| OCR Text |
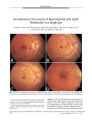
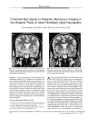
Show STATE OF THE ART Positron Emission Tomography ( PET) and Single Photon Emission Computed Tomography ( SPECT): Clinical Applications Pamela Blake, MD, Britta Johnson, BS, and John W. VanMeter, PhD Abstract: Positron emission tomography and single-photon emission computed tomography are nuclear imaging modalities that excel in depicting the biological function of tissue. Unlike structural imaging methods, they provide functional diagnostic information about brain neoplasms, stroke, neurodegenerative disorders, epilepsy, cortical visual loss, and migraine. (/ Neuro- Ophthalmol 2003; 23: 34^ 11) Positron emission tomography ( PET) and single- photon emission computed tomography ( SPECT) scanning are nuclear imaging modalities that excel in depicting the biology of living tissue. While the resolution of magnetic resonance imaging ( MRI) for structural tissue changes is unsurpassed, the ability of structural MRI to demonstrate alterations in the physiology and metabolic function of tissues remains poor. In some settings, PET or SPECT scanning serves as an adjunct to more structurally sensitive imaging methods such as MRI; in other settings, PET scanning in particular stands alone in its ability to detect changes in tissue metabolism and physiology. PET and SPECT reliably measure, among other things, glucose consumption and regional cerebral blood flow ( rCBF) and thus indirectly, tissue metabolism. Biological processes are imaged in vivo ( 1), with the use of radiolabeled molecules. Radiolabeled molecules, also referred to as radiotracers or radiopharmaceuticals, are molecules, such as glucose, that contain a radionuclide, such as 18F. PET has been used for almost 30 years to quantify normal physiology and metabolism, to characterize disease, and to evaluate the changes that result from disease processes. Theoretically, any compound of biological interest, including protein, fat, receptors, enzymes, or Department of Neurology ( PBY, JWV, BJ) and the Center for the Study of Learning ( JWV), Georgetown University Medical Center, Washington, DC, USA. Address correspondence to Pamela Blake, MD, Department of Neurology, Georgetown University Medical Center, 3800 Reservoir Road, NW Washington, DC 20007, USA; E- mail: blakep@ georgetown. edu carbohydrates, can be labeled with radioactive oxygen, nitrogen, fluorine, or carbon, among other elements, and used as a radiotracer. In this way, biological processes can be located and quantified in a way not possible with structural imaging studies. SPECT, as PET, can be used to measure a variety of biological functions and can be performed in a rapid and inexpensive manner. SPECT is used most often for measurement of rCBF, and has been used extensively in the evaluation of stroke, subarachnoid hemorrhage, and head trauma ( 2). SPECT and PET can also correlate the changes in cerebral perfusion to changes seen on structural MRI. Because rCBF generally parallels metabolic states, SPECT blood flow studies frequently give the same information as PET metabolic studies. An important exception to this principle is the case of brain tumors, which can be hypermeta-bolic and therefore display increased uptake of the glucose metabolism radiotracer 2-[ 18F] fluoro- 2- Deoxy- D- Glucose ( FDG), but often exhibit decreased uptake of Tc- 99m hex-emethylpropylenamine oxime ( HMPAO), the most commonly- used SPECT blood flow radiotracer. Advantages of PET over SPECT are superior sensitivity and spatial resolution, and a greater flexibility of incorporating positron labels into biomolecules. The main disadvantage of PET is greater expense. Most radiopharmaceuticals used for PET can only be labeled with a shortlived positron emitter, which limits the technology to centers with an on- site cyclotron unit and a nuclear chemistry laboratory ( 3). Recently, however, [ 18F] FDG has become more readily available through commercial vendors and can be delivered to PET facilities within a few hours. SPECT is less expensive, more widely available, and has greater applicability in many clinical arenas, such as the use of thallium- 201 or Tc- 99m labeled radiotracers for myocardial perfusion studies ( 3). SPECT radioisotopes typically have a much longer half- lives ( hours to days) than PET radioisotopes, which allows the manufacture of the radiopharmaceutical off- site at a significantly lower cost and the possibility of injecting the radiopharmaceutical hours before imaging ( 4). Copyright © Lippincott Williams & Wilkins. Unauthorized reproduction of this article is prohibited. 