| OCR Text |
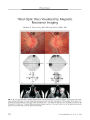
Show ORIGINAL CONTRIBUTION Primary Aberrant Regeneration and Neuromyotonia of the Third Cranial Nerve Kwang- Dong Choi, MD, Jung- Min Hwang, MD, Seong- Ho Park, MD, and Ji Soo Kim, MD Abstract: A 52- year- old woman presented with episodic diplopia with a duration of 6 months. Between the episodes, infraduction of the right eye was mildly impaired with retraction of the right upper lid on downgaze. On resuming the primary position after prolonged left gaze, she developed a right esotropia and reduced abduction, supraduction, and infraduction of the right eye. There was no history of cranial radiation or previous diagnosis of a brain lesion. Brain imaging results were negative. The in-terictal infraduction deficit and lid retraction were interpreted as signs of a mild right third cranial nerve palsy with primary aberrant regeneration. The episodic esotropia and ductional deficits were considered to be signs of neuromyotonia. This combination of findings, rarely described before, suggests a link between primary aberrant regeneration and neuromyotonia. Abnormal and excessive conduction triggered by stimulation of a partially damaged nerve probably underlies ocular neuromyotonia. (/ Neuro- Ophthalmol 2006; 26: 248- 250) Ocular neuromyotonia is a rare disorder characterized by episodic diplopia occurring either spontaneously or after a sustained eccentric gaze ( 1). It may be idiopathic, but some patients have had compressive or inflammatory lesions and others have had radiation to the parasellar and sellar regions months to years earlier ( 1,2). Abnormal electromyographic activity of the extraocular muscles suggests that this phenomenon may result from spontaneous Departments of Neurology ( KDC, SHP, JSK) and Ophthalmology ( JMH), College of Medicine, Seoul National University, Seoul, Korea; and Department of Neurology ( KDC), Pusan National University Hospital, Pusan National University School of Medicine and Medical Research Institute, Pusan, Korea. This work was supported by Korea Research Foundation Grant ( KRF- 2004- 003- E00202). Address correspondence to Ji Soo Kim, MD, Department of Neurology, Seoul National University Bundang Hospital, 300 Gumi- dong, Bundang- gu, Seongnam- si, Gyeonggi- do, 463- 707, Korea; E- mail: jisookim@ snu. ac. kr discharges of the ocular motor nerve axons with unstable cell membranes ( 3). There are reports of patients with aberrant regeneration as an isolated or main sign between the spells of ocular neuromyotonia ( 4- 6). However, the association of aberrant regeneration and neuromyotonia has received little attention. There are no reports of isolated infraduction deficit and lid retraction on downgaze between episodes of neuromyotonia. We describe a 52- year- old woman who had signs of aberrant regeneration of the third cranial nerve with superimposed episodes of ocular neuromyotonia. CASE REPORT A 52- year- old woman was referred for evaluation of intermittent diplopia that had been present for 6 months. The diplopia was mixed horizontal and vertical and often was associated with an inward pulling sensation of the right eye. The diplopia lasted for 3- 4 minutes and resolved after prolonged right gaze or repeated voluntary blinking. She denied having accompanying oscillopsia or headache. She had no history of migraine, cranial radiation, or other medical illnesses. The general medical and neurologic examinations were normal. Visual acuity, visual fields, pupils, and fundi were normal. Between the episodes, she was orthotropic without ptosis or lid retraction in the primary position. However, infraduction of the right eye was mildly impaired, and right upper lid retraction was noted on downgaze ( Fig. 1). There was no widening of the palpebral fissure with adduction of the right eye or pupillary changes with adduction or infraduction of the right eye. On resuming the primary position after prolonged left gaze, she developed 18 prism-diopters of right esotropia and reduced abduction, supraduction, and infraduction of the right eye ( Fig. 2). Sustained right gaze or upgaze did not induce this phenomenon. The esotropia and reduced ductions were eliminated by attempted right gaze. Results of routine chemical analyses and thyroid function tests were normal. Review of the outside MRI showed no abnormalities, especially in the midbrain. The patient reported markedly reduced episodes after taking 200 mg carbamazepine twice a day. In addition, the 248 J Neuro- Ophthalmol, Vol. 26, No. 4, 2006 Primary Aberrant Regeneration and Neuromyotonia J Neuro- Ophthalmol, Vol. 26, No. 4, 2006 FIG. 1. Extraocular movements during the quiescent period. A. The range of eye movements is full except for slightly reduced infraduction in the right eye. B. Upper lid retraction on the right is evident on downgaze. interictal infraduction deficit and lid retraction on down-gaze improved with the medication. However, she could not continue the medication because of elevated liver enzyme levels. Five months later, the neuromyotonia almost resolved without medication. However, mild lid retraction on downgaze remained. DISCUSSION We believe that our patient had neuromyotonia in the setting of primary aberrant regeneration of the third cranial nerve. Ocular neuromyotonia is characterized by brief, episodic contractions of muscles innervated by the oculomotor, trochlear, or abducens nerves, which result in an episodic ocular motility disorder ( 1,4). The episodes may develop spontaneously or