| OCR Text |
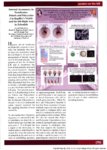
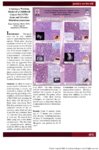
Show posters on the hill Coronary Vascular Function in Insulin Receptor-Deficient Mice Jeffrey Johnson , D. Wade Daniels, Colby Dobson, Daniel Clegg, Rhett Crapo, Jarem Lloyd, J. David Symons Department of Exercise And Sport Science A he heart is a highly aerobic biological organ that requires a constant supply of blood to maintain optimal function. It is important that blood flow and oxygen supply to the heart meet the metabolic requirements of this organ. The heart has its own circulation that is made up of coronary arteries. Arteries are composed of three coats, or "tunics." The innermost layer is the tunica interna, consisting of a single cell layer called the endothe-lium. The middle layer is the tunica media, consisting of a multiple cell layer called vascular smooth muscle (VSM), and the outermost layer is the tunica external. Arteries deliver blood flow to metabolically active tissue, and veins pickup the waste of metabolism; therefore, as metabolism increases, the delivery of blood flow must also increase. In order for blood flow to increase, the vessel diameter must increase. One way blood vessel diameter increases is through the production and release of nitric oxide (NO) located in the endothelium, which then migrates to VSM. Endothelial function refers to the compliancy and reactivity of blood vessels. Dysfunction to the endothelium is associated with physical inactivity, obesity, diabetes, and smoking. In this study we examined the function of the endothelium of coronary arteries of two groups of animals: with insulin receptors and with out insulin receptors. Type 2 diabetics often have a clustering of coronary risk factors including insulin resistance, hypertension, obesity, dyslipidemia, and hyperglycemia. Coronary Vascular Function in Insulin Receptor-Deficient Mice Jeffrey Johnson* , D. Wade Daniels*, Colby Dobson*, Daniel Clegg*, Rhett Crapo**, Jarem Lloyd**, J. David Symons* Department of Exercise And Sport Science* Weber State University** ma'pk p"3t eNQS^ s with type 2 diabetes, the ability of the endothelium to release »xide - a subsUiuv limt -.luimU the \,t>uil.n snu-oili nuisele to dilate -Tipaired. ITiis is termed endothelial <i\ stitnetion. We In pottiesi/ed ilia1 se contributes to endothelial dj sfunction in diabole: To stiufr the indepvii'tvi i i> 'nu iniiiiun from insulin resistance to endothelial disfunction we used mice wherein insulin receptors were deleted genetically. In a damaged \s. ht-;iiih> ireronarj artery the same dose oI.kvIv Idiot me stimulates less nitric oxide release from the eiidotheltum. As such, there is less I relaxation. We hypothesized mat coron;ir\ ;irler\ reflation would be less in vessels from mice with nonet it;iHy deleted insulin receptors. + insulin receptors - insulin receptors Acetylcholine [-log M | + nitric oxide svnthase inhibition ide svnthase inhibition; i > blunted coronary artery relax lin receptors (~); but 2) did signaling molecule oilier than Specifically we wanted to test the hypothesis that insulin resistance per se contributes to coronary artery dysfunction. Insulin is important for all animals and humans due to its ability to allow nutrients to enter tissue cells. Persons with an impaired ability to adequately supply nutrients into tissue cells are termed diabetics. Type 2 diabetes refers to the inability of insulin to allow nutrients into tissue cells. Type 2 diabetics often have a clustering of coronary risk factors including insulin resistance, hypertension, obesity, dyslipidemia, and hyperglycemia. Evaluation of endothelial function can quantify and observe vascular function and occurs in a laboratory setting. Pharmacological drugs such as acetylcholine (ACh) and sodium nitroprusside (SNP) are helpful tools used to study arteries. ACh is used because it is endothelium-dependent, where as SNP is endotheliumindepen-dent. Meaning, when administered locally, these drugs specifically have the ability to stimulate the release of NO from either the endothelium or VSM. This provides researchers with a clearer picture of which aspect of vascular anatomy and function may be impaired. Responses to ACh and SNP were similar in vessels from both groups. These data suggest that a signaling mechanism other than NO can produce vessel diameter dilation to a greater degree in mice without insulin receptors versus mice with insulin receptors. This pathway may be compensating for a lack of insulinmediated NO production due to deletion of insulin receptors in mice. |