34 J Neuro- Ophthalmol, Vol. 23, No. 1, 2003 STATE OF THE ART JNeuro- Ophthalmol, Vol. 23, No. 1, 2003 HISTORY OF PET AND SPECT Blood- brain barrier scintigraphy, or " brain scanning," was initiated in the 1950s as the first form of nuclear medicine technology used extensively to image the body, prior to the advent of computed tomography ( CT) ( 4). Brain scans and catheter angiography were then the only ways to image the intracranial contents. These earliest brain scans used primarily technetium- 99m, which did not cross the blood- brain barrier to enter brain tissue unless there was a breakdown of this barrier. These early brain scanning techniques were supplanted later by CT and MRI. But as radiopharmaceuticals were developed that could be incorporated into the intracellular contents, more sophisticated methods of nuclear imaging medicine emerged. SPECT scanning was introduced in the late 1960s ( 5). PET was originally developed in the early 1970s at the Mallinckrodt Institute in St. Louis by Ter- Pogossian, Phelps et al ( 6) and used almost exclusively as a research tool until the 1990s. Reimbursement issues held back the clinical applications of PET, but recent changes in radiopharmaceutical regulation and reimbursement have resulted in its widespread use. In 1998, 69,000 PET scans were performed; in 1999, 106,000 studies were performed; in 2000, an estimated 155,000 PET scans were performed in the United States ( 7). PRINCIPLES OF PET AND SPECT PET and SPECT use radiolabeled variants of physiologically relevant molecules ( radiotracers) that emit either positrons or gamma rays when they decay. To be effective in neurologic assessment, radiotracers must be transportable across the blood brain barrier. They are designed to trace a particular physiological process, such as glucose metabolism in the case of [ 18F] FDG, or blood flow in the case of [ 150] H20 and [ 99mTc] HMPAO. The radionuclides used in PET emit positrons ( positively charged electrons) when they decay. The emitted positron travels a few millimeters in tissue before losing enough energy to allow interaction with an electron, which results in the annihilation of both particles and the creation of two gamma rays ( high energy photons) that are emitted in opposite directions. Sensors in a PET scanner attempt to detect both gamma rays simultaneously to form a line of coincidence along which the annihilation occurred. These lines of coincidence are used by reconstruction algorithms to determine the location of the source. Unlike PET, radionuclides used in SPECT do not emit positrons. Rather, a single gamma ray is generated either directly ( 99mTc) or indirectly as a result of the decay. The gamma rays are then recorded by a detector. A back projection reconstruction algorithm determines the location of the decay events. The effective spatial resolution of PET and SPECT imaging- the size of the smallest resolvable structure- depends primarily on the number of gamma rays accurately recorded by the scanner's detectors, and in the case of PET, the distance the positron travels before colliding with an electron. The reconstructed spatial resolution of SPECT is typically 8 to 10 mm, while that of PET varies from 5 to 7 mm, depending on the radionuclide. The apparent size of small anatomic structures can appear artifactually larger or smaller. Small structures that have very high uptake of a radiotracer will appear larger. Small structures that have low uptake relative to the surrounding tissues may not be easily visible; the so- called low contrast effect. PET and SPECT scanning indirectly provide functional information, as the recorded signal is that of cerebral blood flow ( in SPECT) or glucose consumption ( in FDG PET). Increased metabolic activity of cerebral tissue during a task demands increased cell nutrients, which thus results in increased perfusion and glucose metabolism in the involved tissue. A task such as unilateral hand movement increases CBF to the motor strip in the precentral gyrus on the contralateral hemisphere; opening the eyes increases flow to the occipital lobe by 30%. Regional cerebral blood flow is thus tightly linked to brain metabolism ( 4). Normal global adult cerebral blood flow ( CBF) is estimated to be about 50 ml/ min/ 100 g. Gray matter receives about 80 ml/ min/ 100 g, whereas the relatively less metabolically active white matter receives about 20 ml/ min/ 100 g. The global CBF of children aged 3 to 10 years is approximately 100 ml/ min/ 100 g. In adults and children, cerebral blood flow appears to be highest in the cerebellum and thalamus, followed by the cortex and basal ganglia, where the uptake is about 75% to 85% that of the cerebellum. Cortical blood flow may be lower in the parietal cortex. Radiation exposure for both PET and SPECT depends on the amount of tracer used in the study and the half- life of the radionuclide. Almost all tracers are cleared through the urinary tract, thus resulting in the urinary bladder experiencing the highest radiation exposure. In general, radiation exposure for both PET and SPECT is approximately equivalent to a CT procedure, and may be as high as 10 effective dose equivalents ( EDE). The radiation exposure in pediatric patients is significantly higher than adults and decreases with age. PET Scanning PET uses positron- labeled molecules in negligible amounts to image and measure the function of biologic processes with minimal disturbance to the tissue under study. Most biologically active molecules may be labeled with a positron- emitting radioisotope to evaluate the function under study. The Food and Drug Administration ( FDA) has approved three PET radiopharmaceuticals for routine clinical use in humans: [ 18F] FDG, [ 13N] ammonia, and [ 18F] fluo-ride. Other radiopharmaceuticals, including [ 150] H20, and Copyright © Lippincott Williams & Wilkins. Unauthorized reproduction of this article is prohibited. 