss in several published reports, although other authors have contended that direct ocular pressure would be expected to cause central retinal artery or venous occlusion rather than ischemic optic neuropathy ( 19- 21). It is common for patients undergoing prolonged posterior fusions or multi- level laminectomies to develop postoperative facial and periocular edema, which may indirectly elevate orbital venous pressure. Our first case did have periocular edema and unilateral eyelid ecchymosis. A combination of local and systemic perturbations during spinal surgery may predispose the optic nerve to ischemic insult even in young individuals without vascular disease. Although the visual prognosis appears to be more favorable in younger patients, the pathogenesis of 32 © 2006 Lippincott Williams & Wilkins Copyright © Lippincott Williams & Wilkins. Unauthorized reproduction of this article is prohibited. Postoperative AION in Young Patients J Neuro- Ophthalmol, Vol. 26, No. 1, 2006 TABLE 1 ( Continued). Reported cases of peri- operative ischemic optic neuropathy in patients aged thirty years or less Disc edema ( yes/ no) N N N N 7 7 Y N Unilateral/ bilateral ( U/ B) U U B B B B B B Initial postoperative visual acuity ( hours after surgery) 20/ 80 (< 24 h) 20/ 20 ( 48 h) ? (< 24 h) 20/ 30, 20/ 400 ( 24 h) ? ( 72 h) 7 Hand movements, 20/ 200 ( 72 h) No light perception, OU ( 48 h) Final visual acuity ( months) 20/ 80 ( 60 m) 20/ 20 (?) Hand movements, 16/ 200 ( 12 m) 20/ 20, 20/ 60 ( 48 m) 20/ 30,20/ 15 ( 18 m) 7 5/ 200, 20/ 25 ( 9 m) No light perception, 20/ 200 ( 10 m) peri- operative ischemic optic neuropathy is likely to be similar to that of older patients. REFERENCES Katz DM, Trobe JD, Cornblath WT, Kline LB. Ischemic optic neuropathy after lumbar spine surgery. Arch Ophthalmol 1994; 112: 925- 31. Stevens WR, Glazer PA, Kelley SD, et al. Ophthalmic complications after spinal surgery. Spine 1997; 22: 1319- 24. Shapira OM, Kimmel WA, Lindsey PS, Shahian DM. Anterior ischemic optic neuropathy after open heart operations. Ann Thorac Surg 1996; 61: 660- 6. Nuttall GA, Garrity JA, Dearani JA, et al. Risk factors for ischemic optic neuropathy after cardiopulmonary bypass: a matched case/ control study. Anesth Analg 2001; 93: 1410- 6. Jaben SL, Glaser JS, Daily M. Ischemic optic neuropathy following general surgical procedures. J Clin Neuroophthalmol 1983; 3: 239^ 4. Rizzo JF, 3rd Lessell S. Posterior ischemic optic neuropathy during general surgery. Am J Ophthalmol 1987; 103: 808- 11. Schobel GA, Schmidbauer M, Millesi W, Undt G Posterior ischemic optic neuropathy following bilateral radical neck dissection. Int J Oral Maxillofac Surg 1995; 24: 283- 7. Luscavage LE, Volpe NJ, Liss R. Posterior ischemic optic neuropathy after uncomplicated cataract extraction. Am J Ophthalmol 2001; 132: 408- 9. Sadda SR, Nee M, Miller NR, et al. Clinical spectrum of posterior ischemic optic neuropathy. Am J Ophthalmol 2001; 132: 743- 50. 10. Myers MA, Hamilton SR, Bogosian AJ, et al. Visual loss as a complication of spine surgery. A review of 37 cases. Spine 1997; 22: 1325- 9. 11. Dunker S, Hsu HY, Sebag J, Sadun AA. Peri- operative risk factors for posterior ischemic optic neuropathy. J Am Coll Surg 2002; 194: 705- 10. 12. Brown RH, Schauble JF, Miller NR. Anemia and hypotension as contributors to perioperative loss of vision. Anesthesiology 1994; 80: 222- 6. 13. Roth S, Nunez R, Schreider BD. Unexplained visual loss after lumbar spinal fusion. JNeurosurg Anesthes 1997; 9: 346- 8. 14. Cheng MA, Sigurdson W, Tempelhoff R, Lauryssen C. Visual loss after spine surgery. Neurosurgery 2000; 46: 625- 31. 15. Buono LM, Foroozan R. Peri- operative posterior ischemic optic neuropathy: review of the literature. Surv Ophthalmol 2005; 50: 15- 26. 16. Brown JC, Zeller JL, Swank SM, et al. Surgical and functional results of spine fusion in spinal muscular dystrophy. Spine 1989; 14: 763- 70. 17. Bridwell KH. Surgical treatment of idiopathic adolescent scoliosis. Spine 1999; 24: 2607- 16. 18. Roth S, Thisted RA, Erickson JP, et al. Eye injuries after nonocular surgery. A study of 60,965 anesthetics from 1988 to 1992. Anesthesiology 1996; 85: 1020- 7. 19. Hollenhorst RW, Svien HJ, Benoit CF. Unilateral blindness occurring during anesthesia for neurosurgical operations. Arch Ophthalmol 1954; 52: 819- 30. 20. Walkup HE, Murphy JD. Retinal ischemia with unilateral blindness: a complication occurring during pulmonary resection in the prone position. J Thorac Cardiovasc Surg 1952; 23: 174- 5. 21. Locastro A, Novak KD, Biglan AW. Central retinal artery occlusion in child after general anesthesia. Am J Ophthalmol 1991; 112: 91- 2. 33 Copyright © Lippincott Williams & Wilkins. Unauthorized reproduction of this article is prohibited. |