| OCR Text |
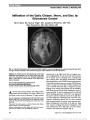
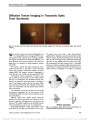
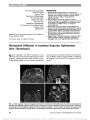
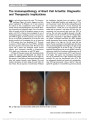
Show Papilledema Due to a Permanent Catheter for Renal Dialysis and an Arteriovenous Fistula: A "Two Hit" Hypothesis Melissa A. Simon, MD, Ennis J. Duffis, MD, Michael A. Curi, MD, Roger E. Turbin, MD, Charles J. Prestigiacomo, MD, Larry P. Frohman, MD Abstract: Elevated intracranial pressure in patients with chronic renal failure has several potential causes. Its rare occurrence secondary to the hemodynamic effects of hemodialysis is described and the findings support a multi-factorial etiology ("two hits"). Journal of Neuro-Ophthalmology 2014;34:29-33 doi: 10.1097/WNO.0000000000000063 © 2013 by North American Neuro-Ophthalmology Society Avariety of factors may lead to elevated intracranial pres-sure (ICP) in patients with chronic renal failure. Our patient had a permanent central catheter for hemodialysis and, after multiple procedures for dialysis access, presented with headaches and bilateral papilledema caused by elevated ICP. We propose a multifactorial etiology to explain our patient's clinical findings. CASE REPORT A 65-year-old man complained of headaches, tinnitus, and slowly progressive blurring of vision for several months. He had end-stage renal disease and had undergone multiple angioplasties and revisions of arteriovenous fistulas (AVF) for dialysis. At the time of presentation, he had a permanent dialysis catheter in the right internal jugular vein (IJV). The patient was obese, with a history of hypertension, hypercholesterolemia, and seizures and had a pacemaker for episodes of bradycardia. Medications included sevelamer carbonate, benzonatate, enalapril, fexofenadine, isosorbide, hydralazine, amlodipine, nifedi-pine, and phenytoin. A failed AVF placed in the left arm required ligation and led to placement of a permanent catheter in the right IJV and a new AVF was created in his right arm. Because the patient developed a steal syndrome affecting his right hand, the distal radial artery was treated with coil embolization. The right AVF continued to mature and the patient continued to rely on the central catheter for dialysis. Three weeks later, visual acuity was 20/50 in each eye, with normal pupillary reactions, color vision, and ocular motility. Bilateral cataracts were present on slit-lamp examination. Confrontation visual fields were intact, and fundoscopy revealed bilateral optic disc edema. Neurolog-ical examination was normal. Magnetic resonance imaging (MRI) studies could not be performed because of the patient's pacemaker. Computed tomography (CT) of the brain without contrast (due to renal failure) showed only microvascular ischemic changes and mild pansinusitis. Opening pressure on lumbar puncture was 30 cm H2O with mild elevation of cerebrospinal fluid (CSF) protein of 51 mg/dL (normal, 15-45 mg/dL). CSF glucose and cell count were normal. Because of his renal failure, the patient could not be treated with acetazolamide. Three days after the lumbar puncture, acuity was 20/30 bilaterally. Automated visual fields revealed enlargement of the blind spots and there was bilateral optic disc edema on funduscopy (Fig. 1). An intracranial venogram demonstrated elevated intra-cranial venous pressures throughout the cerebral venous system with measurements ranging from 40 to 50 mm Hg. Although the venous system was patent, there was reduced opacification of the transverse sinuses and the IJVs. In addition, the transit times from the cerebral arterial through venous phases was increased. Departments of Ophthalmology and Visual Science (MAS, RET, LPF), Neurosurgery (EJD), Vascular Surgery (MAC), Neurology and Neurosciences (LPF), Rutgers-New Jersey Medical School, Newark, New Jersey. The authors report no conflicts of interest. Address correspondence to Melissa A. Simon, MD, 90 Bergen Street, Suite 6100, Newark, NJ 07103; E-mail: simome@ohsu.edu Simon et al: J Neuro-Ophthalmol 2014; 34: 29-33 29 Original Contribution Copyright © North American Neuro-Ophthalmology Society. Unauthorized reproduction of this article is prohibited. Six days later, a fistulogram of the right dialysis shunt showed a patent AVF of the right forearm. A central venogram demonstrated a patent right subclavian vein and superior vena cava, the permanent catheter in the right IJV, and high-grade stenosis of the proximal right subclavian vein extending into the brachiocephalic vein (Fig. 2). Angioplasty of the right subclavian vein was performed and the right IJV catheter was removed. A repeat venogram immediately after these procedures demonstrated improved flow from the sub-clavian vein into the superior vena