35 JNeuro- Ophthalmol, Vol. 23, No. 1, 2003 STATE OF THE ART many [ nC] labeled compounds are used primarily for research. The most commonly used agent, 2-[ 18F] fluoro- 2- deoxy- D- Glucose, or FDG, is injected intravenously and distributes throughout the body via the bloodstream. Upon entering organs, it traces the transport and phosphorylation of glucose. Tissues with higher glucose metabolism demonstrate a proportionately higher uptake of FDG. Glucose metabolism provides about 95% of the adenosine triphosphate ( ATP) required for brain function ( 8). FDG is rapidly taken into the intracellular compartment, but because its metabolism stops following its phosphorylation to fluoro- deoxyglucose- 6- phosphate, the radiolabel cannot diffuse from the brain. It remains trapped intracellularly, and is thus particularly well suited for imaging cerebral metabolism. The regional cerebral metabolic rate for glucose ( rCMRglc) and the rCBF, which corresponds to the rCMRglc, correlate strongly with local brain functional activity at the level of the synapse ( 9). The entire body or a single organ may be imaged during one PET session. A whole body PET scan, such as that performed in search of metastatic disease, can be completed in 1 to 2 hours. A study of the brain generally requires 15 to 30 minutes. SPECT Scanning For the performance of most neurologic SPECT studies, a flow tracer is tagged with a radionuclide and injected intravenously. The radiotracer accumulates in different areas of the brain relative to the amount of blood perfusing the area. Single photons are emitted, and for most clinical purposes, the level of activity is quantified as a reflection of regional cerebral blood flow. The FDA has approved three brain perfusion radiopharmaceutical agents for SPECT clinical use: ( 1) Io-dine- 123 ( 123I) N- isopropyl- p- iodoamhetamine ( IMP, Spectamine); ( 2) Technetium- 99m ( 99mTc) hexemethylpro-pylenamine oxime ( HMPAO, Ceretec); and ( 3) 99mTc ethyl cysteinate dimmer ( ECD, Neurolite). Each agent has benefits and drawbacks. [ 99mTc] HMPAO, the agent in greatest use in clinical practice, has a rapid uptake into the brain and reaches its maximum within 10 minutes, with the radiotracer remaining at a constant distribution for many hours, allowing for flexibility in obtaining images. The radiolabeled tracer is unstable in vitro after about 30 minutes. 123I IMP is used less often, because its concentration may be decreased in the face of the low plasma pH seen in cerebral ischemia, has a rapid blood clearance, which results in high brain- to- soft- tissue rations early after injection. Unlike [ 99mTc] HMPAO, [ 99mTc] ECD is stable in vitro for 6 hours, allowing great flexibility in the study of episodic phenomena such as seizures. Thallium- 201 chloride ( 201T1) SPECT is a commonly used radionuclide technique for imaging CNS tumors and differentiating radiation necrosis from recurrent tumor. 201T1 cannot normally diffuse into healthy brain tissue because of an intact blood- brain barrier. In one study ( 10), patients with high 201T1 uptake were proven pathologically to have local tumor recurrence, while those with low 201T1 uptake were proven to have radiation changes. 201T1 SPECT is also important in differentiating benign from malignant conditions and in assessing tumor grade. The inert gas xenon, or 133Xe, has also been used to study rCBF. After 133Xe is inhaled, clearance techniques are used to relate the change in radiotracer activity over time to blood flow. The principle advantage of 133Xe over other tracers is its ability to measure rCBF quantitatively and repeatedly without arterial blood sampling. As with all SPECT imaging, the spatial resolution of this method is less than that of H2015 PET measurements of blood flow. A brain SPECT scan generally requires 20 to 45 minutes. CLINICAL USES OF PET AND SPECT Neoplasms The most common clinical use for PET scanning today is the investigation of malignancy ( Fig. 1) ( 11). Whole-body studies are routinely performed to search for distant metastases once a patient has been diagnosed with a primary tumor. Because tumor cells require more energy than normal cells, glucose metabolism in malignant cells usually is significantly higher. Whole- body FDG- PET can detect abnormal tumor metabolism before anatomic changes # FIG. 1. PET scan of a 54- year- old man with right frontoparietal lesion on magnetic resonance imaging. Brisk uptake of tracer is consistent with a neoplastic process. Biopsy showed anaplastic astrocytoma. ( This figure can be viewed in color on the Journal Web site, www. jneuro- ophthalmology. com). Copyright © Lippincott Williams & Wilkins. Unauthorized reproduction of this article is prohibited. 