| OCR Text |
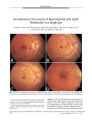
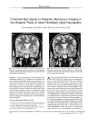
Show PHOTO ESSAY Progressive Visual Failure in an Eye with Optic Disc Drusen and an Orbital Mass Nancy M. Younan MB, BS, MPH, and Ian C. Francis, FASOPRS FIG. 1. Axial computed tomography demonstrating high attenuation in the right optic nerve head consistent with drusen, and a lobular mixed attenuation mass in the right orbital apex consistent with dermoid. Abstract: A 44- year- old woman with progressive monocular visual loss was found to have ipsilateral optic disc drusen and an ipsilateral orbital apex mass compressing the optic nerve. The mass, not the drusen, was considered responsible for the worsening vision. Visual loss should not be glibly attributed to drusen, particularly if the visual loss is rapidly progressive. Retrobulbar imaging should be considered in such cases. ( JNeuro- Ophthalmol 2003; 23: 31- 33) The Ocular Plastics Unit, The Prince of Wales Hospital, Randwick, Sydney, Australia, and the University of NSW, Sydney, Australia. Address correspondence to Ian C. Francis, FASOPRS, Suite 12, Chats-wood Grove, 12- 14 Malvern Avenue, Chatswood 2067, NSW, Australia; E- mail: if@ student. unsw. edu. au A44- year- old woman with long- standing subnormal visual acuity in the OD attributed to amblyopia presented with a 1- month history of further decline in OD vision. The patient stated that visual acuity in that eye had been measured at 20/ 120 3 years earlier. There was no other significant medical history. Examination revealed visual acuities of count fingers OD and 20/ 15 OS. There was a marked right relative afferent pupillary defect. Funduscopy of the OD demonstrated optic nerve pallor with gross optic nerve drusen and a thin nerve fiber layer. In the OS, funduscopy revealed a normal left optic nerve head. Ocular rotations and alignment were normal and there was no proptosis. Automated static perimetry demonstrated patchy right central field loss OD and a normal field OS. Because of her history of progressive visual loss, the patient underwent a computed tomography ( CT) of the head Copyright © Lippincott Williams & Wilkins. Unauthorized reproduction of this article is prohibited. J Neuro- Ophthalmol, Vol. 23, No. 1, 2003 31 JNeuro- Ophthalmol, Vol. 23, No. 1, 2003 PHOTO ESSAY FIG. 2. Proton density axial magnetic resonance imaging shows the sphenoid sinus component of the mass. FIG. 4 Coronal T1 magnetic resonance imaging shows contour deformity of the displaced optic nerve ( arrow). and orbits. This demonstrated calcification consistent with the optic nerve head drusen, as well as a 1.6 x 0.9 cm fat density bilobulated extraconal mass displacing right lateral rectus medially ( Fig. 1). The mass was located near the apex of the right orbit, but there was no intracranial extension. The provisional diagnosis of right orbital apex dermoid was made. Magnetic resonance imaging ( MRI) was then performed to evaluate intracranial spread, which disclosed that the mass extended through a small bony defect to communicate with the sphenoid sinus ( Figs. 2- 4). The decision was made to observe, rather than biopsy, the mass. Optic nerve head drusen occur in an incidence of 0.4 to 2% of the general population and are bilateral in two- thirds of cases ( 1). They represent one of the causes of pseudo-papilledema ( 2). A proposed process of formation of drusen is abnormal axonal metabolism leading to extrusion of intracellular mitochondria. Calcium is then heavily deposited in extracellular mitochondria ( 3). Most patients with optic nerve drusen are asymptomatic. However, optic nerve drusen may lead to visual field deficits including enlargement of the blind spot and arcuate scotomas ( 4,5). Nevertheless, loss of central visual acuity is rare ( 1,6). When visual acuity decreases relatively suddenly, as in our patient, a second pathology should be suspected. There have been few publications describing the infrequent simultaneous occurrence of optic disc drusen FIG. 3. Axial T1 enhanced ( left) and ( right) axial T2 magnetic resonance imaging show displacement and compression of the right optic nerve by the mass. Copyright © Lippincott Williams & Wilkins. Unauthorized reproduction of this article is prohibited. 32 © 2003 Lippincott Williams & Wilkins PHOTO ESSAY JNeuro- Ophthalmol, Vol. 23, No. 1, 2003 and orbital and intracranial tumors ( 2,7,8), and only one case of an orbital apex dermoid, which did not extend in-tracranially ( 9). Acknowledgment The authors thank Michael Biggs, FRACS, Consultant Neurosurgeon of The Royal North Shore Hospital, Sydney, Australia, for his clinical expertise. REFERENCES 1. Walsh FB, Hoyt WF. Clinical Neuro- Ophthalmology, vol 1, edn 5. In Miller N, Newman N, eds. Baltimore: Williams & Wilkins, 1998: 803. 2. Lowder C, Tomsak R, Zakov N, et al. Visual loss from pituitary tumor masked by optic nerve drusen. Neurosurgery 1981; 8: 473- 6. 3. Tso M. Pathology and pathogenesis of drusen of the optic nerve-head. Ophthalmology 1981 ; 88: 1066- 79. 4. Brodrick JD. Drusen of the disc and retinal haemorrhages. Br J Ophthalmol 1973; 57: 299- 306. 5. Cohen DN. Drusen of the optic disc and the development of field defects. Arch Ophthalmol 1971; 85: 224- 6. 6. Beck RW, Corbett JJ, Thompson HS, et al. Decreased visual acuity from optic disc drusen. Arch Ophthalmol 1985; 103: 1155- 9. 7. Rucker CW, Kearns TP. Mistaken diagnoses in some cases of meningioma. Am J Opthalmol 1961; 51: 15- 9. 8. Stiefel JW, Smith JL. Hyaline bodies ( drusen) of the optic nerve and intracranial tumor. Arch Ophthalmol 1961; 65: 814- 6. 9. Pollard Z, Calhoun J. Deep orbital dermoid with draining sinus. Am J Ophthalmol 1975; 79: 310- 3. Copyright © Lippincott Williams & Wilkins. Unauthorized reproduction of this article is prohibited. |