cava (Fig. 3). The next day, the patient reported that his headaches had resolved, and 5 months later, visual acuity was 20/25 bilaterally, with normal visual fields and fundi. The patient noted resolution of headaches and tinnitus. Over the following year, the patient experienced recur-rent subclavian vein stenosis with right arm swelling. However, he had no recurrence of headaches or visual complaints. DISCUSSION There are 5 reported cases of patients with increased ICP linked to dialysis catheters or grafts, all with a combination of increased flow from the AVF and obstruction from venous stenosis or thrombosis (1-5). In 3 patients, papil-ledema resolved after ligation of the graft, 1 after balloon dilation to improve stenosis, and 1 patient's symptoms did not resolve before her illness progressed to brain infarction FIG. 1. Bilateral papilledema is present. FIG. 2. Venogram with high-grade stenosis of the right subclavian vein extending into the brachiocephalic vein. 30 Simon et al: J Neuro-Ophthalmol 2014; 34: 29-33 Original Contribution Copyright © North American Neuro-Ophthalmology Society. Unauthorized reproduction of this article is prohibited. and death (Table 1). All cases, including ours, are unified by similar etiologies: high venous flow in conjunction with venous obstruction. Retrograde venous flow from AVFs into the ipsilateral IJV led to impaired cerebral venous drainage. In addition, compromised venous outflow by an obstructed central vessel caused increased flow elsewhere in the cerebral venous network. Both factors led to elevated ICP. Our patient had both an AVF-causing high flow and a central venous obstruction caused by ipsilateral permanent catheter and extended pacemaker wire. Our case is unique, in that the permanent catheter was still in place at the onset of elevated ICP. Because the symptoms improved dramat-ically after removal of the catheter and the AVF remained in place, the increased ICP cannot be explained solely by the AVF. Rather, the central catheter caused decreased venous return from the intracranial venous system, being partially obstructive in the IJV, the brachiocephalic vein, and superior vena cava. Increased venous flow from the arteriovenous graft combined with outflow obstruction resulted in elevated intracranial venous pressure. Given the lack of reflux of dye into the jugular system after catheter removal (Fig. 3), we do not think that the fistula alone or the right subclavian stenosis alone caused our patient's symptoms. Additionally, our patient devel-oped right arm swelling and subclavian vein stenosis in the same location over a year after catheter removal, requiring repeat angioplasty. It is interesting that this did not lead to headache and papilledema. This suggests that the catheter was restricting outflow from the right IJV, either directly or by increasing IJV pressure with compromised superior vena cava outflow. Our patient's condition was unusual because he had no alternative pathways for drainage; he had a chronic left innominate vein occlusion because of the pacemaker wire restricting outflow from the left side of the head and a fistula on the right with the subclavian stenosis. The result was high pressure in the right subcla-vian vein and restricted drainage of the external jugular vein, which could have provided an alternative drainage pathway. No vascular collaterals were apparent on his fistulogram. Dialysis catheters have been associated with venous stenosis. Surratt et al (6) evaluated 43 patients for new fistula placement. In preoperative evaluation, 17 patients with previous or existing temporary dialysis catheters in the subclavian vein had moderate or severe subclavian vein stenosis. No stenoses were found in patients without a his-tory of dialysis catheters in the subclavian vein. Wilkin et al (7) used ultrasound to evaluate the IJV of 143 patients with a history of dialysis catheter placement and found right IJV thrombosis in 25.9% of patients and 62% of these were occluded. Neither study assessed visual symptoms or head-ache related to stenosis or occlusion. The question remains whether more aggressive screening measures for papilledema should be instituted for patients with hemodialysis catheters or AVFs to detect possible elevated ICP. A cross-sectional observational case series of 44 patients with peripheral arteriovenous shunts found that none had optic disc edema or symptoms of elevated ICP (8). This low prevalence supports our theory that "two-hits" are required in these patients if they are to develop elevated ICP: 1) the presence of a patent arteriovenous graft poten-tially increasing venous pressures and/or flow and 2) a thrombotic occlusion, as in the other reported cases, or FIG. 