36 © 2003 Lippincott Williams & Wilkins STATE OF THE ART JNeuro- Ophthalmol, Vol. 23, No. 1, 2003 appear, and allows differentiation of malignant from benign anatomic abnormalities. Conversely, the false positive rate of MRI for intracranial metastasis in patients with known primary neoplasia has been found to be as high as 11 % ( 12). A positive PET study can help to establish the diagnosis of brain tumors without biopsy, which is of particular value in tumors that are not accessible ( 10). PET has been shown to improve detection and staging of malignancy by 8% to 43% compared with conventional evaluations in direct comparisons ( 1), and can therefore potentially replace a compendium of studies including bone scan and CT of the chest, abdomen, and pelvis. Studies have shown that treatment is changed in 20%> to 40%> of patients based on the findings of whole- body PET ( 13- 16). About 65%> of these patients are " upstaged" because unsuspected metastases are detected, and about 35%> are " downstaged" when structural changes are found not to be malignant. An FDG- PET study of 31 patients with suspected intracranial metastases ( 17) based on CT or MRI showed focal hypermetabolic abnormalities in 19 patients, all of whom were proven to have metastatic disease. Two of the 22 patients with proven metastatic disease had hypometabolic lesions on PET scanning. All lesions seen on CT or MRI that were eventually shown to be benign in nature were hypometabolic. The most common indication for a PET scan in a patient with a known brain tumor is to distinguish recurrent tumor from postradiation changes, a difficult task for clinical or structural imaging methods alone. PET scanning takes advantage of the different metabolic conditions of these two pathologies, namely the hypermetabolism of a malignant lesion and the hypometabolism of radiation necrosis. [ 18F] FDG PET scans generally demonstrate increased uptake of tracer in malignancies, and decreased uptake in radiation necrosis. The relatively brief scanning time and minimal claustrophobia associated with PET and SPECT studies make them particularly useful in children with brain tumors. SPECT is widely used, as 80%> of pediatric tumors demonstrate uptake of thallium- 201 chloride ( 201T1) ( 15,18). SPECT and PET scanning may also be used to evaluate intracerebral lesions in immunocompromised patients. In HIV disease, for instance, the differential diagnosis of a CNS structural lesion includes lymphoma ( 30%), toxoplasmosis ( 60%), and other infections. Intracerebral lymphoma typically demonstrates significantly increased uptake of FDG, whereas infection does not ( 19). A new radiopharmaceutical, 18F fluorochlorine, is currently under development for the detection of prostate malignancies ( 4). Stroke Stroke was the first clinical application of SPECT cerebral perfusion imaging. Decreased rCBF is visualized in the form of decreased signal on SPECT and PET. The sensitivity of SPECT to cerebral ischemia is 90% o within the first hours after the event ( 2). This sensitivity is greater than that of CT ( 20%), but less than that of diffusion- weighted magnetic resonance imaging ( DWI), which is nearly 100%. The specificity of SPECT for ischemia is 88% to 90%, higher than that of DWI. DWI will show high signal whenever there is a very hyperintense signal on T2- weighted images ( T2 shine- through effect), as may be seen with many nonischemic conditions including demyelinating disease or white matter shearing injuries from head trauma. SPECT scanning is also helpful in determining the size of the ischemic penumbra, the area of ischemic tissue that surrounds the core of infarcted tissue, and is vulnerable to subsequent infarction. Preventing infarction of the pen-umbric tissue is one of the major aims of the management of acute stroke today. In clinical trials, a combination of DWI and SPECT may be used to determine if there is sufficient penumbric tissue to warrant acute thrombolytic or neuroprotective intervention. Within 1 to 10 days after an infarct, the ischemic area may display increased perfusion on SPECT. This is " luxury perfusion," the non- nutritive flow that occurs in the setting of uncoupled metabolism and rCBF in the infarcted brain. Local accumulation of metabolic end products of infarction, such as potassium ions and lactic acid, are responsible for this phenomenon. SPECT may also be helpful in determining cardiovascular reserve. In the setting of decreased CBF, a compensatory tissue response is to extract an increased amount of oxygen by local vasodilatation. This increases the ratio of blood volume to blood flow in brain tissue, an indication that the tissue is at risk for infarction. Later after a brain infarction, SPECT and PET scans may still show areas of decreased perfusion ( Fig. 2). SPECT perfusion scans have been used to detect intracranial vasospasm following subarachnoid hemorrhage, particularly inpatients who cannot be tested accurately with transcranial Doppler, or in whom one wishes to avoid the hazards of a conventional cerebral angiogram. SPECT scanning has also been used to detect steal phenomena in arteriovenous malformations. Degenerative Disorders PET scanning has been extensively studied in the diagnosis of degenerative disorders, particularly the dementias. The most common degenerative dementing illness is Alzheimer disease ( AD), a slowly progressive process characterized neuropathologically by the presence of paired helical filaments composed of tau proteins in the nerve cell body, where they are referred to as neurofibrillary tangles. Extracellular amyloid plaques are also seen, although these may also occur in normal aging ( 20). Structural neuroimag-ing in patients with AD is usually normal in the early stage Copyright © Lippincott Williams & Wilkins. Unauthorized reproduction of this article is prohibited. 