| Title |
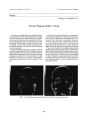
Magnetic Resonance Imaging of Optic Perineuritis |
| Creator |
Fay, AM; Kane, SA; Kazim, M; Millar, WS; Odel, JG |
| Affiliation |
Orbit and Plastics Service, Edward S. Harkness Eye Institute, Columbia-Presbyterian Medical Center, New York, NY 10023, USA. |
| Abstract |
Optic perineuritis, an uncommon variant of orbital pseudotumor, may be clinically indistinguishable from retrobulbar optic neuritis. Because treatment and prognosis for these two entities are different, early diagnosis is important. We report a case of a 47 year-old woman with clinical findings suggestive of retrobulbar optic neuritis, but whose magnetic resonance images suggested optic perineuritis. A dramatic clinical response to oral corticosteroids was observed. Optic perineuritis should be considered in cases of presumed retrobulbar optic neuritis. MRI may differentiate these two entities in the acute stage, and should be considered before treatment is decided. |
| Subject |
Contrast Media; Diagnosis, Differential; Female; Gadolinium DTPA; Humans; Magnetic Resonance Imaging/methods; Middle Older people; Optic Neuritis/diagnosis; Orbital Diseases/diagnosis |
| Format |
application/pdf |
| Publication Type |
Journal Article |
| Collection |
Neuro-Ophthalmology Virtual Education Library: Journal of Neuro-Ophthalmology Archives: https://novel.utah.edu/jno/ |
| Publisher |
Lippincott, Williams & Wilkins |
| Holding Institution |
Spencer S. Eccles Health Sciences Library, University of Utah |
| Rights Management |
© North American Neuro-Ophthalmology Society |
| Setname |
ehsl_novel_jno |
| ID |
224890 |
| Reference URL |
https://collections.lib.utah.edu/ark:/87278/s6wx0pr1/224890 |