after sustained eccentric gaze ( 1,4). Between the episodes, patients may show signs of ophthalmoplegia ( 4). Ocular neuromyotonia has been described in 45 patients and has involved the third cranial nerve in 28 ( 62.2%), the fourth cranial nerve in 4 ( 8.9%), and the sixth cranial nerve in 13 ( 28.9%) ( 1,7- 12). Ocular neuromyotonia may be idiopathic ( 1). However, most of the previously reported patients had identifiable causes including cranial irradiation ( n = 22, 48.9%) ( 4,7,13,14), neurovascular compression ( n = 3, 6.7%) ( 2,9,15), dysthyroid orbitopathy ( n = 3, 6.7%) ( 16,17), previous intracranial surgery ( n = 2, 4.4%) ( 18,19), compression by Paget disease ( n = 1,2.2%) ( 6), cavernous sinus thrombosis due to mucormycosis ( n = 1) ( 20), previous myelography ( n = 1, 2.2%) ( 21), and brainstem stroke ( n = 1, 2.2%) ( 10). Ocular neuromyotonia involving the third cranial nerve usually manifests with episodes of horizontal or vertical diplopia, lid retraction, or pupillary disorder ( 1,4,19). Previously, features of aberrant regeneration ( widening of FIG. 2. Extraocular movements during a neuromyotonic episode. On resuming primary gaze after sustained left gaze, the patient has esotropia and reduced abduction, supraduction, and infraduction of the right eye. 249 J Neuro- Ophthalmol, Vol. 26, No. 4, 2006 Choi et al the palpebral fissure on downgaze or pupillary synkinesis) had been described between the episodes in only 7 patients with third cranial nerve neuromyotonia ( 4- 6). Five of these patients also had a baseline partial third nerve palsy consisting of mild ptosis ( n = 2), ptosis with elevation deficit ( n = 1), ptosis with pupillary dilatation ( n = 1), and impaired all ductions ( n = 1) ( 4- 6). Four of the 7 patients with third cranial nerve neuromyotonia and interictal signs of aberrant regeneration had a history of cranial radiation due to parasellar tumor ( 4,5), one showed an aneurysm of the internal carotid artery, and another one exhibited severe remodeling of the skull base along with third and sixth cranial nerve palsy due to Paget disease ( 6). The remaining patient had a history of only local radiation after radical excision of a breast adenocarcinoma ( 4). Neuromyotonia associated with isolated infraduction deficit and lid retraction on downward gaze between the episodes, without a previous history of cranial radiation or a compressive cavernous sinus lesion, as was true of our patient, has not been described previously. The fact that neuromyotonia and aberrant regeneration occurred together in our patient and in previously described patients suggests a link between these two phenomena. Aberrant transmission and excessive conduction triggered by firing within a partially damaged cranial nerve may underlie them. REFERENCES 1. Frohman EM, Zee DS. Ocular neuromyotonia: clinical features, physiological mechanisms, and response to therapy. Ann Neurol 1995; 37: 620- 6. 2. Tilikete C, Vial C, Niederlaender M, et al. Idiopathic ocular neuromyotonia: a neurovascular compression syndrome? J Neurol Neurosurg Psychiatry 2000; 69: 642^ k 3. Papst W. Differential diagnosis of ocular neuromyotonia ( in German). Ophthalmologica 1972; 164: 252- 63. 4. Shults WT, Hoyt WF, Behrens M, et al. Ocular neuromyotonia: a clinical description of six patients. Arch Ophthalmol 1986; 104: 1028- 34. 5. Ezra E, Spalton D, Sanders MD, et al. Ocular neuromyotonia. Br J Ophthalmol 1996; 80: 350- 5. 6. Boschi A, Spiritus M, Cioffi M, et al. Ocular neuromyotonia in a case of Paget's disease of bone. Neuroophthalmology 1997; 18: 67- 71. 7. Eggenberger ER. Ocular neuromyotonia: report of 2 cases, review of the literature and pathophysiologic hypothesis. Neuroophthalmology 1999; 21: 249- 54. 8. Miller NR, Lee AG. Adult- onset acquired oculomotor nerve paresis with cyclic spasms: Relationship to ocular neuromyotonia. Am J Ophthalmol 2004; 137: 70- 6. 9. Versino M, Colnaghi S, Todeschini A, et al. Ocular neuromyotonia with both tonic and paroxysmal components due to vascular compression. J Neurol 2005; 252: 227- 9. 10. Banks MC, Caruso PA, Lessell S. Midbrain- thalamic ocular neuromyotonia. Arch Ophthalmol 2005; 123: 118- 9. 11. Koop G, Graf M. Ocular neuromyotonia. Klin Monatsbl Augenheilkd 2006; 223: 247- 51. 12. Morris EB 3rd, Gajjar A, Hoehn ME. Ocular neuromyotonia: video case report. Neurology 2006; 66: E27. 13. Lessell S, Lessell IM, Rizzo JF 3rd. Ocular neuromyotonia after radiation therapy. Am J Ophthalmol 1986; 102: 766- 70. 14. Fricke J, Neugebauer A, Kirsch A, Rusmann W. Ocular neuromyotonia: a case report. Strabismus 2002; 10: 119- 24. 15. Ezra E, Spalton D, Sanders MD, et al. Ocular neuromyotonia. Br J Ophthalmol 1996; 80: 350- 5. 16. Johns RJ, Knox DL, Walsh FB, et al. Involuntary eye movements in a patient with myasthenia and hyperthyroidism. Arch Ophthalmol 1962; 67: 35^ 1. 17. Chung SM, Lee AG, Holds JB, et al. Ocular neuromyotonia in Graves dysthyroid orbitopathy. Arch Ophthalmol 1997; 115: 365- 70. 18. Metz HS, Sterns G. Varying esotropia- exotropia. J Pediatr Ophthalmol Strabismus 1985; 22: 97- 9. 19. Abdulla N, Eustace P. A case of ocular neuromyotonia with tonic pupil. JNeuroophthalmol 1999; 19: 125- 7. 20. Harrison AR, Wirtschafter JD. Ocular neuromyotonia in a patient with cavernous sinus thrombosis secondary to mucormycosis. Am J Ophthalmol 1997; 124: 122- 3. 21. Yee RD, Purvin VA. Ocular neuromyotonia: three case reports with eye movement recordings. J Neuroophthalmol 1998; 18: 1- 8. 250 © 2006 Lippincott Williams & Wilkins |