37 JNeuro- Ophthalmol, Vol. 23, No. 1, 2003 STATE OF THE ART FIG. 2. PET scan of a 28- year- old woman with persistent right- sided sensory symptoms. Magnetic resonance imaging showed vague signal changes in the left frontoparietal area. PET scan demonstrates decreased uptake of tracer in the same area, consistent with an infarct. ( This figure can be viewed in color on the Journal Web site, www. jneuro- ophthalmology. com). of the disease and typically shows only nonspecific cortical atrophy as the disease advances. The typical FDG PET changes seen in AD, including reduced uptake of FDG in the bilateral temporal, parietal, and particularly cingulated gyrus may be seen in its very earliest stages ( 21). Similar to FDG PET, Tc- HMPAO SPECT studies have shown a striking pattern of reduced glucose uptake in the parietotemporal cortex ( 22). This contribution of PET and SPECT scanning is extremely important in the management of patients with AD, for whom the available treatments may be effective only when administered early in the course of the disease. By contrast, other dementing illnesses demonstrate different patterns of reduced cortical uptake with functional imaging. Lewy Body Disease, which is characterized by the presence of cytoplasmic concentric hyaline inclusions ( Lewy bodies) demonstrates reduced uptake in the frontal cortex and also in the posterior association cortex, and fr-ontotemporal dementias demonstrate reduced uptake in the frontal cortex ( 20). In patients with early and intermediate Huntington disease ( HD), subcortical metabolic defects are apparent in the caudate and putamen, while the structural MRI may be normal in early HD and may show reduction in volume of the caudate and putamen in intermediate and advanced disease. As is the case with familial AD, PET studies of HD offer the possibility of disease detection in the presymptom-atic phase. Epilepsy Among the methods available to determine epileptogenic foci, including surface electroencephalogram ( EEG), depth electrocorticography, intraoperative corticography, and structural MRI, none is 100% sensitive, and some are highly invasive. As surgical resection of epileptogenic foci becomes more widely available, highly specific localization of the seizure focus becomes paramount. SPECT scanning may also be a useful adjunct to the above methods ( 2). Several examiners have shown that during the seizure ictus there is a dramatic increase in CBF on SPECT. The increased CBF is focal in partial seizures and diffuse in generalized seizures. The same epileptogenic tissue shows decreased CBF on inter- ictal SPECT scans. This combination of findings on scans performed during and between seizures is highly sensitive and specific for the localization of seizure foci, even in patients with seizures that clinically generalized. An ictal study does not mean that the scan must be performed at the moment the patient is seizing; a SPECT scan taken several hours after the injection will show the distribution of tracer at the time the tracer was injected. Hence, a seizing patient can be injected with tracer in the intensive care unit or EEG laboratory, stabilized, and then transported to the scanner several hours later. SPECT scanning may also be helpful in differentiating seizures from pseudoseizures. Because of the low resolution of SPECT, its combination with MRI in patients with partial epilepsy has enhanced diagnosis. SPECT and MRI are compared side by side ( coregistered) to localize the anatomic structure corresponding to an abnormality seen on the SPECT scan ( 4). PET has been used in delineating the function of tissue in the setting of neuronal migration anomalies. While MRI scanning in some patients with intractable epilepsy has shown the presence of ectopic gray matter in the cerebral hemispheres, PET scanning has allowed confirmation that the tissue is metabolically active and therefore consistent with a heterotopia capable of generating seizures ( 23). Cortical Visual Loss An intriguing aspect of PET and SPECT scanning is the ability to detect abnormalities in brain physiology in areas that appear normal on structural MRI. Silverman et al ( 24) described seven patients with visual loss whose symptoms could not be adequately explained on the basis of MRI imaging, which was either normal or inadequately abnormal to account for the degree of visual loss. [ 99mTc] HMPAO SPECT revealed alterations in cerebral blood flow in the visual pathways in patients with visual loss due to traumatic brain injury, status epilepticus, stroke, carbon monoxide exposure, and AD. Moster et al ( 25) described a patient with carbon monoxide exposure and a patient with post-hypoxic encephalopathy who complained of visual loss Copyright © Lippincott Williams & Wilkins. Unauthorized reproduction of this article is prohibited. 