3. Venogram after removal of catheter from the right internal jugular vein with improved flow from the right subclavian vein into the superior vena cava. Simon et al: J Neuro-Ophthalmol 2014; 34: 29-33 31 Original Contribution Copyright © North American Neuro-Ophthalmology Society. Unauthorized reproduction of this article is prohibited. TABLE 1. Cases of increased intracranial pressure linked to patient with dialysis catheters or grafts Report Summary of Findings Proposed Mechanism of Increased ICP Intervention and Outcome Lal et al (1) Patient with right AVF, right BCV thrombosis after repeat subclavian vein catheterizations, developed papilledema Retrograde blood flow in the cerebral venous system Arteriovenous graft ligation with resolution of elevated ICP Molina et al (2) Patient with both right and left BCV thrombosis after repeat subclavian and IJV catheterizations developed ICP with bilateral papilledema after placement of right forearm Gor-tex graft Intracranial venous outflow obstruction and retrograde flow Graft was ligated with only partial resolution of elevated ICP Chang et al (5) Patient with left HD shunt and left BCV stenosis developed right optic disc edema, left-sided headache, left face and neck swelling Retrograde flow in left IJV and cerebral venous system and outflow obstruction Balloon dilation of left BCV, with improvement of stenosis and retrograde flow; resolution of symptoms and optic disc edema Cuadra et al (3) Patient with right brachial to IJV graft remaining after successful renal transplant and occlusion of the right axillary, subclavian, and IJVs with bilateral papilledema Cerebral venous hypertension attributed to combination of internal jugular occlusion causing retrograde flow into cerebral and jugular circulation and functioning hemoaccess graft causing increased blow flow Permanent graft occlusion with resolution of cerebral venous hypertension and papilledema Cleper et al (4) Patient with failed kidney transplants, occlusion of the left subclavian and left and right BCVs, calcified right subclavian stent, and stenosed SVC had left brachiobasilic AVF placed and developed facial edema, bilateral optic disc edema, and elevated opening pressure on lumbar puncture Retrograde flow caused by high flow in left AVF contributed to impaired cerebral venous outflow and elevated ICP Balloon dilation of SVC without resolution. Lumboperitoneal shunt with resolution of elevated ICP and disc edema. Patient then developed recurrent elevated intracranial pressure and superior sagittal sinus thrombosis and brain infarction. The AVF was closed, but patient ultimately expired. AVF, arteriovenous fistula; BCV, brachiocephalic vein; ICP, intracranial pressure; IJV, internal jugular vein; HD, hemodialysis; SVC, superior vena cava. 32 Simon et al: J Neuro-Ophthalmol 2014; 34: 29-33 Original Contribution Copyright © North American Neuro-Ophthalmology Society. Unauthorized reproduction of this article is prohibited. occlusion from a permanent central catheter as a mechanism for compromising venous drainage from the jugular system. REFERENCES 1. Lal SM, Twardowski ZJ, Van Stone J, Keniston D, Scott WJ, Berg G, Kirt Nichols W. Benign intracranial hypertension: a complication of subclavian vein catheterization and arteriovenous fistula. Am J Kidney Dis. 1986;8:262-264. 2. Molina JC, Martinez-Vea A, Riu S, Callizo J, Barbod A, Garcia C, Peralta C, Oliver JA. Pseudotumor cerebri: an unusual complication of brachiocephalic vein thrombosis associated with hemodialysis catheters. Am J Kidney Dis. 1998;31:E3. 3. Cauda SA, Padberg FT, Turbin RE, Farkas J, Frohman LP. Cerebral venous hypertension and blindness: a reversible complication. J Vasc Surg. 2005;42:792-795. 4. Cleper R, Goldenberg-Cohen N, Kornreich L, Krause I, Davidovits M. Neurologic and ophthalmologic complications of vascular access in a hemodialysis patient. Pediatr Nephrol. 2007;22:1377-1382. 5. Chang S, Masaryk TJ, Lee MS. Optic nerve edema: complication of peripheral hemodialysis shunt. Semin Ophthalmol. 2004;19:88-90. 6. Surratt RS, Picus D, Hicks ME, Darcy MD, Kleinhoffer M, Jendrisak M. The importance of preoperative evaluation of the subclavian vein in dialysis access planning. AJR. 1991;156:623-625. 7. Wilkin TD, Kraus MA, Lane KA, Trerotola SO. Internal jugular vein thrombosis associated with hemodialysis catheters. Radiology. 2003;228:697-700. 8. Taban M, Taban M, Lee MS, Smith SD, Heyka R, Kosmorsky GS. Prevalence of optic nerve edema in patients on peripheral hemodialysis. Ophthalmology. 2007;114:1580-1583. Simon et al: J Neuro-Ophthalmol 2014; 34: 29-33 33 Original Contribution Copyright © North American Neuro-Ophthalmology Society. Unauthorized reproduction of this article is prohibited. |