| Title |
Subretinal Hemorrhage from a Peripapillary Choroidal Neovascular Membrane in Papilledema Caused by Idiopathic Intracranial Hypertension |
| Creator |
Sathornsumetee, B; Webb, A; Hill, DL; Newman, NJ; Biousse, V |
| Affiliation |
Department of Ophthalmology, and Neurological Surgery (NJN), Emory University, Atlanta, Georgia, USA. |
| Abstract |
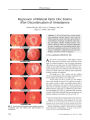
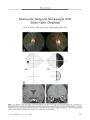
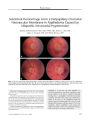
A 42-year-old man with idiopathic intracranial hypertension and chronic papilledema had severe visual loss in his left eye caused by subretinal bleeding from a peripapillary choroidal neovascular membrane (CNVM). After optic nerve sheath fenestration in his left eye, the papilledema improved, allowing improved visualization of the CNVM. Visual function did not improve after the surgery. CNVM can complicate chronic papilledema and account for sudden worsening of vision. The appropriate management of this type of CNVM is unresolved. |
| Subject |
Adult; Fluorescein Angiography, methods; Humans; Male; Papilledema, etiology; Pseudotumor Cerebri, complications; Retinal Hemorrhage, etiology; Retinal Hemorrhage, pathology; Retinal Neovascularization, etiology; Retinal Neovascularization, pathology |
| Format |
application/pdf |
| Publication Type |
Journal Article |
| Collection |
Neuro-Ophthalmology Virtual Education Library: Journal of Neuro-Ophthalmology Archives: https://novel.utah.edu/jno/ |
| Publisher |
Lippincott, Williams & Wilkins |
| Holding Institution |
Spencer S. Eccles Health Sciences Library, University of Utah |
| Rights Management |
© North American Neuro-Ophthalmology Society |
| Setname |
ehsl_novel_jno |
| ID |
225530 |
| Reference URL |
https://collections.lib.utah.edu/ark:/87278/s6s217mp/225530 |