38 © 2003 Lippincott Williams & Wilkins STATE OF THE ART JNeuro- Ophthalmol, Vol. 23, No. 1, 2003 but who had normal MRI scans. The patients had initially been diagnosed as having psychogenic visual loss, but both showed reduced FDG- PET signal in the occipital regions. Drubach et al ( 26) described a patient with a unilateral occipital ischemic lesion by MRI but bilateral homonymous hemianopia. SPECT images revealed bilateral perfusion defects, correlating more closely with the patient's visual field defects. Migraine A reduction in CBF during the aura of migraine was formerly considered the cause of the deficits. We now know that this reduction is due to autoregulatory compensation triggered by a spreading wave of depolarization (" spreading depression") that originates in the occipital lobe and disperses across the rest of the cerebral hemispheric cortex ( 27). Woods et al ( 28) reported a patient who was undergoing SPECT scanning as a control for a research study when she experienced migraine with mild blurring of vision as an aura. The SPECT scan demonstrated an overall 40% decrease in cortical CBF, most marked at the occipital cortex. Bednarczyk et al ( 29) studied chronic migraine patients with oxygen PET scanning in between attacks, and then performed at least one scan during a migraine. They found a 13% reduction in global CBF during the migraine attack compared with periods in between attacks. The oxygen extraction ratio was not significantly diminished, however. PET studies have also been instrumental in determining the location of areas of activation in the brainstem ( 30) and hypothalamus ( 31) ictally in patients with migraine and cluster headaches respectively. Activation of these areas related to increases in ictal blood flow is proposed as a potential etiology of these forms of headache. Mellies et al ( 32) described the SPECT features of a German family with Cerebral Autosomal Dominant Arteri-opathy with Subcortical Infarcts and Leukoencephalopathy ( CADASIL), an autosomally dominant disorder characterized by migraine, transient ischemic attacks ( TIAs), and lacunar stroke with stepwise progression. This first SPECT study of CADASIL showed cortical hypoperfusion in every affected subject compared with healthy relatives. CBF was significantly reduced in the parietal region, but most pronounced in temporal and frontal regions. This study substantiates frontal system impairment in cerebral small-vessel disease. Movement Disorders In ten patients with essential blepharospasm, PET scanning showed significant elevation in the uptake of FDG in the striatum and thalamus as compared with the temporal or parietal cortex ( 33). PET studies were performed before and 2 weeks after the subcutaneous injection of botulinum toxin, at a time when the patients had the expected improvement in their spasm, and the results were unchanged. Conversely, PET scanning in Parkinson disease has shown markedly decreased uptake of radiopharmaceuticals that trace the dopamine system ( such as F- Dopa) in the striatum ( 34). Decreased frontal glucose metabolism has been detected by PET in patients with progressive supranuclear palsy ( PSP) ( 35). SPECT scanning in PSP has shown reduced cerebral perfusion in the frontal lobes bilaterally ( 35). PET and SPECT Scanning and the Human Visual Cortex Perhaps the most exciting role for nuclear medicine imaging is in the further study and delineation of the functions of the human visual cortex. In 1991, Zeki et al ( 36) used PET scanning of human subjects to confirm the existence of specialized centers in the human extrastriate visual cortex to identify color ( V4) and motion ( V5), locations already experimentally verified in the macaque monkey. PET has been a useful tool to evaluate areas of cerebral cortical activation. Cohen et al ( 37) used PET to show that congenitally blind patients and those who lost sight before the age of 14 had strong activation of the occipital cortex in association with Braille reading, an example of cross-modal plasticity. In individuals who lose sight after the age of 14, however, such activation is not seen. PET studies of hypnotized subjects performing visual tasks such as imagining colors ( 38) have shown appropriate activation of area V4 whether the subjects were actually viewing colors or merely imagining that they were. Comparison of PET and SPECT with Functional MRI MRI is capable of functional imaging ( fMRI). Two different MR methods have been developed to image neuronal activity as a function of blood flow. The first uses perfusion- weighted imaging with a contrast agent ( typically gadolinium Gd- DTPA) as a magnetic tracer to derive cerebral blood volume ( CBV) and CBF maps ( perfusion-weighted method) ( 39). The second more widely used method uses the differential effect of oxyhemoglobin and deoxyhemoglobin on the MR signal as an endogenous magnetic tracer of blood flow ( blood oxygen- level dependent, or BOLD, method) ( 40). The perfusion- weighted fMRI method has a temporal resolution of several minutes, similar to that of PET. By contrast, BOLD fMRI has a temporal resolution of a few seconds, allowing the collection over a hundred whole brain scans ( 45 slices) in a matter of minutes. However, an advantage of perfusion- weighted fMRI is its spatial resolution, which is 1 mm3 voxel ( comparable to conventional MRI), while that of the BOLD method is 2 to 3 mm3 voxels. Copyright © Lippincott Williams & Wilkins. Unauthorized reproduction of this article is prohibited. 