| Title |
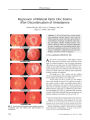
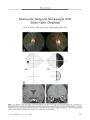
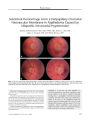
A Case of Bilateral Simultaneous Sixth Cranial Nerve Palsies Secondary to Diabetes Mellitus |
| Creator |
Bayrak, AO; Tilki, HE; Kasm, D |
| Affiliation |
Department of Neurology, Ondokuz Mayis University, Samsun, Turkey. oytun.batrak@gmail.com |
| Abstract |
Ocular motor cranial nerve palsy secondary to diabetes mellitus usually affects one cranial nerve at a time. We report a patient with simultaneous bilateral sixth nerve palsies attributed to diabetes. Although an extremely rare cause of this phenomenon, diabetes may be the explanation after other causes have been excluded. |
| Subject |
Abducens Nerve Diseases, etiology; Abducens Nerve Diseases, pathology; Older people; Diabetes Complications, complications; Diabetes Complications, pathology; Functional Laterality; Humans; Male |
| Format |
application/pdf |
| Publication Type |
Journal Article |
| Collection |
Neuro-Ophthalmology Virtual Education Library: Journal of Neuro-Ophthalmology Archives: https://novel.utah.edu/jno/ |
| Publisher |
Lippincott, Williams & Wilkins |
| Holding Institution |
Spencer S. Eccles Health Sciences Library, University of Utah |
| Rights Management |
© North American Neuro-Ophthalmology Society |
| Setname |
ehsl_novel_jno |
| ID |
225523 |
| Reference URL |
https://collections.lib.utah.edu/ark:/87278/s6s217mp/225523 |