39 JNeuro- Ophthalmol, Vol. 23, No. 1, 2003 STATE OF THE ART While the spatial resolution of both fMRI methods is better than that of PET and SPECT, which is at best 4 mm3, reliance on measuring neuronal activity using hemodynamic correlates limits the ultimate achievable resolution. In addition, unlike PET and SPECT, neither method of functional MRI involves the use of ionizing radiation. This feature allows fMRI studies to be performed in populations that cannot be studied easily with nuclear imaging, such as children. In addition, by using fMRI it is possible to perform multiple research studies in healthy subjects without concerns of radiation exposure, whereas use of PET and SPECT in healthy controls is typically limited to a single study. Another major advantage of fMRI is the temporal resolution, which is more than a factor of two better than PET, and more than an order of magnitude better than SPECT. A disadvantage of fMRI is the relatively small signal change that is measurable. Both PET and SPECT exhibit a percent signal change from a baseline ( resting) state to an activated state on the order of 20% while only a 2% to 7% signal change is observable with BOLD fMRI and approximately 10% with perfusion- weighted fMRI at 1.5 Tesla. Neither fMRI method provides a quantitative measure of activity, which is possible with PET, and in a limited fashion, with SPECT. In addition, both PET and SPECT can be used to measure other facets of neuronal function such as glucose metabolism, receptor density, and neurotransmitter function. These capabilities are not possible with fMRI. These measures provide clinically important information that is not correlated with blood flow- related changes. Finally, while significant progress has been made in understanding the exact relationship between the BOLD signal and neuronal activity, the mechanism of the signal change detected in BOLD fMRI imaging remains only partially explained ( 41). FUTURE PROSPECTS The future of PET scanning is bright, as the technology will improve from the standpoint of both radiopharmaceuticals and instrumentation. CT scanners have been combined with PET scanners to allow for more accurate registration of anatomy and biology and improved PET reconstruction. The development of the micro- PET scanner for use in animal research will allow for improved spatial resolution, which will undoubtedly lead to improved anatomic detail. Neurotransmitter studies employing specific tracers for serotonin ( 42), benzodiazepine receptors ( 43), and dopamine ( 44) have contributed greatly to the understanding of psychiatric and neurologic disorders. These studies, and the ongoing use of PET and SPECT scanning in clinical and research applications, will continue to expand our knowledge of the biologic processes of the brain in normal and disordered states. REFERENCES 1. Phelps ME. PET: the merging of biology and imaging into molecular imaging. JNuclMed 2000; 41: 661- 81. 2. The Therapeutics and Technology Assessment Subcommittee of the American Academy of Neurology. Assessment of brain SPECT. Neurology. 1996; 46: 278- 85. 3. Thrall B. Single- Photon Emission Computed Tomography and Positron Emission Tomography. In: Thrall JH, Zeissman HA, eds. Nuclear Medicine: The Requisites. St. Louis: Mosby, 2001: 33^ 17. 4. Zeissman HE. Central Nervous System. In: Thrall JH, Zeissman HA, eds. Nuclear Medicine: The Requisites. St. Louis: Mosby, 2001: 294- 321. 5. Kuhl DE, Edwards RQ. The Mark 3 Scanner: a compact device for multiple- view and section scanning of the brain. Radiology 1970; 96: 563- 70. 6. Ter- Pogossian MM, Phelps ME, Hoffman EJ, et al. A positron-emission transaxial tomograph for nuclear imaging ( PETT). Radiology 197 5; U4( l): 89- 98. 7. Coleman RE. Clinical PET: role in diagnosis and management. JNucl Med 2000 ; 41: 36N- 42N. 8. Sokoloff L. Circulation and energy metabolism of the brain. In: Sie-gel G, Agranoff B, Albers RW, Molinoff P, eds. Basic Neurochem-istry 4th edn, New York, NY: Raven, 1989: 565- 90. 9. Sokoloff L. Relationship between functional activity and energy metabolism in the nervous system: whether, where and why. In: Lassen NA, Ingvar DH, Raichle ME, Friberg L, eds. Brain Work and Mental Activity: Quantitative Studies with radioactive tracers- Alfred Benzon Symposium VIII, Vol 31. Copenhagen, Denmark: Munksgaard; 1991: 52- 67. 10. Hustinx R, Alavi A. SPECT and PET imaging of brain tumors. Neu-roimaging Clin N Am 1999; 9( 4): 751- 66 11. Phelps ME. Positron emission tomography provides molecular imaging of biologic processes. Proc Natl Acad Sci USA 2000; 97( 16): 9226- 33 12. Schaefer PW, Budzik RF Jr., Gonzalez RG. Imaging of cerebral metastases. Neurosurg Clin North Amer 1996; 7( 3): 313- 23 13. Beets G, Penninckx F, Schiepers C, et al. Clinical value of whole-body positron emission tomography with [ 18F] fluorodeoxygluxose in recurrent colorectal cancer. Br J Surg 1994; 81: 1666- 70. 14. Marom EM, McAdams HP, Erasmus JJ, et al. Staging non- small cell lung cancer with whole- body PET. Radiology 1999; 212: 803- 9. 15. Vitola JV, Delbeke D, Sandler MP, et al. Positron emission tomography to stage suspected metastatic colorectal carcinoma to the liver. Am J Surg 1996; 171: 21- 6. 16. Rinne D, Baum HP, Hor G, et al. Primary staging and follow- up of high- risk melanoma patients with [ 18F] fluorodeoxygluxose positron emission tomography. Cancer 1998; 82: 1664- 71. 17. Gupta NC, Nicholson P, Bloomfield SM. FDG- PET in the staging work- up of patients with suspected intracranial metastatic tumors. Ann Surg 1999; 230( 2): 202- 6. 18. Maria BL, Drane WE, Quisling RG: Value of thallium- 201 SPECT imaging in childhood brain tumors. Pediatr Neurosurg 1994; 20: 11- 8. 19. Skiest D, Erdman W, Chang W, et al. use of thallium- 201 SPECT scanning and Toxoplasma serology for presumptive diagnosis of CNS lesions in patients with AIDS. Int ConfAids 1998; 12: 1049. 20. Dickson DW. Alzheimer's disease and dementia. Clin Ger Med 2001; 17( 2): 209- 28. 21. Minoshima J, Giordani B, Berent S, et al. Metabolic reduction in the posterior cingulate cortex in very early Alzheimer's disease. Ann Neurol 1997; 42( l): 85- 94. 22. Steinling M, Defebvre L, Duhamel A, et al. Is there a typical pattern of brain SPECT imaging in Alzheimer's Disease? Dement Geriatr Cogn Disord 2001; 12( 6): 371- 8. 23. Falconer J, Wada JA, Martin W, et al. PET, CT, and MRI imaging of neuronal migration anomalies in epileptic patients. Can J Neurol Sci 1990; 17( l): 35- 9. 24. Silverman IE, Galetta SL, Gray LG, et al. SPECT in patients with cortical visual loss. JNuclMed 1993; 34( 9): 1447- 51. Copyright © Lippincott Williams & Wilkins. Unauthorized reproduction of this article is prohibited. 40 © 2003 Lippincott Williams & Wilkins STATE OF THE ART JNeuro- Ophthalmol, Vol. 23, No. 1, 2003 25. Moster ML, Galetta SL, Schatz NJ. Physiologic imaging in " functional" visual loss. Surv Ophthalmol 1996; 40( 5): 395- 9. 26. Drabach DA, Carmona S, Mayerrose GE, et al. Brain SPECT in a case of cortical blindness. Stroke 1994; 25( 5): 1061^ 1. 27. Lauritzen M. Cortical spreading depression in migraine. Cephalalgia 2001; 21( 7): 757- 60. 28. Woods R, Jacoboni M, Mazziotta J. Bilateral spreading cerebral hypoperfusion during spontaneous migraine headache. N Engl J Med 1994; 331: 1689- 92. 29. Bednarczyk EM, Remler B, Weikart C. Global cerebral blood flow, blood volume, and oxygen metabolism in patients with migraine headache. Neurology 1998; 50( 6): 1736^ 10. 30. Bahra A, Mathara MS, Buchel C, et al. Brainstem activation specific to migraine headache. Lancet 2001 ; 357( 9261): 1016- 7. 31. May A, Bahra A, Buchel C, et al. PET and MRA findings in cluster headache and MRA in experimental pain. Neurology 2000; 55( 0): 1328- 35. 32. Mellies JK, Baumer T, Muller JA. SPECT study of a German CADASIL family. Neurology 1998; 50( 6): 1715- 21. 33. Esmaeli- Gutstein B, Nahmias C, Thompson M, et al. Positron emission tomography in patients with benign essential blepharospasm. Ophthal Plast Reconstr Surg 1999; 15( l): 23- 7. 34. Martin WRW. Parkinson's Disease: Positron emission tomographic studies. Semin Nerol 1989; 9: 351- 6 35. Anouti A, Koller WC. Diagnostic testing in movement disorders. Neurol Clin 1996; 14( l): 169- 82. 36. Zeki S, Watson JD, Lueck CJ, et al. A direct demonstration of functional specialization in human visual cortex. JNeurosci 1991; 11( 3): 641- 9. 37. Cohen LG, Weeks RA, Sadato N. Period of susceptibility for cross-modal plasticity in the blind. Ann Ate/ ro/ 1999; 45( 4): 451- 60. 38. Kosslyn SM, Thompson WL, Costantini- Ferrando MF, et al. Hypnotic visual illusion alters color processing in the brain. Am J Psychiatry 2000; 157( 8): 1279- 84 39. Belliveay JW, Rosen BR, Kantor HL, et al. Functional cerebral imaging by susceptibility- contrast NMR. Magn Reson Med 1990; 14 ( 3): 538^ 16 40. Kwong KK, Belliveau JW, Chesler DA, et al. Dynamic magnetic resonance imaging of human brain activity during primary sensory stimulation. Proc Natl Acad Sci USA 1992; 89( 12): 5675- 9. 41. Logothetis NK, Pauls J, Auguth M. Neurophysiologiv investigation of the basis of the fMRI signal. Nature 2001; 412( 6843): 150- 7. 42. Wilson AA, Ginovart N, Ffussey D, et al. In vitro and in vivo characterization of [ 11C]- DASB: a probe for in vivo measurements of the serotonin transporter in positron emission tomography. Nucl Med Biol 2002; 29( 5): 509- 15 43. Nutt DJ, Malizia AL. New insights into the role of the GABA( A)- benzodiazepine receptor in psychiatric disorders. Br J Psychiatry 2001; 179: 390- 6 44. Arajuo DM, Cherry SR, Tatsukawa KJ, et al. Deficits in striatal dopamine D( 2) receptors and energy metabolism detected by in vivo micro PET imaging in a rat model of Huntington's Disease. Exp Neurol 2000; 166( 2): 287- 97 Copyright © Lippincott Williams & Wilkins. Unauthorized reproduction of this article is prohibited. 41 |